Introduction
Obstructive sleep apnoea (OSA) is a common disorder, with an estimated prevalence of 9 per cent in women and 24 per cent in men who are aged 30–60 years old.Reference Young, Palta, Dempsey, Skatrud, Weber and Badr1 Treatment of OSA in the 1960s to early 1980s consisted of tracheostomies, which dramatically decreased apnoea indices, oxygen desaturation levels, sleepiness and mortality.Reference Camacho, Certal, Brietzke, Holty, Guilleminault and Capasso2 In 1981, Sullivan et al. developed continuous positive airway pressure (CPAP) therapy,Reference Sullivan, Issa, Berthon-Jones and Eves3 which is as efficacious as tracheostomies; however, the effectiveness is limited as 46–83 per cent of patients do not adhere to CPAP use in the long term.Reference Weaver and Grunstein4
Alternative therapies are often sought by patients who cannot tolerate CPAP. Alternatives include mandibular advancement devices, positional therapy, weight loss, bariatric surgery and upper airway surgical procedures.Reference Powell, Riley, Guilleminault and Troell5–Reference Sarkhosh, Switzer, El-Hadi, Birch, Shi and Karmali8 Nasal trumpets (also known as nasopharyngeal airway tubes or stents) are devices that are placed into the nares. The devices extend into the nasopharyngeal or oropharyngeal airway spaces, while the flared component of the tube rests externally against the nostril.Reference Beattie9 Nasal trumpets are sometimes used by emergency care professionals for patients with facial burns or airway compromise who are awaiting tracheostomy or intubation.Reference Thompson and Frable10, Reference Bajaj, Gadepalli and Knight11 The advantages of using nasal trumpets is that they are generally easily inserted in sedated patients or in patients during emergency situations. However, caution is required as insertion is contraindicated in patients with severe head or facial injuries, as the devices could traverse skull base defects and enter into brain tissue.Reference Schade, Borzotta and Michaels12
The use of nasal trumpets as treatment for sleep-disordered breathing was initially reported by Walsh and colleagues in 1972 without polysomnographic data,Reference Walsh, Michaelson, Harkleroad, Zighelboim and Sackner13 and then by Guilleminault and colleagues in 1975 with polysomnographic data.Reference Guilleminault, Eldridge, Simmon and Dement14 In the latter study, four patients were evaluated pre- and post-insertion; three patients had no improvement in OSA and the fourth had a 10 per cent reduction in obstructive apnoeas. In 1981, Afzelius and colleagues described two patients with severe OSA (40.8 and 51.3 apnoeas per hour per night, respectively) and excessive hypersomnia.Reference Afzelius, Elmqvist, Hougaard, Laurin, Nilsson and Risberg15 There was complete cessation of OSA in these patients after the insertion of size 30–32 French nasal trumpets, with polysomnography demonstrating no apnoeas; in addition, there was resolution of the patients’ hypersomnia.
Nasopharyngeal obturators, which are modified mandibular advancement devices, have also been utilised to move the soft palate forward and stent open the nasopharyngeal airway.Reference Venkat, Gopichander and Vasantakumar16, Reference DeAngelo and Mysliwiec17
This article aimed to systematically review outcomes in adult OSA patients who are treated with nasopharyngeal airway stenting devices (i.e. nasal trumpets and modified mandibular advancement devices).
Materials and methods
All procedures contributing to this work complied with ethical standards. As a systematic review of literature that has already been published, this article was exempt from review by Stanford University's Institutional Review Board.
Search strategy and literature selection criteria
A search of Medline, Scopus, Web of Science and the Cochrane Database of Systematic Reviews was performed from the date of each database inception to 1 June 2013, with an update on 10 January 2014. There were no Medical Subject Headings for ‘nasal trumpet’ or ‘nasopharyngeal obturator’, so the search was performed using the following combinations of key words: ‘nasal stent’, ‘nasal trumpet’, ‘nasopharyngeal trumpet’, ‘nasopharyngeal airway stent’, ‘nasopharyngeal airway tube’, ‘nasopharyngeal obturator’ or ‘nasopharyngeal tube’, in conjunction with and without the key word ‘sleep’.
We also reviewed the references in the articles retrieved, to identify additional relevant articles. In addition, the ‘cited by’ and ‘related citation’ features of the databases were utilised in an attempt to identify additional studies. To increase sensitivity, the search was not limited to OSA; rather, it encompassed sleep-disordered breathing as a broad category (snoring, upper airway resistance syndrome and sleep apnoea).
The inclusion criteria were: posters, abstracts, case reports, case series, literature reviews, systematic reviews and meta-analyses (written in any language) that reported the outcomes of adults using nasopharyngeal airway stenting devices. Studies that reported the findings of nasopharyngeal airway stenting devices used on children and studies that did not report outcomes for sleep-disordered breathing were excluded from the review.
In order to adequately analyse the data, the outcomes for nasopharyngeal airway stenting devices were sub-categorised into either nasal trumpet data or nasal obturator data. At least two studies were necessary in order to pool the data for meta-analysis. Nasal trumpet polysomnographic data were pooled for meta-analysis; however, there were an insufficient number of nasal obturator studies to perform a meta-analysis.
Data abstraction and study quality assessment
Two authors (AK and MC) independently screened titles and abstracts of the search results, and identified articles that met the inclusion and exclusion criteria. Patient data (i.e. age, sex and body mass index (BMI)) were collected. Pre- and post-intervention data were gathered, including: apnoea indices, apnoea–hypopnoea indices (AHIs), oxygen desaturation indices, Epworth Sleepiness Scale scores and lowest oxygen saturation levels. Reported complications and side effects associated with having nasopharyngeal airway stenting devices in position were also noted.
The National Institute for Health and Clinical Excellence (NICE) quality appraisal tool was utilised to assess the methodological quality of the studies included.18 This tool consists of an eight-item evaluation, for each case series. The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (‘PRISMA’) statement was followed during this study.Reference Moher, Liberati, Tetzlaff and Altman19
Statistical analyses
Statistical analyses were performed after the two authors had reviewed titles and abstracts, read full text versions of relevant articles, and come to a consensus regarding the final list of articles to be included in the review. Data were collected and evaluated using the Statistical Package for Social Sciences software, version 20.0 (IBM, Armonk, New York, USA), and the Cochrane Collaboration's Review Manager software, version 5.2.20
Means and 95 per cent confidence intervals (CIs) were used to compare the polysomnographic outcomes pre- and post-treatment. Pooled data excluded studies where: additional interventions (i.e. surgery) were also performed; there were fewer than two subjects; pre- and/or post-nasal trumpet intervention data were missing; or the standard deviation (SD) was 0 (a 0 value cannot be pooled for analysis). The mean differences and SDs before and after interventions were calculated. Statistical significance was defined by a p-value of less than 0.05. Heterogeneity was evaluated using Cochran's Q test. The IReference Camacho, Certal, Brietzke, Holty, Guilleminault and Capasso2 statistic was employed to evaluate inconsistency. A random effects model was used for analysing data.
Results
As an example, a search on Scopus (using the terms ‘nasal stent’, ‘nasal trumpet’, ‘nasopharyngeal trumpet’, ‘nasopharyngeal airway stent’, ‘nasopharyngeal airway tube’, ‘nasopharyngeal obturator’ or ‘nasopharyngeal tube’) on 10 January 2014 yielded 394 articles. The combined searches yielded a total of 573 different studies. The titles and abstracts of these were analysed by both search authors for potential inclusion.
Of all the studies identified, 80 were sleep related. After further evaluating the titles and abstracts, a total of 27 studies were considered potentially relevant. These were downloaded and retrieved for further evaluation. One Spanish study,Reference Bové Ribé, Vidal Marsal, Furquet García and Torre Alonso21 three German studiesReference Freuschle, Heiser, Maurer, Hörmann and Stuck22–Reference Juhasz24 and two Chinese studiesReference Huo, Li, Shen and Liu25, Reference Wang, Jiang, Dong, Liu, Deng and Liu26 were translated into English.
After reading each of the studies and their references, 2 additional articles were identified and retrieved, increasing the total number to 29 studies.
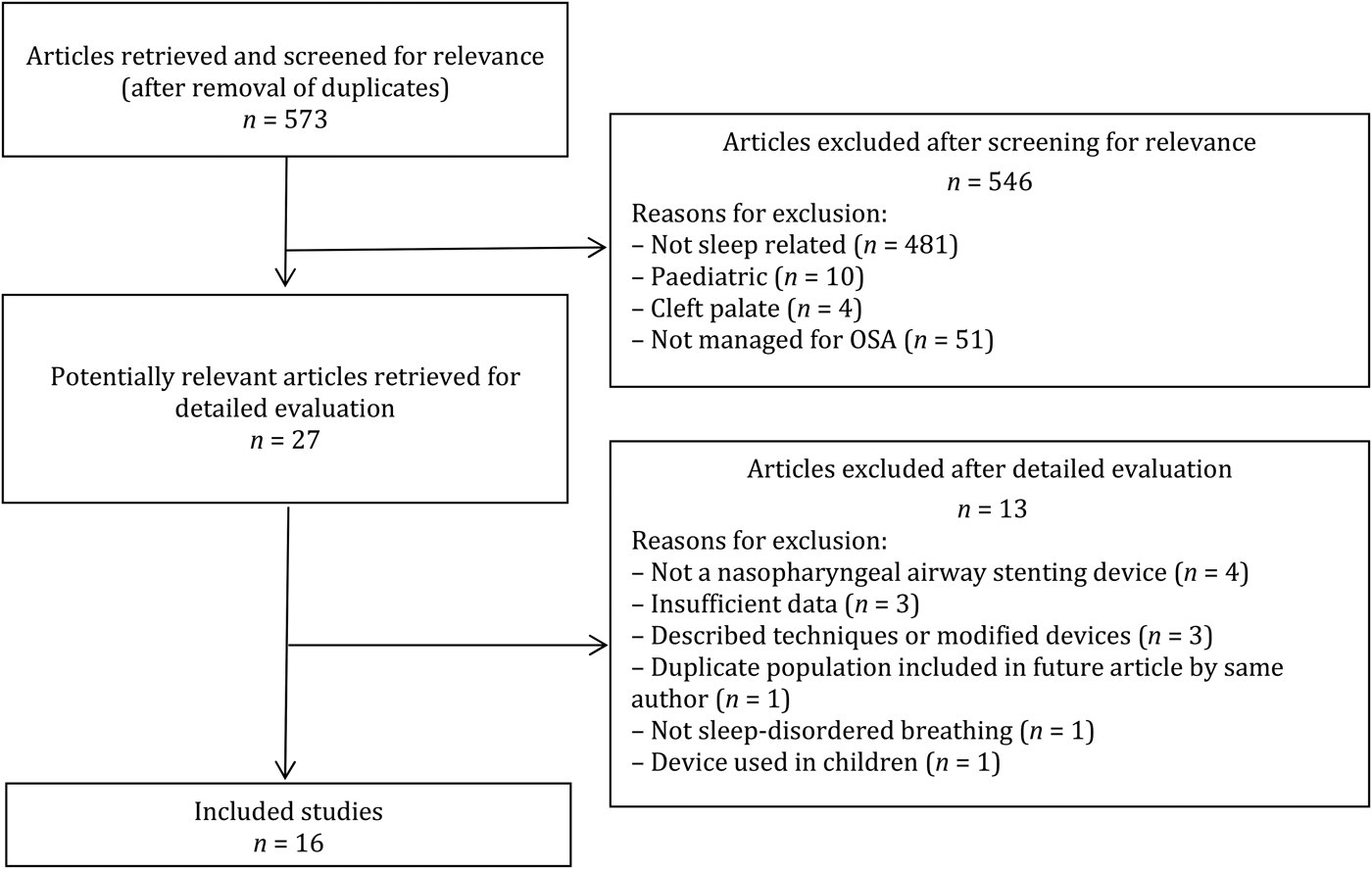
After final review of all the publications, a total of 16 of the 29 studies met the inclusion and exclusion criteria, and were analysed as part of this systematic literature review.Reference Walsh, Michaelson, Harkleroad, Zighelboim and Sackner13–Reference Weaver and Grunstein17, Reference Bové Ribé, Vidal Marsal, Furquet García and Torre Alonso21–Reference Remmers, deGroot, Sauerland and Anch31 The flow diagram for study selection is shown in Figure 1.

Fig. 1 Flow diagram for the literature search and overall study selection. OSA = obstructive sleep apnoea
Characteristics of eligible studies and methodological quality
The characteristics of the included studies are demonstrated in Table I. All studies were level 5 (case reports) or level 4 (case series) evidence. There were no multi-centre studies, randomised controlled trials, systematic reviews or meta-analyses.
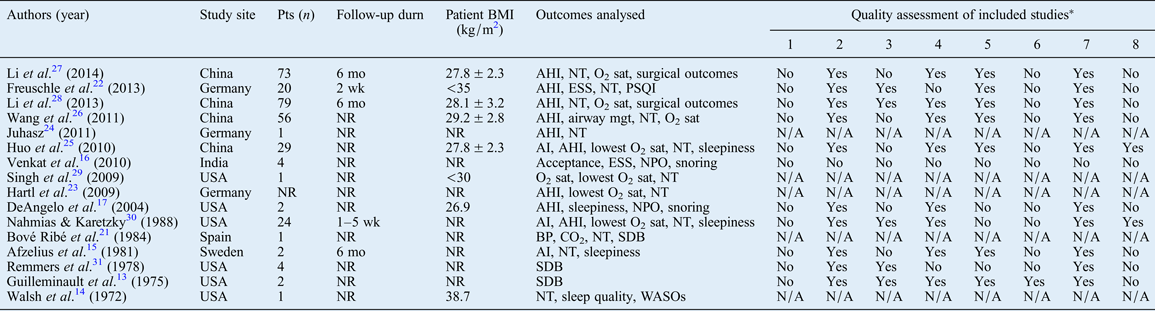
Table I General characteristics and quality assessment of included studies

* Responses to the quality assessment checklist for cases series studies from the National Institute for Health and Clinical Excellence,18 which involved evaluation of the following eight items: (1) Case series collected in more than one centre, i.e. multi-centre study? (2) Is the hypothesis, aim or objective of the study clearly described? (3) Are the inclusion and exclusion criteria (case definition) clearly reported? (4) Is a clear definition of the outcomes reported? (5) Were data collected prospectively? (6) Is there an explicit statement reporting that patients were recruited consecutively? (7) Are the main findings of the study clearly described? (8) Are outcomes stratified (e.g. by disease stage, abnormal test results or patient characteristics)? Pts = patients; durn = duration; BMI = body mass index; mo = months; AHI = apnoea–hypopnoea index; NT = nasal trumpet; O2 sat = oxygen saturation; wk = weeks; ESS = Epworth Sleepiness Scale; PSQI = Pittsburgh Sleep Quality Index; NR = not reported; mgt = management; N/A = not applicable; AI = apnoea index; NPO = nasopharyngeal obturator; BP = blood pressure; CO2 = carbon dioxide; SDB = sleep-disordered breathing; WASO = wake-up after sleep onset
The studies included in this review were evaluated with the NICE quality assessment tool, and were found to satisfy between zero and five of the eight items assessed. One case seriesReference Venkat, Gopichander and Vasantakumar16 did not meet any of the criteria evaluated, while most other studies met at least three of the characteristics and quality criteria evaluated. In general, the methodology of the included studies was limited by: lack of prospective, consecutive patient evaluation; lack of multi-institutional research; and a lack of clear outcome reporting and/or stratification.
Nasal trumpets
Bové Ribé et al. described a case in which a morbidly obese patient, who was observed to have a high (unspecified) number of apnoeas, experienced complete resolution of the events after being treated with a nasal trumpet.Reference Bové Ribé, Vidal Marsal, Furquet García and Torre Alonso21 Remmers et al. described four OSA patients who used nasal trumpets; this treatment eliminated the obstructive apnoeas and led to regular breathing during sleep.Reference Remmers, deGroot, Sauerland and Anch31 Guilleminault et al. reported outcomes for four OSA patients (two adults) who had a nasopharyngeal tube placed overnight; three of the patients experienced no decrease in the obstructive apnoeas during sleep and one patient experienced a 10 per cent decrease from baseline.Reference Guilleminault, Eldridge, Simmon and Dement14
In two separate articles, Li et al. described outcomes for OSA patients who underwent polysomnography pre- and post-nasal trumpet insertion to help determine if the patient had strictly oropharyngeal obstruction or oropharyngeal obstruction in combination with glossopharyngeal obstruction.Reference Li, Wu, Bao and Shi27, Reference Li, Wu, Bao and Shi28 The first study (79 patients) demonstrated respective pre- and post-nasal trumpet insertion AHI values of 43.4 ± 21.9 and 25.1 ± 21.3 episodes per hour.Reference Li, Wu, Bao and Shi28 The second study (73 patients) reported respective pre- and post-nasal trumpet insertion AHI values of 41.2 ± 17.3 and 22.0 ± 21.4 episodes per hour.Reference Li, Wu, Bao and Shi27 The two studies by Li et al. reported an overlap in time between June 2011 and December 2011. The corresponding author was contacted and the response was that there were 12 patients whose data overlapped. The overall combined outcome data were obtained for the 140 patients, which demonstrated pre- and post-nasal trumpet AHI values of 42.23 ± 20.21 and 22.78 ± 21.33 episodes per hour, and pre- and post-nasal trumpet lowest oxygen saturation levels of 65 ± 16 and 73 ± 15 per cent, respectively.Reference Li, Wu, Bao and Shi27, Reference Li, Wu, Bao and Shi28
Wang et al. compared polysomnographic outcome data for 56 patients with a nasopharyngeal airway stenting device versus 45 patients using an oropharyngeal stenting device post-operatively.Reference Wang, Jiang, Dong, Liu, Deng and Liu26 Polysomnography demonstrated that the AHI values for the nasopharyngeal airway stenting device patients decreased from 50.5 ± 6.8 to 2.2 ± 1.5 episodes per hour. There were no differences between the two study arms in terms of AHI or haemodynamic parameters; however, the nasopharyngeal airway stenting device was better tolerated than the oropharyngeal airway stenting device.Reference Wang, Jiang, Dong, Liu, Deng and Liu26
Huo et al. evaluated the feasibility and therapeutic effect of a nasopharyngeal airway stenting device for OSA, based on overnight polysomnography.Reference Huo, Li, Shen and Liu25 The authors found a decrease in AHI from 44.7 ± 16.0 to 14.6 ± 10.0 episodes per hour (p < 0.001). The lowest oxygen saturation level increased from 72.2 ± 0.08 to 86.1 ± 0.07 per cent (p < 0.001). Additionally, 91 per cent of the patients were able to tolerate the device overnight.Reference Huo, Li, Shen and Liu25
Singh et al. described a case in which a traumatic brain injured patient with co-morbid OSA, who was intolerant to CPAP therapy, was treated with a nasal trumpet.Reference Singh, Segal, Malone and Zubair29 While on room air, the patient's oxygen desaturation levels were below 89 per cent 23.1 times per hour, with a lowest oxygen saturation level of 60 per cent.Reference Singh, Segal, Malone and Zubair29 When the nasal trumpet was in position, the patient's oxygen desaturation levels were below 89 per cent 7.8 times per hour, with a lowest oxygen saturation level of 86 per cent.Reference Singh, Segal, Malone and Zubair29
Nahmias and Karetzky evaluated 44 OSA patients (mean age, 53 years); these patients had used a nasal trumpet at home for between 1 and 5 weeks.Reference Nahmias and Karetzky30 Of the 44 patients, only 24 were able to tolerate the therapy, and 16 agreed to undergo subsequent polysomnography. This revealed improvements in: apnoea index, from 40.1 to 14.8 episodes per hour (p < 0.0001); AHI, from 54.8 to 32.2 episodes per hour (p < 0.001); and lowest oxygen saturation level, from 68.7 per cent to 77.1 per cent (p < 0.005).Reference Nahmias and Karetzky30 Thirteen of the 16 patients (81 per cent) were able to use the nasal trumpet long term, with good compliance (patients were followed up for at least 4 months).Reference Nahmias and Karetzky30
Another study, by Afzelius et al., in which two patients were evaluated, demonstrated a reduction in apnoea index, from 46 to 0 episodes per hour.Reference Afzelius, Elmqvist, Hougaard, Laurin, Nilsson and Risberg15 The two patients used either a size 30 or 32 French nasal trumpet. They were taught how to apply topical anaesthesia and insert the devices. The patients were sent home with the nasal trumpets and used them for at least the duration of the follow up (six months). The authors reported no complications of epistaxis, stenosis of the nasal cavity, atrophic rhinitis or lipoid pneumonia (from the oil spray used daily).Reference Afzelius, Elmqvist, Hougaard, Laurin, Nilsson and Risberg15
Walsh et al. evaluated a 52-year-old man with a BMI of 46.8 kg/mReference Camacho, Certal, Brietzke, Holty, Guilleminault and Capasso2 and hypersomnia, with co-morbid congestive heart failure, dyspnoea, peripheral oedema and orthopnoea. Some OSA events lasted 30–60 seconds in this patient.Reference Walsh, Michaelson, Harkleroad, Zighelboim and Sackner13 The patient also experienced 10–20 wake-ups after sleep onset. Subsequent to using a nasal trumpet overnight, he reported feeling more rested than he had in many years.Reference Walsh, Michaelson, Harkleroad, Zighelboim and Sackner13 Despite the dramatic improvement, he declined ongoing therapy.Reference Walsh, Michaelson, Harkleroad, Zighelboim and Sackner13
A newer nasal trumpet modification is the AlaxoStent, which is a smooth, tubular, braided stent made out of nitinol (shape memory metal) that self-expands and stents the pharynx open.22–24 The first study describing the use of the stent was reported by Hartl et al. in a German congress publication (abstract form).Reference Hartl, Goderer, Schick and Iro23 In that report, an unspecified number of patients had a mean reduction in AHI from 31 to 19 episodes per hour. A case report was presented by Juhasz in poster form;Reference Juhasz24 this demonstrated a pre- versus post-nasal trumpet AHI reduction from 74 to 5 episodes per hour, and the patient tolerated the stent well. Freuschle et al. studied 22 patients with AlaxoStents; however, after using the nasal trumpets overnight, none of the patients were able to tolerate them enough to use them for the planned treatment duration of 14 days.Reference Freuschle, Heiser, Maurer, Hörmann and Stuck22
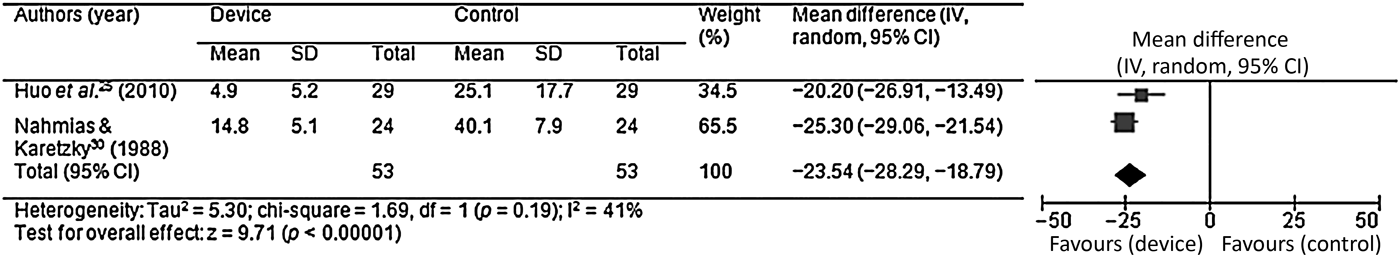
The polysomnographic summary data for patients using nasal trumpets as a treatment for OSA are demonstrated in Table II. Apnoea index values were reported for 55 patients (53 patients’ data could be pooled); this revealed a mean ± SD decrease (pre- vs post-nasal trumpet insertion) from 32.4 ± 15.9 to 9.0 ± 7.2 episodes per hour. The mean difference was −23.5 (95 per cent CI, −28.3 to −18.8), the z score was 9.7 and the p-value was <0.00001 (Figure 2).

Fig. 2 Pooled apnoea index data, demonstrating a mean difference of −23.5 (95 per cent confidence interval −28.29 to −18.79) (p < 0.00001). SD = standard deviation; IV = independent variable; CI = confidence interval; df = degrees of freedom
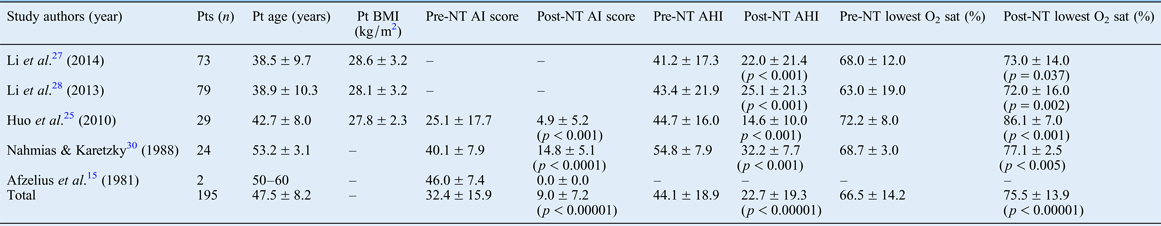
Table II Polysomnographic results for patients with nasal trumpets

Data represent mean ± standard deviation where indicated. Note: pooled data for the studies by Li et al. are based on outcomes for the 140 patients’ data (data in the 2 published studies overlapped for 12 patients). Pt = patient; BMI = body mass index; NT = nasal trumpet; AI = apnoea index; AHI = apnoea–hypopnoea index; O2 sat = oxygen saturation
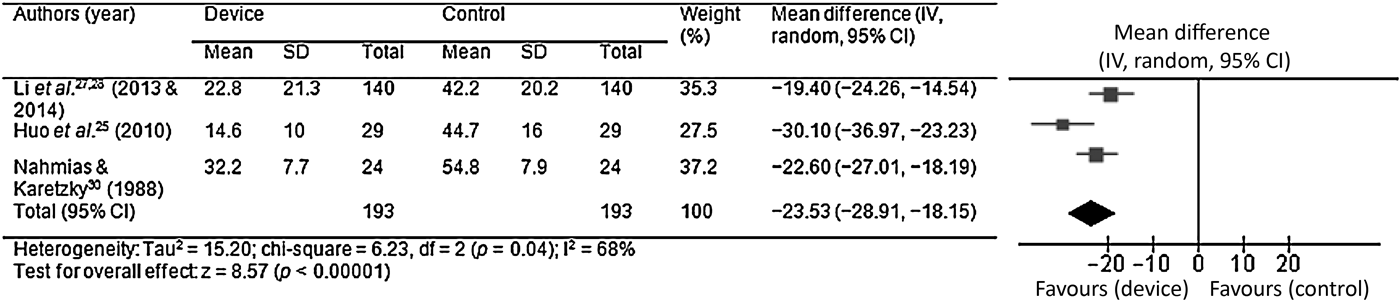
Apnoea–hypopnoea index values were reported for 193 patients. The calculated means ± SDs were 44.1 ± 18.9 episodes per hour pre-nasal trumpet insertion and 22.7 ± 19.3 episodes per hour post-nasal trumpet insertion. The AHI mean difference was −23.5 (95 per cent CI, −28.9 to −18.2), with an IReference Camacho, Certal, Brietzke, Holty, Guilleminault and Capasso2 value of 68 per cent, a z score of 8.57 and a p-value of <0.00001 (Figure 3).

Fig. 3 Pooled apnoea–hypopnoea index data, demonstrating a mean difference of −23.5 (95 per cent confidence interval −28.9 to −18.2) (p < 0.00001). SD = standard deviation; IV = independent variable; CI = confidence interval; df = degrees of freedom
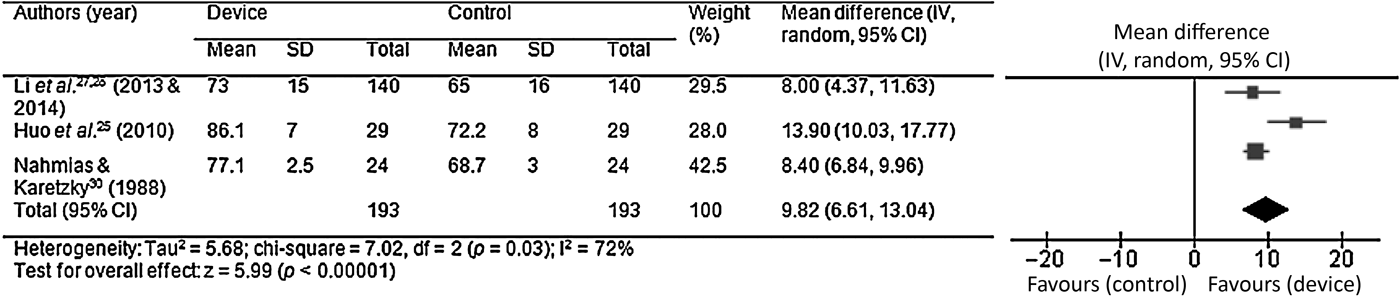
The lowest oxygen saturation levels were reported for 193 patients. This showed improvement from a mean ± SD of 66.5 ± 14.2 per cent pre-nasal trumpet insertion to 75.5 ± 13.9 per cent post-nasal trumpet insertion. The lowest oxygen saturation mean difference was 9.82 per cent (95 per cent CI, 6.6 to 13.0 per cent), with an IReference Camacho, Certal, Brietzke, Holty, Guilleminault and Capasso2 value of 72 per cent, z score of 6.0 and p-value of <0.00001 (Figure 4).

Fig. 4 Pooled lowest oxygen saturation data, demonstrating a mean difference of 9.82 per cent (95 per cent confidence interval 6.6 to 13.0) (p < 0.00001). SD = standard deviation; IV = independent variable; CI = confidence interval; df = degrees of freedom
Nasopharyngeal obturators
Venkat et al. described five prosthodontics devices, four of which had modifications to stent the nasopharyngeal airway.Reference Venkat, Gopichander and Vasantakumar16 The devices were described as: a uvula lift appliance, a uvula and velopharynx lift appliance, a nasopharyngeal aperture guard, and a soft palate lift appliance. The device which demonstrated the best treatment outcomes was the nasopharyngeal aperture guard.Reference Venkat, Gopichander and Vasantakumar16
DeAngelo and Mysliwiec reported two cases in which nasopharyngeal obturators were used to successfully treat OSA.Reference DeAngelo and Mysliwiec17 The first patient (a 31-year-old man with a BMI of 26.6 kg/mReference Camacho, Certal, Brietzke, Holty, Guilleminault and Capasso2) showed a post-treatment decrease in AHI from 46 to 5.7 episodes per hour.Reference DeAngelo and Mysliwiec17 The second patient (a 32-year-old man with a BMI of 27.2 kg/mReference Camacho, Certal, Brietzke, Holty, Guilleminault and Capasso2) showed a decrease in AHI from 57 to 4.7 episodes per hour.Reference DeAngelo and Mysliwiec17 Both patients had improvement in snoring and daytime somnolence.
Discussion
To our knowledge, this is the first systematic review of nasopharyngeal airway stenting devices used as a treatment modality for OSA. This study demonstrates mixed results for the use of such devices. The findings revealed tolerability and success in the immediate post-operative period (following OSA surgery), and in short-term use; however, data demonstrating generalised use in the long term are lacking. In the short term, polysomnographic data demonstrated a statistically significant improvement in outcomes. The mean ± SD for the pooled apnoea indices (53 patients) decreased from 32.4 ± 15.9 to 9.0 ± 7.2 episodes per hour (mean difference p-value of <0.00001). The mean ± SD for the AHI (193 patients) decreased from 44.1 ± 18.9 to 22.7 ± 19.3 episodes per hour (mean difference p-value of <0.00001). The mean ± SD for the lowest oxygen saturation levels (193 patients) increased from 66.5 ± 614.2 to 75.5 ± 13.9 per cent (mean difference p-value of <0.00001).
The stenting effect of nasal trumpets helps to prevent obstruction at the level of the nasopharynx. Depending on the length of the device and the anatomy of the patient, the nasal trumpets may also prevent obstruction at the level of the oropharynx. It has been noted that the soft palate has a wing-like shape; this causes the palate to lift upward into the nasopharynx when there is negative intranasal pressure, predisposing the patient to airway collapse.Reference Stupak32 Additionally, the outer nose itself is susceptible to Bernoulli's principle, as the negative intranasal pressure may induce collapse of the internal and external nasal valve in some patients. Therefore, an additional benefit of nasal trumpets in the short-term management of OSA may be the prevention or decreased risk of dynamic collapse as a result of stenting the internal and external nasal valve open. Nasal trumpets also improve airflow secondary to the decreased nasal resistance, as internal nasal cavity resistance is bypassed with the nasal trumpets present. However, studies have demonstrated that decreasing nasal resistance by performing isolated nasal surgery generally does not significantly improve polysomnographic outcomes in adult OSA.Reference Blakley and Mahowald33
Positioning of the nasal trumpet is important for effective therapy. Bajaj et al. noted that the tube length is more important than the width.Reference Bajaj, Gadepalli and Knight11 A study by Stoneham found that the ideal position for the distal tip of the nasopharyngeal airway is within 1 cm of the tip of the epiglottis; for most men this would be a length of 150 mm and for most women 130 mm.Reference Stoneham34 However, although these values are effective for most patients, the location of the distal end of the nasal trumpet can be unpredictable. It is generally recommended that the distal tip of the nasal trumpet protrude beyond the pharyngeal surface of the soft palate, but not past the epiglottis.Reference Gallagher, Pearce and Power35 Most of the articles in the literature do not report the length of the nasal trumpet, and long trumpets are usually not used in general practice.
The stiffness of the nasal trumpet is not described in the articles. This issue is analogous to that of the stiffness of tracheostomy tubes used as treatment for OSA. It is well known that the type of tracheostomy tube used has an impact on normal air exchange during sleep, and that tracheostomy tubes used in obese OSA patients with large necks must be long and rigid enough to allow for the maintenance of normal air exchange for treating sleep apnoea; however, they must also be comfortable enough to tolerate. Likewise, the comfort and tolerability of long-term nasal trumpet use has been a challenge; causes of patient discomfort and intolerance include a deviated nasal septum and/or turbinate hypertrophy. Such issues would need to be addressed either medically or surgically in order to facilitate the placement of nasal trumpets if patients desire to use them long term.
Nasopharyngeal obturators (modified mandibular advancement devices) should be produced by an experienced dentist. Proper positioning of these devices is essential to ensure patient comfort. Positioning may be verified by oral cavity, oropharyngeal, nasal cavity and nasopharyngeal examinations, which would involve nasopharyngoscopy by an otolaryngologist to confirm the proper relationship to the epiglottis. The data for nasopharyngeal obturators are significantly limited, with only one study reporting polysomnographic data, in two patients. More studies are needed before any generalisations can be made.
In general, medical management of OSA consists of CPAP as a first-line treatment. As many patients cannot use CPAP, alternative treatment options are often pursued. Second-line medical management may include mandibular advancement devices; however, there is a change in bite, particularly after months of use. Mandibular advancement devices also have contraindications that include: insufficient teeth; periodontal tooth disease, which induces mobility of the teeth; active temporomandibular joint pain disorder; and limited maximum protrusion of less than 6 mm.Reference Petit, Pepin, Bettega, Sadek, Raphael and Levy36 Surgery is sometimes considered in patients affected by these issues; however, many patients will continue to pursue additional medical management options. Alternative therapies include weight loss, positional therapy and head of bed elevation; however, none of these will have a significant impact on patients with moderate to severe OSA.
Nasopharyngeal airway stenting devices could be considered as an alternative therapy in the immediate post-operative period or on a temporary basis. Although Nahmias and Karetzky,Reference Nahmias and Karetzky30 and Afzelius et al.,Reference Afzelius, Elmqvist, Hougaard, Laurin, Nilsson and Risberg15 have demonstrated tolerability of nasal trumpets in the long term in several patients, there are an insufficient number of studies to generalise on their use in the long term. Some patients opt to use nasal CPAP at home and employ other portable, non-powered modalities while travelling. According to Nahmias and Karetzky, some patients have chosen to use nasal trumpets for these purposes; however, local trauma and consistency of usage findings are not reported.Reference Nahmias and Karetzky30
There are limitations to this study. First, despite our best attempts to identify all articles, without regard to language, it is possible there are additional studies that meet our inclusion and exclusion criteria, which were not identified during this review. Second, there are inherent limitations of the included studies in that they are either case reports or case series, which prevent us from reaching definitive conclusions. Third, there was heterogeneity among studies with regard to which patients are good candidates for nasopharyngeal airway stenting devices, and there were insufficient data reporting which factors can be used to predict a good candidate. We hypothesise that patients with small turbinates (grade 1)Reference Camacho, Zaghi, Certal, Abdullatif, Means and Acevedo37 and no nasal septal deviation are going to be more accepting of nasal trumpets than patients with nasal septal deviation and turbinate hypertrophy, as it will be more difficult for those latter patients to insert and tolerate the devices. However, this information was not reported in these studies.
Future research on nasal trumpets and other nasopharyngeal airway stenting devices used as a treatment modality for OSA could be performed in a manner that clearly describes: pre- and post-treatment nasal airway anatomy (i.e. the presence of nasal septal deviations and the size of the inferior turbinatesReference Camacho, Zaghi, Certal, Abdullatif, Means and Acevedo37), the frequency of nasal trumpet induced trauma, the effect of nasal trumpets on nasal mucosa with long-term usage, and outcomes of the Nasal Obstruction Symptom Evaluation (‘NOSE’) scale questionnaire.Reference Stewart, Witsell, Smith, Weaver, Yueh and Hannley38 Well-designed studies, such as randomised controlled trials, are needed, with extensive follow up and data collection.
Conclusion
There are mixed results for nasopharyngeal airway stenting devices used as a treatment for OSA. Some studies have demonstrated limited effectiveness and low tolerability, while others have shown a significant benefit in treating OSA with a high level of patient acceptance. Combined data demonstrate approximately a 50 per cent reduction in AHI values, a 72 per cent reduction in apnoea index values and a 9 per cent improvement in lowest oxygen saturation levels. Nasal trumpets have been successful in decreasing airway obstruction in the short term, such as when used immediately following OSA surgery. However, the type and length of nasal trumpet need to be confirmed to assure appropriate placement. Caution must be exercised during placement in order to minimise local trauma in the anaesthetised or sedated patient.