To the Editor—Over the past decade, the prevalence of antibiotic resistance has increased alarmingly worldwide, prompting the General Assembly of the United Nations to label this problem as the greatest threat to human health, sustainable development, and security. Latin American countries are largely affected by antibiotic resistance, which has not only persisted but spread, mainly due to mobile genetic elements carrying several resistance determinants.Reference Escandón-Vargas, Reyes, Gutiérrez and Villegas 1 Antimicrobial stewardship (AMS) and infection prevention are complementary, multidisciplinary approaches for curbing bacterial resistance.Reference Goff, Kullar and Goldstein 2
In Colombia, AMS programs have had a positive impact on optimizing antibiotic use, reducing resistance trends and even saving healthcare costs.Reference Goff, Kullar and Goldstein 2 – Reference Hernández-Gómez, Pallares and Escandón-Vargas 4 Locally developed antibiotic guidelines, based on epidemiological surveillance and clinical studies, assist healthcare providers in clinical decision making, thereby mitigating the overuse and misuse of antibiotics. To the best of our knowledge, no studies have addressed the degree to which healthcare providers in Colombia adhere to antibiotic guidelines when prescribing antibiotics to treat existing infectious disease.
As an initial step toward the assessment of adherence to antibiotic prescribing guidelines in a Colombian hospital, we present our preliminary findings from a prospective study conducted in a tertiary care hospital in Cali, Colombia. In this study, we aimed to determine the clinical and economic outcomes associated with adherence to antibiotic guidelines for treatment of complicated urinary tract infection (cUTI) in the emergency department (ED). These guidelines had been carefully implemented in the ED, and risk factors for multidrug-resistant bacteria and patient stratification by infection severity were also considered. Between January and August 2016, a total of 80 adult patients with cUTI were included in the study and were followed until the completion of their antibiotic regimens. Of those patients, 54 (68%) were empirically treated with an antibiotic regimen that adhered to the guidelines. Interestingly, no statistically significant differences in rates of adherence between specialists and general practitioners involved in the antibiotic prescription were detected (P=.42). When adherent and nonadherent groups were compared (Table 1), clinical complications, change of antibiotic regimen after culture report, and higher costs of laboratory tests and imaging were factors associated with nonadherence to the antibiotic guidelines.
TABLE 1 Clinical and Economic Outcomes in Patients with Complicated Urinary Tract Infection (n=80)
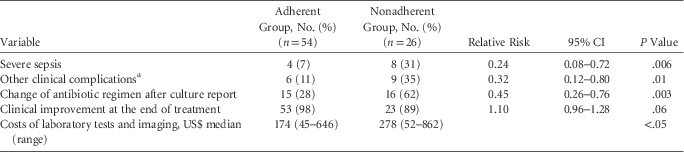
NOTE. CI, confidence interval; RR, relative risk.
a Complications: bacteremia, septic shock, multiple organ dysfunction syndrome, renal failure.
Overall, our findings demonstrate that both clinical and economic outcomes are significantly better for patients treated for cUTI in the ED according to antibiotic guideline recommendations. The adherence rate found in this study (68%) indicates a need for actions to increase compliance to antibiotic prescribing practices to an optimal level. Several barriers to physician adherence to clinical practice or AMS guidelines have been described in the literature, ranging from knowledge-related barriers (lack of familiarity or awareness) to attitude- and behavior-related barriers (lack of agreement, motivation, or outcome expectancy).Reference Cabana, Rand and Powe 5 , Reference Goldstein, Goff and Reeve 6 Such barriers should be addressed with tailored strategies. As a limitation, our study did not explore why healthcare providers did not follow antibiotic guidelines. Future studies aimed at elucidating barriers and strategies related to prescriber adherence to antibiotic guidelines in hospital settings in Colombia would serve as a cornerstone for driving AMS interventions.
Because there are no reports of adherence to therapeutic antibiotic guidelines published elsewhere in the country, our findings represent an initial measure in Colombia; antibiotic prescribing practices should be monitored and improved. Many other healthcare institutions might also have room for improvement. Based on this framework, we posit that cultivating an understanding of healthcare providers’ adherence to antibiotic prescribing guidelines is essential for identifying education and stewardship opportunities in hospital settings. Therefore, we encourage the development of new studies in the field of hospital epidemiology to investigate this health problem.
ACKNOWLEDGMENTS
Financial support: This work was supported in part by Merck Sharp and Dohme. The funders had no role in study design, data collection, statistical analysis, decision to publish or preparation of the manuscript.
Potential conflicts of interest: The authors report no conflicts of interest relevant to this article.



