Acquiring a SCI typically results in a level of physical inactivity and deconditioning that starkly contrasts with the preinjury state (Nash, Reference Nash2005), making SCI a disability that may be most in need of effective behavioural health and rehabilitation counselling interventions. Even among young and healthy persons with SCI, many are physically unable to perform essential activities of daily living, which leads to an increased risk for secondary conditions as well as lower participation in the community and workforce (Krause & Saunders, Reference Krause and Saunders2011; Noreau, Shephard, Simard, Pare, & Pomerleau, Reference Noreau, Shephard, Simard, Pare and Pomerleau1993; Scelza, Kalpakjian, Zemper, & Tate, Reference Scelza, Kalpakjian, Zemper and Tate2005; Washburn, Zhu, McAuley, Frogley, & Figoni, Reference Washburn, Zhu, McAuley, Frogley and Figoni2002). When individuals with SCI are capable of engaging in work, education and leisure pursuits, a higher level of life satisfaction is noted (Nosek, Fuhrer, & Potter, 1995). Therefore, physical activity and exercise has been continuously recognised as a fundamental aspect of rehabilitation strategies for individuals with SCI. Empirical studies indicate that participation in physical activity can also provide significant health benefits to injured persons, such as reducing spasticity and pain as well as improving bone mineral density, muscle endurance, subjective well-being, and physical health-related quality of life (Dearwater et al., Reference Dearwater, LaPorte, Robertson, Brenes, Adams and Becker1986; Myers, Lee, & Kiratli, Reference Myers, Lee and Kiratli2007; Wolfe et al., Reference Wolfe, Martin Ginis, Latimer, Foulon, Eng, Hicks, Hsieh, Eng, Teasell, Miller, Wolfe, Townson and Boily2012).
Despite the far-extending benefits of physical activity and exercise for individuals with SCI, participation in exercise activities is frequently hampered by perceived barriers, which can arise as a function of external and internal factors (Scelza et al., Reference Scelza, Kalpakjian, Zemper and Tate2005). External obstacles include public attitudes, policies, procedures, inaccessible facilities or insufficient resources. Whereas, internal obstacles, which are subjectively experienced as impediments, involve limited motivation, health concerns and psychological barriers (Rimmer, Riley, Wang, Rauworth, & Jurkowski, Reference Rimmer, Riley, Wang, Rauworth and Jurkowski2004). This is confirmed by research conducted in the United States, Canada and Europe, which indicates that individuals with SCI experience numerous external and internal barriers to exercise participation (Anneken, Hanssen-Doose, Hirschfeld, Scheuer, & Thietje, Reference Anneken, Hanssen-Doose, Hirschfeld, Scheuer and Thietje2009; Martin, Latimer, Francoeur, & Hanley, Reference Martin, Latimer, Francoeur and Hanley2002; Scelza, Kalpakjian, Zemper, & Tate, Reference Scelza, Kalpakjian, Zemper and Tate2005; Vissers et al., Reference Vissers, Van dB-E, Sluis, Bergen, Stam and Bussmann2008). However, few studies have investigated the relationship between perceived barriers and SCI severity. One study by Vissers et al. (Reference Vissers, Van dB-E, Sluis, Bergen, Stam and Bussmann2008) indicated that individuals with paraplegia and tetraplegia encountered more external over internal barriers to physical activity, such as limited information on community resources. Similarly, Scelza et al. (Reference Scelza, Kalpakjian, Zemper and Tate2005) reported that injury severity was a predictor of participation in exercise behaviours, and that individuals with tetraplegia experienced significantly more perceived barriers than individuals with paraplegia. These findings suggest that increased sensorimotor function and mobility associated with paraplegia (relative to tetraplegia) may facilitate greater independence and a wider range of choices for physical activity, thus reducing perceived barriers.
A recent study completed by Roberton, Bucks, Skinner, Allison, and Dunlop (Reference Roberton, Bucks, Skinner, Allison and Dunlop2011) focused on investigating differential effects of specific disability-related limitations (level of ambulation and ability to transfer) on perceived barriers to physical activity. The authors reported findings that indicate across levels of SCI-related impairment, only a small number of participants maintained physical activity, and that injury severity was not significantly associated with physical activity participation. According to Roberton et al., due to a small sample size, their study may have been statistically underpowered. Further, while the amount of reported perceived barriers was not significantly different across levels of SCI severity, types of perceived barriers did vary according to severity of impairment, with individuals affected by more significant mobility impairments endorsing higher rates of external barriers. Roberton et al. concluded that there might be a need for additional health resources among individuals with the most significant SCI.
Goals of the Study
As a result of the mixed evidence on the link between post-SCI level of functional disability and perceived barriers to physical activity and exercise, the present study aimed to further examine the relationship in order to clarify the findings pertinent for biopsychosocial interventions in behavioural health and rehabilitation counselling settings. Multivariate analysis of variance was used to evaluate perceived barriers to physical activity and exercise in non-random, convenience sample of people with SCI experiencing varying functional disability. In addition, a mediation analysis, using hierarchical regression analysis, investigated the effects of perceived barriers to physical activity and exercise on the relationship between functional disability and physical health-related quality of life. Our two primary research questions were:
• Do perceived barriers to physical activity and exercise differ among persons with SCI experiencing varying levels of functional disability?
• Do perceived health barriers mediate the relationship between functional disability and physical health-related quality of life?
Based on health promotion research for individuals with SCI, it was hypothesised that functional disability would significantly influence the individual experiences of barriers to physical activity and exercise. Furthermore, it was expected that the relationship between functional disability and physical health-related quality of life would be partially mediated by perceived health barriers.
Method
Participants and Setting
The participants were recruited from the National Spinal Cord Injury Association, as well as from various SCI support groups within the United States. Inclusion criteria for participation were as follows: (a) 18 years old or older, (b) diagnosis of SCI and (c) able to engage in some form of independent physical activity and exercise. A total of 144 surveys were completed online. Participants ranged in age from 19 to 76 years (M = 44.10, SD = 12.84). Over half of the participants were male (n = 88, 61%) and the majority of the sample identified themselves as European American (81.3%), followed by Latino (9.0%), African American (5.6%), Asian (1.4%), Native American (0.7%), and others (2.1%). Over 95% of the participants completed high school and over half (57%) earned a tertiary degree or higher. In regards to employment, 41.3% were working either full-time or part-time, 23.8% described themselves as retired or not seeking employment, 20.6% were seeking employment, and 14.3% had volunteer positions. The majority of the participants reported a spinal cord lesion at the cervical level (41.3%) or thoracic level (43.7%), while those reporting a lesion at the lumbar level (14.3%) were less frequent.
Measures
Participants completed the Barriers to Health Promoting Activities for Disabled Persons Scale (BHADP; Becker, Stuifbergen, & Sands, Reference Becker, Stuifbergen and Sands1991), the Self Report Functional Independence Measure (SRFM; Keith, Granger, Hamilton, & Sherwin, Reference Keith, Granger, Hamilton and Sherwin1987), and the MOS Short form Health Survey (SF-12v2; Ware, Kosinski, & Keller, Reference Ware, Kosinski and Keller1996). These are self-report measures on perceived barriers to physical activity and exercise, functional disability and physical health-related quality of life, respectively.
Perceived barriers to physical activity and exercise
The BHADP was used to evaluate perceived barriers to physical activity and exercise (Becker, Stuifbergen, & Sands, 1991). The scale is comprised of 18 items and two subscales: external barriers (e.g. ‘lack of convenient facilities’) and motivation (e.g. ‘too tired’). Items were rated using a 4-point Likert-type scale (1 = never to 4 = routinely). Total scores range from 18 to 72, and higher scores indicate greater perceived barriers. Becker et al. (1991) reported that the internal consistency reliability estimate of the scale was 0.82.
Functional disability
The severity of SCI-related disability was measured with the SRFM, a modified version of the Functional Independence Measure (FIM; Keith, Granger, Hamilton, & Sherwin, Reference Keith, Granger, Hamilton and Sherwin1987). The SRFM has three subscales: basic activities of daily living (ADL), instrumental activities of daily living (IADL) and resource utilization. The present study only included the ADL subscale that has 13 items. Items were rated using a 4-point Likert-type scale (1 = total help or never do to 4 = no extra time or help). Total scores range from 13 to 52, and items were reverse scored so that high scores indicate high functional dependence/severity and low scores indicate high functional independence. Hoenig et al. (Reference Hoenig, McIntyre, Sloane, Branch, Truncali and Horner1998) reported the intraclass correlation coefficient and internal consistency reliability estimates were 0.90 and 0.96, respectively.
Physical health-related quality of life
The SF-12v2 quantified physical health-related quality of life. The SF-12v2 is composed of 12 items and eight subscales, but only the following physical-health related subscales were used for the current study: (a) physical functioning; (b) role limitations due to physical problems; (c) bodily pain; (d) general health; and (e) vitality. Items were rated on either a 5-point Likert-type scale (1 = excellent to 5 = poor), or a 3-point Likert-type scale of (1 = yes, limited a lot to 3 = no, not limited at all). The subscale items were summed to generate a physical component summary scale (PCS). The scores were standardised on a general population sample as well (M = 50, SD = 10), with higher scores indicating better quality of life. Test-retest reliability over a 2-week interval was estimated at 0.89 for the SF-12 PCS (Ware et al., Reference Ware, Kosinski and Keller1996).
Procedure
After receiving a letter of support from the National Spinal Cord Injury Association (NSCIA) and IRB approval, a study announcement was posted on the NSCIA website and emailed to members and colleagues with a direct link to the anonymous online survey. The survey took approximately 30 minutes to complete. No compensation was offered for completing the survey, but in order to encourage a greater amount of participation, the participants were offered an opportunity to enter a random drawing for one of 25 retail store gift cards valued at $20 upon survey completion.
Data Analysis
The Statistical Package for the Social Sciences (SPSS 15.0) for Windows was used to perform all data analyses. Scores on all measures were computed as the mean item response on each instrument in order to facilitate understanding and interpretation of the meaning of scores in terms of participant responses. Data were summarised by using descriptive statistics, and the measurement characteristics of the BHADP were examined by using factor analysis. The primary analyses included multivariate analysis of variance and hierarchical regression analysis. Multivariate analysis of variance (MANOVA) was used to determine whether participants in the three functional disability groups differed from each other on the two subscales for perceived health barriers to physical activity. Since there were unequal sample sizes for the groups, Pillai's trace was used to evaluate the main effect among the three functional disability groups as it is considered robust for testing the multivariate effect to produce acceptable power and control Type I error (Olsen, Reference Olson1976). Various analytic strategies have been developed for evaluating mediator hypotheses (MacKinnon, Lockwood, Hoffman, West, & Sheets, Reference MacKinnon, Lockwood, Hoffman, West and Sheets2002; Shrout & Bolger, Reference Shrout and Bolger2002), but the most parsimonious strategy involves an application of a 3-step method using multiple regression and correlation techniques proposed by Baron and Kenny (Reference Baron and Kenny1986). In this study, it was hypothesised that the association between functional disability and physical health-related quality of life would be partially mediated by perceived barriers. An a priori power analysis was conducted for the total R 2 value for a multiple regression analysis with two predictor variables, power equal to 0.80, and an alpha level of 0.05. G*Power (Faul, Erdfelder, Lang, & Buchner, Reference Faul, Erdfelder, Lang and Buchner2007), a software tool for a statistical power analysis, yielded a sample size of 68 for a medium effect size (f 2 = 0.15; Cohen, Reference Cohen1988). With only two predictor variables, the sample size of 144 was judged to be more than adequate for regression analysis.
Results
Perceived Barriers to Physical Activity and Exercise
The BHADP scale was subjected to a principal-components analysis. The Kaiser-Meyer-Olkin (KMO) resulted in a measure of sampling adequacy of .84 (greater than 0.50) and the Bartlett's test of sphericity, χ 2 (153, N = 144) = 993.11, p < 0.001, which indicated it was appropriate to proceed with factor analysis. The Kaiser-Guttman rule (eigenvalue greater than one) was used to determine the number of factors to be retained. Five factors were indicated using this rule, resulting in several trivial factors. Cattell's scree test was then used as an alternative to determine the number of factors to be retained. A two-factor solution was indicated using this method. To ensure no meaningful solution was overlooked one-, two-, and three-factor solutions were examined. The two-factor solution (which accounted for 44% of the total variance) was found to be parsimonious, had good simple structure, and compared to the one- and three-factor solutions, could be most meaningfully interpreted. All items loaded on one of the two factors at the level of 0.31 or above. Upon examination of the item clusters, the first factor, which accounted for 35% of the variance, appeared to include external barriers items such as ‘lack of convenient facilities’, ‘lack of transportation’ and ‘lack of money’. The second factor, which accounted for 9% of the variance, appeared to include motivation items such as, ‘feeling I can't do things correctly’, ‘embarrassment about my appearance’ and ‘feeling like what I do doesn't help’.
In order to determine if the two identified factors might be used as subscales, internal consistency reliabilities were examined. Cronbach's alphas for the seven-item external barriers subscale and the eleven-item motivation subscale were 0.81 and 0.83, respectively.
Perceived Health Barriers and Functional Disability
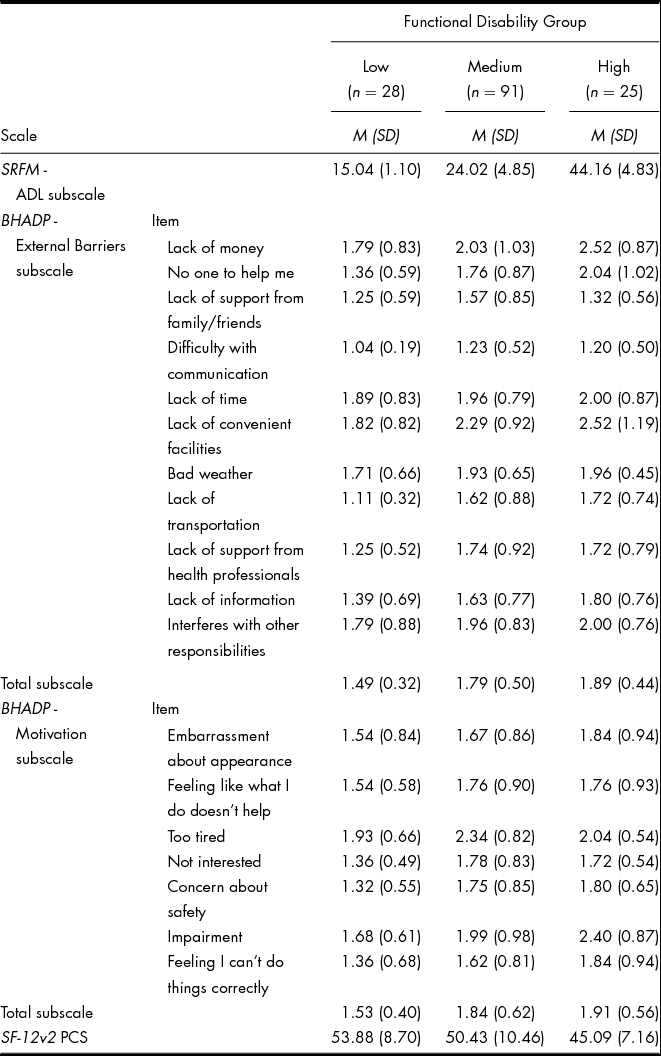
Individuals with SCI were classified into three functional disability groups based on their average SRFM scores: low (1 SD below the mean), medium and high (1 SD above the mean). MANOVA was used to examine group differences in perceived barriers across the three functional disability groups. Functional disability was found to significantly contribute to group differences in perceived barriers, with a Pillai's trace = 0.083, F(4,282) = 3.05, p < 0.02, η 2 = 0.041. On finding significant results, a follow-up univariate analysis of variance (ANOVA) was computed for each dependent variable. The alpha level was divided by two, for each pairwise comparison to control for Type I error (∝ = 0.05/2 = 0.025). These results indicated significant differences between the three functional disability groups for the two barrier factors: external barriers and motivation. The mean item and total subscale scores for the BHADP, in addition to SRFM and SF-12, are provided in Table 1.
TABLE 1 Mean Item and Subscale Scores for Three Functional Disability Groups on SRFM, BHADP and SF-12v2

Note. SRFM = Self Report Functional Independence Measure; BHADP = Barriers to Health Promoting Activities for Disabled Persons Scale; SF-12v2 PCS = MOS Short form Health Survey physical component summary scale. BHADP Items rated on a 4-point scale: 1 = Never a problem, 2 = Sometimes a problem, 3 = Often a problem, and 4 = Routinely a problem.
Post hoc comparisons using the Bonferroni procedure indicated that participants in the low functional disability group had a lower level of external barriers and motivation than the individuals in the medium and high functional disability groups. A close examination of the items indicated that low functional disability groups reported less difficulty with external barrier items, such as ‘lack of convenient facilities’, ‘lack of transportation’ or ‘lack of support from health professionals’. Moreover, low functional disability groups displayed reduced problems with motivation items, such as ‘impairment’, ‘concern about safety’ and ‘feeling I can't do things correctly’.
Perceived Barriers, Functional Disability and Physical Health-Related Quality of Life
The Rand Corporation scoring algorithm was utilised to compute the t-score for the physical component summary scale of the SF-12v2, a health-related quality of life measure. Descriptive statistics revealed that participants’ t-scores on physical health-related quality of life was lower (M = 48.87, SD = 9.27) than the general population mean (M = 50.0, SD = 10.0). Regarding functional disability, participants with SCI in this study do appear to have functional limitations (M = 25.77, SD = 10.13). In addition, functional disability was found to be inversely related to physical health-related quality of life (r = −0.26, p < 0.01). Conversely, functional disability was positively associated with perceived health barriers (r = 0.26, p < 0.01).
The first step of the mediation analyses was to establish a significant relationship between the predictor and outcome variables by regressing physical health-related quality of life on functional disability (see Table 2). As expected, the association between functional disability (IV) and physical health-related quality of life (DV) was significant: β (95% CI) = −0.26 [−0.42, −0.10]. The association was considered significant because the 95% CI excludes 0, which means the effect size differs significantly from 0, p < 0.05. Next, the relationship between the IV (functional disability) and the mediator (perceived barriers) was assessed. Functional disability was significantly related to perceived barriers: β (95% CI) = 0.26 [0.10, 0.42]. Finally, physical health-related quality of life (DV) was simultaneously regressed onto functional disability (IV) and perceived barriers (mediator). The potential mediator was significantly related to the DV (physical health-related quality of life), while statistically controlling for the IV, β (95% CI) = −0.26 [−0.42, −1.0]. The model accounted for 13% of the variance in physical health-related quality of life, R = 0.36, R 2 = 0.13, F (4, 205) = 10.48, p < 0.001, and is considered a small effect size (Cohen, Reference Cohen1988, Reference Cohen1992).
TABLE 2 Steps in Testing Perceived Barriers as a Mediator between Functional Disability and Physical Health-Related Quality of Life (QOL)

*p < .05, **p < .01.
In addition, the association between functional disability and physical health-related quality of life in the final regression equation was examined. This was also statistically significant, β (95% CI) = −0.19 [−0.35, −0.03]. The β for functional disability was reduced from −0.26 to −0.19 after controlling for the effect of the mediator. Thus, although the mediating variable of perceived barriers helps to explain the association between functional disability and physical health-related quality of life, it does not completely explain the relationship.
Discussion
This study explored the potential relationships between functional disability and perceived barriers to physical activity and exercise in a sample of persons with SCI. Regarding the first research question, the results of the MANOVA procedure indicated statistically significant differences in perceived barriers to physical activity across levels of functional disability. Participants in the low severity group endorsed fewer external barriers and motivation than participants in the medium and high severity groups. While these results indicated that individuals’ levels of functional disability were related to perceived barriers, functional disability was not associated with types of perceived barriers (i.e. internal, external barriers). Therefore, functional disability – but not barrier type – was associated with barriers to physical activity and exercise. These findings are similar to results from two previous studies indicating that SCI severity is a predictor of exercise participation (Scelza et al., Reference Scelza, Kalpakjian, Zemper and Tate2005; Vissers et al., Reference Vissers, Van dB-E, Sluis, Bergen, Stam and Bussmann2008). Although the present results are consistent with Scelza et al., Reference Scelza, Kalpakjian, Zemper and Tate2005 and Vissers et al. (Reference Vissers, Van dB-E, Sluis, Bergen, Stam and Bussmann2008), they are inconsistent with findings reported by Roberton et al. (Reference Roberton, Bucks, Skinner, Allison and Dunlop2011); and consequently, may substantiate concerns that Roberton et al. (Reference Roberton, Bucks, Skinner, Allison and Dunlop2011) was underpowered.
With regard to the second research question, a meditation analysis was performed to test perceived health barriers as a partial mediator of the relationship between functional disability and physical health-related quality of life. The mediation analysis was comprised of a series of hierarchical multiple regression equations for which participants were included as a single group. Results indicated that for the complete sample, functional disability had significant effects on physical health-related quality of life, that perceived health barriers had significant effects on the physical health-related quality of life, and that the introduction of perceived health barriers reduced, -but did not eliminate, -effects of functional disability on physical health-related quality of life. These findings yielded support for perceived health barriers as a partial mediator and correspond to a predictive model in which functional disability is associated with physical health-related quality of life, indirectly through its association with perceived barriers. A finding of perceived health barriers as a partial mediator (rather than a complete mediator) is consistent with previous research in the literature indicating that additional factors such as mental health, social support and employment status also mediate the relationship between functional disability and physical well-being (Dijkers, Reference Dijkers1997; Kennedy & Rogers, Reference Kennedy and Rogers2000).
Implications
Results from this study highlight several important implications for rehabilitation theory development, practice and research focused on working with individuals with SCI. Findings related to the primary research questions are consistent with central tenets of the International Classification of Functioning, Disability, and Health (ICF) framework. The ICF framework provides a biopsychosocial perspective that accounts for individuals’ levels of activity (e.g., exercise participation) as a product of the interaction between health conditions (e.g., SCI severity) and contextual factors (e.g., perceived barriers) (World Health Organization, 2002). In line with the ICF model, results support the value of rehabilitation strategies that include holistic assessment and consideration of individuals’ needs, and cross-disciplinary strategies focused on diminishing both external and motivational barriers to physical activity and exercise. Future research focused on the relationship between external and internal barriers to physical activity and exercise would enhance the understanding of health behaviours for individuals with SCI and better inform the implementation of behavioural health and rehabilitation interventions. Specifically, empirical research investigating a potential causal relationship between internal barriers and external barriers, as well as the relative stability of internal barriers across time, could provide useful treatment information.
Limitations
A few methodological limitations should be considered when interpreting the results of this study. First, the characteristics of a convenient sample may limit the generalisability of findings. The results also describe online survey responses from a mostly European American sample. Sample data collected online may underrepresent individuals (e.g. ethnic minorities) with limited access to computers or other expensive resources (Hunter, Reference Hunter2012). Other authors (e.g. Scelza et al., Reference Scelza, Kalpakjian, Zemper and Tate2005) have raised substantial concern that limitations to community access can arise as a function of lower socioeconomic status; therefore, an ecologically based disability variable may have different implications for members of these groups.
Two additional methodological concerns should be noted as study limitations. The study findings utilised responses to self-report measures. The literature indicates that results derived from self-report data may represent bias that affects relationships of substantive interest and should be interpreted with caution (Palmer, Graham, Taylor, & Tatterson, Reference Palmer, Graham, Taylor and Tatterson2002). Finally, the primary results reflect a descriptive design (multivariate analysis of variance, hierarchical regression analysis) using cross-sectional data, which consequently does not establish causality.
Conclusion
The goal of the present study was to explore the relationship between functional disability and perceived barriers to physical activity and exercise in persons with SCI. Primary findings indicated that functional disability was significantly associated with perceived barriers to physical activity and exercise in people with SCI. Meditational analysis demonstrated that perceived health barriers partially explained the relationship between functional disability and physical health-related quality of life. Overall, the current results support the applicability of the biopsychosocial perspective inherent in the ICF, and the value of cross-disciplinary collaboration in rehabilitation work with individuals with SCI.