Crisis resolution/home treatment (CRHT) teams have been central to English mental health policy since 1999. Their implementation has been rigorously performance-managed. The Department of Heath (2000) set a target of 100 000 people being served by 335 CRHT teams by December 2005. The teams aim to provide an alternative to hospital admission by intervening in the pathway between community-based referrers and in-patient care, providing robust assessment and gate-keeping of admissions. This requires a 24-h service to users in their own homes and opportunities to resolve crises in the contexts in which they occur.
Outcomes of CRHT team intervention include reduced length of stay (Reference Johnson, Nolan and HoultJohnson et al, 2005), reduced rates of admission where teams provide out-of-hours cover (Reference Johnson, Nolan and HoultJohnson et al, 2005; Reference Glover, Arts and BabuGlover et al, 2006), cost-effectiveness (Joy et al, 2001), high satisfaction among users and families (Reference Dean, Phillips and GaddDean et al, 1993; Joy et al, 2001; Reference Johnson, Nolan and HoultJohnson et al, 2005), and better staff morale (Minghella et al, 1998).
Method
The implementation of CRHT teams, perceived obstacles and priorities for development were surveyed between late 2005 and early 2006.
A comprehensive questionnaire was developed through national networks of CRHT providers, piloting with ten services, and formatted for online data entry. Using secure access, respondents were asked to complete the questionnaire in preparation for a telephone or face-to-face interview. The research team supported internet access and provided telephone assistance to respondents completing the online questionnaire.
Teams were included in the study if they had been designed to achieve the outcomes required of a CRHT team locally as described in the Mental Health Policy Implementation Guide (Department of Health, 2002). We identified 243 such teams by drawing together information from the national database then held at the University of Durham and local intelligence provided by Care Service Improvement Partnership CRHT leads.
Analysis
Quantitative data were analysed using non-parametric statistics (SPSS version 13 for Windows) because they were either categorical measures or were not normally distributed. Kruskal-Wallis χ2 or the χ2 coefficient was used depending on the number of categories explored. Post hoc multiple comparisons employed the Mann–Whitney U-test for associations between interval level variables and chi-squared test for associations between two-level categorical data. The Spearman's rank correlation coefficient (r s) was used to examine relationships between interval level variables. Free-text material was collected in response to questions concerning obstacles to implementation and priorities for development. Data were organised thematically into categories, and counts of references to a particular issue or aspect of operation are reported.
Results
Of the 243 identified teams, 73% provided usable data (n=177); 54.5% described their locality as urban, 9.6% as rural and 36% as mixed or suburban. The median team age was 20 months, heavily skewed towards younger teams; 32% of teams had been admitting service users for a year or less. Urban teams tended to be older (Kruskal–Wallis χ2=9.01, d.f.=2, P=0.01; urban > suburban on multiple comparisons).
Team composition
Comparisons between reported staffing levels and projections based on the Department of Health's guidelines (2002) revealed that the number of staff working in CRHT teams was at around 88% of the recommended staffing capacity. The relationship to team maturity was complex, with younger teams (less than 2 years old) often having more capacity than their more mature counterparts.
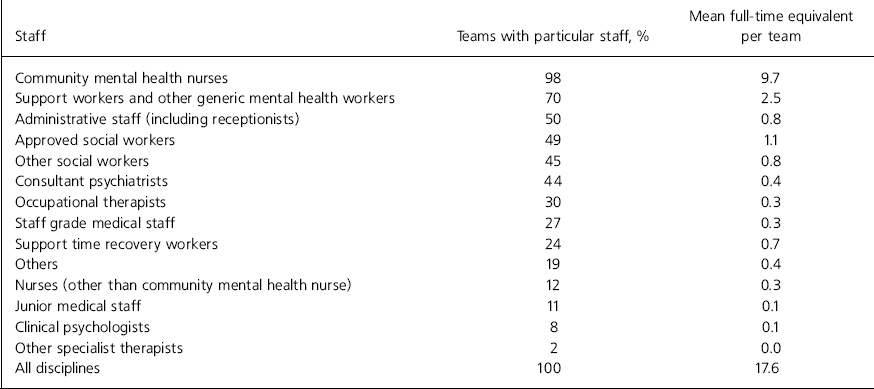
All teams had input from nurses and most had support workers, but less than half had input from any of the other disciplines (Table 1).
Table 1. Team composition (n=164)
| Staff | Teams with particular staff, % | Mean full-time equivalent per team |
|---|---|---|
| Community mental health nurses | 98 | 9.7 |
| Support workers and other generic mental health workers | 70 | 2.5 |
| Administrative staff (including receptionists) | 50 | 0.8 |
| Approved social workers | 49 | 1.1 |
| Other social workers | 45 | 0.8 |
| Consultant psychiatrists | 44 | 0.4 |
| Occupational therapists | 30 | 0.3 |
| Staff grade medical staff | 27 | 0.3 |
| Support time recovery workers | 24 | 0.7 |
| Others | 19 | 0.4 |
| Nurses (other than community mental health nurse) | 12 | 0.3 |
| Junior medical staff | 11 | 0.1 |
| Clinical psychologists | 8 | 0.1 |
| Other specialist therapists | 2 | 0.0 |
| All disciplines | 100 | 17.6 |
Case-load
The mean case-load was 20 service users, the lower end of the policy guidance recommended range. The teams’ case-loads were a mean of 59% of the recommended size taking into account the local populations. Age and size of teams were only moderate predictors of case-load size (r=0.28, P < 0.0005; r=0.24, P < 0.001).
Client group
All teams accepted individuals diagnosed with psychosis or affective disorder, 84% of teams accepted those with a diagnosis of personality disorder and 42% those with a diagnosis of substance misuse.
Progress towards implementation
A measure of ‘fidelity to model’ was developed by determining the extent to which teams’ activities fulfilled the six criteria derived from policy guidance and expert advice. The criteria and frequencies of compliance among the 150 teams that answered all six questions are given in Table 2. Teams reported meeting a mean of 4.9 of the 6 criteria.
Table 2. Fidelity to model criteria

| Criterion | Percentage of teams meeting the criterion, % |
|---|---|
| 1. The team aims to provide an alternative to hospital admission for those experiencing acute mental health difficulties | 98 |
| 2. The team stays intensively involved for as long as necessary for the immediate crisis to be resolved | 97 |
| 3. The team acts as the gatekeeper to the acute in-patient beds by assessing people referred for hospital admission | 72 |
| 4. The team is available on call or on duty between 10 pm and 8 am | 67 |
| 5. The team provides a 7-day per week, 24-h telephone support service | 63 |
| 6. The team provides a 7-day per week, 24-h home-visiting assessment service | 55 |
Fidelity scale ratings were significantly higher among the 40% of teams (n=70) who were described by their team as being fully set up to meet the needs of the numbers of people in their patch who fulfil the criteria for CRHT as defined in the Department of Health's guideline (2002), than among those that did not (mean 5.3 v. 3.9, P < 0.0001).
Fidelity to model was higher among urban teams (Kruskal-Wallis χ2=9.44, d.f.=2, P=0.01; urban > suburban). Half of the urban teams considered themselves fully set up compared with a quarter of suburban teams and 38% of rural teams, and home visiting, telephone support and out-of-hours access were more usual in urban locations.
Key operational features
Only 43% of service users were taken on for ongoing work (median=40%, n=136); 22% were deemed inappropriate, and just over a third were merely assessed. Service users admitted to teams operational for less than 2 years were more likely to be referred on and less likely to be taken on for ongoing work than teams aged 2 years or more suggesting a positive impact of maturation on how teams are used. These differences were accentuated when team size was taken into account.
The most widely and intensively provided interventions beyond assessment were risk management, monitoring of mental state, assistance with self-help strategies, delivering psychosocial interventions and administering medication.
Service users came from community mental health teams (CMHT; 71% reporting daily or more frequently), accident and emergency departments (47.3%), primary care and in-patient services (35.3%).
Service users moved on to CMHTs (31% daily or more often), primary care (20.9%), voluntary sector (8.6%) and in-patient services (8.5%). Almost all (93%) respondents reported delays in referral on to the local CMHT when the crisis had resolved.
Threats to continued effectiveness
Respondents were asked to describe the top three major threats to their continued effectiveness. The most frequent references were to the lack of resources to meet the demands of out-of-hours working and assessments. More staff (n=129) and particularly medical input (n=38) were the most widely sought after resources. Wider funding issues formed the next major category (n=82). There were 67 references to inter-team problems, particularly with CMHT teams (n=24). Medical culture, practices or attitudes formed the fourth major category (n=55). This particularly concerned medical attitudes or practices that undermined the CRHT team's gate-keeping role.
Perceived priorities for development
When asked about the most useful developments or actions that would improve the effectiveness of their service, team developments (n=208) in the form of more staff (n=86), increased medical input (n=30), and particularly dedicated consultant cover (n=18) were most often cited. There were 86 references to wider improvements in local crisis services, including the need for alternative responses to crisis such as crisis beds (n=24) and crisis houses (n=18). There were 19 references to a need for better locally coordinated crisis response, with frequent references to the need for senior managerial support of the CHRT teams’ gate-keeping role. Other ideas included better developed pathways, protocols and criteria (including the recruitment of a pathways development worker) and a manager for the emergency service covering out-of-hours crisis work.
Discussion
Although there were many well-functioning CRHT teams achieving local impact, implementation was variable. Fidelity to policy guidance was compromised in that around a third of teams were not involved in gatekeeping, and only just over half offered a 24-h, 7-day per week home visiting service. More multidisciplinary staffing was the key priority for CRHT team development.
Urban teams formed the majority of CRHT teams, operated with greater fidelity to the guidance and took on a larger proportion of referrals for ongoing work. This lends fuel to the debate over whether CRHT teams offer an essentially urban solution. However, given the wider contextual factors referred to and the constraints of low staffing it would be premature to rush to this conclusion, especially that teams appear to become more targeted in their operation as they mature.
Teams were seeing fewer service users than anticipated. This may reflect lack of staff or the need to remain targeted in the face of pressures to broaden the role of the team in a way that would compromise their capacity for home treatment.
Crisis resolution/home treatment teams exist within complex local systems wherein other key resources such as CMHTs, crisis beds/houses, in-patient and primary care play key roles. Lack of support for CRHT teams in their gate-keeping role was a recurring theme, and the part played by senior medical staff in this is explored further in the accompanying paper.
Comprehensive and detailed implementation guidance does not guarantee adequate implementation even in the context of strong performance management at both provider and commissioner level. Committed and transparent funding, sufficient development support, and strong local leadership to improve inter-team working within a local whole-system of provision are also needed.
Declaration of interest
Funded through the Department of Health's Policy Research Programme.





eLetters
No eLetters have been published for this article.