Psychosocial issues are an important morbidity in the paediatric cardiology population. Children with cardiac diagnoses requiring lifelong care have increased rates of anxiety,Reference Bromberg, Beasley, D’Angelo, Landzberg, DeMaso and Massachusetts 1 , Reference Hövels-Gürich, Konrad and Skorzenski 2 depression,Reference Bromberg, Beasley, D’Angelo, Landzberg, DeMaso and Massachusetts 1 , Reference Hövels-Gürich, Konrad and Skorzenski 2 post-traumatic stress disorder,Reference Connolly, McClowry, Hayman, Mahony and Artman 3 aggression,Reference Hövels-Gürich, Konrad and Skorzenski 2 and social and behavioural problems.Reference Hövels-Gürich, Konrad and Skorzenski 2 Studies of adolescentReference Kim 4 and adultReference Bromberg, Beasley, D’Angelo, Landzberg, DeMaso and Massachusetts 1 , Reference Kim 4 survivors of paediatric cardiac disease indicate that psychosocial morbidities continue to impact these patients. Such mental health issues would be expected to decrease quality of life, as quality of life is comprised of both physical and psychosocial dimensions. Most studies among paediatric cardiac patients have found decreased overall,Reference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 – Reference Berkes, Pataki and Kiss 8 physical,Reference McCrindle, Williams and Mitchell 7 , Reference Berkes, Pataki and Kiss 8 or psychosocialReference Mussatto and Tweddell 6 – Reference Berkes, Pataki and Kiss 8 quality of life, although scores similar to healthy peers have also been reported.Reference Culbert, Ashburn and Cullen-Dean 9 Interestingly, several studies have documented reports of quality of life similar to peers even when assessments indicate significant psychosocial morbidity.Reference Hövels-Gürich, Konrad and Wiesner 10 – Reference Ekman-Joelsson, Berntsson and Sunnegårdh 13
Assessing quality of life and psychosocial health in paediatric populations can be difficult. Although self-reports are considered the gold standard, assessments in the paediatric population typically rely on parent proxy reports, particularly when children are young, cognitively impaired, or too ill or fatigued to answer for themselves.Reference Varni, Limbers and Burwinkle 14 , Reference Eiser and Morse 15 Research demonstrates cross-informant discordance between parent and child reports of quality of life for healthy childrenReference Cremeens, Eiser and Blades 16 , Reference Jozefiak, Larsson, Wichstrøm, Mattejat and Ravens-Sieberer 17 and children with a variety of chronic conditions.Reference Eiser and Morse 15 , Reference Nugent, Kline, Thompson, Reeves and Schiffman 18 – Reference Panepinto, O’Mahar, DeBaun, Loberiza and Scott 25 For paediatric cardiac patients, the accuracy of parent proxy reports is unknown. Studies assessing quality of life have indicated both agreementReference Marino, Shera and Wernovsky 26 and discordanceReference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 , Reference Berkes, Pataki and Kiss 8 between self-reports and parent proxy reports, with discordance indicating higher quality of life via either parentReference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 or childReference Berkes, Pataki and Kiss 8 reports. No reports have compared self-reports and parent proxy reports for more specific measures of psychosocial health in the paediatric cardiology population. Understanding the similarities and differences between parent and child reports of the child’s psychosocial health is important, as parent perceptions of the child’s psychosocial health heavily influence the child’s access to healthcare.Reference Varni, Limbers and Burwinkle 14 The purpose of this study was to compare parent proxy reports and child self-reports of the child’s psychosocial health among children with cardiac diagnoses requiring lifelong care and their parents.
Materials and methods
Study design
This cross-sectional study was approved by the Research Ethics Boards of The Hospital for Sick Children (Toronto, 2011) and Children’s Hospital of Eastern Ontario (Ottawa, 2013). Any clinically relevant indications of suicidal ideation, self-harm, or harm to others identified by the questionnaires were immediately referred to a co-investigator (G.G., clinical psychologist) for follow-up evaluation.
Study participants
Patients aged 6–14 years attending the cardiac clinic for a regularly scheduled appointment were eligible for this study. Children with various cardiac diagnoses were recruited, including CHDs, arrhythmia, infectious/inflammatory disease, or cardiomyopathy. Patients were excluded if they were being treated for acute changes to health status, had an intervention – catheterisation or surgery – within the previous 6 months, had an identified cognitive disability or emotional health diagnosis, or if the child or parents did not speak English or French sufficiently well to answer the study instruments. Eligible participants received a letter of introduction to the study, and their willingness to participate was confirmed upon their arrival at the clinic. Parents and children provided their written informed consent to participate in the study.
Psychosocial health assessments
We used three standardised instruments to assess quality of life – Pediatric Quality of Life InventoryReference Varni, Seid and Kurtin 27 – emotional health and behaviour – Behavioral Assessment Scale for Children (Version 2)Reference Reynolds and Kamphaus 28 – and anxiety – Multidimensional Anxiety Scale for Children.Reference Reynolds and Kamphaus 28 All children and parents completed the Pediatric Quality of Life Inventory Core assessment of general quality of life. Children above age 8 (n=38) were asked to complete the Multidimensional Anxiety Scale for Children questionnaire to assess anxiety. Parents completed the Pediatric Quality of Life Inventory Family Impact module, as an assessment of the impact of the child’s illness on family function, and the Behavioral Assessment Scale for Children (Version 2) questionnaire, as an assessment of the child’s adaptive skills and internalising, externalising, and behavioural symptoms. A subset (n=19) of children also completed the Behavioral Assessment Scale for Children (Version 2) self-report. These psychosocial health instruments have been shown to have strong reliability and validity in children.Reference Varni, Seid and Kurtin 27 – Reference March 29 Parents and children were requested to complete the study questionnaires during their clinic visit. Children were encouraged to complete the questionnaires independent of their parents, with assistance from the researcher as required; five families who were unable to complete all questionnaires during the clinic visit were provided with an envelope to return the completed questionnaires by mail.
Instrument composite scores
All questionnaires were scored according to the established procedures for each instrument. The Pediatric Quality of Life Inventory assessed physical (walk, run, lift, self-care), social (peer relations), school (attention, attendance, ability to do schoolwork), and emotional (fear, depression, anger, worry), quality of life and provided psychosocial – aggregate of the social, school, and emotional health subscales – and total summary scores. Child responses to the Multidimensional Anxiety Scale for Children generated a total Multidimensional Anxiety Scale for Children Score. Parent Behavioral Assessment Scale for Children (Version 2) responses were summarised as scores for externalising problems (composite of hyperactivity, aggression, and conduct problems), internalising problems (composite of anxiety, depression, and somatisation), Behavioral Symptoms Index (composite of atypicality, withdrawal, and attention problems), and adaptive skills (composite of adaptability, social skills, and functional communication). Child responses to the Behavioral Assessment Scale for Children (Version 2) generated scores for the subcategories inattention/hyperactivity, school problems, internalising problems, and personal adjustment. For each instrument, a higher numerical score indicates more of the measured behaviour – for example, higher quality of life, higher anxiety, and more externalising problems. The Multidimensional Anxiety Scale for Children and Behavioral Assessment Scale for Children (Version 2) provide standardised T-scores for each domain that can be compared across different instruments, ages, and genders.Reference Corcoran and Fischer 30
Statistical analyses
Parent and child responses were compared for each questionnaire using three statistical assessments. Pearson’s correlations evaluated whether there was a linear association between parent and child scores. Significant differences between parent and child scores were evaluated using Student’s t-test. Correlational consistency, assuming random variability between subjects and fixed variability in the outcome measures, was evaluated using single measure, two-way mixed effects Intraclass Correlation Coefficient (ICC) (2,1) scores. The ICC scores were classified as poor <0.40, moderate 0.41–0.60, good 0.61–0.8, or excellent 0.81–1.00 on the basis of published conventions.Reference Bartko 31 The effects of patient age, sex, and city/clinic on differences between parent and child reports of the child’s quality of life – Pediatric Quality of Life Inventory – and psychosocial health – Behavioral Assessment Scale for Children (Version 2) – were assessed through regression analyses. In order to compare our study results with previously published research, a secondary analysis assessed the influence of age group: young child (6–7 years of age), child (8–12 years of age), and adolescent (13–16 years of age). As the Behavioral Assessment Scale for Children domain scores differ between the parent and child assessments, comparisons were made between domain scores representing similar psychosocial health issues. Parent- and child-reported anxiety scores were compared using T-scores from the Behavioral Assessment Scale for Children-internalising score (parent report) and the Multidimensional Anxiety Scale for Children total score (child report). Statistical significance was set at p<0.01 to account for multiple comparisons. Fisher’s r-to-z transformation was utilised to compare correlations found in this study with published normative data.Reference Varni, Seid and Kurtin 27
Results
Study population
A total of 50 paediatric cardiology patients (48% male) and their parents (n=50) participated in this study. The mean age of participating children was 10.1±2.4 years (range 6–14). Diagnoses were categorised as congenital structural heart defects (n=38), arrhythmia (n=5), cardiomyopathy (n=4), or infectious/inflammatory disease (n=3). The majority of patients (n=35) had mild dysfunction on echocardiography and were asymptomatic for chest pain, palpitations, and syncope. A few participants had moderate (n=6) or severe (n=4) cardiac dysfunction on echocardiography and/or experienced clinically significant symptoms. Echocardiographic assessments of disease severity were missing for five patients. Of 38 patients, 28 with CHDs (74%) had undergone at least one cardiac surgery. A smaller proportion (33%, 4/12) of patients with cardiomyopathy, arrhythmia, and infectious/inflammatory diseases were managed with invasive procedures, defined as catheterisation, surgery, or rhythm device insertion. Demographic and treatment data for participating children are summarised in Table 1. Participating parents included 32 mothers and nine fathers, with the sex of nine parents not reported. Of the 179 families approached, 73 (40.8%) consented to participate. Of these, 23 families did not return completed study questionnaires, resulting in data for 50 children and their parents. Among all, five participating families (10%) were immediately referred to a clinical psychologist (G.G.) because of Behavioral Assessment Scale for Children (Version 2) responses indicating suicidal ideation, self-harm, or harm to others. These questionnaires were retained in the study data.
Table 1 Demographic and treatment information on participating paediatric cardiology patients.
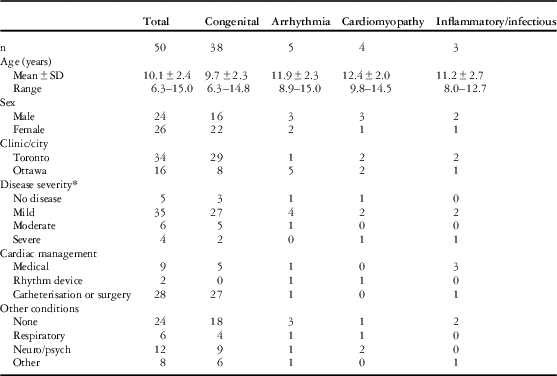
* Disease severity was determined by the classification of cardiac function via echocardiography as none, mild, moderate, or severe
Age, sex, and city effects
There were no significant effects of age, sex, city, or type of cardiac defect on parent–child differences in Pediatric Quality of Life Inventory Total, Physical, and Psychosocial scores (p>0.17, adjusted model R2⩽0.06) or Behavioral Assessment Scale for Children (Version 2) externalising, internalising, and adaptability domains (p>0.13, adjusted model R2⩽0.20). Therefore, all analyses were completed including patients of all ages, both sexes, and from both city centres.
Pediatric Quality of Life Inventory
There were no significant differences between child- and parent-reported quality of life (p>0.25), although child scores were consistently 2–3 points lower than parent scores for all domains (Table 2). Parent and child Pediatric Quality of Life Inventory scores were significantly correlated for school functioning, as well as the psychosocial and total summary scores. Emotional quality of life (R=0.25, p=0.10, ICC=0.25) had the lowest agreement (ICC=0.25).
Table 2 Comparison of child reported and parent proxy reported quality of life (Pediatric Quality of Life Inventory).Footnote ***

CI=confidence interval; ICC=Intraclass Correlation Coefficients
*** Results presented for 44 parent–child dyads; six parent–child dyads had incomplete data
**** Normative data obtained from Varni et alReference Varni, Seid and Kurtin 27 where n=871
***** Significance was established as p<0.01 due to multiple comparisons
****** Published normative data do not provide parent–child comparisons for the summary scores (psychosocial or total)
*p<0.01, **p<0.001
Behavioral Assessment Scale for Children (Version 2)
Comparisons of the parent and child reports of the child’s emotional health and behaviour are summarised in Table 3. Parent-reported externalising problems were correlated with child-reported symptoms of inattention/hyperactivity (n=14, R=0.70, p=0.01) and school problems (R=0.71, p=0.01). Parent reports of the child’s adaptive skills were significantly higher than the children’s own reports of their adjustment (t=2.46, p=0.03). There was no association between parent and child reports for internalising problems such as anxiety and depression.
Table 3 Comparison of the Behavioral Assessment Scale for Children (Version 2) results from cardiac children and their parents.Footnote **

CI=confidence interval; ICC=Intraclass Correlation Coefficients
*Significance was established as p<0.01 due to multiple comparisons
** A subset of 19 patient–parent dyads were asked to complete the Behavioral Assessment Scale for Children (Version 2) assessment. Of these, five parent reports were incomplete; therefore, the results presented are for 14 patient–parent dyads. The first variable listed for each comparison is the child self-report variable, followed by the parent proxy report variable used for comparison
*** Behavioral Assessment Scale for Children (Version 2) domains differ between parent and child reports. Domain scores comprised of similar constructs were compared. Child self-report domains included hyperactivity/inattention, school problems, internalising problems, and personal adjustment. Parent proxy report domains included externalising problems, internalising problems, and adaptive skills
**** Normative data obtained from the Behavioral Assessment Scale for Children (Version 2) Manual (n=892)
Multidimensional Anxiety Scale for Children
Complete Multidimensional Anxiety Scale for Children responses were available for 28 of the 38 children who were 8 years of age or older. Child-reported Multidimensional Anxiety Scale for Children T-scores (mean 45±16) were not correlated with parent-reported Behavioral Assessment Scale for Children (Version 2) T-scores for internalising problems (p=0.78) or anxiety (p=0.72) (Table 4).
Table 4 Comparison of child self-reported anxiety (Multidimensional Anxiety Scale for Children (MASC)) with parent-reported internalising behaviours and anxiety (the Behavioral Assessment Scale for Children (Version 2) (BASC2)).Footnote **

CI=confidence interval; ICC=Intraclass Correlation Coefficients
*Significance was established as p<0.01 due to multiple comparisons
** n=28. In all, 10 of 38 patient MASC to parent BASC2 comparisons were excluded due to incomplete responses
*** At the time of our study, the MASC parent proxy report was not available, and thus comparisons of child responses on the MASC were made with selected subscales from the parent proxy reports of the BASC2Reference Bromberg, Beasley, D’Angelo, Landzberg, DeMaso and Massachusetts 1
Pediatric Quality of Life Inventory Family Impact
Parent-reported family impact was positively correlated with parent-reported Pediatric Quality of Life Inventory total scores (R=0.73, p<0.001), school function (R=0.59, p<0.001), emotional function (R=0.59, p<0.01), social function (R=0.55, p<0.001), and physical function (R=0.69, p<0.001). Analyses indicate that parent reports that the child’s cardiac condition had a large impact on the family were strongly associated with reports of internalising (R=0.60, p<0.001) but not externalising emotional health problems (R=0.26, p=0.11).
Age-group effect
A secondary analysis comparing children within three age groups (6–7 years; 8–12 years; 13–16 years) found a significant interaction between parent and child differences for Pediatric Quality of Life Inventory total score and age group (F=4.49, p=0.02). Tukey’s post hoc tests demonstrated significant differences in Pediatric Quality of Life Inventory scores between young children (6–7 years of age, n=8, mean difference =17.9; 95% confidence interval (CI) of the mean difference: 8.8, 27.0) and their parents, but not older children (8–12 years of age, n=22, mean difference=3.1; 95% CI of mean difference: −10.5, +4.3) or adolescents (13–16 years of age, n=14, mean difference=3.0; 95% CI of mean difference: −6.4, +12.3).
Discussion
Similarities and differences in parent and child reports
The association between parent and child reports differed across various quality-of-life and psychosocial domains. Ratings provided by parents and children were moderately correlated for physical, school, and social quality of life as well as externalising behaviour problems. Parent and child measures of emotional quality of life, internalising problems, personal adjustment/adaptation skills, and anxiety were not correlated, and in fact strong parent–child differences were observed in the latter two categories. These results suggest that there is stronger agreement between parent and child reports for psychosocial health morbidities that may be easier to observe. Psychosocial domains related to thoughts and feelings are often more difficult to discern through observation, increasing the potential for discrepancies between parent and child reports. These patterns of discrepancy between parent and child reports of psychosocial health are consistent with discrepancies previously reported for quality-of-life measures among cardiac patientsReference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 , Reference Berkes, Pataki and Kiss 8 and healthy children.Reference Cremeens, Eiser and Blades 16 , Reference Varni, Seid and Kurtin 27 To our knowledge, this is the first study to compare T-scores from the Multidimensional Anxiety Scale for Children (child response) and Behavioural Assessment Scale for Children (Version 1 or 2, parent response). Although T-scores are specifically designed to enable standardised comparisons across respondent groups, instruments, etc., future research is recommended to examine this comparison among healthy children. Future research could also directly compare parent/child responses on the Behavioral Assessment Scale for Children and Multidimensional Anxiety Scale for Children, as both instruments are now available in both child self-report and parent proxy report formats.
Greater agreement for observable quality-of-life indicators
Berkes et alReference Berkes, Pataki and Kiss 8 administered the Hungarian version of the Pediatric Quality of Life Inventory to 195 patients, 5–18 years of age, with CHD, arrhythmia, cardiomyopathy, and acquired disease. They reported stronger parent–child agreement for reports of physical quality of life (ICC=0.72) in comparison with psychosocial quality of life (ICC=0.65) and emotional functioning (ICC=0.52).Reference Berkes, Pataki and Kiss 8 Similarly, Uzark et alReference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 collected Pediatric Quality of Life Inventory data from 347 patients, 5–18 years of age, with cardiac diagnoses described as mild, moderate, surgically treated, or severe/uncorrectable.Reference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 The results showed the greatest agreement for physical quality of life. Agreement within the psychosocial domains was reported as “consistently lower” in the adolescent population, although specific ICC values were not provided.Reference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 These studies support our findings of statistically significant correlations across all Pediatric Quality of Life Inventory domains except emotional functioning, with a similar trend for the lowest ICC values to occur in relation to emotional functioning. This finding is not unique to the cardiology population. Varni et al27 has demonstrated in a large study of 871 healthy children, 5–18 years of age, that there tends to be stronger parent–child agreement on Pediatric Quality of Life Inventory physical functioning (R=0.50) scores compared with parent–child agreement for emotional functioning (R=0.36).Reference Varni, Seid and Kurtin 27
Our study differs from previous reports in that the mean ICC agreement in our study ranged from poor to moderate (−0.25 to 0.43) for all domains. In contrast, previous research has reported moderate-to-good agreement (0.52–0.72;Reference Berkes, Pataki and Kiss 8 0.41–0.61Reference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 , Reference Berkes, Pataki and Kiss 8 ) between parent and child quality-of-life reports. The lower ICC agreement observed in our study may be due to the smaller number of participants. In our study, the upper limit of the 95% CI for the ICC values for quality of life ranged from 0.51 to 0.64, suggesting that if our study was repeated the level of parent–child agreement could be similar to previous reports. On the other hand, the more moderate parent–child agreement observed in our study may also reflect improved surgical outcomes in the 5–10 years since the previous reports; one could hypothesize that as surgical outcomes improve parents would observe fewer physical differences between their child with a cardiac diagnosis and healthy peers, leading to high ratings of physical quality of life for all patients. In contrast, data indicating the long-term impact of psychosocial health challenges among paediatric cardiac patientsReference Bromberg, Beasley, D’Angelo, Landzberg, DeMaso and Massachusetts 1 , Reference Kim 4 suggest that children may continue to perceive that they have a lower psychosocial quality of life. In combination, these trends would lead to greater parent–child agreement for measures of physical quality of life with greater parent–child discordance among psychosocial quality-of-life measures that may be more difficult to observe. These results highlight the need for clinicians to monitor child self-reported quality of life in addition to parent proxy reports.
Greater agreement for observable psychosocial health indicators
To our knowledge, similar comparisons of Behavioral Assessment Scale for Children (Version 2) psychosocial health reports from paediatric cardiac patients and their parents have not been previously investigated. Our study found a strong correlation (R=0.70) and good agreement (ICC=0.72) between parent and child reports for the more observable “externalising/hyperactivity” domain compared with the internalising domain (R=0.17; ICC=0.14). The externalising/hyperactivity domain includes behaviours such as aggression, hyperactivity, and conduct problems. The internalising domain is comprised of anxiety, depression, and withdrawal. Our results are similar to data for healthy children – R=0.40 for Behavioral Assessment Scale for Children (Version 2) externalising/hyperactivity, R=0.29 for internalisingReference Reynolds and Kamphaus 28 – and mirror our findings for measures of quality of life. Despite a smaller sample size, parent–child agreement in our study was much stronger (n=50, R=0.70) across observable domains than in the normative population (n=871, R=0.40, z=2.96, p=0.003). Correlations for internalising problems among our child–parent dyads were not significantly different from published normative data (z=0.85, p=0.20). Perhaps this is related to parents of cardiac patients being hyperaware of their child’s physical status, possible cardiac symptoms, and, by extension, their child’s externalising behaviours.
Greater parent–child discrepancy for young children
Our initial regression analysis, using age as a continuous variable, did not show a significant effect of age, sex, or city/clinic on parent–child agreement for responses on the Pediatric Quality of Life Inventory or Behavioral Assessment Scale for Children (Version 2) questionnaires. This differs from trends described in the literature by age group, when age is reported as a categorical variable (young child; child; adolescent). In order to compare our results with previous studies, we completed a secondary analysis of our data to examine the impact of age group. We found that the magnitude of parent–child differences for our quality-of-life and psychosocial health indicators were greater for young children, compared with older children or adolescents. Our results are similar to data from healthy children, which found greater parent–child agreement for psychosocial quality of life among children aged 7.5–8.5 years, compared with younger children (5.5–7.5 years).Reference Cremeens, Eiser and Blades 16 These results are in contrast with data from cardiac children, which reported greater parent–child agreement for quality-of-life scores among children aged 8–12, compared with younger (5–7 years)Reference Berkes, Pataki and Kiss 8 and older (13–18 years) children.Reference Uzark, Jones, Slusher, Limbers, Burwinkle and Varni 5 , Reference Berkes, Pataki and Kiss 8 These age-related results may reflect the limited ability of young children to identify and express their concerns and/or a decreased desire for communication with parents during adolescence. That we did not observe a discrepancy in the reports provided by older child or adolescent patients and their parents may indicate that more effective communication regarding quality of life and psychosocial health occurs once children are old enough to express their concerns, and/or adolescents gain better insight through maturation and development.
Parent–child agreement not influenced by the child’s sex
There were no effects of the child’s sex on quality of life and psychosocial health outcomes assessed during our study. Future research to examine the impact of parent–child relationships, mothers or fathers as proxy raters, and parents’ own quality of life on parent–child agreement is recommended to fill this knowledge gap
Strengths and limitations
The results from our study must be interpreted in light of the strengths and limitations of our study design. We investigated the quality of life of children seen in a cardiac clinic and found discrepancies between the perspectives of parents and the children themselves. Our study has confirmed previously reported differences for measures of quality of life, and has extended current knowledge by evaluating parent–child discrepancies across a broader scope of psychosocial health using multiple standardised measures. The diverse cardiac diagnoses among our 50 patients and their families suggest that our results are likely to represent the spectrum of patients seen in a paediatric cardiac clinic. It is unknown whether parent–child discrepancies would be different among participating families in comparison with families who did not participate in the study. As the majority of participants were patients who had surgical interventions for structural cardiac diagnoses, multi-institutional studies that can recruit a larger population of patients with rhythm, infectious, or functional cardiac issues are recommended to increase generalisability.
Direct child–parent comparisons could be made for the Pediatric Quality of Life Inventory. The Behavioral Assessment Scale for Children (Version 2) was administered only to children in Toronto, limiting comparisons with this instrument to 19 parent–child dyads (Table 4). At the time of data collection, the Multidimensional Anxiety Scale for Children was only available in the child report form, limiting our ability to directly compare parent and child perceptions of the child’s anxiety. The wide confidence intervals found for some of our study results reflect our relatively small sample size. Future studies of psychosocial health, in addition to quality of life, require a larger sample in order to more definitely determine the magnitude of the differences between child self-reports and parent proxy reports.
Although an incidental finding, it is important to reiterate that 10% (n=5) of our patient study population required further psychological assessment due to concerning answers on quality of life and psychosocial health instruments. Such findings illustrate the importance of clinical assessments of the psychosocial health of paediatric cardiology patients and research on parent and child perceptions of the child’s emotional health.
Conclusion
Our study found stronger parent–child agreement for more observable parameters, including physical functioning, school functioning, social functioning, and externalising behaviours. This pattern was consistent with data for healthy children and previous reports of quality of life among the paediatric cardiology population. Parent–child agreement was lower for parameters that are more difficult to observe, such as emotional functioning, internalising behaviours, and anxiety. Our data highlight that clinicians should speak with both paediatric cardiac patients and their parents in order to more accurately assess the psychosocial health and emotional quality of life of their patients.
Acknowledgements
The authors thank all the patients, families, and clinicians involved in this research from the Children’s Hospital of Eastern Ontario and The Hospital for Sick Children. The authors also acknowledge Dr Gary Goldfield and Marissa Murray for providing additional psychological support to study participants when indicated by the assessment results, and Dr Nick Barrowman for his statistical expertise and opinion.
Financial Support
The work of B.P. was financially supported by the Mach-Gaensslen Foundation of Canada through the University of Ottawa Faculty of Medicine Studentship and by the University of Ottawa Undergraduate Research Opportunity Program.
Conflicts of Interest
None.
Ethical Standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national guidelines on human experimentation (Canadian Tri-Council Policy Statement – 2) and with the Helsinki Declaration of 1975, as revised in 2008. The study was approved by the institutional review boards (Research Ethics Boards) of the Children’s Hospital of Eastern Ontario and The Hospital for Sick Children.







