Introduction
Tuberculosis (TB) is one of the leading causes of death from an infectious disease in the world (World Health Organization, 2018) and the third highest contributor to disability adjusted life years (DALYS) in Ethiopia (GBD 2016 DALYS and HALE Collaborators, 2017). Timely diagnosis and correct treatment cure most people who develop TB (World Health Organization, 2016). Delayed diagnosis leads to more severe clinical presentations (Virenfeldt et al., Reference Virenfeldt, Rudolf, Camara, Furtado, Gomes, Aaby, Petersen and Wejse2014), longer duration of infectivity and poorer prognosis. Rapid diagnosis is essential in order to decrease the incidence rate of TB (Friedland, Reference Friedland2011) to the extent required to meet the Global End-TB target by the year 2030 (10% decrease/year) (World Health Organization, 2015). Delayed diagnosis of TB has been found to be associated with HIV status, residence, geographical or socio-psychological barriers, health care provider contacted upon seeing symptoms, type of TB, age, sex, substance use, level of education, and stigma (Storla et al., Reference Storla, Yimer and Bjune2008). Many of these variables are known to be associated with depression in people with TB (Ambaw et al., Reference Ambaw, Mayston, Hanlon and Alem2017); but the impact of co-morbid depression on diagnostic delay has not been investigated (Storla et al., Reference Storla, Yimer and Bjune2008).
Co-morbid depression, a common disorder in people with TB (Trenton & Currier, Reference Trenton and Currier2001; Doherty et al., Reference Doherty, Kelly, Mcdonald, O'Dywer, Keane and Cooney2013; Sweetland et al., Reference Sweetland, Oquendo, Wickramaratne, Weissman and Wainberg2014; Sweetland et al., Reference Sweetland, Kritski, Oquendo, Sublette, Norcini Pala, Silva, Karpati, Silva, Moraes, Silva and Wainberg2017, Reference Sweetland, Jaramillo, Wainberg, Chowdhary, Oquendo, Medina-Marino and Dua2018), may negatively affect timely diagnosis and service utilization (Sweetland et al., Reference Sweetland, Jaramillo, Wainberg, Chowdhary, Oquendo, Medina-Marino and Dua2018). People with depression are known to have poor service utilization even in high-income settings (Andrews et al., Reference Andrews, Issakidis and Carter2001; Oliver et al., Reference Oliver, Pearson, Coe and Gunnell2005). Depression is associated with reduced energy levels, impaired concentration and memory, low motivation and hopelessness (Katon, Reference Katon2011). Co-morbid depression could also obscure recognition of TB symptoms because of the overlap of symptoms of depression with physical illnesses (Pachi et al., Reference Pachi, Bratis, Moussas and Tselebis2013) and predominantly vague somatic presentation of depression (Keely et al., Reference Keely, Nutting, Dickinson and Rost2004). Impaired uptake of health education messages may also lead to more indirect pathways to TB care (e.g. via traditional and religious healing), which in turn has been shown to result in diagnostic delay (Finnie et al., Reference Finnie, Khoza, van den Borne, Mabunda, Abotchie and Mullen2011).
The aim of this study was to assess the association between depression and diagnosis delay, pathways to TB care, and its role in mediating the association between diagnosis delay and the known risk factors in people with TB. Our hypotheses were as follows:
(1) Co-morbid depression will be associated with delayed diagnosis in people with TB and may be a mediator of the effects of known risk factors for diagnostic delay.
(2) Co-morbid depression in people with TB will interfere with effective help-seeking and greater use of indirect pathways to care.
Methods
Design
We analyzed cross-sectional data focusing on time to TB diagnosis, pathways to TB care, and depression from the baseline of our cohort study investigating the impact of co-morbid depression on TB outcomes in primary care settings in Ethiopia. In that cohort study, adults with newly diagnosed TB were recruited at the time of initiating Directly Observed Treatment Short-Course (DOTS) and followed up to the end of treatment (6 months after initiation). Data were collected at three time-points: baseline (before anti-TB treatment), at 2 months (end of intensive phase) and at 6 months (end of continuation phase). The exposure variable was depression. The primary outcome variable was TB treatment outcomes (treatment complete, cure, treatment failure, treatment default, or death). Secondary outcome variables were quality of life, disability, and pathways to TB care. Control variables included socio-demographic variables, substance use, perceived social support, perceived cause of TB, perceived barriers to modern TB care, stigma related to TB, and perceived severity of TB (Ambaw et al., Reference Ambaw, Mayston, Hanlon and Alem2015).
Study setting
The study was conducted from December 2014 to July 2016 in 14 primary care centres in South central Ethiopia (the Silti and Gurage zones) and northern Ethiopia (Bahir Dar zone). Two of the primary care centres were hospitals and 12 were health centres. Similar TB services were provided at the different types of facility: providers of TB care were nurses or public health officers, the same treatment guidelines and medications were used, and only outpatients were included. The frontline nurses and public health officers working in those primary care centres had received training in the management of mental disorders according to the evidence-based WHO Mental health gap action programme intervention guide (mhGAP-IG) for mental, neurological and substance use disorders in non-specialized health care settings (WHO, 2016).
Eligibility criteria
• People attending the selected health centres for TB treatment who were within 1 month of starting anti-TB treatment
• Aged 18 years and above
• Did not have plan to move out of the study area
• Not too ill to be interviewed at baseline as perceived by the interviewer or the prospective participant
• Were not admitted to in-patient unit for more than 5 days in the last 1 month as the additional stressors of being hospitalized represent a different range of risk factors for depression.
• Did not have Multidrug-Resistant Tuberculosis (MDR-TB); people with MDR-TB constitute a different population because their treatment and outcomes are different (more toxic medications for a much longer duration and poorer prognosis) and MDR-TB is a more feared and stigmatized condition (Vega et al., Reference Vega, Sweetland, Acha, Castillo, Guerra, Smith Fawzi and Shin2004). Furthermore, only one of the study health facilities had recently started a service for people with MDR-TB.
• Were not on re-treatment for TB as people who experienced previous treatment failures are at high risk of MDR-TB and constitute a different risk group for depression.
Sample size determination
The sample size was based on the primary objective of the longitudinal study which was to examine the effect of depression on default from anti-TB treatment (Ambaw et al., Reference Ambaw, Mayston, Hanlon and Alem2015). The following parameters were used in that calculation: 80% power, 95% confidence level, 2.5% prevalence of treatment default among patients with TB and without depression, 7.5% prevalence of treatment default among people with TB and co-morbid depression, a ratio of 2:1 of non-exposed (not depressed) to exposed (depressed) participants. This provided a required sample size of 639. With a contingency of 10% (64) for possible loss to follow up, the target sample was 703 people with TB. However, only 657 people with newly diagnosed TB were recruited into the study because of the scarcity of cases that meet our selection criteria (Ambaw et al., Reference Ambaw, Mayston, Hanlon and Alem2017). Because one of the required variables, stigma, was measured at 2 months of follow up, 65 (25 transferred out of study area, 22 died, nine diagnoses changed, six lost to follow up, and three refused to participate in the second month) of the 657 participants did not have value for it (Ambaw et al., Reference Ambaw, Mayston, Hanlon, Medhin and Alem2018). Therefore, we analyzed data from the remaining 592 participants who had complete responses for the variables of interest for this study.
Recruitment and ethics
People with newly diagnosed TB who fulfilled the inclusion criteria were identified, informed and invited to participate in the study by health professionals running TB clinics at the health facilities. When the individuals expressed interest to participate, they were linked to trained nurse research assistants who provided them detail information, sought written informed consent or witnessed thumb print, and carried out the data collection generally at the health facilities. The information provided to participants was explained face-to-face and delivered in written form to participants. The proposal was approved by the Institutional Review Board of College of Health Sciences of Addis Ababa University (number 027/14/Psy) before data collection. In the process of data collection, respondents who endorsed the suicide item of PHQ-9 were referred to health workers within the health facilities for further evaluation and treatment.
Dependent variables
Diagnostic delay
Diagnostic delay was defined as the time interval between the onset of TB symptoms and diagnosis of TB (Belay et al., Reference Belay, Bjune, Ameni and Abebe2012). Participants were asked ‘how long did your TB symptoms last before your illness was diagnosed as TB?’ In this study, the diagnosis was considered to be ‘delayed’ if the interval between the onset of symptoms and the date of diagnosis was above 12 weeks. Because there was no standard definition for diagnosis delay, the median of the sample scores (12 weeks) was used as a cut off value to operationally define the variable. A systematic review had found out that previous quantitative studies commonly used the median split to define delay (Finnie et al., Reference Finnie, Khoza, van den Borne, Mabunda, Abotchie and Mullen2011).
Pathways to TB care
This was measured using a modified version of the World Health Organization (WHO) encounter form for mental disorders (WHO, 1987). Pathway to TB care was categorized as ‘direct’ if people with TB directly contacted the modern health care system where TB symptoms were recognized for the current illness episode. Pathways were categorized as ‘indirect’ if participants indicated that they had sought help from the traditional health care system prior to attending biomedical services.
Independent variables
Probable depression:
Depression was an independent variable hypothesized to be associated with both pathways to TB care and diagnosis delay. It was also considered as a mediator of the relationship between other independent variables and the dependent variables. Probable depression was measured using the nine-item version of the Patient Health Questionnaire (PHQ-9). Globally, the scale has been widely used in surveys, effectiveness trials and cohort studies (Kroenke et al., Reference Kroenke, Spitzer, Williams and Lowe2010). In Ethiopia, it has been validated in two settings and was found to be useful in screening depression in adult outpatients (Gelaye et al., Reference Gelaye, Williams, Lemma, Deyessa, Bahretibeb, Shibre, Wondimagegn, Lemenhe, Fann, Vander Stoep and Andrew Zhou2013; Hanlon et al., Reference Hanlon, Medhin, Selamu, Breuer, Worku, Hailemariam, Lund, Prince and Fekadu2015). The optimum cut-off point was five and above in primary healthcare centres in a rural district (Hanlon et al., Reference Hanlon, Medhin, Selamu, Breuer, Worku, Hailemariam, Lund, Prince and Fekadu2015) and ten and above in outpatient medical clinics in a referral hospital in Addis Ababa (Gelaye et al., Reference Gelaye, Williams, Lemma, Deyessa, Bahretibeb, Shibre, Wondimagegn, Lemenhe, Fann, Vander Stoep and Andrew Zhou2013). We applied the more conservative cut-off point of ten and above to define probable depression given the potential overlap between TB and depression symptoms. The baseline data of this study indicated that the PHQ-9 had a single-dimensional structure, Cronbach's alpha of 0.81, and a mean inter-item correlation coefficient of 0.33 (Ambaw et al., Reference Ambaw, Mayston, Hanlon and Alem2017). In this paper, the term depression is used instead of probable depression for simplicity.
Socio-demographic variables
Age, sex, marital status, level of education, religion, household income, occupation and place of residence (urban v. rural) were measured by self-report. Household income was measured by asking the participants to estimate the monthly total income of their household. When the participant was a farmer, we changed the estimates of annual income in kind to cash using the local market price. We converted the monthly income into annual income.
Substance use
Alcohol, tobacco and khat use were measured using the WHO Alcohol, Smoking and Substance Involvement Screening Test (ASSIST) (version 3.1) (WHO, 2010a). ASSIST was designed for use across different cultural settings. The instrument's psychometric properties have been tested using data from multiple countries, including low, middle, and high-income countries and shown to be valid, reliable and easy to administer across settings (Humeniuket al., Reference Humeniuk, Ali, Babor, Farrell, Formigoni, Jittiwutikarn, de Lacerda, Ling, Marsden, Monteiro, Nhiwatiwa, Pal, Poznyak and Simon2008).
Perceived social support: Perceived social support was measured using the three-item Oslo Scale of Perceived Social Support with scores ranging from 3 to 14 (Meltzer, Reference Meltzer, Nosikov and Gudex2003). The scale was previously reported to work well in Ethiopia in TB patients (Duko et al., Reference Duko, Gebeyehu and Ayano2015). The total score was categorized in tertiles which were then operationalized as poor, moderate and strong perceived social support.
Co-morbid illness
Data on the presence of chronic illnesses other than TB were obtained by asking the question ‘Have you ever been told by health professionals that you have cardiac illness, hypertension, diabetes mellitus, depression or mental illnesses other than depression?’ HIV status was recorded from the TB register.
Type of TB (pulmonary or extra-pulmonary)
Information extracted from the TB register in the health facilities.
Disability
Disability was measured using the interviewer administered version of the 12-item World Health Organization Disability Assessment Schedule, version 2.0 (WHODAS 2.0) (WHO, 2010b). Studies have demonstrated the usefulness of the tool for assessing disability in primary care patients with depression (Chwastiak & Von Korff, Reference Chwastiak and Von Korff2003). The scale has been previously used in Ethiopia (Mogga et al., Reference Mogga, Prince, Alem, Kebede, Stewart, Glozier and Hotopf2006; Senturk et al., Reference Senturk, Hanlon, Medhin, Dewey, Araya, Alem, Prince and Stewart2012; Habtamuet al., Reference Habtamu, Alem, Medhin, Fekadu, Dewey, Prince and Hanlon2017). Scores were divided into tertiles and operationalized as no or low disability, moderate and severe disability.
Perceptions about TB
Perceived severity of TB, perceived benefits of TB treatment, perceived barriers to modern TB treatment and perceived causes of TB were captured by asking the respondents, ‘How severe do you think TB is (mild, moderate or severe), how helpful do you think medications for TB are (not helpful, somehow helpful or very helpful), and do you have barriers to take your medications as prescribed (yes or no), what do you think is the cause of TB?’, respectively.
TB-related stigma
TB-related stigma was measured at the second assessment using a 10-item TB stigma scale adapted from Macq et al. (Reference Macq, Solis and Martinez2006), translated into Amharic, and piloted (Ambaw et al., Reference Ambaw, Mayston, Hanlon and Alem2015). In this sample, the scale had an alpha value of 0.84 and a mean inter-item correlation coefficient of 0.34. Scores were cut into three equal parts and operationalized as low, moderate, and high stigma.
Analyses
Data were analyzed using STATA version 15 (StataCorp. URL: http://www.stata.com). Descriptive statistics were used to summarize variables and to describe participants. Logistic regression was fitted using generalized structural equation modelling (GSEM) to identify the association between depression and the dependent variables (diagnostic delay and pathways to TB care) as well as the role of depression as a mediator between other independent variables and the dependent variables. The role of pathways to TB care as a mediator between diagnostic delay and all other independent variables including depression was assessed the same way. GSEM allows modelling categorical outcomes and generalized responses without the need to fulfil the requirement of multivariate normality (Rabe-Hesketh et al., Reference Rabe-Hesketh, Skrondal and Pickles2004; StataCorp, 2017). The inclusion of independent variables in the multivariable analysis was based on its theoretical importance and adequacy of the number of participants in cells for each category (Tabachnic & Fidell, Reference Tabachnic and Fidell2007). Because the study sites were located in two regions of the country, clustered robust standard errors were used. p values <0.05 were considered statistically significant. Associations have been reported using odds ratios and beta (β) coefficients depending on the availability of options for GSEM in STATA 15. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines have been used to report our findings (von Elm et al., Reference von Elm, Altman, Egger, Pocock, Gotzsche, Vandenbroucke and Initiative2007).
Results
Socio-demographic characteristics of the participants
Just over half of the participants (n = 312; 52.7%) were male, 444 (75.0%) had primary education or no formal education and the median age of the participants was 30 years with range 18–85 years (Table 1).
Table 1. Socio-demographic characteristics of participants (n = 592)

Illnesses and substance use characteristics
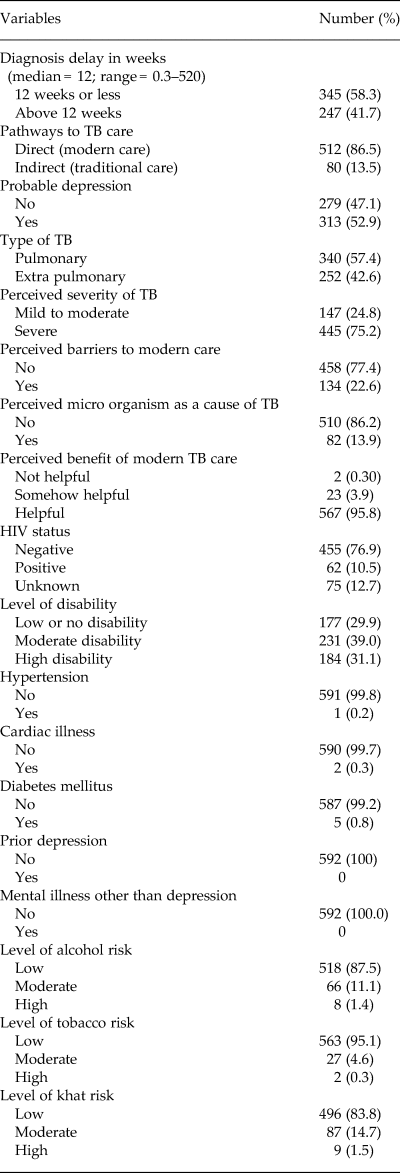
Just over half of the participants (n = 313; 52.9%) had probable depression. In total 445 (75.3%) perceived that TB is a severe illness and only 82 (13.9%) perceived that TB was caused by microorganisms. A total of 62 (10.2%) were living with HIV. Moderate to high risk of alcohol, khat and tobacco was reported by 74 (12.5%), 96 (16.2%), and 29 (4.9%) of participants, respectively (Table 2).
Table 2. Illness, substance use and pathways to TB care (N = 592)
Diagnostic delay and pathways to TB care
The median delay to diagnosis was 12 weeks (range 0.3–520.0 weeks). A total of 512 (86.5%) participants contacted the modern health care system directly. The remaining 80 (13.5%) participants visited the traditional health care system before contacting the modern health care system where they had their illness diagnosed as TB (Table 2).
Factors associated with pathways to TB care and diagnostic delay
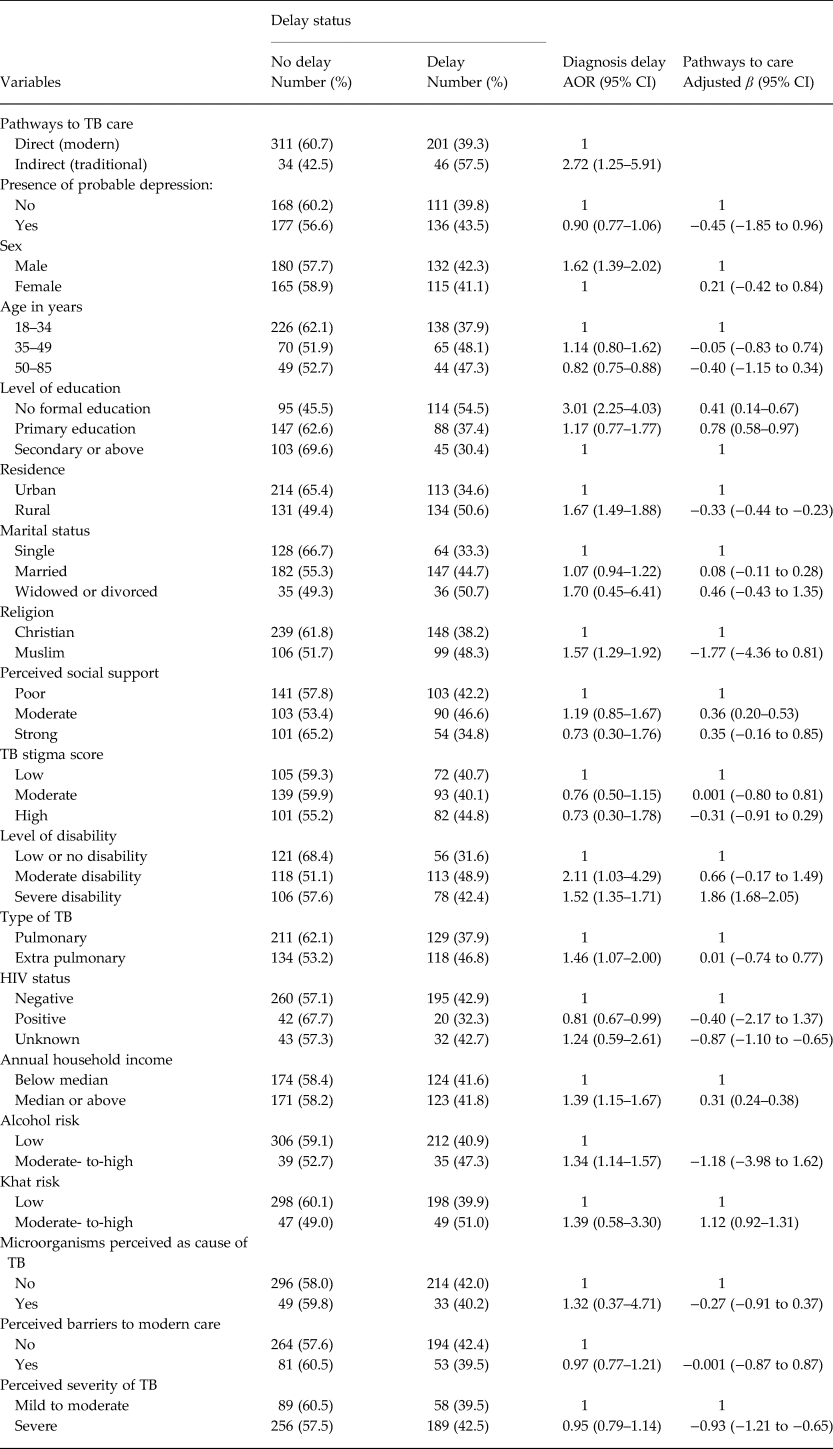
There was no association between depression and diagnostic delay (Adjusted odds ratio (AOR) = 0.90; 0.77, 1.06) or with pathways to TB care (adjusted β = −0.45; 95% CI−1.85 to 0.96). Indirect pathways to TB care (AOR = 2.72; 95% CI 1.25–5.91), male gender (AOR = 1.62; 95% CI 1.39–2.02), absence of formal education (AOR = 3.01; 95% CI 2.25–4.03), being a rural resident (AOR = 1.67; 95% CI 1.49–1.88), being Muslim (AOR = 1.57; 95% CI 1.29–1.92), having moderate (AOR = 2.11; 95% CI 1.03–4.29) or severe disability (AOR = 1.52; 95% CI 1.35–1.71), having extra-pulmonary TB (AOR = 1.46; 95% CI 1.07–2.00), having higher household income (AOR = 1.39; 95% CI 1.15–1.67), and moderate- to- high risk of alcohol use (AOR = 1.34; 95% CI 1.14–1.57) were associated directly with delay of diagnosis in people with TB. HIV positive status (AOR = 0.81; 95% CI 0.67–0.99) and age group 50–85 years (AOR = 0.82; 95% CI 0.75–0.88) had inverse relation with delaying diagnosis of TB.
Absence of formal education (adjusted β = 0.41; 95% CI 0.14–0.67) or having just primary education (adjusted β = 0.78; 95% CI 0.58–0.97), perceived social support (adjusted β = 0.36; 0.20–0.53), severe disability (adjusted β = 1.86; 95% CI 1.68–2.05), higher household income (adjusted β = 0.31; 95% CI 0.24–0.38), and moderate- to- high risk of khat use (adjusted β = 1.12; 95% CI 0.92–1.31) were positively associated with diagnostic delay through increasing visits to the traditional health care system before reaching modern care facilities. On the other hand, rural residence (adjusted β = −0.33; 95% CI −0.44 to −0.23), unknown HIV status (adjusted β = −0.87; 95% CI −1.10 to −0.65), and perceiving TB as a severe illness [adjusted β = −0.93 (−1.21 to −0.65)] indirectly decreased diagnostic delay through decreasing visits to the traditional health care system (Table 3). The path diagram of the analysis is shown in online Supplementary Figure S1).
Table 3. Factors associated with pathways to TB care and diagnosis delay (n = 592)
AOR, adjusted odds ratio.
Discussion
None of our hypotheses was supported: co-morbid depression was not associated with either diagnostic delay or indirect pathways to TB care, and depression did not appear to be a mediator of associations between various socio-demographic and clinical factors and diagnostic delay or pathways to TB care.
There were no previous studies to compare our findings. Two further factors require investigation before we accept the null hypothesises of no difference. First, only 71.0% of all estimated new TB cases in Ethiopia are detected (World Health Organization, 2016). We do not know whether the undetected 29.0% of cases are different from 71.0% in terms of depression status. Second, health extension workers in the Ethiopian health care system encourage people with TB symptoms to receive early diagnosis and treatment by going from home-to-home (Workie & Ramana, Reference Workie and Ramana2013). That means the role of depression in influencing diagnosis delay may be reduced. Health extension workers are more likely to help people with TB symptoms when the symptoms are clear. For example, we found that people with pulmonary TB had shorter diagnosis delay compared to those with extra-pulmonary TB where symptoms vary depending on the site (Pallangyo, Reference Pallangyo2001).
Our findings suggest that depression may not have any impact upon pathways to care for TB and the knowledge of microorganisms as a cause for TB may not be associated with where to go upon experiencing symptoms. These findings generally agree with previous studies. In Ethiopia, the choice of a healer for an illness largely depends on the reputation of the healer in their community (Jakonsson, Reference Jakonsson1991) rather than the symptoms felt or the perceived cause of the illness (Keegstra, Reference Keegstra1986). When people fail with one, they go to another (Kloos et al., Reference Kloos, Degefa, Aga, Solomon, Abera and Abegaz1997).
Our findings that indirect pathway to TB care leads to diagnostic delay agrees with the existing evidence (Barker et al., Reference Barker, Millard, Malatsi, Mkoana, Ngoatwana, Agarawal and de Valliere2006; Finnie et al., Reference Finnie, Khoza, van den Borne, Mabunda, Abotchie and Mullen2011). With all other socio-demographic variables in this study kept constant, better income was found to lead to diagnostic delay both directly and indirectly by leading to indirect pathways to TB care. Perceived good social support also contributed to diagnosis delay through an increasing visit to the traditional health care system. The explanation why people with better income and support encounter a longer delay before diagnosis was not clear. There is some evidence that traditional care is much more expensive than the modern one (Makanjuola, Reference Makanjuola2003). People with more resources may be exploring more options of treatments for their symptoms before accessing modern care. In Ethiopia, modern TB care is totally free.
Our findings that the absence of formal education, being a rural resident, having extra pulmonary TB, and alcohol use are associated with diagnostic delay agree with previous reports (Storla et al., Reference Storla, Yimer and Bjune2008). Contrary to previous reports (Storla et al., Reference Storla, Yimer and Bjune2008; Virenfeldt et al., Reference Virenfeldt, Rudolf, Camara, Furtado, Gomes, Aaby, Petersen and Wejse2014), HIV decreased diagnostic delay in our study probably because people who have known HIV status seek help more actively than those without HIV; they are people who have already sought help for HIV and been informed about potential symptoms of TB. The associations between gender, age, religion, and residence and diagnosis delay and pathways to TB care indicate the need for exploring the underlying cultural drivers (Bailey, Reference Bailey1987). The association between disability and diagnosis delay may show that people with a long period with illness develop severe forms of disability or people with disability find it harder to access services (Virenfeldt et al., Reference Virenfeldt, Rudolf, Camara, Furtado, Gomes, Aaby, Petersen and Wejse2014).
Limitations
We measured depression using a screening tool. We also overly summarized pathways to care in to direct and indirect without considering back and forth visits or simultaneous use of both the traditional and conventional health systems. People may not remember exactly when the symptoms of TB started and, therefore, our estimates of diagnosis delay may not be accurate. Our findings are generalisable only to people with TB who were eventually attending the conventional care regardless of their pathways; specifically, it cannot be generalisable to those attending care in the traditional care system only. Eighty-five per cent of the sample reported to earn <1$/day/person (Ambaw et al., Reference Ambaw, Mayston, Hanlon and Alem2017), and higher income and social support are, therefore, only relative. Although there might be a tendency to under report income, it might not seriously affect regression outputs as those with higher income are likely to report higher values than those with lower income forming a pattern similar to the correct value. The other limitation was the absence of qualitative evidence on how each of the socio-demographic factors was connected to pathways to care and diagnosis delay.
Conclusions
People with TB who had co-morbid depression visited the modern health care system as directly as and as soon as people with TB who did not have co-morbid depression. Depression was not mediating the relationship between diagnostic delay and factors associated with diagnostic delay. Co-morbid depression in people with TB could be diagnosed and treated at TB clinics by integrating mental health components into the TB management protocol. This recommendation can be used in other settings as well. How socio-demographic factors influence pathways to care and diagnosis delay require qualitative exploration.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/gmh.2019.17
Acknowledgement
We are grateful to our research participants, research assistants, and officials of health institutions. The research was mainly funded by the European Union, Seventh Framework Programme (FP7/2007–2013) under the Emerald grant agreement number 305968, and partially funded by the Psychiatry Research Trust. The funding sources had no involvement in the conduct of the research or in the preparation of the article.FA and CH received support from AMARI (African Mental Health Research Initiative), which is funded through the DELTAS Africa Initiative (DEL-15-01). The DELTAS Africa Initiative is an independent funding scheme of the African Academy of Sciences (AAS)'s Alliance for Accelerating Excellence in Science in Africa (AESA) and supported by the New Partnership for Africa's Development Planning and Coordinating Agency (NEPAD Agency) with funding from the Wellcome Trust (DEL-15-01) and the UK government. The views expressed in this publication are those of the author(s) and not necessarily those of AAS, NEPAD Agency, Wellcome Trust or the UK government. CH is supported by the National Institute of Health Research (NIHR) Global Health Research Unit on Health System Strengthening in Sub-Saharan Africa, King's College London (GHRU 16/136/54). The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health and Social Care.
Author contribution
FA, RM, CH, and AA contributed to the design and undertaking of the study. FA trained research assistances, supervized field work, and drafted the manuscript. All authors reviewed the manuscript and approved the final version.
Declaration of interest
None.
Ethical standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.





