Age-related chronic diseases and functional decline in the elderly present an important public health and societal burden(1, Reference Harper2). Both scientists and health policy makers have been highlighting the importance to not only focus on the occurrence of specific age-related diseases but to take a more holistic point of view that also considers physical, cognitive, social and mental functioning(Reference Beard and Bloom3). In that context, multidimensional concepts of ‘healthy ageing (HA)’ or ‘successful ageing’ are increasingly discussed and studied. A large part of such HA concepts are based on the definition proposed by Rowe & Kahn(Reference Rowe and Kahn4), including three components: the absence of disease and disability, good physical/cognitive functioning and an active engagement with life.
Among the different modifiable factors that can be targeted to help maintain good overall functioning and the avoidance of disease and disability throughout ageing, diet and physical activity are prominent(Reference Kiefte-de Jong, Mathers and Franco5–Reference Daskalopoulou, Stubbs and Kralj7). Only few studies have investigated the relationship between adherence to national nutrition guidelines and multidimensional concepts of HA(Reference Gopinath, Russell and Kifley8, Reference Assmann, Andreeva and Camilleri9) – despite the need to better understand the effectiveness of such guidelines, widely disseminated in the general population, for preventing overall health decline in the elderly. Hence, the objective of our study was to investigate the association of adherence to the French national nutrition guidelines of the Programme National Nutrition Santé (PNNS), measured by the PNNS-Guidelines Score (PNNS-GS), with a multidimensional concept of HA. A secondary objective was to examine body weight status at baseline as a potentially mediating factor. As both dietary quality(Reference Assmann, Andreeva and Camilleri9–Reference Samieri, Sun and Townsend11) and body weight status(Reference Ruhunuhewa, Adjibade and Andreeva12–Reference Tyrovolas, Haro and Mariolis14) have been associated with multidimensional HA, we hypothesised that adherence to dietary guidelines could affect overall health during ageing both by direct mechanisms and by protecting from overweight and obesity. We thus applied counterfactual-based mediation analysis to disentangle such direct and indirect relationships.
Methods
Study design
The French NutriNet-Santé study is an ongoing web-based cohort study for which inclusions started in May 2009. Detailed information on the study has been published previously(Reference Hercberg, Castetbon and Czernichow15). Study participants were recruited among the French general population, while specifically focusing on Internet-using individuals aged ≥18 years. Information is collected via online questionnaires available on a dedicated web platform, at baseline and every year thereafter. The enquired information includes data on sociodemographic indicators, lifestyle characteristics including dietary intakes and physical activity and health data. All participants included into the NutriNet-Santé study provided informed consent. Moreover, the NutriNet-Santé study was approved by the international review board of the French Institute for Health and Medical Research (0000388FWA00005831) and the Comité National Informatique et Liberté (908450 and 909216). The study is registered at clinicaltrials.gov under the number NCT03335644.
Definition of ‘healthy ageing’
Information on data related to HA was collected via a dedicated self-administered questionnaire that was proposed between 1 October 2015 and 31 March 2016.
Our definition of HA was largely based on the model proposed by Rowe & Kahn(Reference Rowe and Kahn4). Thus, HA was defined as follows: (A) the absence of different chronic diseases (among others: cancer, cardiovascular disease, diabetes, renal disease and liver disease), limitations in instrumental activities of daily living, function-limiting pain, depressive symptomatology and health-related limitations in social life and (B) the presence of good physical and cognitive functioning and good overall self-perceived health. A comprehensive description of these different components is presented in Table 1. HA was defined as a dichotomous variable (meeting all listed criteria or not).
Table 1. Description of the definition of multidimensional healthy ageing used for the NutriNet-Santé study
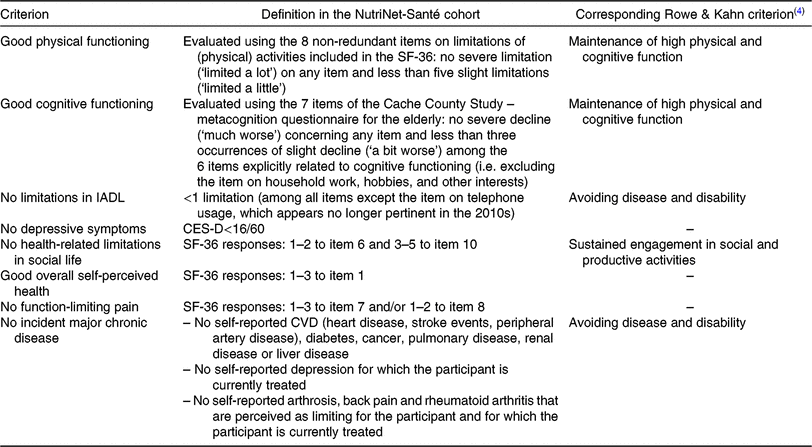
SF-36, Medical Outcome Study Short Form-36; IADL, Instrumental Activities of Daily Living; CES-D, Center for Epidemiologic Studies Depression Scale.
Baseline diet and physical activity data (2009–2014)
Dietary data were collected using repeated 24-h dietary records. Participants could complete one dietary assessment consisting of three dietary records every 6 months. These three records were randomly distributed across a 2-week period, while ensuring that two weekdays and one weekend day were covered. Completing a 24-h dietary record consisted in reporting all foods and beverages consumed at each eating occasion. Portion size estimation was facilitated by photographs derived from a validated picture booklet(Reference Moullec, Deheeger and Preziosi16) including >250 generic foods corresponding to >2000 specific food items, presented in three main portion sizes. It was also possible to directly indicate consumed quantities or volumes.
For the present analysis, all dietary records provided during the first 2 years following inclusion were considered. On average, participants had provided 8·2 (sd 2·5) records (minimum 3; maximum 15 records). Alcohol consumption was estimated via a specific frequency questionnaire, and fish and seafood consumption was estimated based on a specific frequency question. Average daily food consumptions were estimated from the available dietary records, weighted for the type of day. Nutrient intakes were computed using the ad hoc NutriNet-Santé food composition table, which includes >3000 food items. Previous publications based on NutriNet-Santé data have validated the use of web-based 24-h dietary records in comparison with interviews by trained dietitians(Reference Touvier, Kesse-Guyot and Méjean17) and against urine and plasma biomarkers(Reference Lassale, Castetbon and Laporte18, Reference Lassale, Castetbon and Laporte19).
Energy underreporting was detected based on the method developed by Black(Reference Black20) and those identified as under-reporters were not included into the present analyses.
A short form of the French version of the International Physical Activity Questionnaire was used to assess leisure-time physical activity. Metabolic equivalent of task minutes per week was estimated and transformed into three different physical activity levels, according to the guidelines of the PNNS: low (<30 min/d), moderate (30–59 min/d) and high (≥60 min/d).
The computation of the PNNS-GS has been previously published in detail(Reference Estaquio, Castetbon and Kesse-Guyot21). The score includes twelve diet-related components and one physical activity-related component that represent the guidelines of the French National Nutrition and Health Programme launched in 2001(Reference Chauliac22). Scoring and cut-off values for each component are presented in Table 2. To obtain the final score, the points for each component are summed, and a penalty for energy overconsumption is applied if reported energy intakes exceed estimated energy needs by >5 %. In this case, the PNNS-GS is reduced by a fraction that is identical to the proportion by which energy needs are exceeded. The final score can theoretically be negative, and the possible maximum is fifteen points. We also calculated a modified PNNS-score (the mPNNS-GS), which only included the twelve diet-related components and no physical activity component.
Table 2. Adherence to nutritional recommendations according to healthy ageing (HA) status (NutriNet-Santé Study, France, n 21 407)* (Numbers of participants and percentages)
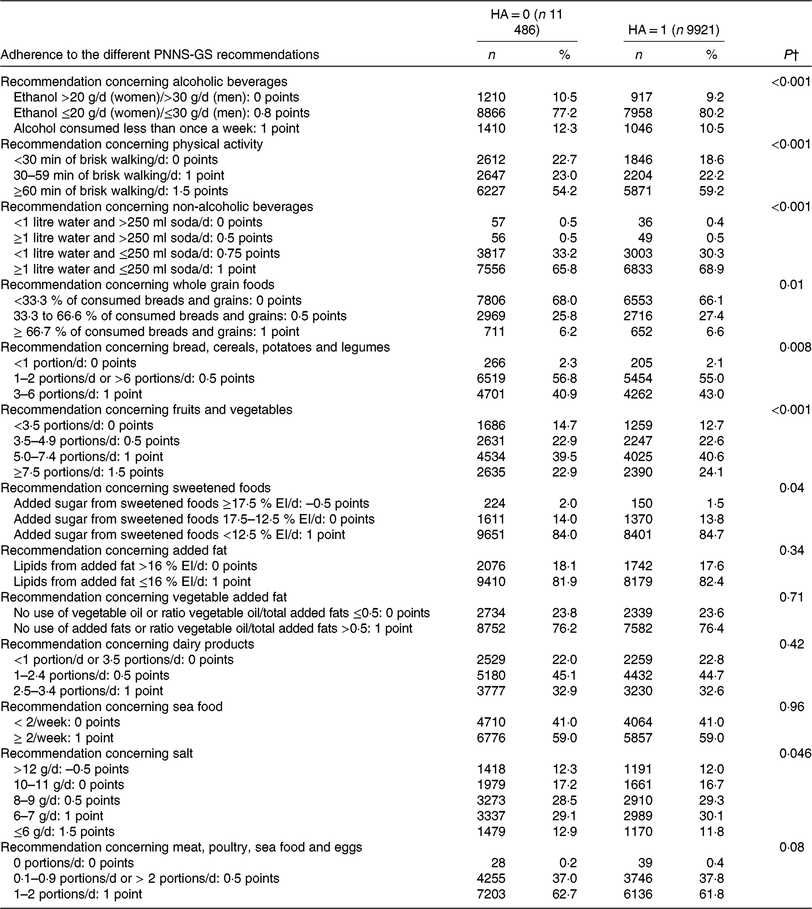
PNNS-GS, Programme National Nutrition-Santé (French National Nutrition and Health Programme) Guidance Score; EI, overall energy intake; PNNS, Programme National Nutrition-Santé.
* This table shows the attribution of points underlying the construction of the PNNS-GS, as well as percentages of adherence to the different recommendations of the PNNS.
† Unadjusted χ2 tests.
Baseline anthropometric data
A validated web-based anthropometric questionnaire was used to collect self-reported information on height and weight at baseline(Reference Touvier, Méjean and Kesse-Guyot23, Reference Lassale, Péneau and Touvier24). BMI was calculated and categories were created as follows: underweight and normal weight (BMI < 25 kg/m2), overweight (25 ≤ BMI < 30 kg/m2) and obesity (BMI ≥ 30 kg/m2).
Other baseline data
NutriNet-Santé participants are asked to complete web-based questionnaires on sociodemographic and lifestyle data at baseline and annually thereafter. These questionnaires provide information on sex, age, educational level, monthly income, socio-professional category, retirement status, living arrangement and smoking status. Socio-professional category either concerned the current occupation or the most recent occupation for unemployed or retired individuals. For income level, a ‘category of missing values’ was also created.
Study sample selection
We included participants who replied to the questionnaire on HA status (n 28 593), aged ≥45 years when completing this questionnaire (n 28 489), without cancer, cardiovascular disease or diabetes at study inclusion (n 24 915), with ≥3 valid dietary records during the first 2 years following inclusion (n 22 402), with available data to compute the PNNS-GS (n 21 772) and no missing data on covariables (n 21 407).
It should be noted that the questionnaire on HA was facultative (i.e. not one of the core questionnaires that NutriNet-Santé participants are regularly asked to complete). Hence, NutriNet participants who were eligible to complete this questionnaire (i.e. those aged ≥45 years) but did not respond may have done so for a variety of reasons: loss to follow-up (due to reasons unrelated to health such as decreased interest or due to health problems), no interest in completing this particular questionnaire or death.
Statistics
Sample size calculation
Our study can be considered as an exploratory analysis of a large-scale observational study. Hence, no calculations related to sample size or statistical power were done.
Descriptive statistics
Participant characteristics were compared according to HA status, using Mann–Whitney U- and χ2 tests. Moreover, proportions of adherence to individual nutritional recommendations were compared according to HA status via χ2 tests.
Main analyses
As the interpretation of OR as proxies for relative risks (RR) is only valid for rare outcomes (<10 %), we used an alternative multivariable model referred to as ‘robust-error variance Poisson regression’ to directly estimate RR(Reference Zou25) (i.e. instead of applying logistic regression).
The main exposure variables were the PNNS-GS and the mPNNS-GS, modelled as quartiles and as continuous variables, and the outcome of interest was HA status (yes/no).
A first model (model 1) was adjusted for age at follow-up and sex, and a second model (model 2) was additionally adjusted for overall energy intake, follow-up time, number of dietary records, educational level, socioprofessional category, income level, living alone (yes/no) and retirement status (yes/no). A third model (model 3, our main model) was also adjusted for smoking status. When modelling the mPNNS-GS as an exposure variable, this third model was also additionally adjusted for physical activity level. Family history of cardiovascular disease (yes/no) was also considered as a potentially confounding factor but not retained as a covariate within our final models as additional adjustment for this factor did not change our main results. Tests for linear trend consisted in modelling score quartiles as ordinal variables.
Tests for interaction
We tested effect modification by age and sex by inserting interaction terms into the fully adjusted models. There was no significant interaction between age and the PNNS-GS score or between sex and the PNNS-GS score (both P > 0·10).
Sensitivity analyses
A first sensitivity analysis consisted in excluding participants with a follow-up <5 years, to reinforce the prospective nature of the present analyses and hence reduce potential reverse causation bias. A second sensitivity analyses aimed to verify whether the investigated association was mainly driven by one or several specific components of the PNNS-GS. We thus created several modified versions of this diet quality score, in addition to the mPNNS-GS from which the physical activity component was removed: twelve additional modified PNNS-GS scores were created by removing each component one by one. The respective models were additionally adjusted for the removed component.
Mediation analyses
A supplementary analysis was conducted to characterise the mediating role of BMI status (normal weight/overweight/obese) in the association between the PNNS-GS and HA. The methodology of this mediation analysis was based on the counterfactual-based approach proposed by Lange et al. (Reference Lange, Vansteelandt and Bekaert26) This methodological approach included the following steps: (1) PNNS-GS quartiles were considered as the exposure (A), BMI class as the mediator (M) and HA as the outcome (Y). (2) A new data set was created that included a new variable A*, corresponding to each of the four PNNS-GS quartiles. For each participant, this new data set included four lines: one line in which A* corresponds to the reality, and three lines in which the participant was part of another PNNS-GS quartile than in reality. (3) Two logistic regression models (adjusted for potential confounders) were run on the above-described new data set, to model the relationship between BMI class and PNNS-GS quartiles: in the first logistic regression model, the original variable ‘A’ was used for this purpose, and in the second model, the new variable ‘A*’ was used. (4) Based on these two logistic regression models, predicted probabilities were extracted and transformed to ‘weights’ as follows: ![]() $W_i^C = P(M = {M_i}|A = A_i^*,C = {C_i})/P(M = {M_i}|A = {A_i},C = {C_i})$ with i: the individual; A: the observed exposure; A*: the created exposure; M: the mediator; C: potential confounding factors (i.e. the same covariables as those used in our main analysis). (5) We ran a weighted and confounder-adjusted robust-error Poisson regression model to obtain relative risk estimates for the relationship of both A and A* with HA. The relative risk associated with A was interpreted as the direct association between PNNS-GS quartiles and HA, and the RR associated with A* was interpreted as the indirect relation mediated by BMI class.
$W_i^C = P(M = {M_i}|A = A_i^*,C = {C_i})/P(M = {M_i}|A = {A_i},C = {C_i})$ with i: the individual; A: the observed exposure; A*: the created exposure; M: the mediator; C: potential confounding factors (i.e. the same covariables as those used in our main analysis). (5) We ran a weighted and confounder-adjusted robust-error Poisson regression model to obtain relative risk estimates for the relationship of both A and A* with HA. The relative risk associated with A was interpreted as the direct association between PNNS-GS quartiles and HA, and the RR associated with A* was interpreted as the indirect relation mediated by BMI class.
All analyses were performed using 9.4 version of the SAS software (SAS Institute Inc.). All P-values were two sided, and P-values <0·05 were considered as statistically significant.
Results
Our study sample’s mean age at follow-up was 60·6 (sd 8·5) years and the mean follow-up time was 5·2 (sd 1·4, median = 5·7, first quartile = 4·4, third quartile = 6·4) years. The criteria of HA were met by 47·5 % of men and 45·9 % of women.
Descriptive statistics
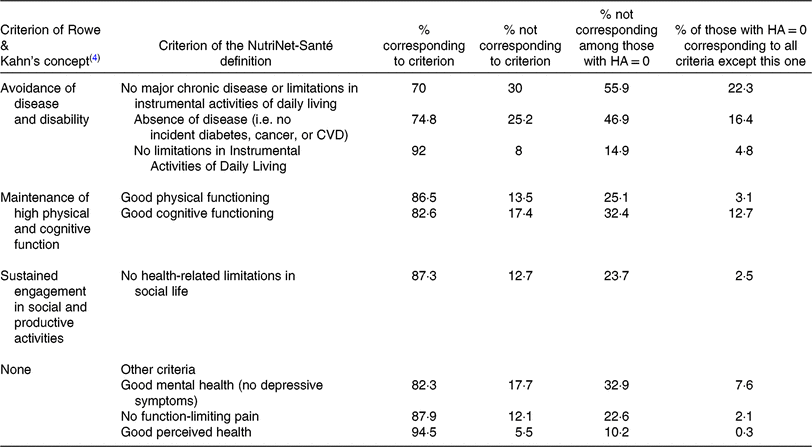
Table 2 presents adherence to the individual recommendations of the French Nutrition and Health Programme (PNNS) at baseline, according to HA status. Those characterised as ‘healthy agers’ at follow-up showed more favourable baseline behaviours concerning physical activity and the consumption of several food groups. Table 3 presents general baseline characteristics of participants according to HA status. ‘Healthy agers’ were slightly younger, more often men, had a higher educational level and income level. They were more often in more ‘advantaged’ socioprofessional categories, were less often retired, less often living alone and less often smokers. Table 4 presents the distribution of individuals that met/did not meet the different criteria of our HA definition. The factors that were the most related to not meeting our definition were the presence of chronic diseases and of depressive symptoms, as well as self-reported decline in cognitive function.
Table 3. Participant characteristics at baseline according to healthy ageing (HA) status (NutriNet-Santé Study, France, n 21 407)
(Numbers of participants and percentages; medians and 25th and 75th percentiles)
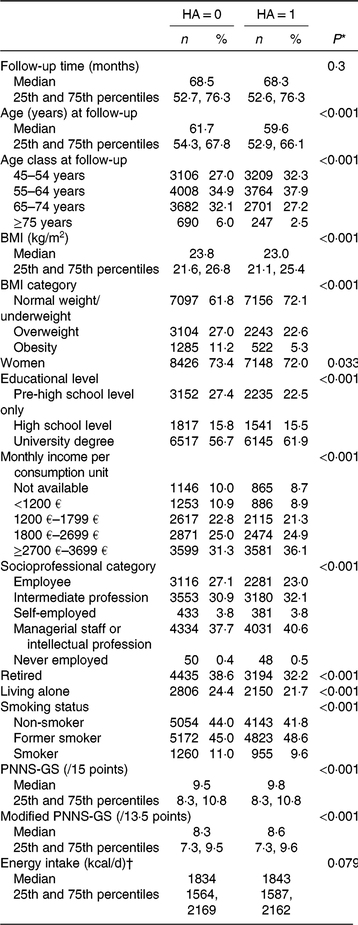
PNNS-GS, Programme National Nutrition-Santé (French National Nutrition and Health Programme) Guidance Score.
* Mann–Whitney U tests for continuous variables and χ2 tests for categorical variables.
† To convert energy in kcal/d to kJ/d, multiply by 4·184.
Table 4. Proportion of participants corresponding to specific criteria of the NutriNet-Santé definition of multidimensional healthy ageing (HA) (NutriNet-Santé Study, France, n 21 407)
Main analyses
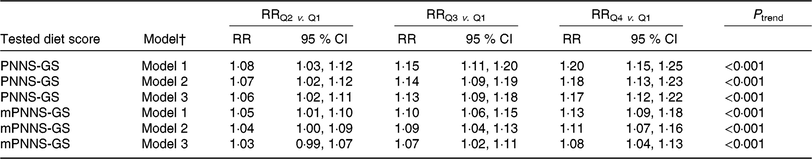
Table 5 presents the association of PNNS-GS and mPNNS-GS quartiles with HA. In the fully adjusted model, both PNNS-GS and mPNNS-GS quartiles were positively related to multidimensional HA status. The RR associated with being in the fourth v. in the first quartile of the PNNS-GS was 1·17 (95 % CI 1·12, 1·22). The RR associated with being in the fourth v. in the first mPNNS-GS quartile was lower (1·08 (95 % CI 1·14, 1·13)). Results concerning the PNNS-GS and mPNNS-GS modelled as standardised continuous scores are shown as part of Table 6.
Table 5. Relationship between quartiles (Q) of the Programme National Nutrition-Santé Guideline Score (PNNS-GS) and modified PNNS-GS (mPNNS-GS; i.e. without the physical activity component) and the probability of overall healthy ageing (NutriNet-Santé Study, France, n 21 407)*
(Relative risks (RR) and 95 % confidence intervals)
P trend, P value for linear trend across quartiles.
* RR were estimated using robust-error Poisson regression. RR higher than 1 indicate an increased probability of multidimensional healthy ageing. Range of PNNS-GS score within each quartile: 0·1–8·3 (Q1), 8·3–9·5 (Q2), 9·6–10·8 (Q3), 10·8–14·5 (Q4). Range of mPNNS-GS score within each quartile: 0·1–7·3 (Q1), 7·3–8·5 (Q2), 8·5–9·5 (Q3), 9·6–13·0 (Q4).
† Model 1: adjusted for age at follow-up and for sex; model 2: additionally adjusted for overall energy intake, follow-up time, number of dietary records, educational level, socioprofessional category, income level, living arrangement (i.e. living alone: yes/no) and retirement status (yes/no); model 3: additionally adjusted for smoking status and physical activity level (except for the PNNS-GS which was not adjusted for physical activity level).
Table 6. Association between modified versions of the Programme National Nutrition-Santé Guideline Score (PNNS-GS) and multidimensional healthy ageing status (NutriNet-Santé Study, France, n 21 407)*
(Relative risks (RR) and 95 % confidence intervals)
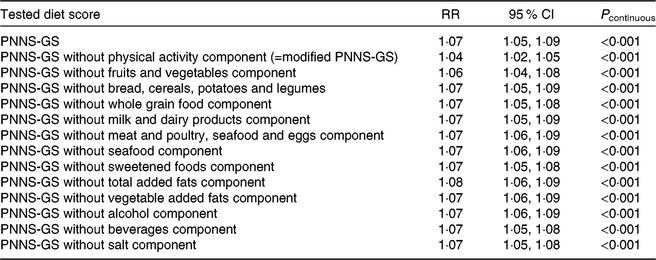
* This table presents the relationship between the PNNS-GS and modified versions of this score, modelled as standardised (i.e. Z-score transformed) continuous variables, with multidimensional healthy ageing. RR were estimated using robust-error Poisson regression. Analyses were adjusted for age, sex, overall energy intake, follow-up time, number of dietary records, educational level, socioprofessional category, income level, living arrangement (i.e. living alone: yes/no) and retirement status (yes/no), and smoking status. Moreover, for each modified version of the PNNS-GS, there was an additional adjustment for the component removed from the initial PNNS-GS score.
Sensitivity analyses
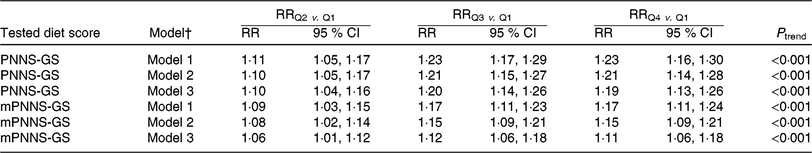
Our sensitivity analyses in which we only included participants with a follow-up time ≥5 years (n 13 668, see Table 7) showed even stronger associations of the PNNS-GS and of the mPNNS-GS with HA than our main analyses. Moreover, our analyses showing the relationship between different types of modified versions of the PNNS-GS and HA (Table 6) indicated that apart from the physical activity component, no other component had a dominant role in the investigated association.
Table 7. Sensitivity analysis: exclusion of participants with a follow-up time <5 years (leaving n 13 668 included in this analysis)*
(Relative risks (RR) and 95 % confidence intervals)
Q, quartile; P trend, P value for linear trend across quartiles; PNNS-GS, Programme National Nutrition-Santé Guideline Score; mPNNS-GS, modified Programme National Nutrition-Santé Guideline Score (i.e. without the physical activity component).
* This table presents the relationship between quartiles of the PNNS-GS and mPNNS-GS and the probability of overall healthy ageing, while excluding participants with a follow-up time <5 years. RR were estimated using robust-error Poisson regression. RR higher than 1 indicate an increased probability of multidimensional healthy ageing.
† Model 1: adjusted for age at follow-up and for sex; model 2: additionally adjusted for overall energy intake, follow-up time, number of dietary records, educational level, socioprofessional category, income level, living arrangement (i.e. living alone: yes/no) and retirement status (yes/no); model 3: additionally adjusted for smoking status and physical activity level (except for the PNNS-GS which was not adjusted for physical activity level).
Mediation analyses
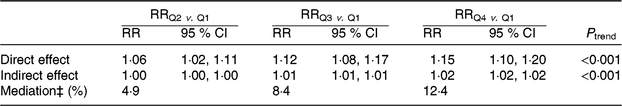
Our supplementary mediation analyses revealed a significant but small ‘natural indirect effect’ related to BMI status, indicating that the relationship between adherence to the French nutrition guidelines and overall HA may, to a small extent, be mediated by BMI status (Table 8). The estimated proportion of the association mediated by BMI status was 12·4 %, for a comparison of the fourth v. the first PNNS-GS quartile.
Table 8. Mediation of the association between the Programme National Nutrition-Santé Guideline Score (PNNS-GS) and healthy ageing status by BMI status (normal weight, overweight, obese)* †
(Relative risks (RR) and 95 % confidence intervals)
Q, quartile; P trend, P value for linear trend across quartiles; NDE, natural direct effect; NIE, natural indirect effect.
* Mediation analysis was conducted using the methodology published by Lange et al. (Reference Lange, Vansteelandt and Bekaert26). The direct effect corresponds to the direct relation between PNNS-GS quartiles and healthy ageing, and the indirect effect corresponds to the relation mediated by BMI status (<25, 25–29, ≥30 kg/m2). Data come from the NutriNet-Santé Study, France (n 21 407).
† RR were estimated using robust-error Poisson regression adjusted for age, sex, overall energy intake, follow-up time, number of dietary records, educational level, socioprofessional category, income level, living arrangement (i.e. living alone: yes/no), retirement status (yes/no), and smoking status.
‡ Values correspond to the percentage of the total association mediated by BMI status. The proportion mediated was computed as (RRNDE(RRNIE − 1)) ÷ (RRNDE × RRNIE – 1) × 100 %.
Discussion
Summary of findings
In this large cohort of French adults, a higher adherence to the French Nutrition and Health Programme food-based dietary guidelines was related to a higher probability of later HA. This relationship was particularly pronounced when considering the combined role of an elevated physical activity level and high dietary quality. Of note, the observed association was even slightly stronger when only including participants with a follow-up of ≥5 years, thus strengthening the prospective nature of our analyses.
Supplementary analyses using modified PNNS-GS scores indicated that the different diet-related components appeared to contribute similarly to the overall relationship. Hence, the combined role of meeting all or several different recommendations seems to be important for maintaining a good overall health status during ageing. The supplemental analyses performed to investigate a potential indirect effect related to BMI status indicated a significant but small mediation of the investigated relationship by corpulence. A very similar observation was made in a previous study based on data from the Supplementation en Vitamines et Mineraux Antioxydants (SU.VI.MAX) study in which 5 % of the prospective association between adherence to the French national nutrition guidelines and multidimensional HA was estimated to be mediated by BMI status(Reference Assmann, Ruhunuhewa and Adjibade27).
Comparison with the literature
To our knowledge, only the French and the Australian national nutrition guidelines have been investigated in relation to multidimensional concepts of HA. An analysis of data from 2329 participants of the French SU.VI.MAX study has shown that a higher adherence to the French nutrition guidelines (as measured by the PNNS-GS) at midlife was related to a higher probability of HA 13 years later(Reference Assmann, Andreeva and Camilleri9). HA was defined in a similar manner as in the present study but combined self-reported information and objective clinical data (while in the present study, all information was self-reported). In that study based on data from the SU.VI.MAX cohort, the strength of the association was higher (OR4 v. quartile 1 of the PNNS-GS = 1·61 compared with an OR of 1·35 in the present study when calculating OR rather than RR, data not shown). It can be hypothesised that this may be related to the longer follow-up time of the study based on SU.VI.MAX data and to the fact that the HA definition used in the SU.VI.MAX study also used objective clinical information.
A study based on data from 1609 participants of the Australian Blue Mountains Eye Study has found a positive association between adherence to the Australian dietary guidelines and a multidimensional concept of ‘successful ageing’, after a follow-up of 10 years. In that study, ‘successful ageing’ was defined as the absence of major chronic diseases, independence in instrumental activities of daily living as well as functional independence, good cognitive, mental and respiratory functioning, as well as blood pressure within a healthy range.
Five other studies have focused on dietary indicators that do not directly reflect adherence to official national nutrition recommendations, but high overall dietary quality(Reference Akbaraly, Sabia and Hagger-Johnson10, Reference Samieri, Sun and Townsend11), high adherence to the Mediterranean diet(Reference Samieri, Sun and Townsend11, Reference Assmann, Adjibade and Andreeva28) or a posteriori dietary patterns(Reference Akbaraly, Sabia and Hagger-Johnson10, Reference Hodge, O’Dea and English29, Reference Assmann, Lassale and Andreeva30).
A prospective investigation of data from the Nurses’ Health Study found a positive relationship between higher scores on the Alternative Healthy Eating Index-2010 and a multidimensional concept of HA. On the other hand, the initial version of the Alternative Healthy Eating Index was not significantly associated with ‘ideal ageing’ in a study based on longitudinal data from the Whitehall II cohort. The aforementioned investigation of data from the SU.VI.MAX study has also focused on the Dietary Quality Index-International and the PANDiet index(Reference Assmann, Andreeva and Camilleri9). Although the Dietary Quality Index-International (a food- and nutrient-based index measuring overall dietary quality) was not related to HA, the PANDiet (measuring adequacy to nutrient-based dietary recommendations) showed a significant positive relationship with HA.
The association between adherence to the Mediterranean diet and HA was investigated within the French SU.VI.MAX study(Reference Assmann, Adjibade and Andreeva28) and within the Nurses’ Health Study(Reference Samieri, Sun and Townsend11). In the SU.VI.MAX study, adherence to the Mediterranean diet at midlife – as measured by the Literature-based Adherence Score to the Mediterranean Diet and the relative Mediterranean Diet Score – showed a significant positive relationship with later HA. Likewise, in the Nurses’ Health study, higher scores on the Alternate Mediterranean Diet Score were prospectively related to a higher probability of HA.
Measures of the overall diet that involve empirically derived dietary patterns are quite different from measures based on a priori constructed dietary scores. Yet, results from three studies that have used principal component analysis to extract such a posteriori dietary patterns(Reference Akbaraly, Sabia and Hagger-Johnson10, Reference Hodge, O’Dea and English29, Reference Assmann, Lassale and Andreeva30) are also in line with the results of the present study. In summary, these three studies emphasise a beneficial role of dietary patterns high in fruits, vegetables, vegetable fat, whole grains and fish and a detrimental role of dietary patterns high in meat and fatty foods.
As expected, our study shows a potentially important role of physical activity for HA, as removal of the physical activity component from the PNNS-GS lead to a substantial decrease in the strength of the association with HA. This is in line with the findings of a recent meta-analysis of prospective observational studies on the relationship between physical activity and (mostly multidimensional) HA concepts(Reference Daskalopoulou, Stubbs and Kralj7).
Limitations and strengths
Our investigation has several limitations. First, no measure of HA status was available at baseline. However, participants were free of major chronic disease, thus strengthening our working hypothesis that individuals were initially healthy. Second, our study sample was not representative of the French general population, as the NutriNet-Santé study included volunteers and has been shown to include more females and individuals with higher education compared with the general population(Reference Kesse-Guyot, Assmann and Andreeva31). Third, the different components of our multidimensional HA construct relied on self-reported data. Fourth, the time of follow-up (median = 5·7) was relatively short. Moreover, given the facultative nature of the NutriNet-Santé HA questionnaire, it was difficult to disentangle non-responses to the questionnaire due to health-unrelated reasons (such as lack of interest in this particular questionnaire or in continued study participation in general) from health-related reasons (i.e. functional limitations preventing participants from continued study participation and death). Non-responses related to health decline and death may have led to an underestimation of the investigated relationship (under the hypothesis that poor diet was implicated in health decline among such participants). The fact that deceased participants were not included into our study is also of importance in the light of the observed ‘gender paradox’, which implies that men tend to die earlier than women despite less co-morbidities and disabilities(Reference Gordon, Peel and Samanta32). The lower proportion of HA among women compared with men that was observed in our study is likely a reflection of this paradox because our study’s HA definition did not include the notion of ‘avoiding premature death’.
A major strength of our study is the availability of a very large data set of >20 000 individuals. Moreover, dietary data were estimated in a particularly precise manner, using a validated methodology of repeated 24-h dietary records – with, on average, eight available records per participant. In addition, mediation analysis emphasised the direct association of high dietary quality and physical activity with HA.
Conclusion
These results indicate that higher adherence to the French nutrition recommendations may be linked to a higher probability of maintaining good overall health during ageing – including disease-related dimensions, functional dimensions, as well as perceived health. Further research is needed to define public health strategies that efficiently help individuals to make changes in their day-to-day lives, towards an improved dietary quality and increased engagement in physical activities.
Acknowledgements
The authors thank all the volunteers of the NutriNet-Santé cohort. They also thank Younes Esseddik, Thi Duong Van, Frédéric Coffinieres, Régis Gatibelza and Paul Flanzy (computer scientists), as well as Nathalie Arnault, Véronique Gourlet, Dr Fabien Szabo, Julien Allegre and Laurent Bourhis (datamanagers/biostatisticians) for their technical contribution to the NutriNet-Santé study.
K. E. A. and M. A. were supported by doctoral fellowships from the University of Paris 13. The NutriNet-Santé study was supported by the following public institutions: Ministère de la Santé, Institut de Veille Sanitaire (InVS), Institut National de la Prévention et de l’Education pour la Santé (INPES), Région Ile-de-France (CORDDIM), Institut National de la Santé et de la Recherche Médicale (INSERM), Institut National de la Recherche Agronomique (INRA), Conservatoire National des Arts et Métiers (CNAM) and Université Paris 13. The funding bodies did not have any involvement in the design/conduct of the research, in data analysis/interpretation, or in writing/approval of the manuscript.
S. H., P. G. and E. K.-G. designed the study (development of the concept, design and protocol of the SU.VI.MAX/SU.VI.MAX 2 studies and coordination of data collection); K.E.A. and E. K.-G. conducted the research, performed the statistical analysis and wrote the article; K. E. A., M. A., S. A., R. V., V. A. A., C. J., S. H., P. G. and E. K.-G. were involved in interpreting the results and editing the manuscript for important intellectual content; E. K.-G. had primary responsibility for the final content. All authors have read and approved the final manuscript.
None of the authors declares any conflicts of interest.











