Background
Previous studies have focused extensively on children who are exposed to parental alcohol use disorder (AUD). It has been estimated that as many as 22–30% of the children in the general population are exposed to parental AUD,Reference Grant1–Reference Manning, Best, Faulkner and Titherington3 and evidence indicates their high risk of exposure to adverse experiences, including chronic family stress,Reference Grekin, Brennan and Hammen4, Reference Hussong, Bauer, Huang, Chassin, Sher and Zucker5 disharmony and conflicts in the family,Reference El-Sheikh and Flanagan6, Reference Rounsaville, O'Farrell, Andreas, Murphy and Murphy7 inter-parental violenceReference Christoffersen and Soothill8, Reference Woodin, Caldeira, Sotskova, Galaugher and Lu9 and emotional, physical and sexual child abuse,Reference Dube, Anda, Felitti, Croft, Edwards and Giles10–Reference Walsh, MacMillan and Jamieson12 which can lead to family separation and foster care.Reference Walsh, MacMillan and Jamieson12 Along with genetic susceptibility, adverse childhood experiences may manifest as psychiatric disorders later in life, and it is particularly well established that these children are at a greater risk of developing AUD and other substance use disorders (SUDs).Reference Yoon, Westermeyer, Kuskowski and Nesheim2, Reference Christoffersen and Soothill8, Reference Hill, Tessner and McDermott13–Reference Sørensen, Manzardo, Knop, Penick, Madarasz and Nickel16
It is imperative to intervene against negative intergenerational heritage, and once a parent has developed an AUD, the best way to intervene is by treating the parent(s) for their AUD.
Improving child welfare is best attained by enhancing the function within the family, by offering the parents supportive initiatives and relevant treatment, as placement in foster care risks another adverse experience.Reference Jones, Everson-Hock, Papaioannou, Guillaume, Goyder and Chilcott17–Reference Fowler, Toro and Miles22 However, there is little knowledge pertaining to the association between childcare responsibility and outcomes of treating parents for AUD. It has been found that parents with AUD are motivated to be treated, to relieve their children of the negative effects of the AUD and avoid intervention from social authorities (i.e. monitoring or forced removal of the children to foster care).Reference Christoffersen and Soothill8, Reference Meier, Donmall and McElduff23, Reference Swift, Copeland and Hall24 Further, a small-scale study conducted in 1991 (n = 130) found that treatment-seeking patients with AUD, with a relatively low degree of addiction impairment and who were living with their children, were less likely to drop out, more likely to comply and achieved better drinking-related outcomes compared with patients without similar childcare responsibility.Reference Koski-Jannes25 Other studies found that parents with other types of SUD, who had children living with them, achieved similar or even better drug-related outcomes compared with parents without childcare responsibility.Reference Stewart, Gossop and Trakada26–Reference Comiskey, Hyland and Hyland28 However, other adverse psychosocial circumstances could have affected the overall severity of the addiction of parents with other SUDs of mainly illegal drugs, such as heroin, cocaine and poly-substances. Neither the early study on AUD nor the majority of later SUD studies investigated the effect of gender on treatment outcomes, but it is plausible that living with children may affect women more than men, as they often have the primary childcare responsibility.Reference Stewart, Gossop and Trakada26, Reference Comiskey27
A contemporary and large-scale study pertaining to the specific prognosis of treating AUDs, as well as its associations with parental gender, is warranted to guide clinical practice, effectuate interventions and inform social authorities within this field.
Aim
This study aimed to investigate whether childcare responsibility (living with children aged <18 years) is related to the addiction severity profile at treatment entry, the treatment course and drinking-related outcomes, when treated in conventional evidence-based pharmacological and psychosocial out-patient AUD treatment. Based on the findings from the early AUD study together with the SUD studies mentioned above, we hypothesized that in parents with AUD, living with children is associated with a better treatment prognosis relative to patients without children and parents without childcare responsibilities.
Method
This observational study is reported in accordance with the Reporting of Studies Conducted using Observational Routinely-Collected Health Data (RECORD) guidelines,29 an extension of the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines.30 These guidelines were applied to ensure an adequate reporting of the study.
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008. Formal ethical approval was not required for this study, in accordance with Danish legislation; however, the use of data from the database for research purposes was approved by the Danish Data Protection Agency (region of Southern Denmark, registration number: 2012-58-0018).
Design and setting
The study was conducted as an observational cohort study in an out-patient alcohol treatment clinic located in Odense, Denmark. AUD is usually treated at out-patient municipal treatment facilities and only alcohol-related problems are addressed there. Public out-patient treatment is free of charge to patients, open for self-referral and anonymity is available. If patients suffer from either illegal SUDs, have severe psychiatric comorbidity (e.g. acute psychotic disorders), severe cognitive impairment (e.g. dementia) or terminal somatic illness, treatment takes place elsewhere.
Treatment
The clinic cooperates closely with the Odense University Hospital and the Unit of Clinical Alcohol Research, University of Southern Denmark. The pharmacological and psychosocial treatment offered at the clinic is evidence-based and provided in accordance with the national clinical recommendations.Reference McLellan, Kushner, Metzger, Peters, Smith and Grissom31, Reference Blacken, Hendriks, Pozzi, Tempesta, Hartgers and Koeter32 Upon entering treatment, patients were provided a medical consultation by a psychiatrist, and other pharmacological treatment targeting the AUD and detoxification was provided as was deemed necessary. Detoxification was conducted with benzodiazepines and disulfiram, acamprosate and/or naltrexone were also prescribed when appropriate. After detoxification, psychiatrists referred the patients to psychosocial treatment, which constituted the main component of the offered treatment and was carried out by the team of therapists in the clinic, comprising nurses and social workers trained within the treatment range. Treatment began with a motivating interview, to engage the patients in their treatment, followed by cognitive–behavioural therapy or supportive consultations focused on the AUD. All treatments were carried out during 1 h individual or group sessions. At the beginning of the treatment, sessions were offered once a week, decreasing to twice a month after 4 weeks. A treatment course was scheduled to last 3 months and comprised eight psychosocial sessions, after which an evaluation of the treatment course was conducted. The duration of treatment was decided together with the patient on an individual basis, and could be extended as long as needed. Frequent supervision of the staff was undertaken, and psychiatrists monitored the treatment course regularly.
Participants
The population consisted of a consecutive sample of patients with harmful use or dependence of alcohol (AUD), entering the out-patient alcohol treatment clinic from October 2006 to October 2016. To be eligible for the study, patients had to have an AUD diagnosis; be aged between 18 and 65 years to assure that they may have children <18 years of age; provide information about biological or adopted children, and the age of the youngest child; have at least one child <18 years of age if having children, to assure that not all the children were adults and finally, have finalised or dropped out of the treatment course (i.e. not currently in treatment). A total of 3569 patients entered treatment and were discharged during this period, of which 1368 were excluded from the study for following reasons: 82 patients did not fulfil the criteria for an AUD, 121 patients were not aged between 18 and 65 years, eight patients did not provide information concerning children in the household, 1049 patients only had grown-up children aged ≥18 years and finally, 186 patients were still/currently in treatment when data were collected/when the study period concluded. Hence, 2201 patients were eligible and included in the study.
Assessment
Data was obtained from the clinical database in the treatment clinic, developed with the purpose of monitoring the overall quality of treatment and conducting research to improve the treatment. All patients entering treatment are required to complete a baseline assessment interview, after medical consultation and before referral to psychosocial treatment, and a follow-up assessment every 3 months and upon treatment conclusion. The clinical data are stored in the database, and data derived for further analysis are encrypted and no person sensitive information is extracted.
The baseline assessment was performed using the ICD-10 Diagnostic Criteria for Research for harmful use of alcohol (F10.1) and alcohol dependence syndrome (F10.2),29, 30 and the European Addiction Severity Index (EuropASI) was applied both at baseline and follow-up.Reference McLellan, Kushner, Metzger, Peters, Smith and Grissom31–Reference Kokkevi and Hartgers33 The EuropASI assesses sociodemographic, clinical AUD-related variables (e.g. years with AUD, prior treatment etc.) and degree of addiction severity related to nine areas of the patients life, including alcohol use and other drug use, medical and psychiatric status, family status and other social status, economy and job satisfaction, and legal status. Further, for each area, a composite score ranging from 0 to 1 was calculated, with higher scores reflecting higher severity of problems. These composite scores are exclusively derived from items relating to the past 30 days.Reference Blacken, Hendriks, Pozzi, Tempesta, Hartgers and Koeter32, Reference McGahan, Griffith, Parente and McLellann34
All assessments were performed in face-to-face interviews by the team of therapists in the clinic, who were trained in the assessment procedures.
Measures
The baseline sample characteristics were derived from ICD-10 and baseline EuropASI assessment, and variables related to treatment course and outcomes were based on baseline and latest follow-up EuropASI assessment, i.e. the treatment conclusion.
The sample was divided into three patient groups: group A, comprising patients with no children; group B, comprising patients with at least one child <18 years of age (biological or adopted) living at home; and group C, comprising patients with at least one child <18 years of age (biological or adopted), living out-of-home.
To describe sample characteristics, the following sociodemographic, clinical AUD-related variables and degree of addiction severity were calculated: age, gender, cohabitation (married or living with a partner), cohabiting with a partner with AUD, vocational education (education leading to a profession, e.g. vocational training, a bachelor's degree at vocational academies or university colleges (≤4 years of education), or a university degree or other higher education (>4 years of education) after finishing elementary or high school), employment (full- or part-time employment for the past 3 years), AUD diagnoses (harmful use or dependence), delirium tremens (one or more episodes during lifetime), years with AUD, prior AUD treatment (in-patient or out-patient treatment), referral form (self-referred or referred by the social services), drinking measures (i.e. abstinence, drinking days and days with excessive drinking the past 30 days) and the nine EuropASI composite scores (also based on items relating to the past 30 days).
The treatment course variables, consisting of whether patients concluded treatment successfully or dropped out, were based on the latest follow-up assessment, and outcome measures were derived from the EuropASI's alcohol use component, comprising abstinence, drinking days and excessive drinking days. Abstinence was defined as not consuming any alcohol, a drinking day as consuming minimum one unit of alcohol (12 g pure ethanol) and days with excessive drinking as drinking six or more units of alcohol in the 30 days preassessment. Abstinence outcomes were calculated from the treatment conclusion, indicating continued (from baseline) or acquired abstinence during treatment. Drinking days and days with excessive drinking were defined as change scores from baseline to treatment conclusion, indicating whether a decrease or increase occurred in these measures.
Statistical analyses
The range and distribution of sociodemographic, AUD-related and addiction severity variables at baseline and the treatment course were examined by χ 2 tests for categorical data, and Kruskal–Wallis rank-sum tests for continuous data. To examine whether the total sample exhibited an improvement from baseline to follow-up, McNemar's χ 2 tests and Wilcoxon signed-rank tests were conducted on categorical and continuous drinking outcomes, respectively.
An intention-to-treat analysis approach was adopted for all treatment outcomes and was analysed by weighted logistic regression, to examine whether the groups differed in their achievements. Further, the logistic regression models were adjusted for the sociodemographic, AUD-related and addiction severity variables that were found to differ between groups at baseline, and were stratified by gender. Inverse probability weighting (IPW), which addresses the potential bias arising from the exclusion of patients with missing data at follow-up,Reference Seaman and White35 provided weights in the model. The IWP method weights each observation by the inverse of the probability of having completed a follow-up, to create a weighted sub-sample of complete cases that resembled the full sample, with respect to chosen observed predictors. The IPW weights were constructed with a logistic model to predict the probability of having answered the question of alcohol consumption in the 30 days before follow-up. The IPW model contained the following predictor variables: age, gender, education, employment, cohabitation, referral form, previous AUD treatment, years of AUD, delirium tremens and psychiatric and somatic composite scores at baseline. As 6% of the patients (n = 206) had missing data on these baseline variables and thus did not receive a weight, a sensitivity analysis was performed, giving these cases a weight of 1. All analyses were conducted with Stata v15 for Windows.
Results
Sample characteristics
At baseline, 41% of the patients (n = 900) belonged to group A, 34% (n = 746) belonged to group B and 25% (n = 550) belonged to group C (Table 1). Group A had the lowest median age, and group B (39%) comprised more female patients than group A (21%) and group C (18%). Group B was also more likely to be cohabiting, have completed their education and be employed, compared with the other groups. Further, group B patients had less severe AUD, fewer years of AUD, were less likely to have suffered from delirium tremens and were less likely to have been in treatment before, whereas group C demonstrated the opposite, with the most severe AUD patterns among this group. Group B patients were also more prone to seek treatment on their own or the family's initiative, whereas group C was more likely to be referred to treatment by social authorities, followed by group B patients. When the patients are referred by social services, the treatment is not mandated, but the patients may feel forced to complete the treatment as there is awareness of their issues that could ultimately have consequences for child custody if they do not resolve their drinking problem.
Table 1 Baseline characteristics of treatment-seeking patients with alcohol use disorder (AUD) in an operating Danish alcohol treatment clinic (N = 2201)

a Married or partner; b higher/continuing education; c full- or part-time employment past three years; d experienced ≥ 1 episodes; e past 30 days. IQR, interquartile range.
* P < 0.05
At baseline drinking measures, the groups only differed on drinking days: group B posted the lowest and group C posted the highest number of drinking days. Regarding the addiction severity reflected by the composite scores, group B was the least impaired on alcohol use, medical status and economy, but the most impaired on family status. Groups A and C were similarly impaired on alcohol use, medical status and economy, but group C was (second to group B) the most impaired on family status and group A was the most impaired on social status.
In general, all patients functioned relatively well, as is apparent from the low composite scores of the groups; impairment was reflected mainly in the alcohol use composite score.
Treatment course and outcomes
More than half of all patients (55%) successfully concluded the treatment course (45% drop-out rate). Among those that concluded treatment, 60% were abstinent at follow-up, which was a significant improvement from the baseline abstinence rate (McNemar's χ 2 = 406.16, P < 0.001). In total, 89% had a decline in number of drinking days, from a median of 15 (interquartile range [IQR] 25) at baseline to 0 (IQR 3) at follow-up (Wilcoxon signed-rank test z = 24.51, P < 0.001), and 94% had a decline in number of excessive drinking days, decreasing from a median of 14 (IQR 25) to 0 (IQR 0) (Wilcoxon signed-rank test z = 25.68, P < 0.001). Thus, an overall significant improvement was observed in all drinking outcomes, from baseline to follow-up, regardless of group assignment. Group B was the most treatment compliant, with 63% successfully concluding treatment and only 37% prematurely dropping out, whereas in groups A and B, 51 and 50% successfully concluded treatment and 49 and 50% dropped out, respectively.
Treatment outcomes are presented in Table 2 as odds ratios and adjusted odds ratios (AORs), and the models were adjusted for age, gender, cohabitation, education, employment, referral form, AUD diagnosis, delirium tremens, years with AUD and relevant composite scores, as these variables were not equally distributed at baseline. Better outcomes were observed in group B, where the odds ratios and AORs of achieving a positive alcohol-related outcome on all parameters were highly significant in relation to group A. Odds ratios for group C also improved, compared with group A, in continued or acquired abstinence as well as in the decline in number of excessive drinking days from baseline to follow-up, but only the former remained significant in AORs. Treatment outcomes stratified by gender are presented in Table 3 as odds ratios and AORs, where the models are adjusted for the same variables as the former inferential analysis presented in Table 2, except for gender. When the treatment outcomes were stratified by gender, even better outcomes were observed in group B among women, whereas the small significant effect in group C disappeared after gender stratification.
Table 2 Treatment outcomes among treatment seeking patients in an operating Danish alcohol treatment institution, by having and/or living with children, or not
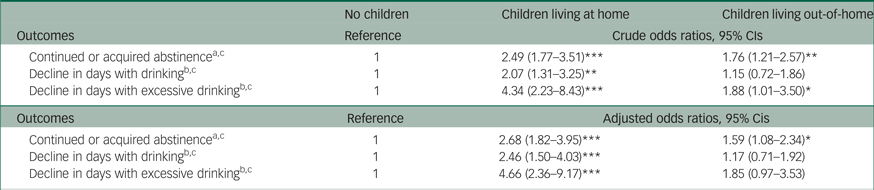
a Variable from the last follow-up interview, indicating continued/acquired abstinence or drinking every day at follow-up; b change score from baseline to the last follow-up, indicating a decline in alcohol consumption; c inverse probability weighting applied.
* P < 0.05, **P < 0.01, ***P < 0.001.
Table 3 Treatment outcomes among treatment seeking female patients in an operating Danish alcohol treatment institution, by having and/or living with children or not, and stratified by gender
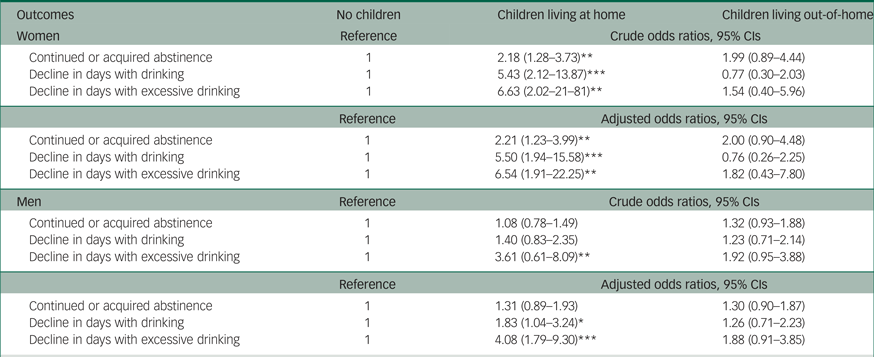
* P < 0.05, **P < 0.01, ***P < 0.001.
Discussion
In patients with AUD who are seeking treatment, those living with children showed a less severe addiction profile at treatment entry, were more compliant and had a lower drop-out rate during the treatment course compared with their counterparts with no children or children living out-of-home. Strong positive associations were found between living with children and all drinking outcomes, and gender stratification revealed that females achieved the most favourable outcomes. In addition, a positive, although less strong, association was found on abstinence outcome among parents not living with children, but gender stratification resulted in non-significant outcomes among both genders. The best outcomes were found among patients living with their children.
Our findings support the previous conclusion of a small-scale study that found having childcare responsibility was positively associated with a parent's prognosis in AUD treatment.Reference Koski-Jannes25 Although the previous study's sample was derived from an in-patient setting compared with this study's out-patient one, it similarly reported a relatively low degree of addiction severity among parents with AUD with children, and a minor degree of psychosocial impairment among those living with their children, indicating that children are a protective factor in the prevention of a severe addiction pattern. The previous study also had a lower drop-out rate and higher compliance during the treatment course, and drinking-related outcomes were more positive at 6- and 12-month follow-up after treatment initiation. Additionally, living with children was found to be the strongest predictor of recovery out of 80 background variables, such as age, gender, education, employment, and non-alcoholic family background. This study's findings reflect similar conclusions in the contemporary context, and add to prior knowledge with the finding that the protective influence of children may be most prominent among female parents with AUD.
Our findings were also consistent with observations of prior studies suggesting that those with SUD that have childcare responsibilities improves treatment outcomes for legal and illegal drugs.Reference Stewart, Gossop and Trakada26–Reference Comiskey, Hyland and Hyland28 Stewart et al's study of 1075 treatment-seeking individuals with SUD in out-patient and in-patient treatments for misuse or dependence of illegal substances in England found that, despite their more severe addiction profiles (most were women with children in their care), their consumption of illicit drugs was reduced at 12-month follow-up after treatment initiation, although not significantly more for patients living with children compared with patients not living with their children, and no difference was found between parental gender.Reference Stewart, Gossop and Trakada26 Comiskey and colleagues examined 404 individuals with SUD (23% had children in their care) in both clinical settings in Ireland, with more severe addiction-related problems.Reference Comiskey27, Reference Cox and Comiskey36 In contrast to the findings of Stewart et al, they found that significantly fewer individuals with children in their care were using drugs at 1-year follow-up,Reference Comiskey27 and the effect persisted after 3 years.Reference Comiskey, Hyland and Hyland28 However, the study did not examine parental gender effects, but these findings are in line with gender-specific studies on mothers with SUD, suggesting that increased retention rates and better outcomes were found among women whose children joined them during residential treatment.Reference Conners, Grant, Crone and Whiteside-Mansell37–Reference Hughes, Coletti, Neri, Urmann, Stahl and Sicilian40
As this study focused only on patients with AUD, it can be assumed that they were relatively less psychosocially impaired compared with the individuals in other studies, who suffered mainly from heroin or other opiate addiction as well as poly-substance addictions. However, patients with AUD as their only or at least primary diagnosis may also have a severe addiction profile.Reference Sanvisens, Zuluaga, Fuster, Rivas, Tor and Marcos41–Reference Cargiulo43 Therefore, the treatment of parents with AUD with a pronounced severe addiction profile may, to a higher degree, benefit from being enrolled in a broader and complex integrative treatment, where several other supportive and treatment initiatives are effectuated, including parenting skills training and provision of support to children and other family members.Reference Niccols, Milligan, Smith, Sword, Thabane and Henderson44–Reference Milligan, Niccols, Sword, Thabane, Henderson and Smith46 Furthermore, we do not know whether the patients included in this study could have achieved even better treatment outcomes if the out-patient treatment was combined with other initiatives.
Women with childcare responsibilities have also been found to be reluctant toward seeking treatment because of fear that social authorities could intervene by taking their children from their care.Reference Wilke, Kamata and Cash47, Reference Finkelstein48 Although this issue was not examined directly in this study, it was observed that more women with children attended treatment compared with their male counterparts, and that patients living with their children seek treatment at a relatively earlier stage of AUD compared with those who do not live with their children. Additionally, we observed a relatively higher proportion of patients referred by social services and living with their children, indicating that social services encourage and support families in solving the drinking problem. As AUD negatively affects children and increases the risk of a series of psychiatric disorders, including SUDs,Reference Yoon, Westermeyer, Kuskowski and Nesheim2, Reference Christoffersen and Soothill8, Reference Hill, Tessner and McDermott13–Reference Sørensen, Manzardo, Knop, Penick, Madarasz and Nickel16 collaboration between social services and treatment for addiction plays an important role in ending the negative intergenerational heritage of alcohol use and dependence within the family.
Strengths and limitations
The primary strength of this study is the use of a large sample of patients with AUD in an operating out-patient alcohol treatment clinic.
A number of limitations can be mentioned. First, although we adjusted the models with non-comparable baseline sample characteristics across the groups, the fact that the group living with children was less impaired may have affected the results. Prior studies have demonstrated that lower addiction severity at baseline is associated with better treatment outcome.Reference Adamson, Sellman and Frampton49 However, lower impairment at treatment entry may also reflect the protective role of children in the home. Second, the data were self-reported. Although they are generally considered reliable and valid, they may be less so when children are involved because of fear of reprisals from the social authorities. Third, the treatment outcome measures were based on the assessment of the past 30-day baseline and follow-up. Hence, vital information that occurred in-between this period could have been overlooked. As the outcome data violated assumptions for regression models with continuous outcomes, the outcomes were coded as binary variables, and much information might have been lost in the translation procedure. Moreover, the follow-up window failed to consider the possibility that certain patients might have developed a negative drinking outcome after follow-up, and could potentially develop negative treatment outcomes in the longer term. Fourth, although this study was conducted in a naturalistic setting, giving an optimal setting for the generalisability of the study, all patients functioned relatively well, as is apparent from the low composite scores in the three study groups, where the impairment was reflected mainly in the alcohol use composite score. Thus, this might compromise the external validity of the study as the sample could be representative of patients with minor addiction severity not branching into several areas of a patient's life. Also, the results cannot be generalised to other populations with more severe AUD profiles (e.g. an in-patient setting). Despite these limitations, this study adds to the evidence that childcare responsibilities need not be an obstacle to achieving favourable treatment outcomes for parents with AUD.
In conclusion, patients with childcare responsibilities have a less severe addiction profile at entry and a more coherent treatment course and better drinking-related outcomes compared with patients without similar responsibility when treated in conventional, evidence-based pharmacological and psychosocial out-patient treatment. This knowledge is crucial to guide clinical practice, effectuate interventions and inform social authorities. As a first line of treatment for patients with AUD living with children, healthcare and social care professionals may consider evidence-based out-patient treatment, hereby improving the family function and the welfare of the children. However, a thorough assessment of the degree of addiction severity and psychosocial impairment is needed, as these findings may not be generalisable to patients with AUD with more pronounced psychosocial impairment. In these cases, more complex integrative treatment, including more support and treatment for the diagnosed parent as well as provision of support for the children and other family members, may be needed. Additional studies should replicate the current findings in both out-patient and in-patient settings, and should investigate how treatment targeting the parents influences children's welfare.






eLetters
No eLetters have been published for this article.