CLINICIAN'S CAPSULE
What is known about the topic?
Methoxyflurane is an inhalation analgesic with minimal sedative properties.
What did this study ask?
What is the success rate of methoxyflurane for acute anterior shoulder dislocation reduction and its impact on emergency department (ED) patient flow, as compared with propofol?
What did this study find?
Successful reduction was achieved in 80% of patients administered methoxyflurane; recovery time and ED length of stay was shorter, as compared with propofol sedation.
Why does this study matter to clinicians?
Methoxyflurane can be used for acute anterior shoulder dislocation reduction prior to considering deep sedation and may improve ED patient flow.
INTRODUCTION
Shoulder dislocation is quite common and represents 50% of all joint dislocations.Reference Wakai, O'Sullivan and McCabe1, Reference Goldstein and Ghobrial2 Acute anterior shoulder dislocations (ASD) account for 95% of shoulder dislocations, commonly seen and managed by emergency physicians.Reference Wakai, O'Sullivan and McCabe1
Procedural sedation (deep sedation) is frequently used for ASD in the emergency department (ED); however, deep sedation can be associated with adverse events.Reference Weaver, Hauter, Brizendine and Cordell3 In the current climate of overcrowded EDs, carrying out deep sedation in a timely, safe, and effective manner can be difficult.
Over the last three decades, self-administered inhaled methoxyflurane has been used in Australia's pre-hospital setting as a form of analgesia. An improvement in the administration device, namely reducing the amount of methoxyflurane exposure to staff, has allowed its use in hospitals.Reference Coffey, Wright and Hartshorn4 Recent studies have shown its efficacy for performing procedures (colonoscopy and dental extraction), as it provides minimal sedation and good analgesia.Reference Abdullah, Sheta and Nooh5, Reference Nguyen, Toscano and Lawrence6
The major aim of this study was to evaluate the success rate of methoxyflurane for ASD reduction. The secondary aim was to assess the impact of methoxyflurane on ED patient flow measures such as recovery time and ED length of stay (LOS), as compared with deep sedation with propofol.
METHODS
Study design and setting
This was a health record review of all patients seen in the ED of a tertiary university hospital with an annual attendance of 65,000 patients. This study was approved by the Clinical Research Ethics Committee prior to data collection. Patients presenting with ASD to the ED from December 2016 (when methoxyflurane was introduced) to December 2017 were assessed.
Study population
Patients were included if methoxyflurane or propofol was used for shoulder relocation in the ED and patients more than 14 years of age. Exclusion criteria included patients with fracture dislocations, polytrauma, intravenous or intramuscular opioids in the pre-hospital setting, no sedation for reduction, and alternative techniques of sedation or analgesia for reduction. Patients having methoxyflurane for only analgesia without a reduction attempt prior to propofol sedation were also excluded.
Data collection
A standardized data report form was used for retrieving data from the online ED hospital records by trained data abstractors who were not blinded to the study objectives. The picture-archiving radiology system provided a list of all patients who had ASD, and their clinical and sedation records were reviewed. Basic demographic data such as age, gender, date, and mode of arrival were collected. Other variables collated included triage category, mechanism of injury, triage analgesia, sedation agent with doses, and procedural analgesia with doses.
Standard of care
The standards for sedation in our ED are in accordance with guidance from the Royal College of Emergency Medicine.7 All patients who necessitated reduction of ASD with sedation were managed and monitored in the resuscitation area following departmental procedural sedation guidelines with three staff members present. Patient education and use of methoxyflurane were as described by Abdullah et al.Reference Abdullah, Sheta and Nooh5 Choice of sedation method was left to the senior emergency physician based on personal preference and experience. The reduction technique was at the discretion of the treating physician. As per departmental policy, physicians adhered to a limit of two attempts at ASD reduction. Failure to achieve reduction obligated deeper sedation or analgesia, a change in sedation method, or occasionally full anesthesia.
Outcome measure and analysis
The primary outcome was the success of reduction for patients undergoing relocation with methoxyflurane or propofol as front-line agents. Secondary outcomes were recovery time (defined as the time from procedure onset to the post-reduction X-ray), ED LOS, and rate of adverse events (hypoxia, apnea, vomiting, hypotension, and requiring advanced airway management), as documented by physicians on hospital notes. Data analysis was performed using Microsoft Excel (Microsoft, Redmond, WA) and R Programming Language (version 3.4.0, 2018). Continuous variables are presented as mean (standard deviation) or median (interquartile range), and categorical variables are summarized as counts and percentages. The 95% confidence intervals (CI) were also calculated. Student's t-test and Mann-Whitney U test were used for comparisons of normally and non-normally distributed continuous data, respectively. Chi-Square and Fisher's exact tests were used for categorical data. A p value of <0.05 was considered statistically significant.
RESULTS
A total of 151 patients presented with ASD during the study period. Eighty-two patients were included in the study. Fifty-two patients underwent ASD reduction with propofol, and 30 patients had methoxyflurane. The patient characteristics and associated variables for both groups are shown in Table 1.
Table 1. Baseline characteristics
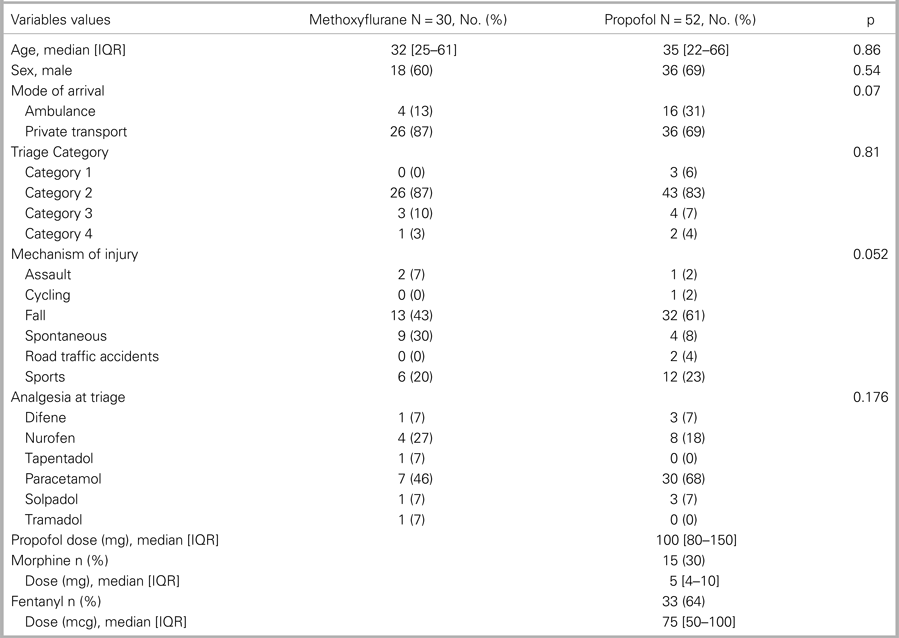
Methoxyflurane group
Successful reduction was achieved in 80% (95% confidence interval [CI] 65.69% to 94.31%) of patients who were administered methoxyflurane. Six patients failed reduction with methoxyflurane and required sedation with propofol (dose: median [interquartile range; IQR] 85 mg [55–100]) to achieve the reduction. The median recovery time was 30 minutes (IQR 19.3–44), and the median ED LOS was 70.5 minutes (IQR 49.3-105) for the methoxyflurane group for those who had successful reductions. No adverse events were documented.
Propofol group
In the propofol group, 98% (95% CI 94.2% to 100%) achieved successful reduction. Only one patient did not achieve reduction with propofol and was ultimately admitted for closed reduction under general anesthesia. The median recovery time for successful reductions was 47 minutes (IQR 32–68), and the median ED LOS was 135 minutes (IQR 77–211) in the propofol group. The median recovery time and ED LOS were longer in the propofol group, as compared with the MF group (p < 0.004 and p < 0.001, respectively). No adverse events were documented.
DISCUSSION
There is a paucity of data on the use of methoxyflurane for performing procedures in the ED, with only one observational case series reporting its use in a pediatric population.Reference Babl, Barnett, Palmer, Oakley and Davidson8 Abdullah et al. conducted a randomized, crossover study comparing methoxyflurane with nitrous oxide for dental extraction and reported similar levels of sedation and minimal adverse events with most patients stating they preferred methoxyflurane.Reference Abdullah, Sheta and Nooh5 When methoxyflurane was compared with conventional endoscopy sedation (midazolam plus fentanyl) for colonoscopies, significantly decreased anxiety scores, comparable procedural success, shorter recovery time, and high patient satisfaction scores were demonstrated.Reference Nguyen, Toscano and Lawrence6 In our study, methoxyflurane was used successfully in 30% of the 82 patients undergoing reduction for ASD. Methoxyflurane had a shorter recovery time and shorter ED LOS, as compared with the propofol group. It is normal practice in our department to have three staff members present for sedation, but as methoxyflurane is self-administered, we generally do not use an airway doctor (similar to reductions with nitrous oxide).
The limitations observed were partially because of the retrospective nature of this study and dependence on documentation by ED physicians. The use of methoxyflurane or propofol was at the discretion of the treating physician and may have led to selection bias. Because of extensive variations in reduction techniques available, we chose not to look at reduction techniques used for ASD. Certain factors such as measure of patient satisfaction on analgesia or amnesia were not assessed in this study. Future research is needed to further explore the impact of the reduction technique and cost analysis on the use of methoxyflurane for ASD. Prospective studies could also investigate both patient and physician factors that could influence the use of methoxyflurane in shoulder relocations.
CONCLUSION
Methoxyflurane was used successfully in 30% of the 82 patients undergoing reduction for ASD, potentially improving ED efficiency. Methoxyflurane could be used as the initial agent for reduction prior to considering deeper sedation.
Acknowledgements
EU, JHK, and BM conceived the study, designed, and secured ethical approval. The study was supervised by EU and BM, and data abstraction was carried out by CJB and JHK. EU and BM carried out the statistical analysis. EU drafted the manuscript, and all authors contributed to its revision. EU takes full responsibility for the paper. It was presented at the following meetings: University Hospital Galway Research Day, June 6, 2018; and the Irish Association of Emergency Medicine Annual Scientific Meeting, October 19, 2018. No grants have been awarded for this study.
SUPPLEMENTARY MATERIAL
The supplementary material for this article can be found at https://doi.org/10.1017/cem.2018.493.
Competing interests
None declared.



