Despite substantial declines in the rate of smoking over several decades to a current general population prevalence of approximately 15% (Australian Institute of Health and Welfare [AIHW] 2011), tobacco smoking remains the largest single cause of preventable death and disease in Australia (AIHW, 2011). Opportunistic smoking cessation intervention during routine clinical encounters with a range of health professionals has the potential to reach the majority of smokers, and can be effective (An et al., Reference An, Foldes, Alesci, Bluhm, Bland, Davern and Manley2008; Edwards et al., Reference Edwards, Freeman and Roche2006; Fiore et al., Reference Fiore, Jaen, Baker, Bailey, Benowitz, Curry and Wewers2008; Rice & Stead, Reference Rice and Stead2002; Zwar & Richmond, Reference Zwar and Richmond2006). As a consequence, the World Health Organisation (WHO) and peak bodies for a range of health professions such as general medical practitioners and oral health professionals, recommend that health professionals provide cessation intervention routinely and systematically to all smokers (FDI/WHO, Reference Beaglehole and Benzian2005; Royal Australian College of General Practitioners; RACGP, 2005; WHO, 2001; WHO, 2003). The value of all health professionals providing smoking cessation intervention is reinforced by findings which suggest that interventions by more than one type of health professional have the potential to substantially increase quitting and readiness to quit in the smoking population (An et al., Reference An, Foldes, Alesci, Bluhm, Bland, Davern and Manley2008).
Behavioural health providers such as psychologists seem especially well-suited to provide smoking cessation intervention for a multitude of reasons (Akpanudo et al., Reference Akpanudo, Price, Jordan, Khuder and Price2009; Wetter et al., Reference Wetter, Fiore, Gritz, Lando, Stitzer, Hasselblad and Baker1998; Williams & Ziedonis, Reference Williams and Ziedonis2004). Nicotine dependence is recognised as a substance use disorder by the Diagnostic and Statistical Manual of Mental Disorders, (DSM-IV; American Psychiatric Association, 1994), and is often co-morbid with other psychological disorders with which patients are likely to present to psychologists (Access Economics, 2007; Australian Bureau of Statistics, 2010; Morissette et al., Reference Morissette, Tull, Gulliver, Kamholz and Zimering2007). Determining smoking status and nicotine dependence may often be clinically relevant to the treatment of presenting ‘psychological’ problems (Morissette et al., Reference Morissette, Tull, Gulliver, Kamholz and Zimering2007). Psychologists might be expected to have the knowledge and the skills to intervene effectively, with expertise in techniques such as cognitive behavioural therapy (Paul & Lucas, Reference Paul and Lucas2005), and be in a better position to intervene than many other health professionals as they often have longer and more frequent sessions with clients. People with mental illnesses who smoke are likely to smoke more and be more highly dependent than smokers in general and so might be anticipated to require more intensive support to quit (Access Economics, 2007; Williams & Ziedonis, Reference Williams and Ziedonis2004). Further, a meta-analysis examining the effect of type of provider on the effectiveness of smoking cessation intervention found that while interventions delivered by a range of health professionals were effective, intervention by psychologists was more likely to be effective than that delivered by any of the other health professional groups such as physicians and nurses (Mojica et al., Reference Mojica, Suttorp, Sherman, Morton, Roth, Maglione and Shekelle2004).
Despite the potential of psychologists, and the existence of comprehensive evidence-based guidelines for providing smoking cessation intervention that might be adopted in psychological practice (Fiore et al., Reference Fiore, Jaen, Baker, Bailey, Benowitz, Curry and Wewers2008; Zwar et al., Reference Zwar, Richmond, Borland, Stillman and Cunningham2005), research suggests that psychologists do not routinely assess the smoking status of their clients (Akpanudo et al., Reference Akpanudo, Price, Jordan, Khuder and Price2009; Leffingwell & Babitzke, Reference Leffingwell and Babitzke2006; Phillips & Brandon, Reference Phillips and Brandon2004) let alone offer opportunistic smoking cessation intervention (Akpanudo et al., Reference Akpanudo, Price, Jordan, Khuder and Price2009; Hjalmarson & Saljoojee, Reference Hjalmarson and Saloojee2005; Phillips & Brandon, Reference Phillips and Brandon2004). Two studies undertaken in the US, suggest that intervention for smoking seems less likely to occur than intervention for the use of other substances such as alcohol and illicit drug abuse (Phillips & Brandon, Reference Phillips and Brandon2004) and other health risk behaviours, such as unsafe sex, reckless driving, gambling and lack of physical activity (Phillips & Brandon, Reference Phillips and Brandon2004; Wendt, Reference Wendt2005).
Potential barriers to the provision of smoking cessation intervention by psychologists have been reported to include: lack of training, lack of time, perceived costs of cessation intervention for the therapeutic relationship, perception that smoking cessation intervention is not a psychologists’ responsibility or role, and beliefs that clients are uninterested or will be unreceptive to intervention (Akpanudo et al., Reference Akpanudo, Price, Jordan, Khuder and Price2009; Fiore et al., Reference Fiore, Jaen, Baker, Bailey, Benowitz, Curry and Wewers2008; Leffingwell & Babitzke, Reference Leffingwell and Babitzke2006; Phillips & Brandon, Reference Phillips and Brandon2004; Wetter et al., Reference Wetter, Fiore, Gritz, Lando, Stitzer, Hasselblad and Baker1998).
To date, there has been no research on the provision of smoking cessation intervention by Australian psychologists, nor the barriers to providing such care. The primary aim of the current exploratory study was to assess the prevalence of smoking assessment and cessation intervention provided by Australian psychologists, and to identify possible barriers to their provision of smoking intervention. Further, the study sought to compare psychologists’ perceptions regarding the provision of smoking cessation interventions with their perceptions regarding the provision of interventions for other health risk behaviours.
Methods
Study design and participants
A cross-sectional survey was undertaken, utilising a self-administered questionnaire. Eligible participants were psychologists in one region of New South Wales, Australia, whose work involved clinical contact with clients, identified through membership of the local branch of the Australian Psychological Society (APS) (n = 122), and/or through employment within the local health service (n = 150).
Procedure
Participants were contacted by email, with the assistance of the local branch of the APS and the Director of Psychology for the local health service, and provided with a study information sheet and invitation to participate in the study. The survey could be completed either on-line or as a hard copy.
Measures
The survey questionnaire was created with reference to those used by other researchers (Phillips & Brandon, Reference Phillips and Brandon2004; Wendt, Reference Wendt2005). Respondents were asked to report their gender, age, smoking status, sector of practice, number of years practicing as a psychologist, highest qualification, estimated percentage of clients who smoke, training in smoking cessation care (recency and context of previous training received), and interest in future training.
To assess the usual provision of smoking interventions where smoking was not the client's presenting problem, participants were asked to indicate how many of their clients they usually assessed for smoking status (‘None or Almost None’, ‘Some’, ‘About Half’, ‘Most’, ‘All, Nearly All’), and how many identified smokers they usually provided a range of smoking cessation interventions to (‘None or Almost None’, ‘Some’, ‘About Half’, ‘Most’, ‘All or Nearly All’; Table 2).
To assess perceived barriers to the provision of such interventions, participants were asked to indicate their extent of agreement or disagreement with a list of possible barrier statements using a four-point Likert scale format (Strongly Agree to Strongly Disagree; Table 3).
To assess likelihood of assessing smoking status relative to assessing client status of other health risk behaviours (lack of exercise, alcohol use, methamphetamine ‘ice’ and cannabis), participants were asked to rate (1 [low] to 4 [high]) their likelihood of detecting a patient's risk status where the risk behaviour was not the client's presenting problem. For smoking and each of the other risk behaviours, participants were also asked to rate (1 [low] to 5 [high]) their perceptions of their: role in providing an intervention; likelihood of providing such intervention; confidence/competence in providing such interventions; and likelihood of referring a client elsewhere for further care.
Statistical analyses
Simple proportions are used to describe the characteristics of the sample, the provision of smoking cessation intervention, and barriers to the provision of such care. Repeated measures ANOVA and simple effects analyses were conducted to assess differences between risk behaviours in ratings for: perceived role to intervene, likelihood of intervening, confidence/competence in intervening, and likelihood of referring elsewhere intervention.
Results
Sample description
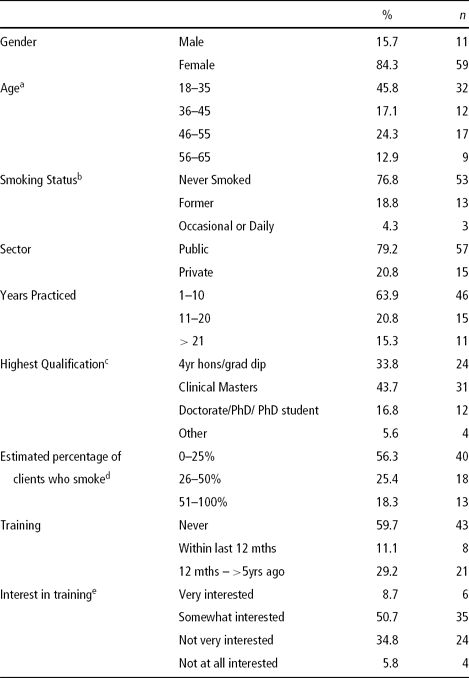
The recruitment email was sent to 150 health service psychologists, and 122 members of the local branch of the APS. Completed surveys were received from 72 psychologists. Most participants (71%) chose to complete the survey online. Table 1 illustrates demographic information and sample descriptors. Nearly half of the participants were aged 18 to 35, most were female, and 4.3% were current smokers. Most of the participants worked in the public sector (79.2%), and the mean length of practice as a psychologist was 11 years (SD = 8.65). The mean proportion of clients estimated to be smokers was 32.6% (SD = 28.57), although a majority of participants (56.3%) indicated that less than 25% of their clients smoked. The majority of participants (59.7%) had not received formal training in smoking cessation intervention, and 11% had received training in the past 12 months. For those who had received some training, it had most commonly occurred within postgraduate coursework (32.1%). More than half of all participants were either ‘very’ or ‘somewhat’ interested in receiving training, with only 5.8% ‘not at all interested’. Three participants indicated having no clients over the age of 18 years or estimated that less than 1% of their clients were smokers, and hence were excluded from further analysis, leaving a sample of 69.
Table 1 Sample Characteristics

a 2 missing
b 3 missing
c 1 missing
d 1 missing
e 3 missing
Assessment of smoking status
Less than half of participants (42.0%) reported asking the smoking status of ‘All or Nearly All’ of their clients. One-quarter (24.6%) reported assessing smoking status for ‘None or Almost None’ of their clients; with 17.4% reporting doing so for ‘Some’; 5.8% for ‘About Half’ and 10.1% for ‘Most’.
Provision of smoking cessation intervention
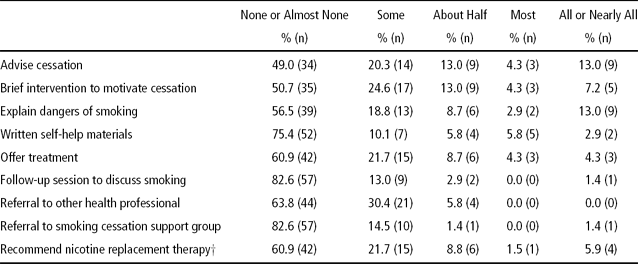
For each of eleven types of intervention considered, the most common response (given by between 49.0% and 82.6% of participants) was that intervention was provided to ‘None or Almost None’ of their smoking clients (Table 2).
Table 2 Frequency of Responses for Intervention Items: “With how many of your clients who smoke do you do the following?”

All N = 69, apart from † N = 68.
Approximately 50% of the participants were unlikely to provide even the simplest and briefest levels of intervention, to ‘advise cessation’ or to provide ‘brief intervention to motivate cessation’. Levels of referral to another health professional or to a smoking cessation support group were also very low: a majority of participants indicating a response of ‘None or Almost None’ for both of these items.
Barriers to provision of smoking cessation intervention
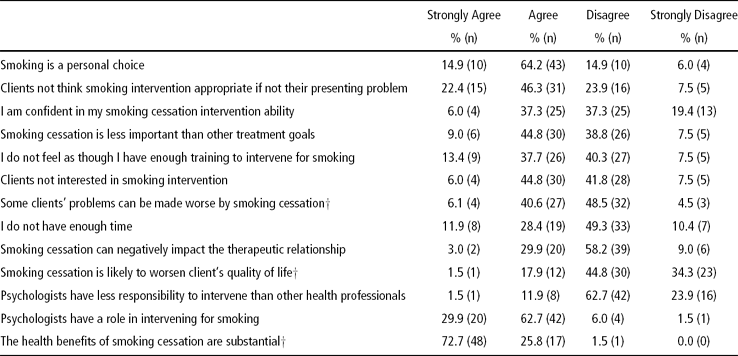
Reponses to the possible barrier items are reported in Table 3. The majority of participants agreed that smoking is a personal choice, and that clients would not think it appropriate for them to intervene if smoking were not the client's presenting problem. More than half of participants reported a lack of confidence in their smoking cessation intervention ability, agreed that smoking cessation was less important than other treatment goals, felt they did not have enough training to intervene, and agreed that clients were not interested in smoking intervention.
Table 3 Frequency of Responses to Barriers Items

All N = 67, apart from †N = 66.
On a more positive note, the majority of participants acknowledged the substantial health benefits of smoking cessation, did not feel that smoking cessation is likely to worsen the client's quality of life, or negatively impact the therapeutic relationship. Most participants agreed that psychologists have a role in intervening for smoking (30% ‘Strongly’ agreeing), and did not feel that psychologists have less responsibility to intervene for smoking than do other health professionals.
Clinician perceptions of intervention for smoking relative to other health risk behaviours
In comparing mean ratings of the likelihood of identifying smoking as compared with doing so for the use of other substances (alcohol, methamphetamine, ice and cannabis) and lack of physical activity, alcohol use was most likely to be identified (M = 3.57, SD = .58), followed by cannabis (M = 3.43, SD = .76), ice (M = 3.36, SD = .81), smoking (M = 3.21, SD = .86), and lack of physical activity (M = 3.09, SD = .83). Smoking status was significantly less likely to be identified than alcohol consumption status (F(1, 66) = 18.07, p <.001).
In comparing smoking and the other ‘health risk behaviours’ with respect to ‘clinician perceptions’ of ‘role’ to intervene, ‘likelihood of intervening’ ‘confidence’ to intervene, and ‘likelihood of referring’, ANOVA analyses indicated a significant effect of ‘health risk behaviour’ (Wilk's L = 0.51, F(4,62) = 14.85, p<.001), and a significant ‘clinician perceptions’-by-’health risk behaviour’ interaction effect (Wilk's L = 0.420, F(12,54) = 6.21, p<.001). Smoking had the lowest mean score, indicating that participants were overall less willing to provide any type of intervention for clients who were smokers than for those who engaged in the other health risk behaviours. Exploration of the significant interaction indicated that the mean for role to intervene for smoking (see Figure 1) was significantly lower than the mean role rating for all the other health risk behaviours (all p<.001). Likelihood of providing intervention was lower for smoking than for each other health risk behaviour, and significantly so for alcohol (t(65) = −4.47, p<.001) and exercise (t(65) = −6.01, p<.001). The mean rating for confidence to intervene for smoking was lower than all health risk behaviours, other than ice, and significantly lower for alcohol (t(66) = −5.38, p<.001), and for exercise (t(66) = −2.73, p = .008). The mean likelihood of referring was significantly lower for smoking than for alcohol (t(66) = −2.76, p = .007), ice (t(66) = −5.43, p<.001), and cannabis (t(66) = −3.27, p = .002), and significantly higher for smoking than for exercise (t(66) = 3.71, p<.001).

Figure 1 Clinician perceptions of intervention for smoking relative to other health risk behaviours.
Discussion
Less than half (42%) of the psychologists participating in this survey reported that they assessed smoking status for ‘All or Nearly All’ of their clients. A quarter of the sample reported that they assessed smoking status for ‘None or Almost None’ of their clients. These results suggest that there is no possibility of either smoking cessation assistance being provided directly by their treating psychologist or of referral elsewhere for a large proportion of smokers, as their status as a smoker is not established.
The reported level of smoking cessation intervention provided was very low, with the most common response to every type of intervention listed being that it was provided to ‘None or Almost None’ of a psychologist's clients, with up to 80% of responses in this category for some interventions. Where intervention was reported to occur, it was clearly for a very small proportion of the very few clients identified to be smokers. Additionally, the responses of participants who said they provided intervention indicated that the most common form of intervention was the most minimal; suggesting that smokers who received intervention nevertheless had little likelihood of achieving cessation.
Recent literature has suggested that given barriers such as limited time and competing priorities, it may be more realistic for clinicians to be encouraged to at least refer elsewhere to ensure more patients receive appropriate preventive care (Glasgow et al., Reference Glasgow, Goldstein, Ockene and Pronk2004; Laws et al., Reference Laws, Kemp, Harris, Davies, Williams and Eames-Brown2009; Ministry of Health, 2007). Such logic might well be applied to the role of psychologists in providing smoking cessation intervention. The results of the present study however would suggest that referral of smokers elsewhere for treatment is currently no more likely to occur than active intervention delivered by the psychologist, and hence that a significant shift in psychological practice would be required to effect even this level of care provision.
Less than half of participants reported receiving any training in smoking cessation (40.3%), with most training having been completed during postgraduate studies. The majority of participants indicated that they were interested in receiving training for smoking cessation intervention, mirrored by over half who perceived that their current training was insufficient. Hence, training psychologists in how to carry out brief opportunistic intervention could be an effective and acceptable approach to increasing smoking cessation intervention: at least as an important first step. The WHO recommends that all health professionals be trained to advise and help smokers stop smoking, and that education and training start at the undergraduate level and continue on through clinical training (WHO, 2001; WHO, 2003). Evidence from a range of health professional training programmes suggests that relatively brief training can have an impact (Borelli et al., Reference Borelli, Lee and Novak2008; Sheffer et al., Reference Sheffer, Barone and Anders2009; Maynard et al., Reference Maynard, Metcalf and Hance2012). To provide further training for health professionals such as psychologists following the completion of formal university education, it may be important to explore flexible forms of delivery, such as tele-health, videoconferencing and on-line formats (Mitchell et al., Reference Mitchell, Hawkshaw, Naylor, Soewido and Sanders2008; Maynard et al., Reference Maynard, Metcalf and Hance2012). To our knowledge, there has been no investigation of the smoking cessation training which might be feasibly, acceptably and cost-effectively provided to psychologists, in Australia or elsewhere.
While most participants in the present study agreed smoking cessation intervention to be part of their role as a psychologist and psychologists to have as much responsibility to intervene as do other health professionals, such statements of acceptance were contradicted by self-reported practice and other apparent beliefs. As has been found in surveys of mental health professionals in other contexts (Wye et al., Reference Wye, Bowman, Wiggers, Baker, Carr, Terry, Knight and Clancy2009; Wye et al., Reference Wye, Bowman, Wiggers, Baker, Knight, Carr, Terry and Clancy2010) this study identified a concern about the receptivity of clients to smoking cessation intervention, although such concerns are not likely to be well-founded (Conroy et al., Reference Conroy, Majchrzak, Regan, Silverman, Schneider and Rigotti2005; Fiore et al., Reference Fiore, Jaen, Baker, Bailey, Benowitz, Curry and Wewers2008; Moeller-Saxone, Reference Moeller-Saxone2008). Training and education for psychologists may assist in dispelling some of the myths and misperceptions around the desire and need of smokers for assistance to quit, as well as reinforcing smoking as a legitimate clinical concern and cessation as a treatment goal of high priority.
The extent to which smoking cessation intervention is absent from psychological care provision is highlighted further by comparing psychologists’ smoking-related treatment beliefs and practices with those pertaining to other health risk behaviours. Generally, psychologists reported being less likely to detect smoking, having less of a professional role to intervene, less confidence in doing so and were also less likely to refer with respect to smoking than the other health risk behaviours investigated. The findings support those of a number of previous studies indicating smoking care to be less likely to be provided by psychologists than care for other health risk behaviours and substance use (Phillips & Brandon, Reference Phillips and Brandon2004; Wendt, Reference Wendt2005).
The apparent reluctance of psychologists to address smoking relative to other behaviours is mirrored among other health professional groups, such as general practitioners (Degenhardt et al., Reference Degenhardt, Knox, Barker, Britt and Shakeshaft2006; Vogt et al., Reference Vogt, Hall and Marteau2005). Smoking, unfortunately, seems to hold a special place with respect to a reluctance by health care professionals to see it as appropriate or possible to successfully intervene. Undoubtedly, the reasons are complex and deserving of greater research attention. Most certainly, a number of misperceptions about smoking need to be dispelled so that it is seen as an addiction requiring the same clinical care as other addictions.
This study was conducted as an initial exploration of Australian psychologists’ attitudes and practices regarding smoking care. It's low response rate, although comparable to previous similar studies (Leffingwell & Babitzke, Reference Leffingwell and Babitzke2006; Wendt, Reference Wendt2005), and limited geographical coverage limit the confidence with which the findings can be generalised. The study sample likely over-represents younger psychologists, who may be speculated to have been exposed to more training in regards to smoking cessation, and non-smokers. It is likely that those who responded were more favourably disposed to the provision of smoking cessation care, suggesting that the observed findings may in fact reflect an overestimate of smoking intervention. (Some overlap in membership of the health service psychologist group and those who were members of the local APS branch is acknowledged, but unfortunately not possible to quantify: hence, the calculated response rate of 26% – which assumes no overlap between the two sampling frames – is a conservative estimate.)
The low levels of smoking intervention and referral indicated by this study, and the implicit negative consequences for the well-being of the client group concerned, supports the need for further research to explore barriers to smoking cessation care provision by Australian psychologists and the development of strategies for increasing such care. A change in culture and more positive perception amongst psychologists of the importance of providing opportunistic, preventive care for smoking is needed. Smoking needs to be viewed as a legitimate part of clinical care provision, as a drug dependency, and ultimately, to be as important as other therapeutic agendas.
There are no Australian guidelines for smoking cessation intervention specifically for psychologists and the Australian Psychological Society does not appear to have a stance on smoking cessation, nor actively encourage its members to provide opportunistic smoking cessation care. The same need for systems approaches to the provision of smoking care within health care settings generally (Fiore et al., Reference Fiore, Keller and Curry2007) can be argued to apply to psychological practice. A shift in perspective needs to occur both within the profession and also at government level for real changes to occur. Current Medicare arrangements serve to send messages down-playing the importance of psychologists providing smoking cessation treatment, and to set smoking apart as not so deserving or in need of clinical care and psychological expertise as other substances of abuse. Whilst psychological treatments for other licit and illicit drugs are now eligible for a Medicare rebate, treatment for ‘tobacco use disorder’ remains almost exclusively, ineligible (Department of Health & Aging [DoHA], 2011).
Acknowledgements
The authors wish to acknowledge the contributions of Prof Don Munro and Mr Wayne Levick for their assistance in facilitating survey administration, and Mr Kim Colyvas for statistical advice. Additionally, the authors are grateful to those psychologists who gave of their time to complete the survey.
Financial Support
Funding support was provided by the School of Psychology, University of Newcastle.
Conflicts of Interest Statement
None.
Ethical Standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki declaration of 1974, as revised in 2008.