Recent Department of Health Guidelines (1999, 2001) have encouraged the development of crisis intervention teams. This paper describes the development and activity of an emergency response service (ERS) that aimed to offer crisis intervention to individuals who presented to primary care teams in one sector of Newcastle upon Tyne. The activity of the service over the first 6 months after its inception was evaluated by monitoring the nature of the referrals and the workload of the staff. In addition, we explored satisfaction with this service from the point of view of the patients referred to the service, the general practitioners (GPs) using it and the community psychiatric nurses (CPNs) providing it.
The service
In the late 1990s in Newcastle upon Tyne, it was noted that over a 4-year period there was a twofold increase in GP referrals for urgent psychiatric assessment of individuals in crisis. There were multiple points of access to the service for these referrals: some were assessed by junior doctors in accident and emergency departments; some as emergency assessments at out-patient clinics; some were seen by members of community mental health teams, either at home or at resource centres; and some individuals were admitted directly to hospital via their GPs. However, there was no consistent or predictable pattern regarding who saw the individuals referred, where they were seen or the treatment package provided. A substantial number of the referrals were admitted to hospital, even though it was acknowledged by primary and secondary care staff that this was often less than ideal.
Discussions between primary and secondary care teams identified that the concerns of the GPs focused on difficulties in providing the appropriate time, skills and resources to assess and manage individuals presenting in crisis in primary care. The concerns of the specialist mental health service providers focused on the need to reduce pressure on in-patient facilities and staff by avoiding inappropriate admissions and identifying and referring individuals efficiently to the most appropriate treatment option. Representatives of the two groups decided to devise a service for individuals presenting in primary care in crisis that met the needs of the individual and addressed the concerns of the professionals.
The agreed goals of the emergency response service were:
-
(a) to improve access to clinical assessment for individuals in acute crisis;
-
(b) to streamline the referral and assessment process so that all parties were clear about where and when such referrals would be seen; and
-
(c) to improve the standard of crisis assessment, providing a consistent response and early feedback to GPs.
The service initially was set up in the West End of Newcastle upon Tyne. This sector comprises about 140 000 people living in a deprived inner-city area with high levels of unemployment and a large ethnic minority population. It was decided that the emergency response service would be extended to other catchment areas in the city if it met the needs of the patients and was acceptable to patients, GPs and service staff. No new staff were employed to provide the service, but the ten CPNs currently attached to community mental health teams in the western sector participated in an on-call rota for the service. Its hours of operation were 9.00 to 21.00 on Monday to Friday and 10.00 to 16.00 over the weekend.
Method
Using a pre-coded proforma, data were recorded on consecutive referrals to the emergency response service over the first 6 months of operation. The information on service activity included total number of referrals, source of referral, total number of assessments undertaken, time and venue of assessments, waiting time from referral to assessment and data on the amount of time that service staff spent in face-to-face contact with clients during their working week. For each individual who was assessed, information was collated on demographic details, reasons for referral, whether they were known to the mental health services, whether they had a past history of mental disorder and the outcome of the referral. Data on psychiatric admissions via the service were then compared with direct admissions via primary care teams for the same months, a year prior to the introduction of the new service.
To assess patient views of the emergency response service, all individuals referred during the fourth month of operation (n=47) were offered the opportunity to complete the Client Satisfaction Questionnaire (CSQ; Reference Larson, Atkinson and HargreavesLarson et al, 1979). The CSQ is a self-report questionnaire that has eight closed questions, each answered on a four-point scale (1=very dissatisfied, 4=very satisfied). Six additional questions (answered on the same four-point scale) were added to the CSQ, asking participants specific questions regarding the quality of the response they received from the service. Thus, the questionnaire scores ranged from 14 to 56. Additional open questions also asked subjects what they liked or disliked about the service and offered the opportunity for further comments or recommendations. To assess the GP and ERS staff views of the service offered, all the GPs in the catchment area and all the CPNs working with the ERS were sent a modified version of the 14-item CSQ so that the questions related to their perceptions and satisfaction with the service.
The questionnaire took about 10 minutes to complete. Participants were encouraged to contact an independent research assistant (Janine Williamson) for more information if required. In some instances, the researcher visited practice meetings or emergency response service team meetings to explain the purpose of the questionnaire. Confidentiality was guaranteed and participants were encouraged to provide their honest opinions. Participants who failed to respond after 4 weeks were sent a reminder letter, a further copy of the CSQ and a pre-paid envelope.
Data were analysed using the Statistical Package for the Social Sciences (SPSS, version 9.5). Descriptive statistics were used to compare continuous and categorical ratings.
Results
Emergency response service referrals and activity
The service received 167 referrals in the first 6 months of operation. The number of referrals per month for the first 3 months ranged from 23 to 28 (mean=25.3), but increased significantly to a mean rate of 51.5 (range=47-59; t=3.5; d.f.=166; P<0.05) during the second quarter. Ninety per cent of referrals (n=151) were made by GPs and all but five of the 82 GPs working in the catchment area made at least one referral (median=4; range=0-11). One in five referrals (n=35) were made after 17.00 and one in seven (n=23) over the weekend. Seventy-five per cent (n=126) of referrals participated in an assessment interview. Of the 41 individuals who were not assessed, just over 50% (n=23) refused the offer of an assessment during a preliminary telephone contact and the other 18 were not at home or not available when emergency response service staff visited (1-4 attempts to visit were made for each person). Over 90% of assessments were made in the individual's home (n=114), with 62% seen within 2 hours and less than 15% (n=18) waiting longer than 4 hours. Seventeen assessment visits were undertaken jointly with the GP, and ERS staff alone undertook the rest. Staff working with the ERS calculated that just under half of their time (45%) was spent in face-to-face contact with patients, whereas 10% of their time was spent travelling and 15% on telephone work.
Characteristics of emergency response service patients (Table 1)
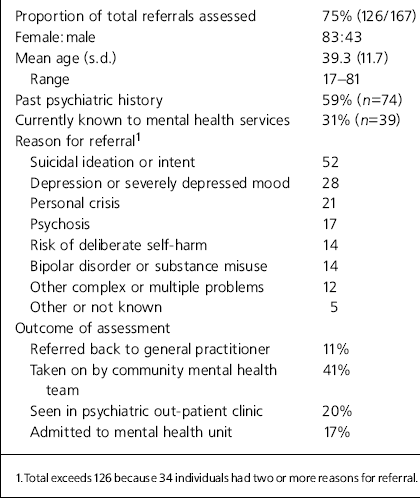
Two-thirds of the 126 subjects assessed by the ERS were female (n=83) and 48 (38%) lived alone. The age of the sample ranged from 17 to 82 years (mean=39.3; s.d.=11.7). The limited data available on the individuals who did not participate in the assessment interview (n=41) did not reveal any significant demographic differences from those who were assessed. Although the majority of those assessed (59%) had a past psychiatric history, only 31% (n=39) were currently known to the local mental health services. Exploration of reasons for referral revealed that the 126 subjects reported at least 164 key problems, with about one in three subjects (n=37) reporting two or more major problems. The most common reasons for referral were: suicidal ideation or intent (n=52); depression or severely depressed mood (n=28); personal crisis (n=21); psychosis (n=17); risk of deliberate self-harm (n=14); problems related to bipolar disorder (n=8) or substance misuse (n=6); toxic confusional state (n=2); other complex or multiple problems (n=12); and not known or not clear (n=5). After assessment, 14 subjects (11%) were referred back to their GP, the community mental health team staff took on 41% of cases, 20% were referred to psychiatric out-patient clinics (including specialist services such as Problem Drug Use) and 17% (n=21) were admitted.
Table 1. Characteristics of 126 individuals assessed by the emergency response service
| Proportion of total referrals assessed | 75% (126/167) |
| Female: male | 83:43 |
| Mean age (s.d.) | 39.3 (11.7) |
| Range | 17-81 |
| Past psychiatric history | 59% (n=74) |
| Currently known to mental health services | 31% (n=39) |
| Reason for referral1 | |
| Suicidal ideation or intent | 52 |
| Depression or severely depressed mood | 28 |
| Personal crisis | 21 |
| Psychosis | 17 |
| Risk of deliberate self-harm | 14 |
| Bipolar disorder or substance misuse | 14 |
| Other complex or multiple problems | 12 |
| Other or not known | 5 |
| Outcome of assessment | |
| Referred back to general practitioner | 11% |
| Taken on by community mental health team | 41% |
| Seen in psychiatric out-patient clinic | 20% |
| Admitted to mental health unit | 17% |
Changes in admission via primary care
The ERS team admitted 21 of the referrals from primary care teams. Data from the hospital information system demonstrated that there were 53 direct admissions via primary care teams during the equivalent 6-month period of the year prior to introduction of the service.
Satisfaction with the emergency response service
Twenty of the 47 individuals (43%) referred to the ERS during a pre-selected 1-month period returned a completed CSQ. The mean CSQ score of 43.1 (s.d.=7.3) indicated that the majority of clients were ‘mostly satisfied’ with the service. Answers to specific questions revealed that 60% of clients felt that the service met ‘most or all’ of their needs. Only two of the individuals who made a response gave negative feedback about the service, although four specifically stated that they would have preferred to be seen away from their own home. Eight subjects suggested that the hours of the service should be extended.
Seventy-two GPs returned questionnaires and 67 (75%) had completed sufficient questions to allow a CSQ rating to be made. The mean CSQ score was 39.4 (s.d.=9.1). Forty-three GPs were satisfied or very satisfied with the service; 13% (n=18) felt that it had reduced their workload, 47% liked the quick response and 64% felt that the feedback from assessments was comprehensive and prompt. However, four GPs were unhappy that they had to see each patient before making the referral, eight felt that it increased barriers to seeing a psychiatrist and eight also felt that it delayed the admission process. Overall, 58% of GPs thought that the service was worthwhile, but 44% suggested that the hours should be extended further.
Eight of the ten CPNs working with the emergency response service returned questionnaires. The mean CSQ score was 34.7 (s.d.=5.1). Seven staff commented that working for the service had been a positive experience, although four commented that they had received inappropriate referrals and three had concerns about personal safety. Half of the group felt satisfied with the input that they offered to clients and 75% felt that the service offered appropriate and timely help to the clients referred. Overall, the eight CPNs all thought that the service was worthwhile but 38% (n=3) suggested that the hours should be reduced.
Conclusions
This study suggests that the emergency response service achieved many of its key objectives. It appeared to reach its target population, it assessed the majority of those referred quickly (over 60% seen within 2 hours) and it reduced the number of admissions for acute crises. Interestingly, although 60% of those assessed had a past history of psychiatric problems, the majority were not currently in contact with any local services. Following the assessment, about one in ten individuals were referred back to their GP without any further specialist mental health input, whereas about one in six were admitted. This admission rate represented a 60% reduction on direct admissions via primary care in the equivalent 6-month period of the year prior to the introduction of the service.
The above successes are balanced by the low rate of referrals to the service, averaging less than one per day in the first 3 months. Although the referral rate increased significantly during the second 3-month period, it still only averaged about two per day during the week and about three per weekend. Furthermore, over the whole 6 months, only a third of the referrals were made outside of office hours. We do not know whether other referral pathways were still being used (e.g. direct referrals to accident and emergency departments or to senior psychiatrists), but the level of activity of the service will need to be monitored carefully to establish whether it represents a cost-effective approach.
The majority of patients, GPs and CPNs who completed the CSQ were satisfied with the service offered. However, given that 90% of individuals assessed were seen in their own homes, it is of interest that, although patients liked the speed of response, a significant minority (20%) stated that they would have preferred the anonymity of being seen elsewhere. (Many of the CPNs expressed a similar view, but for reasons of personal safety.) General practitioners mostly liked the speed of response and the feedback they received from the CPNs. It is noteworthy that the individuals least satisfied with the service were the staff providing it. Some of the CPNs' frustrations related to the service configuration. Although they offered assessments to all the clients referred and recommended a variety of treatments, the CPNs were rarely involved any further in that individual's care. Second, no senior medical input was identified to support specifically the emergency response service staff. This often meant that further expert advice was not available when it was most required. Finally, the CPNs reported significant periods of inactivity and suggested that the service hours could be reduced without a detrimental effect on its quality. In contrast, the GPs and the individuals using the service suggested that its hours should be extended.
In summary, the introduction of the service led to a faster, more consistent process of assessment of crisis referrals. In addition, undertaking assessments in the community appeared to increase the use of alternative treatments for individuals in crisis before resorting to admission. Although this paper supports the general principle of crisis services, it highlights that clinicians believed that an emergency response service might be more effective if the crisis team also offered the care and treatment that they advocate. Although the latter is in keeping with other models of crisis intervention, many of these require the introduction of a new dedicated service, with obvious resource implications (Reference Geller, Fisher and McdermeitGeller et al, 1995). If funding opportunities are restricted, the development of an emergency response service through the use of current staff from a number of community mental health teams is an option worth considering. However, for maximum efficiency, dedicated senior medical psychiatric input needs to be included in the service specification so that the decisions about case management are made by frontline staff in collaboration with psychiatrists having the appropriate level of expertise and experience.
Acknowledgements
Janine Williamson (formerly research assistant in Newcastle upon Tyne) collected the data and wrote the preliminary draft of a report on satisfaction with the emergency response service for the District Health Authority. Unfortunately, she left Newcastle to join a clinical psychology training course and we have not been able to re-establish contact to get Janine's permission to include her as an author on this paper. However, we wish to acknowledge her considerable input to this project.
Newcastle and North Tyneside District Health Authority funded this project.




eLetters
No eLetters have been published for this article.