CASE HISTORY
A 14-year-old male presented to the pediatric emergency department (ED) with a chief complaint of changes to his tongue. He described a 3-day history of a gradually worsening sore, swollen tongue associated with a white plaque. This was accompanied by a 3-day history of a gradually worsening left-sided facial rash that had an intermittent mild tingling sensation. He also had a 1-week history of a productive cough with yellow mucus and generalized malaise. He had been seen at a walk-in clinic 2 days prior to presentation and was prescribed amoxicillin for presumed pneumonia, which he began the same day. He denied any history of fevers, facial weakness, neck stiffness, or eye symptoms. He was an otherwise well child, with up-to-date immunizations and a past medical history of chickenpox and recurrent furuncles as a younger child.
On examination, he appeared well with the following vital signs: blood pressure 122/64 mm Hg, heart rate 73 beats per minute, respiratory rate 18 breaths per minute, temperature 36.8°C, and oxygen saturation of 99% on room air. Examination of his tongue revealed a symmetric white plaque along with ulcerative lesions on the left tongue and buccal mucosa (Figure 1). Head and neck examination revealed a left-sided facial vesicular rash, extending from the corner of the mouth to the ear (Figure 2). There were no lesions surrounding the eye or within the external auditory canal. Respiratory examination revealed a mild right-sided wheeze. Cardiovascular, abdominal, and neurological (including cranial nerve) examinations were unremarkable.
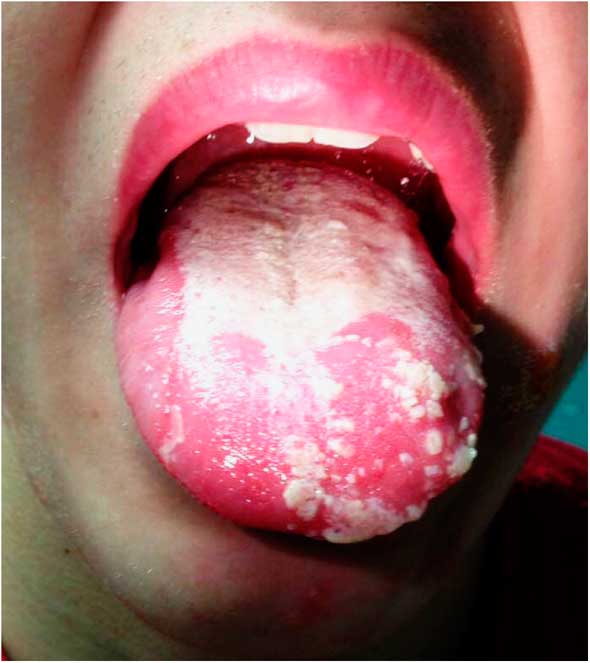
Figure 1 Leukoplakia and ulcerative lesions on tongue.
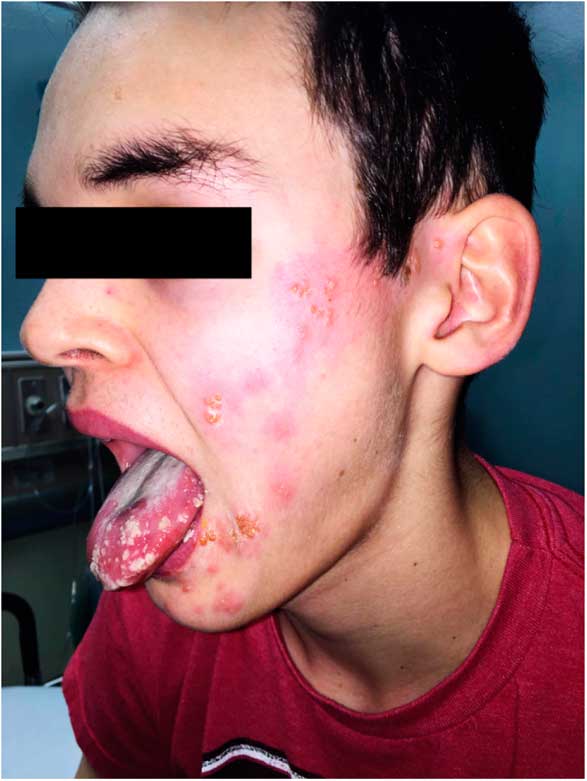
Figure 2 Facial rash extending from corner of mouth to ear.
What is the most likely diagnosis?
-
a) Drug eruption
-
b) Varicella zoster virus (VZV)
-
c) Oral candidiasis
-
d) Epstein-Barr virus
-
e) Oral lichen planus
Answer: This patient’s history and physical examination are consistent with a VZV infection, manifesting as herpes zoster (HZ). HZ (shingles) is caused by reactivation of latent VZV in the cranial nerves or dorsal root ganglia, and most commonly presents as an erythematous vesicular rash grouped along a sensory dermatome.Reference Steiner, Kennedy and Pachner 1 VZV can also manifest as a primary infection, commonly referred to as varicella (chickenpox), which classically presents as a diffuse vesicular rash over the face, trunk, and extremities.
HZ most commonly affects older adult patients or those with some form of immunodeficiency, but is also seen in the otherwise healthy pediatric population. A recent U.S. studyReference Weinmann, Chun and Schmid 2 found an incidence of 112 per 100,000 person-years in children ages 0 to 17 years. HZ can be caused by both wild-type VZV and vaccine-strain VZV; however, vaccinated children have a lower incidence rate of zoster than unvaccinated children.Reference Weinmann, Chun and Schmid 2 Reference Wen and Wen-Liang - Reference Feder and Hoss 4 There also appears to be a higher risk of developing zoster if varicella is contracted in the first year of life.Reference Wen and Wen-Liang 3 , Reference Feder and Hoss 4 Unlike the adult population, pediatric zoster is associated with minimal pain on initial presentation and is rarely complicated by postherpetic neuralgia. It most commonly affects the thoracic dermatomes, with 5% of cases involving cranial nerves.Reference Feder and Hoss 4
The facial rash in this case presentation was consistent with HZ, given the grouped vesicles spread along the maxillary (CN V2) and mandibular (CN V3) divisions of the trigeminal nerve (CN V). However, the leukoplakia remained more of a diagnostic challenge. Although the left-sided facial rash pointed us towards a diagnosis of zoster, the symmetry of the leukoplakia was puzzling; this prompted consideration of the differential diagnosis of leukoplakia (Table 1) and a review of the cranial nerve innervation of the tongue. As shown in Figure 3, the lingual nerve, a branch of the CN V3, supplies sensory innervation to the anterior two-thirds of the tongue. This explains the potential for spread of lesions to the tongue in a VZV infection of the CN V. Anterior tongue involvement can also occur in VZV affecting the facial nerve (CN VII) and has been previously documented in case reportsReference Lee and Baek 10 - Reference Neagu and Prasad 13 of the Ramsay Hunt syndrome (further discussed after the following paragraph).

Figure 3 Cranial nerve innervation of the tongue.
Table 1 Differential diagnosis of oral leukoplakia, and oral lesions that can mimic leukoplakiaReference Gonsalves, Chi and Neville 5 - Reference Siu, Landon and Ramos 9

In this case, on careful inspection, the ulcers were more prominent in the anterior left tongue, with secondary leukoplakia developing. A review of the literature did not reveal any published statistics on the frequency of associated leukoplakia in VZV infections of the trigeminal nerve (specifically, CN V3). Part of this may be due to varying definitions of leukoplakia amongst clinicians (as a descriptive term versus a specific diagnosis); however, it is known that mandibular nerve involvement of VZV can result in ulcerative lesions appearing on the tongue, buccal mucosa, and gingival.Reference Mangold, Torgerson and Rogers 14 Confluent ulcerations or vesicles can often appear similar to leukoplakia, and, in fact, there is a case reportReference Braverman, Uri and Greenberg 15 of VZV affecting the trigeminal nerve in which the tongue was unilaterally affected by white ulcerations, in a manner somewhat similar to this patient’s presentation.
For any patient with a suspected zoster infection involving the head and neck, it is important to rule out HZ ophthalmicus (infection of the ophthalmic nerve branch, CN V1). Evaluation for visual symptoms, lesions around the eye, and lesions around the nose (Hutchinson sign) is crucial. It is also important to look for conjunctival injection and edema, because conjunctivitis is one of the most common presentations of HZ ophthalmicus.Reference Shaikh and Ta 16 If ophthalmic nerve involvement is suspected, a thorough eye exam with ophthalmology consultation is warranted.Reference Shaikh and Ta 16 It is also important to evaluate the patient for facial paralysis, lesions within the ear canal and adjacent skin, otalgia, and hearing loss. These symptoms can indicate HZ oticus (also known as Ramsay Hunt syndrome), which arises from VZV infection of the CN VII. The geniculate ganglion of CN VII has two major sensory branches; the first is responsible for taste sensation to the anterior tongue via the chorda tympani, and the second supplies sensation to the external auditory canal and pinna.Reference Grose, Bonthius and Afifi 17 Ramsay Hunt syndrome is managed with a course of acyclovir, as well as corticosteroids (such as prednisone) in severe cases.Reference Feder and Hoss 4
Our patient was treated as a HZ infection involving CN V2 and V3, and was given a 7-day course of acyclovir 800 mg five times daily. His oral antibiotics were discontinued because his chest radiograph was clear. Given his wheeze, a component of asthma was suspected and Ventolin was trialed with success. Initiation of oral antibiotics 2 days prior to presentation to the ED was likely appropriate given his productive cough, auscultatory finding presumably consistent with pneumonia, and absence of significant facial findings at that time. He was seen in follow-up by our pediatric infectious disease specialist several days after initial presentation, by which time the facial lesions were already crusting over. Swabs taken of a vesicular lesion on his face returned positive for VZV via polymerase chain reaction (PCR) genotyping, confirming our diagnosis. He was seen again in follow-up 2 weeks later, by which time the tongue lesions had resolved as well.
Competing interests: None declared.






