INTRODUCTION
The fall in tuberculosis (TB) incidence in England over the last century was, at least in part, due to a reduction in levels of poverty and socio-economic deprivation. TB has recently re-emerged as a serious public health problem in England [1]. Control of TB is founded on early diagnosis and treatment of active cases and infected contacts. Delay in initiating treatment not only impacts on TB control by increasing the risk of disease transmission [Reference Rieder2], but also adversely affects clinical outcomes including increasing the risk of mortality [Reference Lefebvre and Falzon3–Reference Zahar5]. The interval from symptom onset to diagnosis and initiation of treatment among TB cases presenting passively to health-care services is influenced by a number of factors.
Most studies looking at factors associated with treatment delay are from high prevalence countries [Reference Thomas6]. Studies from developed countries include those from the United States [Reference Sarmiento7–Reference Sherman10], Japan [Reference Ohmori11], Canada [Reference Greenaway12], and the United Kingdom [Reference Rodger13–Reference Wares, Ormerod and Morton15]. Social and cultural factors such as unemployment, cost of care, lack of knowledge of health services, language barriers, homelessness, and concerns regarding immigration status, have been associated with delayed access to care in developed countries [Reference Sarmiento7, Reference Asch9–Reference Ohmori11]. Earlier studies from the United Kingdom have reported longer TB treatment delays among those of white ethnicity, females, older patients, and those born in low prevalence countries [Reference Rodger13, Reference Paynter14]. None of these studies examined the effect of socio-economic deprivation on TB treatment delays.
Understanding the factors associated with TB treatment delays, including potentially modifiable factors such as socio-economic deprivation, is essential for effective disease control. This analysis of national surveillance data, therefore, aims to investigate whether there is an association between an ecological measure of socio-economic deprivation and the interval from symptom onset to initiation of TB treatment.
METHODS
Data sources
Information on TB cases reported to the Enhanced Tuberculosis Surveillance (ETS) system for England during the period 2000–2005 was analysed. This national surveillance system collects information on the demographic and clinical characteristics of TB cases. Details of the system have been published elsewhere [1].
The index of multiple deprivation (IMD) provides deprivation scores for small census areas in England (Lower Super Output Areas). IMD scores are a composite measure based on seven dimensions of deprivation (income, employment, health and disability, education, skills and training, barriers to housing and services, living environment and crime) [16]. MapInfo Professional (version 8.0) was used to assign a deprivation score, based on residential postcode, to each patient using the 2004 IMD. Patients were then categorized into quartiles of deprivation according to their IMD score.
Definitions
TB cases were either those with culture-confirmed disease due to Mycobacterium tuberculosis complex (M. tuberculosis, M. bovis or M. africanum) or other cases meeting the following criteria: (a) a clinician's judgement that the patient's clinical or radiological signs are compatible with TB and (b) the clinician's decision to treat the patient with a full course of anti-TB treatment.
The interval to start of treatment was defined as the total number of days between onset of symptoms (as reported by the patient) and date of start of treatment, or, if this was missing, date of diagnosis. Since the ETS system does not collect information on the date that patients first present to health-care services, it was not possible to separate patient delays (i.e. delay from onset of symptoms to presentation to health-care services), from health-care delays (i.e. delay from patient presentation to initiation of treatment).
Ethnic groups were based on the Office of National Statistics (ONS) classifications. Recent UK entrants were defined as those born abroad who entered the United Kingdom <2 years prior to being diagnosed with TB.
Statistical analysis
Median intervals and inter-quartile ranges (IQRs) were calculated by deprivation score quartile and by age group, sex, ethnic group, place of birth/time since entry into the United Kingdom, site of disease, and previous TB diagnosis. Cox proportional hazards regression was used to investigate the association between the interval to treatment and each of these variables. The likelihood ratio (LR) test was used to assess interactions between deprivation and each other variable. Multivariable Cox proportional hazards models adjusted for age and gender were stratified by those variables found to significantly modify the effect of deprivation on the interval to initiation of treatment. A hazard ratio (HR) <1 indicates a longer interval. Data were analysed using Stata statistical software, version 9 [17].
Ethics approval
The Health Protection Agency has Patient Information Advisory Group approval to hold and analyse national surveillance data for public health purposes under Section 60 of the Health and Social Care Act 2001. Strict confidentiality of all data is maintained.
RESULTS
Study population
A total of 40 779 TB cases were reported to the ETS system in England during 2000–2005. The interval to start of treatment could be derived for 56% (22 856) of these. The median age of this study population was 36 years (IQR 26–54), 55% were male, and 68% were non-UK born (Table 1).
Table 1. Median intervals and univariable hazard ratios for the association between tuberculosis (TB) case characteristics and the interval to initiation of TB treatment
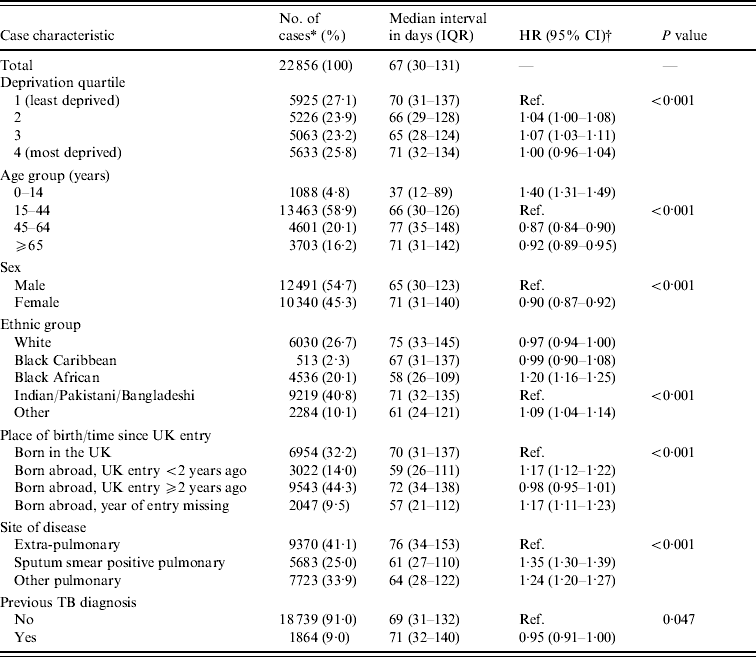
HR, Hazard ratio; IQR, inter-quartile range; CI, confidence interval.
* Sum of numbers for each characteristic will not equal the total due to missing information.
† HR <1 indicates a longer interval.
Cases without information available on the interval to start of treatment were similar to the study population in terms of age (median age 35 years, IQR 25–54) and gender (55% male). They did, however, differ slightly by level of deprivation (of those missing data on interval to treatment, 22% were in the least deprived quartile compared to 27% of the study population).
Interval to start of treatment
The overall median interval to start of treatment for the population was 67 days (IQR 30–131). The interval was similar among those living in the four deprivation quartiles, although slightly longer among the least deprived and most deprived compared to those in the middle two quartiles. Longer intervals were experienced by older patients, females, those of white ethnicity, those born in the United Kingdom or born abroad with UK entry ⩾2 years prior to TB diagnosis, patients with extra-pulmonary disease, and those with a previous TB diagnosis (Table 1).
Effect of socio-economic deprivation on the interval to start of treatment
There was strong evidence that the effect of deprivation on the interval to initiation of treatment was modified by ethnic group (LR test, P=0·004) and by place of birth/time since entry into the UK (LR test, P=0·002). Therefore, for further analyses, the effect of deprivation on the interval to start of treatment was stratified by these variables.
After adjusting for age and sex, longer intervals were experienced by the most deprived black Africans [adjusted hazard ratio (aHR) 0·84, 95% confidence interval (CI) 0·77–0·92, P<0·001], Indians/Pakistanis/Bangladeshis (aHR 0·93, 95% CI 0·88–0·99, P=0·014), and recent UK entrants (aHR 0·88, 95% CI 0·79–0·97, P=0·012) compared to the least deprived (Table 2). In contrast, among white and UK-born patients, shorter intervals were experienced by the most deprived (aHR 1·09, 95% CI 1·01–1·17 and aHR 1·08, 95% CI 1·01–1·16, respectively) (Table 2).
Table 2. Median intervals and adjusted hazard ratios for the interval to initiation of tuberculosis treatment in patients living in the most deprived areas compared to those in the least deprived, stratified by ethnic group and place of birth/time since entry into the United Kingdom
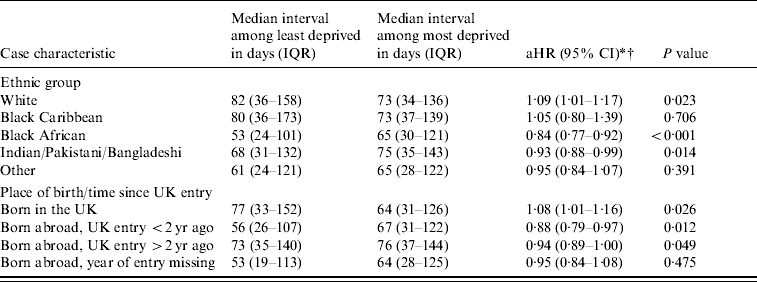
aHR, Adjusted hazard ratio; CI, confidence interval.
* aHR <1 indicates a longer interval.
† Adjusted for age and sex.
DISCUSSION
TB patients in England experience a median interval of 67 days from onset of symptoms to start of treatment. This interval falls within the range observed in previous studies in England [Reference Rodger13–Reference Wares, Ormerod and Morton15], and other developed countries [Reference Asch9, Reference Pirkis18, Reference Farah19]. There is currently no consensus as to what is considered as an ‘acceptable’ interval although 30 days has been suggested [Reference Pirkis18]. The substantial interval observed here is therefore of concern.
Although overall there was little evidence of an association between deprivation and interval to treatment on univariable analysis, this did vary by ethnic group and place of birth/time since UK entry. The particularly long median intervals observed among the least deprived white and UK-born patients [82 days (IQR 36–158) and 77 days (IQR 33–152), respectively] are of concern, and may be due to the lower index of clinical suspicion of TB (compared to that among the most deprived patients in these population groups). The longer intervals observed among the most deprived black Africans, Indians/Pakistanis/Bangladeshis and recent UK entrants may be related to language barriers, lack of knowledge of health services, or issues related to immigration status. Such factors have been found to be associated with treatment delays elsewhere [Reference Sarmiento7, Reference Asch9, Reference Sherman10]. These deprived population groups may also experience barriers to accessing care, for example, difficulties registering with a general practitioner [Reference Cooke20].
In this study, longer intervals were also found to be associated with older age, female gender, having extra-pulmonary disease, and having had a previous TB diagnosis. However, the actual differences in median delays between some of these groups were quite small and may therefore not be of public health significance. The longer intervals among the elderly could be explained by the higher frequency of comorbidities in this group which can complicate TB diagnosis [Reference Paynter14]. Meanwhile, the longer intervals experienced by the middle-aged population could be related to factors such as place of birth and ethnic group, or possibly social factors such as homelessness, imprisonment or drug use [Reference Story21]. Longer intervals among females have been observed previously [Reference Rodger13]. Patients with extra-pulmonary TB experienced longer intervals compared to those with pulmonary disease. However, a 61-day median interval was observed among sputum smear-positive pulmonary cases which is of particular concern in terms of potential transmission of TB. The identification and implementation of methods to reduce these intervals should be addressed as a priority for TB control.
It was not possible to separate patient delays from health-care delays. Such information would be useful in interpreting the associations observed in this study. There will be differences in both the duration of, and reasons for, these two aspects of delay. For example, patient delays may be due to social and behavioural factors such as health-care-seeking behaviours, awareness of TB and its symptoms, cultural norms, perceived stigma, and access to services. In addition, biological factors such as severity of symptoms will also play a role. Meanwhile, health-care delays may relate to the clinician's index of suspicion/awareness of TB, access to diagnostic facilities, referral procedures and other organizational factors. The collection of data that allows the separation of patient delays from health-care delays is an important consideration for future surveillance.
The IMD score is an ecological measure of deprivation and was used as a proxy for individual levels of deprivation. There will be some misclassification of an individual's level of deprivation using an area measure, e.g. there may be some clustering of certain population subgroups in geographical areas. Consequently, the association between deprivation and treatment delays may have been underestimated in this study [Reference Galobardes22, Reference Strong, Maheswaran and Pearson23]. It is also difficult to disentangle the effects of an individual's level of deprivation from the effects of the level of deprivation of the area in which they live, e.g. availability of health-care services. However, the IMD score is a composite deprivation measure, and its domains have been correlated to other health indicators such as mortality [Reference Strong, Maheswaran and Pearson23] and life expectancy [Reference Woods24].
Other limitations of this study are that 44% of cases were missing information on the interval to start of treatment which may have introduced some selection bias. Cases with missing information were, however, similar to those with information in terms of age and gender. Date of onset of symptoms was self-reported and may therefore lack accuracy. Finally, not all patients have a postcode of residence, in particular, deprived groups such as the homeless. However, only a small proportion of cases (4·6%) could not be assigned a deprivation score.
CONCLUSION
The association between deprivation and TB treatment delay in some population groups demonstrates that deprivation is still playing a role in the epidemiology of TB in England today. The overall median delay of 67 days is substantial, and delays need to be minimized for all patients. Particular efforts may be needed among certain population groups especially the least deprived white and UK-born populations, and also the most deprived minority ethnic populations and recent UK entrants. Prompt diagnosis and initiation of effective anti-TB treatment is a key element of TB control, and any inequities in this need to be addressed. Improving awareness of TB, ensuring better access to health care, and increasing the clinical index of suspicion of TB among certain population groups and their health-care providers, should help reduce delays.
ACKNOWLEDGEMENTS
We thank all those who provided information on TB cases to the Enhanced Tuberculosis Surveillance system. Many thanks to David Quinn for the management and preparation of the dataset for analysis, and to Chris Lane for assigning TB cases to Lower Super Output Areas. Thanks are also due to John Watson for his helpful comments on an earlier draft of this paper.
DECLARATION OF INTEREST
None.




