Government statistics suggest that approximately one-quarter of those presenting to drug misuse agencies are women of child-bearing age and a significant number of women using substances are therefore likely to become pregnant (Department of Health, 1999). It is not easy to accurately quantify the prevalence of illicit drug use in obstetric populations and this is likely to vary considerably according to time and place. Research in the United States shows that more than 5% of the 4 million women who gave birth there in 1992 used illegal drugs while they were pregnant, with cannabis and cocaine being the most commonly detected (Westat Inc., 1996). Studies of anonymous testing in obstetric populations in the UK have been conducted in inner cities, demonstrating that between 6.5% and 8.5% of urine samples were positive for cannabis and 2% for opioids (Reference London, Caldwell and LipsedgeLondon et al, 1990).
Treatment of pregnant women dependent on opioids is of great importance. There is evidence indicating an improvement in neonatal and obstetric outcome with the provision of regular antenatal care and reduction and/or stabilisation of drug use (Reference Ward, Mattick, Hall, Ward, Mattick and HallWard et al, 1998, Reference FischerFischer, 2000). Pregnancy may be a crucial point for potential change in a career of drug use and may offer the woman the chance to resolve a number of housing, employment, legal and other social problems. The Addictive Behaviours Centre in Birmingham was one of the earliest regional drug treatment units and one of the first to establish a mother and baby team in June 1987. The initial aims have remained consistent throughout the past 14 years and include:
-
• engaging women in treatment for the duration of their pregnancy and beyond;
-
• providing practical and emotional support to drug users during pregnancy and early motherhood;
-
• encouraging mothers to use antenatal and post-natal services;
-
• promoting the welfare of the children;
-
• supporting parents if they want to withdraw from drugs and providing ongoing support to help them remain drug-free.
We set out to review the past 5 years of the service to see if the aims were being met.
Method
We conducted a retrospective case note review, looking at referrals to the service over 5 years (1996-2000). A data collection form was developed and a pilot analysis undertaken on 20 referrals, studying both the notes kept by the member of the mother and baby team and the medical notes. The data collection tool was then revised and all the referrals taken on by the service between January 1996 and December 2000 were reviewed.
Results
Changing pattern of referrals to the service
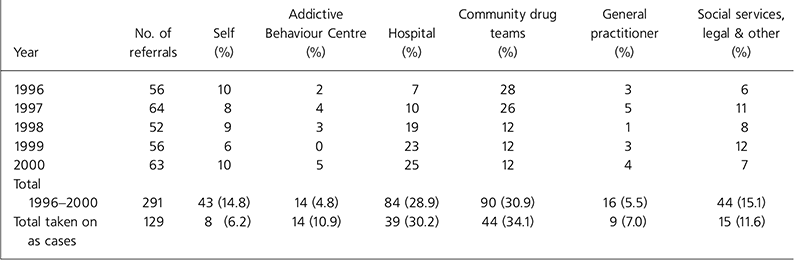
In the 5-year period under study, 291 referrals were made to the mother and baby team, with 129 seen at least once. The 129 cases comprised 118 women, with nine having two pregnancies in the time period under study and one having three. There were a number of different referring agents, which are summarised in Table 1.
Table 1. Agent referrals to the mother & baby team
| Year | No. of referrals | Self (%) | Addictive Behaviour Centre (%) | Hospital (%) | Community drug teams (%) | General practitioner (%) | Social services, legal & other (%) |
|---|---|---|---|---|---|---|---|
| 1996 | 56 | 10 | 2 | 7 | 28 | 3 | 6 |
| 1997 | 64 | 8 | 4 | 10 | 26 | 5 | 11 |
| 1998 | 52 | 9 | 3 | 19 | 12 | 1 | 8 |
| 1999 | 56 | 6 | 0 | 23 | 12 | 3 | 12 |
| 2000 | 63 | 10 | 5 | 25 | 12 | 4 | 7 |
| Total | |||||||
| 1996-2000 | 291 | 43 (14.8) | 14 (4.8) | 84 (28.9) | 90 (30.9) | 16 (5.5) | 44 (15.1) |
| Total taken on as cases | 129 | 8 (6.2) | 14 (10.9) | 39 (30.2) | 44 (34.1) | 9 (7.0) | 15 (11.6) |
Demographic details of cases
The mean age at presentation to the service was 24.3 years, with a range of 15 to 39 years. Mean gestation at first assessment was 19.8 weeks (range 6-38 weeks) and 20 of the 129 cases (15.5%) had been in contact with the service previously. Of the 118 women in the sample, 40 admitted to ever having injected drugs and nearly half of these (19) had shared equipment. At the time of first assessment, 25 women had previously undergone viral testing, and a further three had tests facilitated by the mother and baby team during their pregnancies. In total, two were positive for hepatitis B and C, nine were positive for hepatitis C only and one for HIV. A majority of the contacts (81, 68.6%) recorded a partner who used drugs.
Contact with the service
The 129 cases remained in contact with the team for an average of 40 weeks (range 0-236), with an average of 9.8 face-to-face contacts during that period. Table 2 shows that 92 (71.3%) remained in contact with the service for more than 20 weeks. The percentage of cases that had attended at least one antenatal appointment increased from 49% to 67% after contact with the team.
Table 2. Length of contact with the mother & baby team

| Time in contact with service | Number |
|---|---|
| 30 weeks+ | 66 |
| 20-29 weeks | 26 |
| 10-19 weeks | 23 |
| < 10 weeks | 14 |
Drug use
At initial assessment, 65 women were using heroin, at an average dose of 0.74 g per day (range 0.05-2.5 g). A total of 54 were being prescribed methadone, at an average dose of 38.9 mg, with a further 12 admitting to buying street methadone (average daily dose of 55.5 mg). Other drugs used at the time of initial assessment were crack cocaine (23 cases), benzodiazepines (22), amphetamines (11) and dihydrocodeine (5).
Treatment
During the review period, the preferred treatment strategy for women using heroin was methadone replacement therapy, with the option of slowly withdrawing the drug if the patient wished. Of the 129 cases, 40 commenced a reducing oral methadone regime, which 10 had completed by the time of delivery. In total, 99 patients were prescribed methadone mixture, at an average dose of 35.9 mg/day (range 15-130 mg). Data were available on 80 of these cases at the time of delivery and the mean dose of prescribed methadone had fallen to 31.8 mg/day (0-100 mg), with 12 patients being opioid-free. Benzodiazepines were prescribed to 22 patients, at an average initial dose of 25.0 mg diazepam per day. At delivery, data were available for 16 of these cases, with the average dose then being 23.4 mg. Five women were taking prescribed amphetamines prior to becoming pregnant and were therefore maintained on dexamphetamine throughout pregnancy at an average dose of 35 mg. By delivery, one woman had reduced her dexamphetamine intake to zero, with the other four remaining on a constant dose throughout pregnancy. At delivery, 16 of 113 women prescribed medication were completely drug-free.
Outcome of the pregnancy
Data were available for 108 cases, with 101 live births. Three women had terminations of pregnancy and there was one miscarriage. One woman had a stillborn baby and a further two babies died soon after birth. On average, each pregnancy lasted 37.7 weeks (19-44 weeks).
Child protection issues
Of the 89 cases with a history of a previous pregnancy, 35 had experienced child protection issues. In 66 of the cases studied, social services were contacted during the pregnancy and child protection proceedings were initiated in 32 of them.
Conclusions
Pregnant women who are dependent on opioids form an important group to target, given the potential medical and obstetric complications. Use of opioids can lead to poor nutrition and neglect of basic self-care, leading to an inhibition of foetal growth and an increase in perinatal mortality due to prematurity and late-pregnancy stillbirth. The problem is compounded by the failure of women using heroin to access antenatal care, possibly due to fears of negative attitudes from staff and concerns that their babies will be taken into care. Furthermore, the lifestyles led by some users of illicit drugs may lead to poor communication between treatment agencies.
This was a retrospective case note review and, as with many such studies, we encountered the problem of missing data. As the mother and baby team served most of the West Midlands area throughout much of the period under study, detailed records of births and the early neonatal period were unavailable. However, the data do illustrate that many of the aims of the team were met. Table 1 shows that, throughout the period under study, there was a steady increase in the number of referrals from hospital obstetric services, demonstrating the growing awareness of the benefits of the team. Furthermore, referrals from the community drug teams decreased, as each became more skilled at managing pregnant women who misused drugs with support from the tertiary service.
There was a high level of engagement with the service, as the majority of women stayed in contact for over 20 weeks. This ensured support throughout most of the pregnancy and resulted in increased contact with antenatal services. At the initial contact with the mother and baby team, 113 of the 129 women (87.6%) were using opioid drugs and the service prescribed methadone to 99 of these. The average dose of methadone fell during the course of the pregnancy and at the time of delivery, only 20 of the 80 (25%) cases still in contact with the service had urine tests that were positive for heroin. The primary aim for those women using opioid drugs was usually stabilisation on methadone but, contrary to the experience of other authors (Reference FinneganFinnegan, 1991), a significant number of women managed to completely detoxify from all drugs by the point of delivery. Furthermore, although dexamphetamine maintenance prescribing for amphetamine use is a controversial (but commonly used) treatment (Reference Fleming and RobertsFleming & Roberts, 1994; Reference WhiteWhite, 2000), it is interesting to note that the five women maintained on the drug had good outcomes from their pregnancies.
One of the reasons often cited for pregnant women not accessing medical services is the fear that their child will be removed by social services. There is some evidence that the mother and baby team was able to overcome this fear, as a large number of women returned for care after problems in their first pregnancy. Child protection proceedings were initiated in nearly a quarter of the cases studied, but in each case, the mother was supported by the ongoing work of the team. This issue will be the subject of a further prospective study of this group of women who misuse substances.
Declaration of interest
None.





eLetters
No eLetters have been published for this article.