Osteoporosis is a growing concern in both developed and developing countries. This situation is to some extent related to the increased longevity of the population. In the developing world, the growth of the general population as well as the life expectancy of the elderly is increasing dramatically. Women are four times more vulnerable to developing osteoporosis, as it is one of the serious physiological consequences of menopause. A decrease in the production of oestrogens during menopause triggers an accelerated rate of bone loss in women. Osteoporosis is a significant public health problem associated with increased mortality and morbidity. Recent studies indicate the growing prevalence of osteoporosis and osteoporotic fractures in developing countries and suggest that the situation be taken into account by improved health care planning(Reference Cooper, Campion and Melton1).
Two major determinants of osteoporosis are adult peak bone mass and the rate of bone loss during ageing. Earlier studies have found that a high adult peak bone mass is protective against late-life osteoporotic fractures(Reference Prince2, Reference Eastell3). Maximising peak bone mass during the first few decades of life is currently seen as a major strategy in osteoporosis prevention. Vitamin D (VD) is an important nutrient for bone metabolism. Despite abundant sunlight, the prevalence of hypovitaminosis D among women of reproductive age is unexpectedly high in Asian countries, and this problem remains a silent epidemic(Reference Islam, Lamberg-Allardt and Kärkkäinen4–Reference Islam, Shamim and Kemi8). Traditional concealment of the body with clothes, limited outdoor activity, high pollution levels and low dietary intake of VD and Ca may be the causes of the situation.
Bangladeshi women suffer from chronic nutritional deficiencies, especially in low-income families. The dietary intake of Ca in Bangladeshi women is typically low and far below recommended levels(Reference Jahan and Hossain9–Reference Islam, Lamberg-Allardt and Kärkkäinen11). Several studies indicate a positive effect of Ca and VD on bone mineral accretion in female adolescents and in young and postmenopausal women with adequate habitual dietary intake of Ca(Reference Lips, Wiersinga and van Ginkel12–Reference Zhu, Devine and Dick18). Data are scarce on VD, Ca and multiple micronutrient supplementation and its influence on bone mineral accretion at different sites in young premenopausal women accustomed to very low dietary intakes of Ca.
The present study was designed to examine whether the use of VD could affect VD status and bone mineral augmentation in low-income women with low dietary intake of Ca and whether more effective outcomes could be obtained using a holistic approach combining VD or multiple micronutrient with Ca. The effectiveness of these three treatment arms was determined based on changes induced in VD status and bone mineral accrual in the femoral neck and lumbar spine over a 1-year intervention period.
Subjects and methods
Study setting and subjects
A total of 200 subjects aged 18–36 years were studied in the Mirpur region of Dhaka city in central Bangladesh (latitude 20°43′–26°36′N and longitude 88°3′–92°4′E). The study setting was in an export-oriented garment factory located in an urban area belonging to Standard Group Bangladesh, which maintains a high-quality working environment for its workers. The participants were mainly young women from low-income rural families who had migrated to the city for employment at least 2 years earlier. Subjects live in an underdeveloped area in low-cost accommodation close to their working place. They work from dawn to dusk, 7 d/week, and wear concealing clothing with only their hands and faces remaining uncovered. The eligibility criteria for inclusion of subjects comprised no history of serious medical conditions, no history of medication known to affect bone metabolism, no current pregnancies, no lactation within the previous 3 years and residing in the city for at least 2 years.
Our first step was to contact the Chief Medical Officer of the Standard Group to explain the purpose of the study and to request his cooperation. We found him most co-operative. The medical assistant of the Standard Group and our two field assistants were also responsible for recruiting the subjects. They explain the objectives of the study to the subjects in an understandable way. Written informed consent was obtained from both interested subjects and the authority of the garment factory before initiating the study. The study protocol was approved by the Ethics Committee of the Faculty of Agriculture and Forestry, University of Helsinki. During the field study in Bangladesh, we also followed the ethical guidelines of the University of Dhaka.
Study design
The study comprised a 1-year, double-blind, placebo-controlled, randomised intervention trial. Participants were randomly assigned to one of the four groups after their eligibility had been determined at the screening; 200 women met all of the inclusion criteria. The recruitment and randomisation processes are presented in Fig. 1. Randomisation was performed for equal-size blocks and carried out by a person who was not involved in the project. The subjects received daily supplements of 10 μg of VD group, 10 μg of VD+600 mg of Ca as Ca-lactate (VD-Ca group), multiple micronutrients with 10 μg of VD+600 mg of Ca as Ca-lactate (MMN-Ca group) or a placebo (placebo group).

Fig. 1 Flow chart of the number of subjects recruited and dropping out. DEXA, dual-energy X-ray absorptiometry; VD, vitamin D; VD-Ca, VD and Ca; MMN-Ca, multiple micronutrient and Ca.
The composition of supplements comprising oral Ca tablets (‘G-Calcium’ from Gonoshasthaya Pharmaceuticals Limited, Dhaka, Bangladesh), MMN tablets (‘Aristovit M’ from Beximco Pharmaceuticals Limited, Dhaka, Bangladesh containing fifteen micronutrients) and VD tablets (‘Minisun’ from Oy Verman AB, Jarvenpaa, Finland) is shown in Table 1. Both Ca and VD placebos were donated by the same companies and were identical to the active tablets.
Table 1 Composition of supplements in the different groups
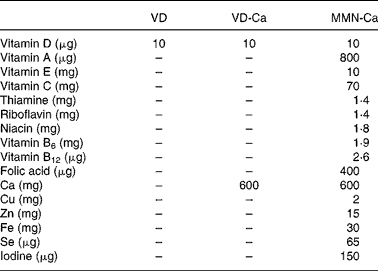
VD, vitamin D; VD-Ca, vitamin D-Ca; MMN-Ca, multiple micronutrient-Ca.
Subjects received their supplements daily from the field assistants for 12 months. The field assistants arrived at the garment factory every day (7 d a week) before the lunch break. Tablets were given to the subjects during their lunch break, inside the garment factory under the close observation of the field assistants. The field assistants always ensured that the tablets were swallowed with a glass of water, and they maintained a written daily record of supplement consumption for each subject. In case a subject was absent from work, supplements were given to their colleagues to deliver to their co-worker for consumption in the evening at home. The total time that the subjects spent outdoors in the sunshine was recorded daily.
On every working day, a small group of about ten subjects were brought in a minibus to the Centre for Nuclear Medicine and Ultrasound, Sir Salimullah Medical College, Mitford, Dhaka, where blood samples were collected. Background information, anthropometric and dual-energy X-ray absorptiometry measurements were carried out sequentially. Supplementation was started (in April 2004) sequentially based on completion of all measurements and continued for 12 months. We repeated the same process to collect the follow-up data.
Laboratory measurements
Blood samples were collected between 08.30 and 10.00 hours after an overnight fast. Five millilitres of venous blood were drawn using disposable syringes protected from sunlight. After clotting, the serum was separated by complete centrifuge of the blood sample. The serum was collected in tubes and preserved at − 20°C. Finally, the serum samples were transported to Helsinki in a special container with dry ice and preserved in the freezing room of the Division of Nutrition, Department of Applied Chemistry and Microbiology, University of Helsinki, at − 20°C until analysis.
Serum 25-hydroxyvitamin D (S-25OHD) was used to evaluate VD status. The concentration was determined by the enzyme immunoassay method with kits from OCTEIA (IDS, Boldon, UK). The laboratory is a partner of the VD External Quality Assessment Scheme, (www.DEQAS.org.uk). The intra-and inter-assay CV were 5·4 and 7·0 %, respectively. Serum intact parathyroid hormone (S-iPTH) level was measured with a commercial two-site immunoenzymometric assay (OCTEIA, IDS), with 10–65 ng/l as a reference range. Intra-and inter-assay CV for S-iPTH were 3·5 and 5·6 %, respectively. Serum levels of alkaline phosphatase activity, Ca, phosphate and creatinine were measured with an automated KoneLab spectrophotometer (Thermo Clinical Labsystems Limited, Espoo, Finland) using routine methods to obtain additional information about VD status. The inter-and intra-assay CV for these analyses were less than 7·5 %. The laboratory analysis was carried out at the Department of Applied Chemistry and Microbiology. We defined VD deficiency as S-25OHD levels < 25 nmol/l (reference range 25–120 nmol/l). We defined secondary hyperparathyroidism as S-iPTH levels >65 ng/l. Abnormally high values for serum variables were not included in statistical analysis. The study was conducted from April 2004 to April 2005.
Bone mineral density measurements
The measurements of bone mineral content and bone mineral density (BMD) of the left femur region and lumbar spine L2–L4 vertebrae (in anterio-posterior projection) were collected at the beginning and at the end of the study by a single trained X-ray technician using dual-energy X-ray absorptiometry DXA (Norland XR 36; Norland Corporation, Fort Atkinson, WI, USA). The femoral region included the femoral neck, trochanter and Ward's triangle. Calibration of the measurement was performed using a spine phantom; the inter-assay CV for the phantom was 0·45 %. Intra-assay CV were determined with duplicate measurements of ten subjects. CV for BMD in the left femur and lumbar vertebrae were 0·71 and 1·45 %, respectively.
Other data
Anthropometric, socio-economic and background data were collected at baseline and at the 1-year follow-up. A questionnaire was used to obtain information on level of education, age at menarche, duration of residence in the city, daily time spent outdoors, etc. Standing height was measured with a wall mounted scale to the nearest 0·5 cm. Body weight was measured without shoes and with light clothing on a portable weighing scale to the nearest 0·5 kg. We used the classifications of BMI (weight (kg)/height (cm2)) recommended by the WHO(19).
Statistical analysis
Statistical analyses were carried out with SPSS version 15.0 for Windows (SPSS, Inc., Chicago, IL, USA). Univariate analyses were performed for selected variables. The normal distribution of variables was assessed with a Kolmogorov–Smirnov test. If the data were not normally distributed, they were transformed before further analysis. Repeated measures ANOVA was used to detect the effect of supplementation on S-25OHD and S-iPTH. The post hoc tests were performed with Tukey's honestly significant different test and Dunnett's test. Bone data and other selected variables were tested with both ANOVA and analysis of covariance to show the effect of confounding factors. Comparison of groups in analysis of covariance was performed with contrasts, and for each analysis, covariates are mentioned in the footnotes. All data are reported as mean values and standard deviations; P < 0·05 was considered significant.
Results
Characteristics at baseline and at 1-year
Of the 200 subjects studied at baseline, 153 completed the 12-month intervention trial. A total of thirty-seven subjects (18·5 %) dropped out for reasons unrelated to the study. The number of subjects at various stages is shown in Fig. 1. Short stature was highly prevalent in the subjects, and BMI was close to the lower limit of the desirable range at both baseline and post-supplementation(19). No significant differences emerged in socio-economic, most anthropometric characteristics and daily time spent outdoors in the sunshine between the supplemented groups at either baseline or post-supplementation (all data not shown). A summary of the baseline descriptive and biochemical characteristics of the study population completing the trial is given in Table 2, and the change in these characteristics after 1 year is shown in Table 3. No significant group differences were present with respect to physical activity and education levels.
Table 2 Baseline characteristics of the randomly assigned groups
(Mean values and standard deviations)

VD, vitamin D; VD-Ca, vitamin D-Ca; MMN-Ca, multiple micronutrient-Ca; S-25OHD, serum 25-hydroxyvitamin D; S-iPTH, serum intact parathyroid hormone; S-Ca, serum Ca; S-P, serum phosphate; S-ALP, serum alkaline phosphatase activity; BMD, bone mineral density; BMC, bone mineral content.
Table 3 Change from baseline characteristics after 1 year

VD, vitamin D; VD-Ca, vitamin D-Ca; MMN-Ca, multiple micronutrient-Ca; S-25OHD, serum 25-hydroxyvitamin D; S-iPTH, serum intact parathyroid hormone; S-Ca, serum Ca; S-P, serum phosphate; S-ALP, serum alkaline phosphatase activity; BMD, bone mineral density; BMC, bone mineral content.
Mean values were significantly different with those of analysis of covariance using baseline value as covariate: * P = 0·020, ** P = 0·527.
Mean values were significantly different with those of analysis of covariance using baseline value and Δ weight as covariates: † P < 0·001, ‡ P = 0·205.
Effect of supplementation on serum 25-hydroxyvitamin D and intact parathyroid hormone
At baseline, 87 % of subjects had S-25OHD < 50 nmol/l, which is generally considered the lower limit of the desired range(Reference Vieth20–Reference Lips21). S-25OHD levels < 25 nmol/l, indicative of VD deficiency, were observed in twenty-two subjects in four groups, five in the placebo group, nine in the VD group, three in the VD-Ca group and five in the MMN-Ca group. No significant difference was seen in VD status among placebo and supplemented groups at baseline. After the 1-year intervention, significantly (P < 0·001) higher S-25OHD concentrations were observed in the supplemented groups than in the placebo group (Table 3). During post-supplementation, seven subjects in the placebo group were deemed VD-deficient (S-25OHD level < 25 nmol/l), whereas no subjects were deficient in the other groups. The mean concentrations of S-25OHD increased in the VD group by 32·2 (sd 23·7) nmol, in the VD-Ca group by 32·4 (sd 24·3) nmol and in the MMN-Ca group by 28·8 (sd 24·8) nmol, whereas in the placebo group the concentrations only increased by 0·6 (sd 13·8) nmol.
The overall response in S-iPTH to supplementation was significant (P < 0·05) in the VD, VD-Ca and MMN-Ca groups compared with the placebo group (Table 3). S-iPTH showed a strong negative correlation with S-25OHD at both baseline and follow-up (r − 0·20, P = 0·005; r − 0·28, P = 0·001, respectively). Both baseline and post-intervention data indicated that S-iPTH concentrations start to rise when S-25OHD levels fall below 40 nmol/l.
Effect of supplementation on bone mineral content and bone mineral density
Supplemented groups showed an increased femoral neck BMD and bone mineral content compared with the placebo group (analysis of covariance, P < 0·001). Bone mineral augmentation increased significantly at the femur after the 1-year supplementation (Table 3). We also observed a positive effect of supplementation on BMD and bone mineral content of the greater trochanter and Ward's triangle compared with the placebo group (analysis of covariance, P < 0·05). No significant difference was observed in BMD and bone mineral content of the lumbar spine (L2–L4) of the subjects at either baseline or the end of the study.
Discussion
VD is an integral part of Ca metabolism and bone mineralisation. Numerous studies have reported an effect of VD supplementation on VD and bone status among postmenopausal women(Reference Lips, Wiersinga and van Ginkel12–Reference Harris, Soteriades and Coolidge14, Reference Zhu, Devine and Dick18, Reference Cooper, Clifton-Bligh and Nery22), and a few studies have examined the effect of VD supplementation on VD and bone status among young women of child-bearing age. Such studies are of particular importance for low-income Bangladeshi women accustomed to low dietary intake of Ca(Reference Jahan and Hossain9, Reference Islam, Lamberg-Allardt and Kärkkäinen11), as they wear concealing clothes and have limited or no outdoor activities despite living in a sunny country.
We have investigated the effect of supplementation on S-25OHD levels and bone status among young women with hypovitaminosis D resulting from an exclusive indoor lifestyle and low dietary intake of VD. The dietary guidelines for Americans recommend that groups at risk for VD deficiency, including those exposed to insufficient UV radiation, people with dark skin and older adults, should consume 25 μg (1000 IU) VD daily(Reference Johnson and Kimlin23). Our data support VD and Ca supplementation in premenopausal women with an exclusive indoor lifestyle even in sunny countries such as Bangladesh. Our study showed that VD and Ca supplementation in these subjects is necessary to maintain normal S-25OHD levels, to augment bone gain and to maintain normal S-iPTH concentrations. Administration of Ca and VD supplements is well documented not only to inhibit bone resorption but also to reduce fractures. A recent study in elderly care residents revealed associations of supplementation of multiple micronutrients with increased S-25OHD levels, improved bone quality and less falls and fractures, probably due to increased muscle function(Reference Grieger, Nowson and Jarman24). Our study indicated that low-income female garment factory workers in Bangladesh are susceptible to osteomalacia or osteoporosis even at premenopausal age due to the high prevalence of hypovitaminosis D and a decreasing trend of bone status. However, earlier studies have also shown that declining levels of S-25OHD and increasing S-iPTH concentrations can start to exert adverse effects on bone mass before middle age by inducing endocortical bone resorption. The manufacture of garments is the main industry in Bangladesh, employing nearly two million young female workers. To the best of our knowledge, no study has reported the effect of VD supplementation on VD and bone status among Bangladeshi low-income young working women.
Research to date has indicated a direct relationship between VD and BMD as VD playing an active role in bone mineralisation(Reference Islam, Shamim and Kemi8, Reference Aguado, del Campo and Garcés25–Reference Suda, Ueno and Fujii27). Several studies have described an association of higher concentrations of S-25OHD with higher bone mineral parameters. Our results support these relationships. The improvement in VD status following supplementation observed here may be sufficient to promote bone health of the femoral neck. Research has generally indicated the threshold of S-25OHD levels to vary from 70 to 95 nmol/l for beneficial effects on bone metabolism in adults and the elderly(Reference Lips21, Reference Chapuy Preziosi, Maamer and Arnaud28, Reference Dawson-Hughes, Heaney and Holic29), whereas some studies have observed a positive effect on bone status in adolescents when the mean S-25OHD is >50 nmol/l(Reference Viljakainen, Natri and Kärkkäinen16). Based on our results, the following observations were made: compared with the placebo group, a 2-fold increase in S-25OHD levels and a significant decrease in S-iPTH levels occurred in the supplemented (VD, VD-Ca and MMN-Ca) groups. Our findings are consistent with the significant improvement in bone mass in the femoral neck in the supplemented groups of young women. Some studies have indicated that it may take 12 months or more to observe any significant changes in bone status. We therefore believe that the result could have been different for the lumbar spine (L2–L4) had we continued supplementation for an additional 1 or 2 years. Secondly, the complexity of studying the effects of supplementation on the lumbar spine are subjected to misinterpretations since the subjects must be measured in exactly the same geometric position at baseline and after supplementation.
Due to some technical limitations, we could not measure the dietary intake of Ca despite 3 d food records being completed. Moreover, dietary intake of VD was not taken into account, as the present food composition database does not include VD. We believe, however, that dietary intake of Ca should be considered when adequate VD status is defined(Reference Lips21). Bone biochemical markers could also provide us with additional information on VD and bone status.
Conclusions
Our study confirms the benefit of supplementation with VD and Ca in underprivileged Bangladeshi premenopausal women with hypovitaminosis D and low bone status. Supplementation with VD and Ca or multiple nutrients significantly improves the VD status in these individuals and also increases the femoral neck BMD status. As the prevalence of multiple subclinical micronutrient deficiencies is very high in low-income Bangladeshi women, supplementation with multiple nutrients including VD and Ca is probably the better option. Achievement of optimal VD status and increased bone status in these subjects is anticipated to have future positive health implications alleviating strain on the health care system by reducing morbidity associated with osteoporosis and other VD deficiency-related health problems.
Acknowledgements
The present study was supported by research grants of the Development Fund of the Academy of Finland. We thank Beximco Pharmaceuticals Limited, Dhaka, Bangladesh, for providing MMN and Gonoshasthaya Pharmaceuticals Limited, Dhaka, Bangladesh, for Ca preparations. The authors are grateful to officials of the directory board of the Standard Garments Factory for their tireless help throughout the study. The 153 volunteer subjects who completed the study are thanked for making this research possible. M. Z. I. and C. L.-A. designed the study, secured funding and participated in carrying out the study. M. Z. I. was the principal investigator of the study, providing guidance in data collection and participating in data entry, statistical analysis and writing the manuscript. A. A. S. contributed to field data collection and writing of the manuscript. C. L.-A. checked the manuscript and approved the final version. H. T. V. participated in statistical analysis and interpretation. M. A., A. H. J., H. U. K. and F. A. A.-A. contributed to field data collection. None of the contributing authors had any financial or personal conflicts of interest.






