Introduction
By definition, any location which is 2700 m (9000 feet) or more above sea level is considered to be at high altitude. Many health problems hamper healthy human life at such elevations. However, the scientific literature lacks information on ENT morbidity associated with high altitudes.
This article presents a personal experience of ENT problems encountered at the highest multi-specialty hospital in the world, located at an altitude of 3600 m.
The atmospheric pressure at sea level is 1 Atmosphere. Above sea level, the atmospheric pressure decreases by 50 per cent for every increase of approximately 5400 m.Reference Farmer, Gillespie, Alberti and Ruben1 Thus, air has a lower density at high altitude because its component gases expand.
The response of gas to pressure changes also governs the behaviour of air in the middle ear and paranasal sinuses. During ascent, gas in the middle ear expands, whereas during descent the volume of gas decreases as the atmospheric pressure increases. During descent, the eustachian tube must be opened by swallowing movements to enable the middle-ear volume to be adjusted. If this mechanism fails or is delayed, increasing differential pressure acting on the soft nasopharyngeal end of the eustachian tube will close it. When this pressure becomes greater than that which can be generated by the tubal dilator muscles, the eustachian tube becomes ‘locked’. Thereafter, assuming descent continues, the pathological changes of otic barotrauma are inevitable. These changes affect the tympanic membrane and middle ear and are mainly vascular. They manifest clinically as tympanic membrane invagination, congestion along the handle of the malleus and in the attic, interstitial haemorrhage, middle-ear effusion, and tympanic membrane rupture.Reference Edward, Freeman, Thomas, Tonkin and Blackwood2
During descent, forceful coughing and sneezing, or production of an overpressure in the middle ear via performing the Valsalva manoeuvre, may cause sudden pressure transfer into the inner ear, causing inner-ear barotrauma.
Sinus barotrauma during descent is caused by obstruction of the ostium from the nasal side. If obstruction remains unrelieved and descent continues, the decreasing volume of air in the sinus exerts a suction effect on the lining mucosa, thus increasing ostium blockage. During ascent, the ostium may be blocked from within the sinus cavity. Symptoms are produced by unrelieved expansion of air contained in the closed bony sinus.Reference Benson, King and Wright3
The present study was conducted in the north Indian region of Ladakh, situated at high altitude in the state of Jammu and Kashmir. Ladakh shares its geographical boundary with Pakistan in the west and China in the east. The climate is extremely cold and dry, and the terrain lacks vegetation. Such extreme weather causes severe crusting of the upper airway mucosa. This leads to an unusually high incidence of epistaxis and pharyngitis, tracheostomy problems, and chilblain and frostbite of the nose and pinna.
Materials and methods
The present study was carried out from September 2005 to January 2008 in a garrison hospital located 3600 m above sea level. The ENT department evaluated deployed soldiers operating in various high altitude locations, from sparsely vegetated areas at 2700 m and cold deserts at 3000–4500 m to the icy heights of the Siachen glacier at 6900 m. All patients were male, of various ages. All soldiers had been medically examined prior to their induction into high altitude work and had been declared medically fit. Patients included soldiers new to high altitude service, those who had remained in the area for up to two years, and those returning to the area after lower altitude service.
Thirteen cases of otic barotrauma and 11 cases of sinus barotrauma were diagnosed. These cases were analysed for their presenting symptoms, clinical signs and predisposing factors. Treatment aimed to relieve pain and to maintain the ventilation of the middle ear and paranasal sinuses. Surgery was reserved for underlying nasal pathology and non-healing tympanic membrane perforations.
Three cases of sudden-onset vertigo during descent from altitude were evaluated. Otological monitoring comprised otoneurological testing and pure tone audiometry.
Twelve cases of high altitude cerebral oedema and nine cases of high altitude pulmonary oedema were treated in a hyperbaric chamber. As a precautionary measure, these patients were asked to evacuate their bladder and bowel and were taught the Valsalva manoeuvre. Nasal decongestant drops were instilled into the nose, drinking water was available inside the hyperbaric chamber to assist swallowing, and a nursing assistant stayed inside the chamber to monitor the patient's vital signs and oxygen saturation. The chamber was pressurised with air, and patients were given 100 per cent, pressurised oxygen via a face mask.
A total of 262 cases of epistaxis were evaluated with nasal endoscopic examination to determine their aetiology.
Forty-two cases of frostbite and 36 cases of chilblain were examined for head and neck involvement.
A large number of cases of chronic cough were seen in the hospital out-patient department. A careful clinical history excluded smoking, chronic infection, gastroesophageal reflux disease, angiotensin-converting enzyme medication, etc. Local causes in the throat were excluded by oropharyngeal examination and flexible fibre-optic laryngoscopy.
Results and analysis
Otic barotrauma
All 13 cases of otic barotrauma had no history of previous aural disease. Three patients were new to high altitude service, whereas 10 had returned to high altitude service after low altitude work. Nine cases were unilateral and four bilateral. All presented with acute earache, while six also complained of upper respiratory tract infection symptoms. Only three patients had tympanic membrane perforation on otoscopic examination at presentation (Table I).
Table I Otic barotrauma cases: otoscopic findings on presentation*
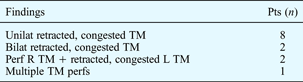
* Within 24 hours of arrival. Pts = patients; unilat = unilateral; TM = tympanic membrane; bilat = bilateral; perf = perforation; R = right; L = left
The majority of patients recovered with conservative treatment (Table II). All 13 cases had identifiable predisposing factors. Surgery was undertaken to treat the underlying nasal causes in six cases, to drain middle-ear effusion in one case and to repair tympanic membrane perforation in another. One patient was lost to follow up (Table III).
Table II Otic barotrauma patients: otoscopic findings after medical treatment

*Following active coryza treatment. †On 10th day; right tympanic membrane (TM) healed after four weeks. Pts = patients; OME = otitis media with effusion; HL = hearing loss; bilat = bilateral; perf = perforation; R = right
Table III Otic barotrauma patients: predisposing factors and treatment

*Successful. †Patient had multiple right tympanic membrane perforations. Pts = patients; DNS = deviated nasal septal; FESS = functional endoscopic sinus surgery
Sinus barotrauma
Of the 11 cases of sinus barotrauma, nine were unilateral and two bilateral. Two patients presented with frontal headache only. Nine patients had facial pain. All patients were assessed for predisposing factors, and most were treated surgically (Table IV).
Table IV Sinus barotrauma patients: predisposing factors and treatment

Pts = patients; DNS = deviated nasal septum; FESS = functional endoscopic sinus surgery
Vertigo
Three patients, all new to high altitude service, presented immediately upon arrival with acute-onset vertigo with no other aural symptoms. None of the three patients had nystagmus, and the fistula sign was negative. They were managed conservatively with bed rest, vasodilators, laxatives and otological monitoring. Clinical features resolved in three days.
Barotruma related to hyperbaric chamber therapy
Of the 21 patients treated in the hyperbaric chamber, three (14 per cent) suffered otic barotrauma.
Frostbite
Of the 78 cases of cold injury, six were found to have frostbite of the pinna. Both ears were affected in two cases. Prolonged contact of the pinna with the flaps of a wet cap was found to be the cause in all cases. Patients were treated with rapid re-warming in water heated to 40–42°C, aloe vera cream application, oral pentoxyphyllin 400 mg twice daily and oral aspirin 150 mg once daily.
High altitude pharyngitis
Sore throat and chronic cough were found to be nearly universal in any personnel who had spent some time at high altitude. These symptoms occurred without fever, chills, myalgia, lymphadenopathy, exudate, gastroesophageal reflux or any sign of infection.
Epistaxis
Of the 262 cases of epistaxis (comprising 8.7 per cent of total out-patient department attendance), 107 (41 per cent) were caused by nasal crusts and their dislodgement – a significant proportion (Table V). Commonly affected sites were Little's area, the septal spur and the anterior end of the inferior turbinate. All active bleeding was treated by chemical cautery.
Table V Epistaxis patients: aetiology

Pts = patients; DIC = disseminated intravascular coagulation
Discussion
Otic barotrauma
The development of otic barotrauma is dependent upon the rate of descent or the rate of ambient pressure increase, in contrast to the rate of middle-ear pressure increase. The latter is affected by the patency of the lumen and by the degree, frequency and duration of eustachian tube opening.Reference Dickson and King4 One episode of otic barotrauma can predispose an individual to further episodes, if the original predisposing factor persists, or if sufficient time has not been allowed for the original lesion to recover before the individual is exposed to further pressure changes.Reference Miller5
Sinus barotrauma
Humans can voluntarily control the ostium of the eustachian tube by swallowing, yawning, gaping, or performing the Valsalva or Frenzel manoeuvre, but have no such control over the ostia of sinuses. Sinus ostia may be occluded by a plug of mucus, mucosal oedema, polyp or mass. This obstruction is often valvular in nature, so that air passes easily in one direction only. Coryza, vasomotor rhinitis, allergic rhinitis and rhinosinusitis can also cause oedema of the nasal mucosa, which predisposes to sinus barotrauma. Nasal trauma and nasal septum deviations can also act in the same way.
Described in aviators by King in 1965, sinus barotrauma most commonly involves the frontal sinus.Reference King and Gilles6 In Fagan and colleagues' series of affected patients, there was a prior history of previous paranasal sinus barotrauma in one-third, and a history of recent upper respiratory tract infection or chronic nasal and sinus inflammatory disease in one-half.Reference Fagan, Mckensie and Edmonds7 None of these cases required surgery.
Inner-ear barotrauma
Goodhill stated in 1971 that an increase in intracranial pressure from coughing, sneezing or straining may cause sudden, spontaneous rupture of the round window.Reference Goodhill8 This same author also believed that a sudden change in middle-ear pressure may have the same effect during flight. Jones termed this ‘pressure vertigo’, and Lundgren ‘alternobaric vertigo’.Reference Jones9, Reference Lundgren10 Afflicted patients present with sudden deafness, tinnitus, and intense, short-lasting vertigo or ataxia. Otorhinolaryngological examination will reveal nystagmus and sensorineural hearing loss. Findings of decompression sickness, such as joint pain or central nervous system symptoms, will be conspicuously lacking.
It is postulated that this overpressure in the middle ear is not transmitted equally to the fluid system of the inner ear by the round and oval windows at the same time, and there may also be a mismatch between the left and the right ear.
However, in the present study none of the three vertigo cases had tinnitus or deafness. In the absence of nystagmus and the fistula sign, it was presumed that vertigo could have resulted from temporary vasospasm due to extremely cold weather.
Hyperbaric chamber therapy
At sea level, the atmospheric pressure is 1 Atmosphere; at 3600 m it is 0.6 Atmospheres. During hyperbaric chamber therapy, the rate of increase or decrease of pressure inside the chamber should not exceed 0.01 Atmospheres per minute. Therefore, in the present study it took 35 minutes to attain a pressure of 1 Atmosphere; this was then maintained for 6 hours. As patients breathe in oxygen under pressure, middle-ear ventilation is essential, otherwise otic barotrauma is inevitable.
Karhatay et al. assessed the development of otic barotrauma following hyperbaric chamber therapy, and reported a 66.7 per cent incidence, compared with incidences of 8–82 per cent published elsewhere.Reference Karhatay, Yilmaz, Birkent, Ay and Satar11 In the present study, 14 per cent of patients receiving hyperbaric chamber treatment developed otic barotrauma.
Tracheostomy problems
On the plains of India, the relative humidity varies between 60 and 99 per cent, whereas in Ladakh it ranges from 10 to 50 per cent, with an average of just 30 per cent. After tracheostomy, the tracheal mucosa has to be kept moist and humidified, otherwise there will be crusting, with the possibility of subsequent blockage and asphyxia. At high altitudes, saline nebulisation at frequent intervals keeps the respiratory tract moist, and early decannulation is advisable.
Epistaxis
Dry inspired air invariably causes crusting in the nose. As a result, epistaxis is a very common ENT problem at high altitude. Almost 100 per cent of the general population will experience minor nasal bleeding at some stage, but most will not seek ENT consultation. In Ladakh, as part of their health education, troops are advised to instil saline or glycerine nasal drops to keep the nasal mucosa moist and prevent crusting.
Cold injuries
The present study included patients exposed to temperatures varying from −5 to −50°C. Cold injuries result from the inability to properly protect oneself from exposure to cold. These injuries can be of two types: (Reference Farmer, Gillespie, Alberti and Ruben1) generalised (i.e. hypothermia) and (Reference Edward, Freeman, Thomas, Tonkin and Blackwood2) localised (i.e. chilblain and frostbite).
Chilblain comprises local swelling and tenderness after exposure to cold and moisture for 3–6 hours, and has little or no residual consequence. In contrast, frostbite involves the formation of ice crystals in tissues, along with denaturation of lipid-protein complexes, which may be followed by thrombosis, ischaemia and gangrene. The severity of frostbite depends on the temperature, length of exposure, wind chill factor and moisture level.
Cold injuries commonly affect the fingers and toes but can also affect the nose and ears. A common site in the head and neck region is the pinna (Figure 1).

Fig. 1 Frostbite of the pinna.
High altitude pharyngitis
The term ‘high altitude pharyngitis’ is suggested because of the present study's finding of a high incidence of chronic cough in individuals living in a high altitude location, which could not be attributed to any other cause. Hypoxia and hypobaria at high altitude demand extra breathing effort. The increase in ventilation forces obligate mouth-breathing, bypassing the warming and moisturising action of the nasal mucous membrane and sinuses. It is suggested that the movement of large amounts of cold, dry air across the pharyngeal mucosa causes marked dehydration, irritation and pain, similar to pharyngitis. Vasomotor rhinitis, which is quite common at cold temperatures, aggravates this condition by necessitating mouth-breathing during sleep.
• This study documented ENT morbidity in military personnel serving at high altitude
• Factors producing morbidity at high altitude include hypoxia, hypobaria, extreme cold, low humidity and hypercoagulability
• Particular ENT problems include frostbite, epistaxis, and barotrauma of the ear and sinuses
• Many high altitude ENT problems are preventable
Cases of high altitude pharyngitis were successfully treated by steam inhalation, forced hydration, throat lozenges and saline nasal drops.
Conclusion
Analysis of ENT morbidity encountered at high altitude reveals three types of disease: (Reference Farmer, Gillespie, Alberti and Ruben1) life-threatening diseases such as high altitude pulmonary oedema, high altitude cerebral oedema and deep vein thrombosis; (Reference Edward, Freeman, Thomas, Tonkin and Blackwood2) limb-threatening diseases such as chilblain and frostbite; and (Reference Benson, King and Wright3) other diseases, including the ENT ailments detailed above (Table VI). Epistaxis is so common that it is accepted as part of life, until one suffers a severe case. Pharyngitis is bothersome but does not prevent soldiers from carrying out their duties. Barotrauma has not gained a place amongst the notifiable diseases of high altitude, not only because of less awareness of this problem, but also because the majority of cases go unreported. In Ladakh, the medical treatment given by Regimental Medical Officers to soldiers suffering barotrauma is simple yet effective, and recovery is good with few residual consequences; hence, referral to an ENT specialist is infrequent.
Table VI Ent morbidity at high altitude: distribution*

* Patients treated September 2005 to January 2008.
These ENT problems are preventable if those at risk are aware. Hence, individuals living and working in high altitude areas should be educated about the possible ENT problems they face, and how to avoid them.









