Introduction
Superior semicircular canal dehiscence is a relatively novel diagnosis that was first described by Minor et al. in 1998.Reference Minor, Solomon, Zinreich and Zee1 The initial series described patients with chronic disequilibrium, vertigo (induced by either pressure or sound) and nystagmus. A bony dehiscence overlying the semicircular canal was identified in these patients, and following semicircular canal resurfacing, patients experienced symptomatic improvement.Reference Minor, Solomon, Zinreich and Zee1 In the subsequent two decades, superior semicircular canal dehiscence has become an increasingly recognised cause of vestibular and auditory symptoms in both adult and paediatric patients.Reference Bi, Brewster, Poe, Vernick, Lee and Corrales2 With increased awareness, additional symptoms have been identified, such as pulsatile tinnitus, autophony and hyperacusis to otherwise benign bodily functions.Reference Allsopp, Kim, Robbins, Page and Dornhoffer3
Sound pressure entering the oval window via the stapes usually exits through the round window. In superior semicircular canal dehiscence, there is a path of low impedance for pressure entering through the oval window to dissipate into the labyrinth as opposed to the cochlea.Reference Ward, Carey and Minor4 The result is a loss of energy for air-conducted sound. Conversely, the dehiscence allows bone-conducted sounds to access the inner-ear perilymph, allowing a communication between this perilymph and the cochlea. The result is increased perception of bone-conducted sounds, termed ‘bony hyperacusis’.Reference Ward, Carey and Minor4
The diagnosis of superior semicircular canal dehiscence is suspected in cases of sound or pressure induced nystagmus in the plane of the affected semicircular canal. Vestibular-evoked myogenic potential tests and audiometry are used to aid diagnosis, which is confirmed on high-resolution temporal bone computed tomography (CT).Reference Beyea, Agrawal and Parnes5 The majority of patients can be managed conservatively with avoidance of provocative stimuli.Reference Beyea, Agrawal and Parnes5 Surgery is reserved for cases of intractable or debilitating symptoms that persist despite conservative management.Reference Bi, Brewster, Poe, Vernick, Lee and Corrales2
The traditional surgical approach involves resurfacing or plugging the superior semicircular canal via a middle cranial fossa approach. Recent studies have demonstrated good outcomes from transmastoid approaches to plugging or capping. This approach is more familiar to otologists and avoids a craniotomy.Reference Allsopp, Kim, Robbins, Page and Dornhoffer3,Reference Beyea, Agrawal and Parnes5 We are a busy otology practice with a large balance service. We therefore set up a new service providing transmastoid plugging for superior semicircular canal dehiscence. In this study, we described the outcomes of our initial surgical procedures for transmastoid plugging.
Materials and methods
A new service for transmastoid superior semicircular canal plugging was introduced by the senior author (PB) in the University Hospitals of Leicester NHS Trust. This underwent approval by the Trust’s new intervention guidance committee. The surgical procedures were performed by the senior author at University Hospitals of Leicester NHS Trust with proctorship from the senior surgeon (RI) from the University Hospitals of Birmingham NHS Trust.
Three patients underwent transmastoid semicircular canal plugging for superior semicircular canal dehiscence between September 2019 and March 2020. In order to evaluate the efficacy of the surgery as well as the service, patients were asked to complete a questionnaire evaluating symptoms of superior semicircular canal dehiscence (pre-operative and post-operative) and quality-of-life measures (post-operative). Pre-operative and post-operative vestibular-evoked myogenic potential tests were also recorded. This study was approved by the audit committee of the University Hospitals of Leicester NHS Trust (reference: 10735).
Diagnostic workup
All patients underwent pre-operative audiometric testing, tympanometry, vestibular-evoked myogenic potential tests, detailed vestibular testing and high-resolution CT scan of the temporal bones. Diagnosis was confirmed with radiological evidence of superior semicircular canal dehiscence supported by vestibular-evoked myogenic potential results.
Surgical technique
The procedure was performed under general anaesthetic. A 4 cm superiorly based post-auricular incision was used, and a standard cortical mastoidectomy was performed using a cutting burr. The lateral canal was identified and skeletonised. The bone between the lateral canal and the tegmen was carefully drilled away using a diamond burr until the superior canal was visible. The superior canal was then blue-lined proximally and distally to the area of dehiscence. Small fenestrations were created in the semicircular canal either side of the dehiscence, avoiding the ampulla and common crus. Fascia and bone dust were used to plug the canal. The plugged areas were then covered with bone dust and sealed with fibrin sealant.
Outcome measures
Patients undergoing transmastoid semicircular canal plugging completed a questionnaire prior to and equal to or more than six months after surgery. The questionnaire consisted of 11 statements to assess the disability caused to the patient by each of the symptoms of superior semicircular canal dehiscence. Patients graded each statement on a Likert scale of 1 (not bothered at all by symptom) to 5 (completely disabled by symptoms).
Patients also completed a post-operative quality-of-life questionnaire, in the form of the Glasgow Benefit Inventory. The Glasgow Benefit Inventory is a validated patient-recorded outcome measure used in otolaryngology. It comprises 18 questions, each with 5 answers on a Likert scale. The total score ranges between −100 (poorest outcome) and 100 (best outcome). A score of 0 indicates no change.Reference Hendry, Chin, Swan, Akeroyd and Browning6 The Glasgow Benefit Inventory has sub-sections that are split into general, physical and social categories.
Results
Between September 2019 and March 2020, three patients underwent transmastoid plugging of superior semicircular canal dehiscence. In all three patients, the dehiscence was unilateral and confirmed on CT imaging. There were two females and one male. The age range of the patients was 41–45 years with a mean age of 42 years. None of the patients had previously undergone any surgical intervention for superior semicircular canal dehiscence. Mean follow up was 12 months with a range of 8–14 months.
Symptoms and quality-of-life outcomes
The subjective reported disability caused by symptoms of superior semicircular canal dehiscence before and after surgery are mapped out in Table 1 for three patients, identified as A, B and C. Responses to the Glasgow Benefit Inventory are outlined in Table 2, and the overall Glasgow Benefit Inventory score, as well as breakdown by category, is outlined in Table 3.
Table 1. Pre- and post-operative disability caused by symptoms of superior semicircular canal dehiscence

*Pre-operative responses are indicated by uppercase letters and an asterisk; post-operative responses are indicated by lowercase letters with a cross. Three patients have been nominated as A, B and C
Table 2. Patient responses to Glasgow Benefit Inventory questionnaire

Three patients have been nominated as A, B and C
Table 3. Glasgow Benefit Inventory scores by category

Score interpretation: −100 is poorest outcome; 0 indicates no change; +100 is best possible outcome
Vestibular-evoked myogenic potential tests
High-frequency vestibular-evoked myogenic potential testing is a highly specific test for the detection of superior semicircular canal dehiscence and is used in the decision-making process to guide surgical intervention.Reference Noij and Rauch7 Tests on patients with superior semicircular canal dehiscence demonstrated abnormally low thresholds and large amplitude potentials. Vestibular-evoked myogenic potential testing is also a valuable tool in post-operative monitoring of patients.Reference Rinaldi and Portmann8 Pre-operative and post-operative vestibular-evoked myogenic potential results for our patients are displayed in Figure 1. Because of current coronavirus disease 2019 restrictions on elective activity, we were unable to obtain post-operative vestibular-evoked myogenic potential tests for patient B.
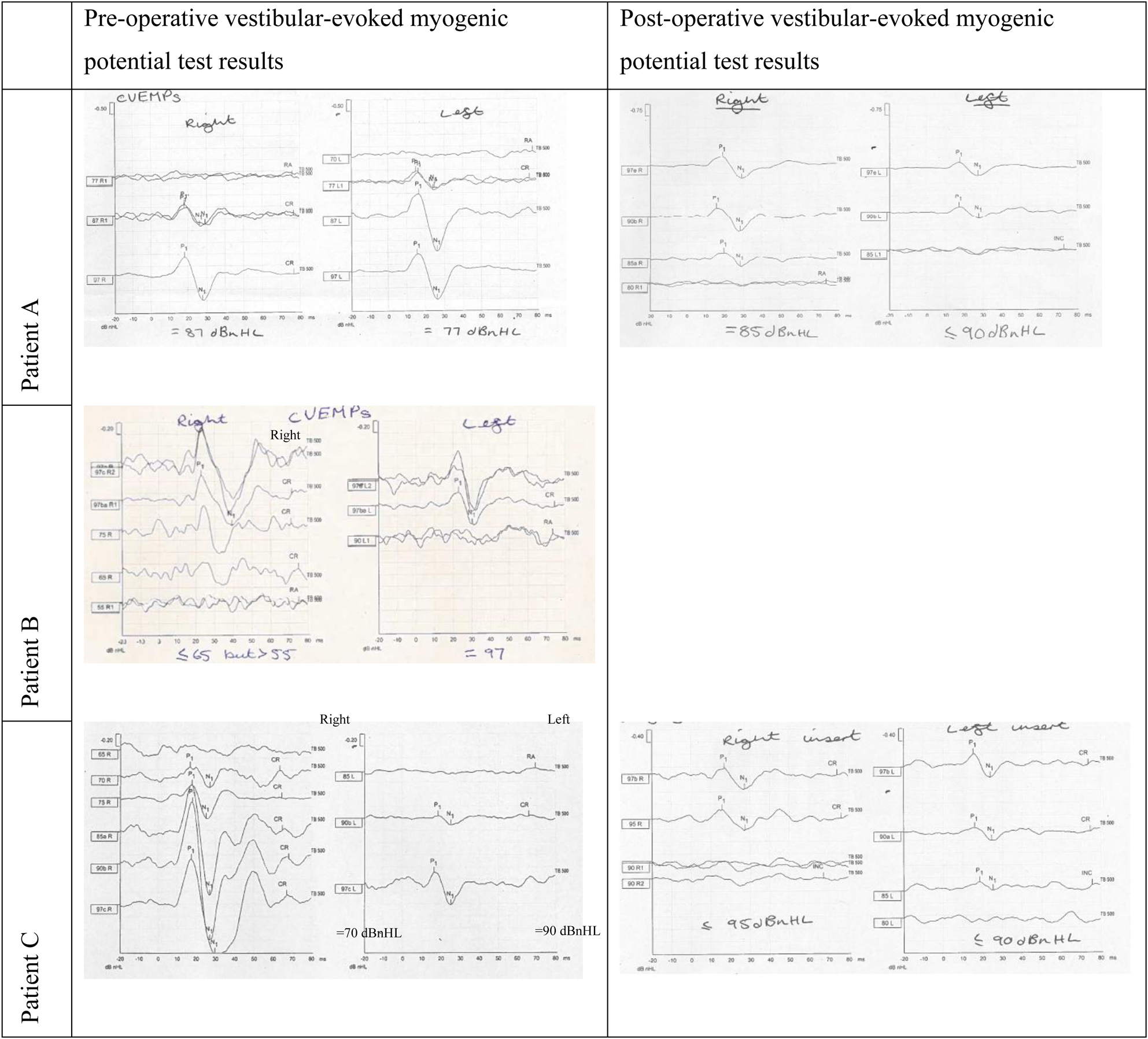
Fig. 1. Vestibular-evoked myogenic potential test results pre- and post-operatively. Unable to obtain post-operative vestibular-evoked myogenic potential for patient B because of coronavirus disease 2019 restrictions.
Discussion
We describe herein our experience with setting up a new service to provide transmastoid plugging of dehiscent semicircular canal and the initial results. Superior semicircular canal dehiscence remains a relatively novel condition, and good results have been described with the middle cranial fossa approach as well as the transmastoid approach to plugging or resurfacing of the dehiscent semicircular canal.Reference Bi, Brewster, Poe, Vernick, Lee and Corrales2,Reference Beyea, Agrawal and Parnes5,Reference Amoodi, Makki, McNeil and Bance9–Reference Goddard and Wilkinson11 The middle cranial fossa approach is primarily used in neurosurgical units. The transmastoid procedure is suited to most otologists because of familiarity with the approach,Reference Allsopp, Kim, Robbins, Page and Dornhoffer3,Reference Beyea, Agrawal and Parnes5 and the procedure can be performed in any ENT unit and avoids the risks of craniotomy.
Not every dehiscent semicircular canal requires surgical intervention. Conservative management with avoidance of provocative stimuli is chosen by many patients once the condition is explained to them. Surgery is reserved for cases of intractable or debilitating symptoms. Symptomatic improvement following surgical intervention has been reported for all approaches.Reference Bi, Brewster, Poe, Vernick, Lee and Corrales2,Reference Beyea, Agrawal and Parnes5,Reference Amoodi, Makki, McNeil and Bance9–Reference Goddard and Wilkinson11 The middle cranial fossa approach is the original technique described by Minor et al. and is the traditional approach for which the most data is available.Reference Ward, Agrawal, Nguyen, Della Santina, Limb and Francis12 Proponents of this approach argue it offers a more extensive visualisation of the dehiscence and is safer in challenging cases where there may be a poorly pneumatised temporal bone, extensive tegmen defects or a low-lying temporal fossa.Reference Bi, Brewster, Poe, Vernick, Lee and Corrales2
On the other hand, the transmastoid approach avoids the morbidity of a craniotomy and has a higher patient acceptance.Reference Schwartz, Almosnino, Noonan, Banakis Hartl, Zeitler and Saunders13 This approach is of interest to otologists as the transmastoid approach is familiar territory. A systematic review from 2017 showed that transmastoid plugging, when compared with the middle cranial fossa approach, reduced hospital stay, complication rates and revision rates.Reference Ziylan, Kinaci, Beynon and Kunst14 More than 90 per cent of patients report improvement in vestibular and hearing symptoms following semicircular canal plugging via a transmastoid approach (bone pâté or temporalis fascia).Reference Beyea, Agrawal and Parnes5
A systematic review of 20 studies and 150 cases found no significant statistical difference in terms of success rate and surgical complications between approach (transmastoid vs middle cranial fossa) and modalities of surgery (plugging, capping, resurfacing and plugging with resurfacing).Reference Gioacchini, Alicandri-Ciufelli, Kaleci, Scarpa, Cassandro and Re15 There are several studies that report higher success rates for plugging as compared with canal resurfacing,Reference Minor16 and a meta-analysis encompassing 64 operations found higher success rates for plugging and capping techniques when compared with canal resurfacing.Reference Vlastarakos, Proikas, Tavoulari, Kikidis, Maragoudakis and Nikolopoulos17
We set up a surgical transmastoid superior semicircular canal dehiscence service in a busy otology unit. The procedure underwent approval by the Trust’s new intervention guidance committee. Support and proctorship were elicited (and kindly provided) from the senior surgeon (RI). Patients were provided with comprehensive information about the middle cranial fossa and transmastoid approaches and offered the option of referral to a lateral skull base or neurosurgical centre if they preferred the middle cranial fossa approach or if the temporal bone anatomy (as assessed on the pre-operative CT scan) precluded the transmastoid approach.
In our initial series, all three patients underwent transmastoid superior semicircular canal dehiscence repair successfully. No immediate post-operative complications occurred and hearing was preserved. One patient developed benign paroxysmal positional vertigo that responded to the Epley manoeuvre; this has been described to occur following superior semicircular canal dehiscence surgery previously.Reference Barber, Cheng, Owoc, Lin, Remenschneider and Kozin18 Pre-operative and post-operative patient symptom scores demonstrated improvement in symptoms post-operatively (Table 1). Interestingly, all symptoms showed improvement in scores with the exception of ‘fullness in the ear’, which tended towards persistence despite surgery. All patients in our series demonstrated an improvement in quality-of-life outcomes following transmastoid superior semicircular canal dehiscence (Table 3). This improvement encompassed general quality-of-life measures as opposed to those specific to social support and physical health measures (Table 3).
• Superior semicircular canal dehiscence has become an increasingly recognised cause of vestibular and auditory symptoms in both adults and children
• Diagnosis is suspected in cases of sound or pressure induced nystagmus in the plane of the affected semicircular canal
• Traditional surgical approach involves resurfacing or plugging via a middle cranial fossa approach
• Recent studies have demonstrated good outcomes from a transmastoid approach
• The transmastoid approach is more familiar to otologists, avoids the morbidity of a craniotomy and has a higher patient acceptance
• This study used the transmastoid approach; all patients reported improvement in symptoms and quality-of-life outcomes
Limited data is currently available in literature on the patient-reported outcomes of superior semicircular canal dehiscence surgery. In our experience, pre-operative and post-operative recording of patient outcomes is very helpful in assessing the surgical results and also providing patients with a measurable readout of their symptom improvement. Our data has the limitation of being a small series but nevertheless demonstrates a clear benefit in terms of patient-reported outcomes. The lack of a validated disease-specific outcome measure for superior semicircular canal dehiscence renders it difficult to objectively delineate outcomes.Reference Ward, Carey and Minor4 In addition to patient questionnaires, we also propose the routine use of post-operative vestibular-evoked myogenic potentials to document improvement in vestibular-evoked myogenic potential thresholds as a measure of effective plugging of superior semicircular canal dehiscence.
Conclusion
This was a report of our initial successful experience with transmastoid plugging performed for superior semicircular canal dehiscence and the patient-reported outcome measures. In all our patients, symptomatic improvement and improvement in quality-of-life measures were reported. There were no surgical complications.
Acknowledgements
A special thanks to Shazia Ahmed for facilitating data collection for this study.
Competing interests
None declared






