Cancer is one of the leading causes of death worldwide, with its prevalence expected to rise (National Cancer Institute 2020). In terms of illness-related needs and with respect to how it impacts each family member (Rolland Reference Rolland2005) and the relative family dynamics, the toll seems profound. Family caregivers frequently feel alone in the decision-making process and report difficulties communicating with their loved ones as they try to make sense of an impending death (Rolland Reference Rolland2018; Totman et al. Reference Totman, Pistrang and Smith2015).
As people are living longer (WHO 2022), our society has come to need informal “frontline health care workers” (Kent et al. Reference Kent, Ornstein and Dionne-Odom2020: 67), such as family caregivers, among whom the strain is evident. This is particularly true for people in their sixties who are no longer able to care for older family members (Rolland Reference Rolland2018), given that they are potentially still working full time or taking care of children and/or grandchildren, in addition to sometimes managing personal health issues.
Demographically, this population tends to be mostly women, who spend more time providing care than their male counterparts (Northouse et al. Reference Northouse, Katapodi and Schafenacker2012; Rolland Reference Rolland2018). In Europe, it is estimated that from 10% to 25% of the population comprises informal caregivers (European Commission 2018). Similarly, in the United States, around 1 in 5 Americans represents this population of caregivers (National Alliance for Caregiving [NAC] & AARP 2020). On average, informal caregiving implies about 20 hours a week, which involves helping with daily life activities and providing social, emotional, and practical support (Lightfoot and Moone Reference Lightfoot and Moone2020) (e.g., buying medication and going to the supermarket). The data, which frequently pertain to lower-income families (Rolland Reference Rolland2018), show that most family caregivers must juggle work with caregiving tasks. Therefore, family caregivers of cancer patients are a vulnerable population, presenting significant levels of psychological morbidity (Areia et al. Reference Areia, Major and Gaspar2017). Research has already indicated that caregivers of cancer patients have higher levels of depression and anxiety than the patients themselves (Fu et al. Reference Fu, Zhao and Tong2017).
Palliative care among cancer patients
According to Neto (Reference Neto2020), 8 in 10 patients enrolled in palliative care (PC) services have cancer. The PC approach is mainly focused on preventing and relieving physical, psychological, social, and spiritual suffering of both patients and their families facing life-threatening illnesses (World Health Organization 2018). Nonetheless, the continued “disease-fighting approach” takes over, which sometimes extends the agony of the person (Neto Reference Neto2020) and, consequently, of their family.
Due to some gaps in this field (e.g., insufficient resources and a lack of accurate information to make referrals), most patients and families only start to benefit from PC at a later stage in the course of the illness. This means that the aforementioned “frontline workers” are going to be enrolled in this 24/7 role for longer periods.
PC during uncertain times
In addition to its physical and emotional toll and uncertainty, the Covid-19 pandemic made us think about “goodbyes.” With the pandemic outbreak, the Portuguese government implemented several contingency measures (Passos et al. Reference Passos, Prazeres and Teixeira2020), such as stay-at-home orders, social distancing, recommendation of remote working, wearing facemasks, or, when necessary, confinement periods (Oliveira et al. Reference Oliveira, Sotero and Relvas2022). Within health institutions, it imposed some restrictions and created a general fear for the most vulnerable, leading to situations where relatives and primary caregivers were prevented from having face-to-face contact with their ill family members throughout their hospital admissions during the pandemic’s worst outbreaks. In fact, Passos et al. (Reference Passos, Prazeres and Teixeira2020) suggested that isolation might be a risk factor for depression. Imber‐Black (Reference Imber‐Black2020) reinforces the role that end-of-life rituals have on helping us go through loss and bereavement, and even though PC institutions tried to continue to do their work, some processes were modified or suppressed due to the virus. Therefore, Covid-19 hampered these processes and made us “dive” into an even more technological daily world, where old rituals were transformed and new ones emerged (e.g., celebrating anniversaries on balconies and “zoom” gatherings) (Imber‐Black Reference Imber‐Black2020).
The present study
We tried to grasp the main obstacles related to being a family caregiver of a cancer patient receiving PC – reported by caregivers and/or perceived by health professionals working in these settings. An obstacle was any difficulty, struggle, problem, or less adaptive coping strategy. To achieve the research goal, we collected data from 3 different sources to ensure corroboration (Bowen Reference Bowen2009): written files from 2 Portuguese PC institutions, to which the present paper refers to; focus groups with health professionals working in PC; and focus groups with family caregivers of cancer patients receiving PC. (Bowen Reference Bowen2009). This study considered a “primary caregiver” the person or people mainly responsible for taking permanent care of a family member or friend who is terminally ill or with a disabling condition.
We employed a thematic analysis of the information collected from institutional written files.
Methodology
The present study draws on a qualitative research methodology to provide a more in-depth understanding of family caregivers of cancer patients’ experiences as well as health professionals’ from a PC setting who support them. The data used in the current paper stem from information collected from a subsample of written files from 2 Portuguese PC institutions, including 159 individuals’ processes. The current study was submitted to each institutions’ ethics committee to obtain permission, in addition to an ethical evaluation of the process of its funding.
Data collection and the institutions’ description
Both institutions have multidisciplinary teams, with different professionals working collaboratively. One is based in the north of Portugal (referred here as Institution A), and the other is in the central region (mentioned as Institution B). Besides the Palliative Care unit, Institution A has a Long-term and Maintenance unit, and a Medium Duration and Rehabilitation unit, which are part of the National Network for Integrated Continued Care. Its Palliative Care unit can admit 10 patients. In turn, Institution B has a Palliative Care and a Recovery unit, an Outpatient Surgery Unit, an Outpatient Unit with various medical services, Day Unit, and Home Support. This institution has 18 beds. Data collection took place between March 2021 and December 2021. The files from one institution are from May 2020 to June 2021, whereas the others pertain to January 2021–April 2021. As the process occurred during an active Covid-19 pandemic period in the country of research, some delays were experienced.
The first author went in-person to both establishments. Institution A had its written files organized in folders, whereas Institution B provided the files through a secure online platform. To assemble data in a standardized manner, the first author developed a table that was filled in with the relevant data from the written files. Some of the latter were the files’ ID (only recognized by the first author), dates of admission and discharge or death of the patient, the diagnosis, number of (primary) caregivers, relationship with them, their ages, and occupation, caregivers’ obstacles written in the files and to whom they were reported – if this information was possible to obtain – and also other notes that might be important to the study.
No personal information from the patient was collected, except the diagnosis. Files from non-cancer patients were excluded. The process of data collection ceased when theoretical saturation was reached.
Data analysis
The authors coded the data using QSR NVivo 12 software. Considering Braun and Clarke (Reference Braun and Clarke2006), they conducted an inductive thematic analysis – a type of data-driven analysis in which data did not fit into a pre-existing coding frame – with a latent approach, considering the analysis went beyond the semantic content of professionals’ notes (Braun and Clarke Reference Braun and Clarke2006). Nonetheless, there was a research question formulated at the outset. Initially, the first author proceeded to an open code of the written files creating categories; these were then grouped into larger categories, which generated the central themes identified. For the purposes of counting, categories were only acknowledged when there was at least one reference coded. Those categories that were only the name of the larger category (e.g., “Burden”) were not considered for this counting.
To ensure methodological integrity in the coding process (O’Connor and Joffe Reference O’Connor and Joffe2020), after all data were initially coded by the first author, the second author double-coded around 56% of all datasets. It promoted a more in-depth reflection on the codes and led to a progressive refinement of each category and confidence in the results.
Results
Content analysis of the written files yielded 40 interrelated categories, organized in 3 overarching categories, which we will examine for the purpose of this study: (a) burden; (b) intra-family impact of the illness; and (c) network vulnerabilities. In addition to the latter, 6 categories were defined regarding important caregivers’ features, such as their role (i.e., formal caregiver, primary caregiver, or secondary caregiver), their relationship with the patient (i.e., son, partner, or friend), age, and gender (Table 1), and the way the caregivers were grouped (e.g., only one primary caregiver, one primary caregiver and one formal, and so on) (Table 2). For the synthesis and description of the entire group of categories and subcategories, please refer to Table 3.
Table 1. Family caregivers’ sociodemographic variables and their relationship with the patient

FCG = family caregiver. 81.8% of the files did not provide all the information about caregivers’ age; 16.4% did not provide information about their sex.
Table 2. Who was taking care? Primary and non-primary caregivers

FCG = family caregiver; NONPRIM = non-primary; PRIM = primary.
Table 3. In-depth description of each category and subcategory
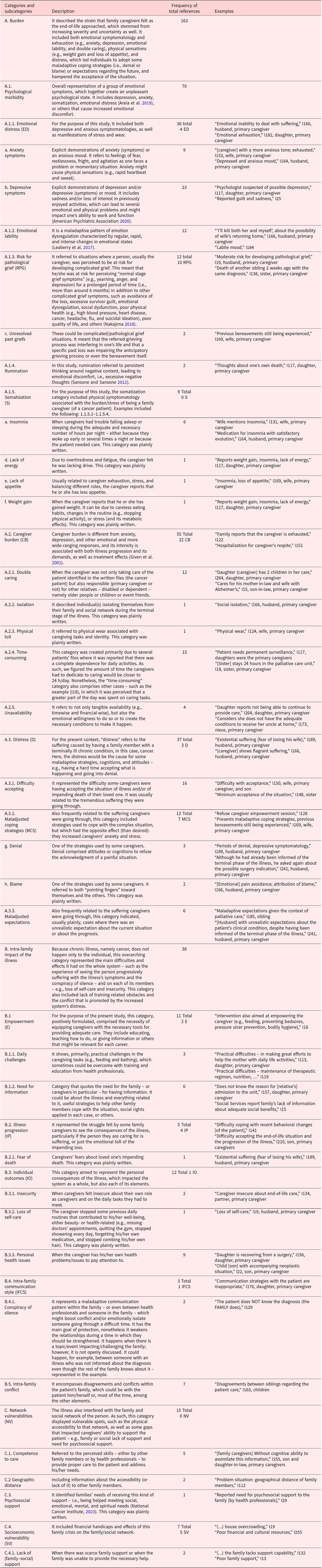
Some quotations from professionals’ notes and entries about family caregivers’ experiences are included to better explain and describe each (overarching) category. To present them, we created an identification code to each file, which does not allow the identification of the person or file. Hence, we present each entry’s code, followed by the person’s relationship with the patient and role in the family – usually primary caregiver – or only the code if the entry is about the family unit (e.g., “Family’s lack of information about adequate social benefits,” I15).
Figure 1 summarily depicts the main results and Fig. 2 details the number of references of each (main) categories.

Figure 1. Main overarching themes and subthemes.
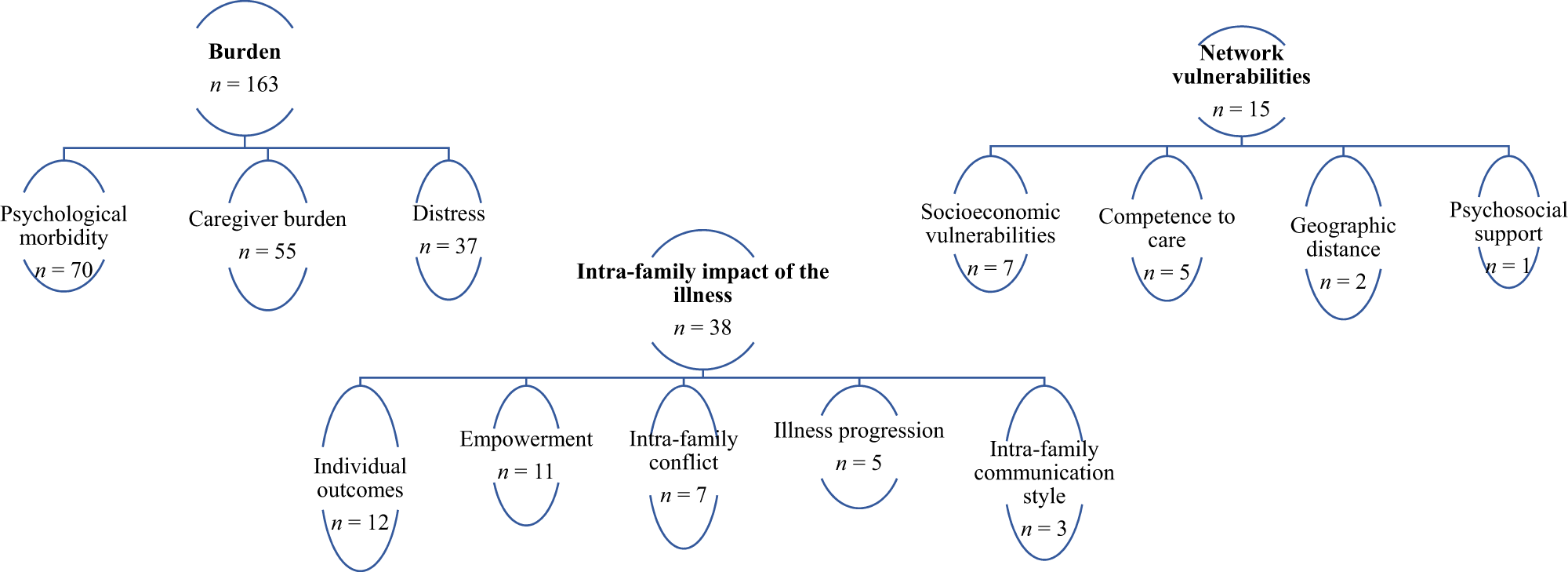
Figure 2. References of each main theme and subtheme.
In these written files, professionals tend to be straightforward in their notes of caregiver’s feelings and experiences – for example, they simply write “emotional exhaustion” (I182, daughter, primary caregiver). Therefore, the present section stems from not only the analysis but also authors’ interpretation of the said notes. It is also important to highlight that we only have access to health professionals’ “lens,” thus our interpretation is merely based on their entries.
How burdened are caregivers?
Burden is one of the overarching categories representing the obstacles associated with caring for a terminally ill cancer patient in PC. It represented the toll this population usually suffers from over long periods of time, often with no extra-help or education to perform the tasks they are expected to do, which has a cascading effect on their mental health. The burden can be expressed psychologically – through emotional discomfort or disorders (e.g., anxiety and depression) – as well as by physical problems, namely somatic complaints (e.g., tension, headaches, and pain) (Gratao et al. Reference Gratao, Vendrúscolo and Talmelli2012).
With 163 coded references in total, it emphasized the “caregiver burden,” the “psychological morbidity,” and the “distress” at having a terminally ill family member. The authors verified caregiving involved an extensive amount of time, conforming to the literature and to their reports about one of their struggles: “Difficulty reconciling her professional and caregiving roles” (I157, daughter as primary caregiver). The perception of pathological states, including atypical levels of negative psychological, emotional, and/or behavioral states (Craig et al. Reference Craig, Tran and Middleton2009) (e.g., depression, anxiety, emotional liability, and others), was included in 1 of 5 subthemes of the psychological morbidity’s category.
As expected, oftentimes there was a perceived expression of depression, which was, occasionally, related with other negative emotional symptomatology (n = 12), such as emotional lability, anxiety, or symptoms that prevented the natural course of the grieving process. In fact, professionals considered that a significant number of caregivers felt anxious and depressed when confronted with cancer (Sklenarova et al. Reference Sklenarova, Krümpelmann and Haun2015). A depressive state was considerably more prevalent in female caregivers – around 73% (e.g., “Depressive mood; emotional lability; pathological grief,” I117, daughter, primary caregiver).
With 9 coded references, anxiety appeared to be, from professionals’ notes, an important obstacle during the caregiving period, particularly given its apparent relationship with exhaustion: 5 family caregivers simultaneously coded for anxiety and caregiver burden – this is, “Mood with a somewhat anxious tone; signs of caregiver exhaustion,” I160, son, primary caregiver. In addition, 4 out of 9 references from anxiety were grouped with depressive mood (e.g., “depressive and anxious mood,” I168, daughter, primary caregiver).
Health professionals also reported the potential risk for the development of pathological grief as a probable obstacle for family caregivers, usually present when the caregiver was exhausted and with anxious and/or depressive mood: “Insomnia, loss of appetite, ruminative thoughts, emotional lability,(…), previous bereavements still being experienced, caregiver burden,” I169, wife, primary caregiver.
“Caregiver burden” was both a title for a subcategory and a subcategory itself, considering 22 units of data were coded, specifically, as “caregiver burden” – e.g., “Signs of caregiver burnout,” I160, son, primary caregiver. Twelve references embodied family caregivers with a double-role of caring. They were responsible not only for a family member with cancer but also for another disabled person, or someone who is still dependent. We verified that this latter situation might have occurred more than what was informed, given that, from cases that reported age information – 43 cases –, around 35% of caregivers were between 41 and 60 years old. This is a period of life in which people usually either have already had children or start to have family members with persistent health issues: “She also cares for her 94-year-old mother as well as her son with autism,” I188, sister, primary caregiver.
Finally, with 37 coded references, the distress subcategory expressed family caregivers’ suffering throughout the process of caring for a loved one. Here, the authors tried to reflect the anguish, the sorrow, and grief. These feelings could be expressed both explicitly and implicitly. The following is an example of a plain expression of distress: “Cognitions and feelings that cause [her] distress and suffering,” I162, daughter, primary caregiver. Distress led some caregivers to have difficulty accepting the condition of illness, to adopt maladaptive coping strategies, or to have unrealistic expectations about the illness and its progression. We interpreted that the most frequent consequence of distress was the difficulty accepting the present situation. Some appeared to be struggling with the impending loss; others were just having trouble accepting the harsh reality – “Son with difficulty accepting the finiteness of life and the progression of the [father’s] illness,” I210, son, primary caregiver. For instance, sometimes after being informed by the clinical team, family members seemed hopeful that there might be a positive outcome in the situation, namely the recovery of the patient or another experimental treatment that could be attempted. This could be an obstacle in the sense that it might hinder important family conversations or unfinished business as the example shows: “[Husband] with unrealistic expectations of the patient’s clinical condition, despite having been informed of the terminal phase of the disease,” I241, husband, primary caregiver.
Intra-family’s aftershock of the Illness
Cancer has consequences that impair family and individual dynamics, relation-wise (e.g., communication) and at a more personal and customized level (e.g., how do I experience my family member’s illness?). At first, caring every day for a relative or a close friend could be related to their own personal health – e.g., “Patient [the caregiver] on dialysis,” I211, wife, primary caregiver.
Authors understood that there were psychoeducational and practical needs that family caregivers have throughout the course of the illness, particularly during the terminal stage – e.g., “There is a need to receive practical guidance on day-to-day care tasks (e.g., managing therapy, transfers and placements),” I187, friend, primary caregiver. An example is the perceived need for information concerning social benefits and rights, the reasons for hospitalization in a PC service, or even on how to help other family members cope with the end-of-life situation. It can be an additional challenge if family caregivers are not completely aware of what their family member is going through, which are their rights – and obligations – and how they can help more fragile relatives to cope with the present – “Family’s lack of information about adequate social benefits” [reported by social services], I15.
In the end-of-life, the conflict dimension is central. Here, a caregiver was identified as having a “complex relationship with the patient” (I116, partner/ex-wife, primary caregiver) stemming from a “conflicted” divorce, which was also identified as “intra-family conflict.”
The illness’s progression has a great power on the emotional state of each person in the family system, including the patient him/herself. Therefore, the “difficulty coping with recent behavioral changes” (I141, wife, daughter, primary caregivers) can be evident, or the caregiver might report that they are having a hard time “dealing with the [family member’s] situation” (I27, wife, primary caregiver). The so-called “conspiracy of silence” is one example of an inappropriate strategy to deal with what is happening: “Does not know diagnosis” [but the family does], I129.
And if there are vulnerabilities in the family’s network?
As a result of the illness, there is a greater need for support and for establishing a safety net. Nevertheless, the complexity of the illness impairs many families, both on emotional – “psychosocial support” – and socioeconomic level. On the other hand, current family conditions (e.g., geographic distance between family members) impact the family’s ability to help. This category shows the authors’ findings on some vulnerabilities that might weaken the whole system.
There can be socioeconomic and cultural constraints (n = 7) experienced over the course of the terminal phase of the illness (e.g., “Poor financial and cultural resources,” I255), emphasizing gaps in terms of family and social support.
At last, authors identified five references focused on family caregivers’ skills to care for the cancer patient. There could be a case where health professionals perceive some powerlessness in reaching this goal: “Unable to care for his wife,” I166, husband, primary caregiver. Or, as one file indicated, a person might feel his/her caregiver does not have the competence to provide care, which, in this case, made professionals report a parent–child conflict: “Thinks his son doesn’t have the skills to be a caregiver” [a patient about his caregiver, his son] (I126).
Discussion
The present qualitative study aimed to examine the main obstacles family caregivers have throughout the terminal phase of their loved ones’ battle with cancer. However, this work only allowed to ascertain the ones that were either reported to professionals or noted by them and, thus, written in each patient’s files.
Caregiver burden: It is not only a category, it is real
Not surprisingly, family caregivers mentioned in these files appeared to present high levels of psychological morbidity and caregiver burden. As a result of the daily toll, time-consuming tasks, family impact of the illness, and other illness-related variables, they appeared to be at greater risk for stress, depression, and anxiety symptoms (Reblin et al. Reference Reblin, Baucom and Clayton2019) during this terminal stage of the loved one’s illness. With its progression, there are physical symptoms reported by the patients (e.g., pain, nausea, anorexia), which promote greater changes in family roles and negatively impact the whole system’s quality of life (Given et al. Reference Given, Given and Kozachik2001). The latter is also associated with the functional dependence in terms of daily activities, which underscores the time-consuming aspect of the caregiving role, and from which can result poor physical and psychological health and burden (Nicholas Dionne-Odom et al. Reference Nicholas Dionne-Odom, Taylor and Rocque2018).
The significant levels of psychological morbidity (Areia et al. 2017) with the scarcity of interventions with the family unit and/or focused on family caregivers (Oliveira et al. Reference Oliveira, Fonseca and Areia2022b) perpetuates the inadequacy of care provided to the ones who care. Furthermore, compared with non-caregivers, people involved in high levels of care often lack enough rest (Given et al. Reference Given, Given and Kozachik2001), pay less attention to their own health, and few allocate time to do activities that give them pleasure.
Is there such a thing as “too much communication”?
In line with previous literature concerning caregivers’ opinions (Areia et al. 2017; Given et al. Reference Given, Given and Kozachik2001), health professionals believe that family caregivers consider receiving information in several domains (i.e., practical, medical, social) as extremely valuable to cope with a chronic condition. Our findings sustained that the lack of information was seen as an obstacle. Therefore, information about the illness and about the resources which the family can turn to (Given et al. Reference Given, Given and Kozachik2001), such as the community or the health system are key to satisfy caregivers’ needs and to reduce their emotional distress, empowering them to deal with daily challenges.
Facing the emotional, physical, and/or spiritual suffering and imminent death of a loved one could be a distressing experience. Our analysis showed that, for some, dealing with “the illness’s progression” might be challenging, mostly if the family does not have all the information to deal with it. That is why helping families to approach the illness as a shared battle and providing psychoeducation that not only informs but also normalizes challenges and emotions (Rolland Reference Rolland2005) could minimize caregiver burden and malfunctioning family dynamics.
Effective communication within the family is vital “for family mastery of the illness” (Rolland Reference Rolland2018: 85), and in opposition, blocked communication boosts anxiety (Rolland Reference Rolland1999). In fact, in families with less conflict, caregivers appear to report less burden (Northouse et al. Reference Northouse, Katapodi and Schafenacker2012). Thus, clinicians ought to try to stop this chain of relational patterns, understanding each family’s cultural norms and history of loss and illness in the family (Rolland Reference Rolland2018), helping them get over secrecy, shame, or guilt, and building mutual support along the way (Walsh Reference Walsh2016a).
When the personal social network is Pathogenic
The outcomes of this family crisis on the family and social network and lack of adequate competence to care were the most perceived obstacles related to the vulnerabilities of the family network. These results emphasize the importance of the support and resources available throughout this period. As Sluzki (Reference Sluzki2010) stated, an unreliable or impaired social network might contribute to higher morbidity and mortality, and poorer rehabilitation related to an array of diseases. In fact, when illness strikes, an active and “healthy” network is vital to promote a “virtuous” cycle (Sluzki Reference Sluzki2010) of support (e.g., practical and emotional), to meet information-related needs about the patient, the illness, and social benefits, and to avoid the social and emotional isolation of the family. In opposition, our findings raised the suspicion of a not-that-infrequent “pathogenic” cycle (Sluzki Reference Sluzki2010) where an inadequate social network contributes negatively to the family coping strategies.
Who takes care?
The most common constellation of caregivers was 1 (n = 55) or 2 (n = 42) primary caregivers (Table 2). This meant that in most cases, cancer patients had 1 or 2 people as the primary individual(s) responsible for their daily care. According to the literature (e.g., Rolland Reference Rolland2018), we might suggest that it could be more beneficial for the whole family to try to share caring responsibilities for more people, avoiding the exhaustion of someone. Nonetheless, it is understandable that there might be some obstacles, such as physical/geographic distance, personal health issues, family norms that sustain who is expected to provide the caregiving, or others.
In line with Eurocarers/IRCCS-INRCA (2021), it was usually the spouse/partner or the child who cared for these cancer patients, followed by the siblings. From the total number of mentioned caregivers, 62.5% were female, although 16.4% of the files did not have all these information. Our study is in line with the literature regarding gender roles among the caregiving task and its continued prevalence nowadays (Walsh Reference Walsh2016b). The Covid-19 pandemic emphasized the aforementioned, given that women were more prone to renounce their work life to care for children and/or family members during lockdown (Tavares et al. Reference Tavares, Malta and Fabrizio2020).
Based on the information we have, most family caregivers are between 40 and 60 years old. Thus, they are likely to be experiencing their own health issues as well, shown by some of our reports, which they often ignore (Jansen et al. Reference Jansen, Dauphin and De Burghgraeve2021), given their 24/7 attention to their ill relative.
Strengths and limitations
The present study gathered data from 2 institutions whose ways of reporting the information and collecting it were different, as well as its storage. In addition, these were in 2 distinct regions of the country – North and Central Region – which, presumably, influences their personnel.
This kind of document analysis provides information about a sensitive topic, without creating reactivity in its process (Bowen Reference Bowen2009), which is an important advantage. Its findings, together with the successive qualitative studies we are currently conducting (focus-group studies, as previously mentioned), are expected to provide valuable information about the experience (and its recognition) of family caregivers of cancer patients receiving PC, in particular, their obstacles during this terminal stage. Furthermore, it allowed us to grasp the way the referred PC units work, which is important when thinking about a way to intervene in these contexts. Furthermore, we analyzed health professionals’ written notes, which mean we had access to the insights of those who care for the caregivers about obstacles during the terminal phase of one’s illness. To the best of our knowledge, here is where the major novelty of our study lies.
This study is not without limitations. Despite the richness that comes from the qualitative analysis of written files, these might be skewed both by the perception and interpretation of the person who writes them – the health professionals – and, above all, by the willingness of caregivers to freely express their feelings and frustrations or difficulties. Moreover, these files refer to a period of pandemic, which modified the professionals–caregivers’ communication and created additional obstacles – e.g., the decrease in in-person contact and increased financial strain (Kent et al. Reference Kent, Ornstein and Dionne-Odom2020). The latter underlines the importance of being cautious when interpreting and generalizing these results. Even though we analyze files from institutions from 2 different places of the country, it would be important to have the same information from PC institutions from the South of Portugal, as well as from the Azores and Madeira. At last, sometimes, due to lack of time, opportunity, or knowledge, no information about some important aspects was provided, so our analysis is only based on what is written, which highlights the need to be careful when generalizing these results.
Conclusion
As expected, caregiver burden, distress, psychological morbidity, emotional lability, anxiety, and others were some of the key words/expressions identified in the current analysis. Moreover, juggling personal, professional, and “caregiver” identities is a struggle, considering how Lightfoot and Moone’s (Reference Lightfoot and Moone2020) conclusions state that, on average, informal caregiving takes up around 20 hours a week. Taking the latter into account, this study could work as a guideline pointing to which key aspects caregivers struggle with and want to see addressed. It is vital to care for this burdened population and its network – not seldom pathogenic – experiencing the aftershock of the illness.
Acknowledgments
I wish to acknowledge Inês Sousa, MS, for her comments and suggestions for this paper.
Funding
This research was supported by a PhD scholarship (2020.06575.BD) from the Portuguese Foundation for Science and Technology (FCT) to the first author.
Competing interests
None.








