Introduction
It is widely accepted that near-miss and adverse events occur during the process of delivering care to patients in the in-hospital setting.Reference Kohn, Corrigan and Molla 1 , Reference Baker, Norton and Flintoft 2 Some of these events can likely be attributed to lapses in paramedic judgment and decision-making.Reference Graber, Franklin and Gordon 3 - Reference Calder, Forster and Nelson 5 As with other health professions, it is important to understand how paramedics make decisions so that adverse events related to clinical judgment can be reduced or prevented.
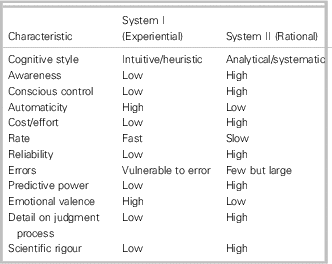
The leading theory to explain how clinicians engage in clinical decision-making is the Dual Process Theory.Reference Norman 6 Dual Process Theory suggests that decisions are made using one of two thinking systems (Table 1). System I is rapid and subconscious, and is often referred to as intuitive or experiential thinking. System II is conscious and deliberate, and is often referred to as rational thinking.Reference Croskerry 7 The Rational Experiential Inventory-40 (REI-40) is a psychometric survey tool developed to identify thinking style preferences.Reference Pacini and Epstein 8 The REI-40 is designed to measure ability to use and favourability towards each of the two major styles of decision-making: experiential (Type I) and rational (Type II).
Table 1 Dual Processing Theory of clinical decision-making (adapted from Croskerry, 2009Reference Croskerry 7 )
Clinical decision-making styles have been studied in a number of populations, including United States university students,Reference Pacini and Epstein 8 New Zealand cardiologists,Reference Sladek, Bond and Huynh 9 and Canadian emergency physicians,Reference Calder, Forster and Stiell 10 but to date decision-making styles have not been studied in paramedics or paramedic student populations. Paramedic clinical decision-making is arguably unique compared to other professions, as paramedics practice in variable locations, are presented with a wide variety of unpredictable patient conditions, and often have few resources other than their partner. Moreover, how paramedics make decisions may play a large role in the safety and effectiveness of the care they deliver.Reference Bigham, Maher and Brooks 11 Paramedics may tend to use one thinking strategy more than the other in most circumstances. For example, when presented with a middle-aged male with flank pain, a paramedic may employ experiential or intuitive thinking by immediately assigning a working diagnosis of renal colic through matching the patient’s presentation to an illness script developed from previous observations of similar patients. Another paramedic, faced with the same patient, may tend more towards rational thinking, consciously working through other alternatives, such as aortic aneurysm, before assigning a provisional diagnosis and commencing down a treatment path. Given the increasing scope of paramedic practice 12 and expanded roles and settings in which paramedics can now work (for example, involving community paramedicine initiatives),Reference Jensen, Travers and Bardua 13 understanding how paramedics think and whether thinking styles change with work experience has the potential to help inform early and ongoing education and the development of paramedic training modules and clinical aides.
The objective of this study was to determine paramedic and paramedic student preferences toward, and perceived ability to use, experiential and rational thinking styles, and to determine whether thinking styles differ between these two groups.
Methods
Study design
A cross-sectional paper-based survey was undertaken in Nova Scotia, Canada, to determine decision-making styles of two populations: 1) working ground ambulance paramedics, and 2) student paramedics at entry to practice level. The study was reviewed and approved by the Capital District Health Authority Research Ethics Board and the research ethics boards of participating paramedic colleges. Consent to participate was implied through submission of completed or partially completed surveys.
Study setting and population
Emergency medical services (EMS) in the study region is delivered by a single service with an annual call volume of approximately 70,000 calls, involving approximately 1,100 registered ground ambulance paramedics, who serve an a urban, suburban, and rural population of approximately one million people. EMS staff in the study region consisted of primary care paramedics (PCPs, 49%), intermediate care paramedics (ICPs, 12%), and advanced care paramedics (ACPs, 39%). The survey was administered to paramedics at mandatory in-service classroom professional development sessions held between May 1 and June 15, 2012.
PCP students from 15 colleges in Nova Scotia, New Brunswick, and Ontario were invited to participate in the study during their last week of training in 2013. Approximately 375 students were registered in PCP programs at the time of the survey.
Potential participants were given a survey and a blank envelope. Trainers or school faculty members distributed the surveys using scripted instructions. Surveys were sealed in the envelopes by participants, and were then mailed directly to the principal investigator, ensuring that trainers and faculty remained blinded to the participation decision of any specific individual.
Study protocol
Permission for use of the REI-40 was obtained from the developer (personal communication, Dr. S. Epstein, January 21, 2012).
The survey instrument consisted of demographic questions and the REI-40. The REI-40 is a psychometric tool that has been validated to identify thinking styles in several populations to assess thinking strategy and preferences. The REI-40 has been found to be reliable (Cronbach’s alpha 0.74–0.91) and consistent.Reference Pacini and Epstein 8 , Reference Calder, Forster and Stiell 10 , Reference Björklund and Bäckström 14 - Reference Shiloh, Salton and Sharabi 16 It involves 40 questions that are scored on a five-point Likert scale from “Definitely False” to “Definitely True.” Twenty of these questions assess each thinking style (rational or experiential), of which 10 assess favourability towards a style and 10 assess ability to use a style. Higher scores indicate a higher affinity for the style in question. Participants were instructed to consider decisions made in their EMS clinical work rather than in their general everyday life (see Appendix). The English survey was translated to French by a professional translator and participants in bilingual regions were free to choose the language in which they preferred to respond.
The survey was pilot tested with 24 paramedics for face validity and was found to require approximately 15 minutes to complete. Based on pilot testing feedback, minor revisions were made to the demographic questions and format. Data were entered by a single investigator (AB) for the working paramedic group and by a research assistant for the student group. Every tenth record was checked against the original by another investigator (JLJ) for accuracy of data entry.
Data analysis
The REI-40 was scored based on a coding manual provided by the lead investigator of the instrument (personal communication, Dr. S. Epstein, February 21, 2012). Coding included identifying the questions which addressed each of: Rational Ability, Rational Favourability, Experiential Ability, and Experiential Favourability (10 questions each). The responses for negatively-worded questions were reverse scored. The responses for questions in each category were summed and divided by 10 for the average score for each participant for each category. Analysis included descriptive statistics and t tests to determine differences in overall thinking style scores within and between groups. Within each group, differences in favourability towards and ability to use each style were also evaluated with t tests. If more than three responses per set of 20 questions for a thinking style were missing in a survey, that survey was excluded from analysis. For surveys with three or fewer missing responses per set of thinking style questions, any missing responses were replaced with the mode of the remaining responses for that style (personal communication, Dr. S Epstein, July 30, 2012). Differences in thinking styles within demographic variables were evaluated with t tests and ANOVA. Significance (p value) was established at 0.05 for all tests, with corrections for multiple comparisons (with Hochberg’s GT2 procedure for categories with different sample sizes, and Games-Howell procedure for uncertainty of population variances of categories as appropriate), and the most conservative resulting p values were reported.
Results
Paramedics from the aforementioned single EMS service and paramedic students from fifteen colleges participated, with a response rate of 1172/1263 (88.4%) (Figure 1). 1,206 surveys were received, including 32 that had missing data and were excluded (2.6%) and two where the respondents indicated they did not wish to participate. During data quality review, 10 records of 117 (8.5%) had minor data entry errors, which were corrected.

Figure 1 Flow of working paramedic and student paramedic survey responses. N: number.
Paramedic student participants were younger than paramedic participants; there was a higher percentage of female participants among students than among paramedics. Of the paramedic participants (n=904), most were male (69.5%), the median age was 36, most were PCPs (55.5%) and ACPs (32.5%), and the median years of experience was 10 years (Table 2). Among student paramedic (n=268), the median age was 23 years, most were male (63.1%), most completed their training in Ontario (76.1%), and most had completed high school (31.7%) or an undergraduate degree (25.4%) prior to paramedic training.
Table 2 Characteristics of working paramedic and student paramedic participants.

* Urban, rural, and mixed settings were self-identified by participants.
n: number
Overall, paramedics scored questions on rational thinking style higher than experiential thinking style (3.86/5 vs. 3.41/5, p<0.001), perceived that they were better able to use rational thinking than experiential thinking (3.93/5 vs. 3.60/5, p<0.001), and indicated that they preferred to use rational thinking over experiential thinking (3.79/5 vs. 3.22/5, p<0.001) (Table 3). Paramedics who were male (p=0.02), younger (p<0.001), Advanced Care Paramedics (p=0.001), or had fewer years working experience (p=0.001) or years since last training (p<0.001) and who worked in urban or a mix of urban-rural settings (p=0.001) scored higher on rational questions than their counterparts. No differences were found between demographic strata in rational thinking scores categorized by the type of paramedic training completed or hours worked per week. There were no differences found between strata in any demographic for scores on experiential thinking. (Table 4)
Table 3 Mean rational and experiential scores, mean rational and experiential ability scores, and mean rational and experiential favourability scores by working paramedics group and student paramedics group.
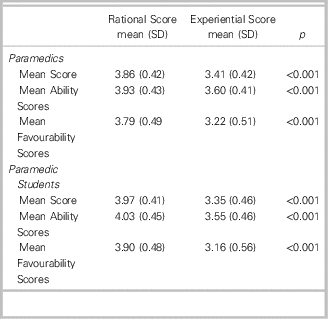
Calculated with single sample t tests.
SD: standard deviation
Table 4 Mean rational and experiential scores by working paramedics group and student paramedics group; and gender and age data for all study participants.
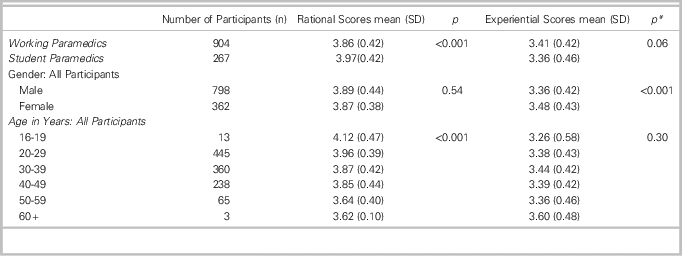
Compared with independent samples t test.
n: number; SD: standard deviation
* Equal variances not assumed.
Overall, paramedic students also scored rational thinking style questions higher than experiential thinking style questions (3.97/5 vs. 3.35/5, p<0.001), perceived that they were better able to use rational thinking than experiential thinking (4.03/5 vs. 3.55/5, p<0.001), and indicated that they preferred to use rational thinking over experiential thinking (3.90/5 vs. 3.16/5, p<0.001). Rational thinking style questions were given higher scores by paramedic students who were younger (p=0.04) and who had more prior education (p<0.01) compared with their counterparts. Similar to the situation with paramedics, no differences were found between any demographic for experiential thinking scores.
When all participants’ scores were grouped for age and gender, no difference was found in rational thinking scores between males and females (p=0.54). Males were found to score experiential thinking lower than females (p<0.001). Younger participants were more likely to score rational thinking higher than older participants (p<0.001); however, no difference was found in experiential thinking scores by age (Table 5).
Table 5 Rational and experiential scores among demographic strata by working paramedics group and student paramedics group.

n: number; SD: standard deviation
Discussion
In this study we used the REI-40 to determine paramedic and paramedic student preferences toward and perceived ability to use experiential and rational thinking styles in the context of their clinical work, and to determine whether thinking styles differed between these two groups. Scores for rational thinking were higher than experiential thinking in both groups, suggesting that both paramedics and paramedic students perceived that they had the ability to use rational more than experiential thinking and that they preferred rational over experiential thinking. Our results are consistent with studies involving cardiologists and emergency physicians (Table 6).Reference Sladek, Bond and Huynh 9 , Reference Calder, Forster and Stiell 10 However, our results differ from American college students, who were found to score higher on experiential thinking.Reference Pacini and Epstein 8
Table 6 Results of the REI-40 by study groups (Nova Scotia ground ambulance paramedics and student paramedics in Nova Scotia, New Brunswick, and Ontario) and other studies (Ontario emergency physicians, New Zealand cardiologists, and United States college students).
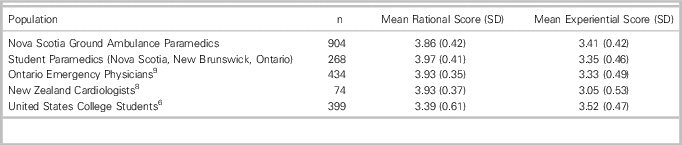
n: number; SD: standard deviation
In this study, both participant groups scored experiential and intuitive thinking higher than the mid-point of the scale, indicating they likely used both thinking strategies. The Dual Processing Theory suggests that System II (rational) thinking may have a “supervisory” role over System I (experiential), and that clinicians with critical thinking move between the two systems efficiently, a skill that has been described as the ability to “calibrate” one’s thinking.Reference Croskerry 7 A similar activity has been postulated in nurses, a group that has traditionally viewed intuition to be a hallmark trait of expert clinicians,Reference Carper 17 - Reference White 19 although a recent review found that nurses placed equal emphasis on experiential and rational thinking and concluded that nurses likely use a mix of both styles in practice.Reference Paley, Cheyne and Dalgleish 20
While it is unknown specifically which thinking style or particular strategy is superior for different clinical situations, paramedics and paramedic students can become more aware of their thinking style and can be trained in the benefits and pitfalls of each thinking style.Reference Graber 21 , Reference Ericsson, Nandagopal and Roring 22 Errors in the decision-making process represent a threat to the delivery of appropriate prehospital care and thus a threat to patient safety.Reference Hagiwara, Suserud and Andersson-Gare 23 We feel that training on the decision-making process and thinking styles should be included in the National Occupational Competency Profile, a resource that defines the required content for foundational paramedic training in Canada. 24 Clinical decision-making education modules could include topics such as understanding meta-cognition and the Dual Processing Theory, understanding and appropriate use of various decision-making strategies (ranging from exhaustive to ruling out the worst case scenario to algorithmic), awareness of cognitive biases, and ensuring knowledge of cognitive error–avoiding strategies.Reference Croskerry 25 , Reference McGregor, Paton and Thomson 26 Similarly, continuing education opportunities for paramedics could include clinical decision-making. Case presentations are a common quality assurance practice in many EMS services and are suitable for adaptation to a “cognitive autopsy” style of case review, which includes a focus on the thinking strategies used and the internal and external factors that may have affected paramedic decision-making.Reference Croskerry 25 Simulation, another common continuing education tool for paramedics, could be structured such that selected simulated cases were run as “think aloud” scenarios. In such an approach, participants are prompted to stop at each decision point and discuss the decision made, why they made it, and what thinking strategy was used.Reference Skånér, Backlund and Montgomery 27 Strategies of this nature have the potential to raise paramedics’ awareness of their own thinking and cognitive errors. Our findings and their implications may be particularly timely given the increasing paramedic scope of practice in Canada, expanded scope roles, and movement away from linear algorithms in favour of guidelines.Reference Jensen and Dobson 28 - 31
The differences we found in scores between groups and between the demographic strata of each group suggest that preferences toward and ability to use each thinking style may evolve with age. Rational thinking scores were higher in the student paramedic group than the working paramedic group. In the working paramedic group, rational scores were higher among those who were younger, ACPs, working in urban or mixed urban-rural environments, and who had fewer years working experience. These findings may be attributable in part to more previous education (e.g., undergraduate degrees) and ACP training among younger paramedics—both of which emphasize decision-making skills—and the increased likelihood of working in an urban area when beginning a career in paramedicine. Alternatively or in addition, they may reflect a secular change in the nature of paramedic education. In contrast with a previous study wherein female health care professionals were found to score higher on experiential thinking than their male counterpartsReference Calder, Forster and Stiell 10 , we found that male paramedics scored experiential thinking higher than did females, suggesting that male paramedics tend more towards intuitive thinking. This finding could, however, be a function of experience rather than gender, as there were more male paramedics in older age groups and with more years of EMS experience than females. Our findings are important to consider in paramedic continuing education and the design of cognitive aids, as they suggest paramedics do not uniformly tend to value or use an identical thinking strategy. This finding provides further support for the notion that incorporating awareness of decision-making into paramedic clinical education may provide an essential awareness that helps practitioners refine their own cognitive practices.
Limitations
The most significant limitation of this study is that REI-40 captures self-reported perception of ability to use, and preference toward, rational and experiential thinking, and may therefore not be an accurate representation of thinking style in actual clinical settings. Unlike other tools, such as pain scales, a meaningful important difference in scores has not been established for the REI-40; as a result it is difficult to know whether the differences in scores in our study represent an important difference in thinking. For this reason, we provided comparison scores from other populations to give readers further context. Other potential limitations include response bias, such that some paramedics and paramedic students may have answered questions in the way they felt was socially desirable, or they felt investigators wished them to respond, or the way that was impressed upon them in their educational setting. However, we believe the effect of response bias would be minimal, as participants were not provided with any training in decision-making theory prior to completing the survey. Paramedics and students were clearly instructed that their participation was voluntary; however, our high response rate could suggest paramedics may have completed the survey simply because it was delivered during a professional development session, and paramedic students may have completed the survey because it was distributed during class time. We carefully inspected all received surveys for any comments indicating the paramedic or student did not voluntarily agree to participate, and as a result two participants were excluded. Differences existed in demographic characteristics between the paramedic and paramedic student groups regarding gender, age, and training. It is possible that one or more of these factors had a significant influence on reported thinking style, rather than work experience, and our lack of a multivariate analysis methodology makes it impossible to determine whether or not this is the case. The working paramedic sample was entirely from Nova Scotia, potentially limiting the generalizability to paramedics trained in and working in other systems. While we do not believe there are significant differences with other Canadian paramedics, it is possible that recent focus on clinical practice guidelines and other related topics in the targeted study setting may have affected responses from our paramedic sample. The majority of paramedic students in our study population were from Ontario and had not been exposed to the Nova Scotia EMS system, so it is noteworthy that they scored rational thinking higher than the working paramedic group. This may suggest that rational thinkers self-select to become paramedics, regardless of setting.
Future studies could focus on determining how to assess decision-making in training, identifying the optimal thinking style for specific clinical scenarios, identifying the thinking style and other characteristics of paramedics who are expert practitioners, determining if paramedics can be taught these optimal thinking strategies to apply to given clinical scenarios, and the development of cognitive aids tailored towards specific thinking styles.Reference McGregor, Paton and Thomson 26 , Reference Jensen and Dobson 28 , 31 , Reference Ericsson 32
Conclusion
In this cross-sectional survey of ground ambulance paramedics in a provincial EMS system and primary care paramedic students at entry to practice level, we found paramedics and paramedic students prefer and perceive that they have the ability to use rational over experiential thinking. This information adds to our current knowledge on paramedic decision-making and is potentially important for developing continuing education and clinical support tools.
Competing Interests: None to declare.
Supplementary Material
To view supplementary material for this article, please visit http://dx.doi.org/10.1017/cem.2015.95









