Bipolar disorder is a severe mental illness characterised by recurrent depressive and manic episodes and associated with high levels of disability and premature mortality.1–Reference Fekadu, Kebede, Alem, Fekadu, Mogga and Negash3 Although there are limited data from low- and middle-income countries (LMICs), the burden of bipolar disorder may be even higher in these settings because of the high treatment gap.1 As few as 10% of people with bipolar disorder receive care in some LMICs.Reference Fekadu, Hanlon, Thornicroft, Lund, Kaaya and Alem4, Reference Kebede, Alem, Shibire, Deyassa, Negash and Beyero5 Even those who receive care may have limited access to evidence-based interventions, including mood stabilisers and psychosocial interventions.Reference Kebede, Alem, Shibire, Deyassa, Negash and Beyero5, Reference Negash, Kebede, Alem, Melaku, Deyessa and Shibire6 In a cohort study of 312 community-ascertained people with bipolar disorder in Ethiopia, over 60% relapsed and only 5% remained continuously in remission over 2.5 years of follow-up,Reference Kebede, Alem, Shibire, Deyassa, Negash and Beyero5 which appears much lower than what has been reported in high-income countries.Reference Keck, McElroy, Strakowski, West, Sax and Hawkins7 Patients in low-income countries also appear to have substantially increased rates of mortality with nearly three decades of life lost because of premature death.Reference Fekadu, Medhin, Kebede, Alem, Cleare and Prince2
Mood stabilisers, such as lithium and sodium valproate, and atypical antipsychotics such as olanzapine, quetiapine and risperidone are the recommended evidence-based treatments for bipolar disorder.8 However, these medications are not widely available in many LMICs.Reference Fekadu, Hanlon, Thornicroft, Lund, Kaaya and Alem4, 9 As a result, people with bipolar disorder in LMICs are often treated with first-generation antipsychotics during the maintenance phase.Reference Kebede, Alem, Shibire, Deyassa, Negash and Beyero5, Reference Negash, Kebede, Alem, Melaku, Deyessa and Shibire6 First-generation antipsychotic medications are recommended in the latest version of the intervention guide of the Mental Health Gap Action Programme (mhGAP) in the absence of other options.10 However, they have extrapyramidal side-effects, especially when taken in high doses for an extended period of timeReference Pakpoor and Agius11 and have poor evidence of efficacy as a maintenance treatment. Psychological treatments may play a crucial role in improving the outcome of bipolar disorder in LMICs where first-line treatments are not available for the majority of the population.
There is evidence from high-income countries that complementing pharmacotherapy with psychoeducation, family therapy or cognitive–behavioural therapy (CBT) for people with bipolar disorder is more effective at preventing relapse, improving medication adherence and overall disease outcome than pharmacotherapy alone.Reference Scott, Paykel, Morriss, Bentall, Kinderman and Johnson12–Reference Perlick, Miklowitz, Lopez, Chou, Kalvin and Adzhiashvili14 The mhGAP intervention guideline recommends psychological intervention, especially psychoeducation to be delivered routinely for individuals with bipolar disorders.Reference Dua, Barbui, Clark, Fleischmann, Poznyak and van Ommeren15 However, to date there has been no published synthesis of the evidence on the efficacy of adjunctive psychological interventions for bipolar disorder in LMIC settings. In this systematic review we aimed to synthesise the evidence base for the efficacy of adjunctive psychological interventions in improving clinical and functional outcomes in people with bipolar disorder in LMICs.
Method
Scope of review
We reviewed studies that aimed to examine the efficacy of any psychological intervention in improving clinical and functional outcomes, including prevention of relapse or recurrence and hospital admissions; treatment adherence, biological rhythms, quality of life (QoL) and knowledge and attitude about bipolar disorder among people with bipolar disorder.
Search strategies
We searched Medline, PsycINFO, EMBASE, PubMed, Cochrane database for systematic review, Cochrane central register of controlled trials, Latin America and Caribbean Center on Health Science Literature and African Journal of Online databases since the inception of the respective databases until the second week of May 2017 with no language restriction. The following terms were used to identify psychological interventions: ‘Psychosocial intervention’ OR ‘Psychological intervention’ OR ‘Psychosocial therapy’ OR ‘Cognitive behavioral therapy’ OR ‘Cognitive Therapy’ OR ‘Behavior Therapy’ OR ‘Family focused intervention’ OR ‘Family intervention’ OR ‘Family therapy’ OR Psychoeducation OR ‘Interpersonal and social rhythm therapy’ OR ‘Social rhythm therapy’ OR ‘Interpersonal therapy’ OR ‘Mindfulness based cognitive therapy’ OR Psychotherapy OR ‘Expressed emotion’ OR ‘Individual therapy’ OR ‘Group therapy’). The search terms used for bipolar disorder were: ‘Bipolar disorder’ OR ‘Bipolar and related disorders’ OR Bipolar OR Mania OR ‘Major affective disorder’. We used the World Bank definition and list of countries to identify LMICs. The search terms for intervention, bipolar disorder and LMICs were combined with the Boolean term ‘AND’.
Outcomes of interest
The main measures of efficacy of psychological interventions included: number of relapses or recurrence, severity of mood symptoms, treatment adherence, QoL, functional status, number of hospital admissions, knowledge and attitudes about bipolar disorder, and stigma and biological rhythms. The review protocol was registered in the PROSPERO database (CRD42017054572).16
Inclusion criteria
Eligible articles were assessed against the following inclusion criteria:
(a) age: all ages were included;
(b) diagnosis: bipolar disorder I or II in any phase of the illness (depressive/manic/mixed episode or in remission);
(c) study setting: conducted in a LMIC according to the World Bank classification at the time of the study;17
(d) type of study: (i) randomised controlled studies (RCT), or (ii) controlled before-and-after study;
(e) comparison groups: usual care, waiting list control or an active adjunctive psychological intervention;
(f) type of intervention: any psychological intervention delivered either face to face (individual or group format) or online.
Data extraction
Studies were first screened based on of their titles and abstracts, with the full texts obtained for those fulfilling the inclusion criteria. Two researchers (M.D. and R.B.) screened and extracted data independently using a customised data extraction form, which was piloted before the main data extraction. Any discrepancies were reconciled through discussions. Excluded articles and reasons for exclusion were documented.
Quality assessment
The consolidated standards of reporting studies (CONSORT)Reference Schulz, Altman and Moher18 and the Cochrane assessment of risk of biasReference Higgins and Green19 were used to assess the quality of the studies. The CONSORT checklist has 25 items on the quality of reporting of each section of the study including funding sources. The Cochrane assessment of risk of bias measures selection bias, performance bias, detection bias, attrition bias and reporting bias. The quality of studies was assessed independently by two researchers (M.D. and R.B.) and any differences were reconciled by a third researcher (A.F.). Assessment of the quality of the included studies was not used to exclude studies, but, to inform interpretation of the findings.
Method of analysis
Key findings were summarised in the form of figures, tables and text. Although the original plan was to conduct a meta-analysis and generate summary effect sizes of interventions, this was not possible because of the heterogeneity of the included studies in terms of: type of intervention, number of intervention sessions, duration of follow-up, format of intervention delivery and qualifications of the individuals delivering the intervention.
Results
A total of 7987 articles were identified from the primary search. Of these, 532 were duplicates and were excluded. An additional 7213 were excluded because they were not related to bipolar disorder or to psychological interventions during the title screen and a further 162 during the abstract screen. Of the 80 studies included in full-text review, 62 were excluded because they were not from LMICs or were not related to bipolar disorder. This resulted in a total of 18 intervention studies for final analysis (Fig. 1). Four types of psychological intervention were identified: psychoeducation, family psychoeducation, CBT and mindfulness-based cognitive therapy (MBCT) (Table 1).
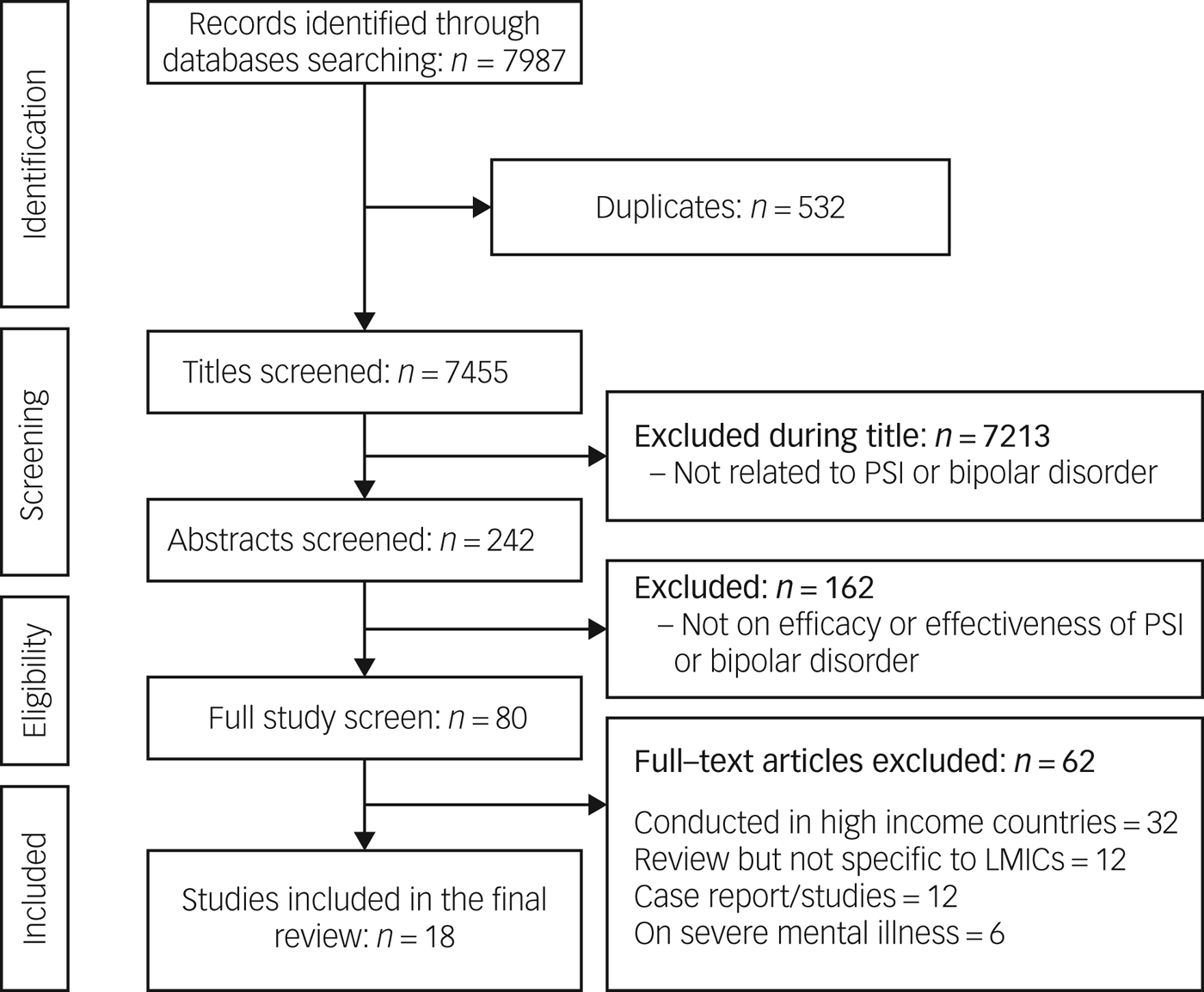
Fig. 1 PRISMA flow diagram of the study selection process.
Table 1 Summary of studies, interventions and patient characteristics for included studies
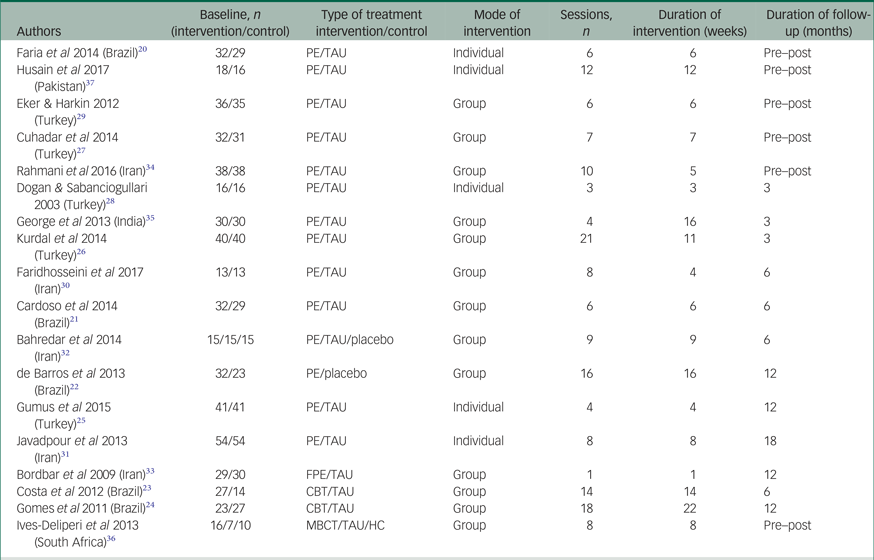
PE, psychoeducation; TAU, treatment as usual; FPE, family psychoeducation; CBT, cognitive–behavioural therapy; MBCT, mindfulness-based cognitive therapy; HC, Healthy control.
Included studies
All studies were conducted in upper-middle-income countries except two, which was conducted in middle-income countries. There was only one study from Africa (South Africa). All of the 18 studies were published between 2003 and 2017 and were conducted in six countries. Brazil,Reference Faria, de Mattos Souza, de Azevedo Cardoso, Pinheiro, Pinheiro and da Silva20–Reference Gomes, Abreu, Brietzke, Caetano, Kleinman and Nery24 TurkeyReference Gumus, Buzlu and Cakir25–Reference Eker and Harkin29 and IranReference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30–Reference Rahmani, Ebrahimi, Ranjbar, Razavi and Asghari34 each contributed five studies, and India,Reference George, Sharma and Nair35 South AfricaReference Ives-Deliperi, Howells, Stein, Meintjes and Horn36 and PakistanReference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 each contributing only one study. Fifteen studies examined psychoeducation (five individual, nine groups, and one family intervention); two studies were of group CBT; and one study was group MBCT. All studies were RCTs, and all but two studies compared adjunctive psychological interventions with treatment as usual. The nature of ‘treatment as usual’ or the type of medication, was not specified in all these studies. the two studies that used an intervention comparison group, had used an equal number of sessions of relaxation and informal conversation,Reference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22 or non-specific support.Reference Bahredar, Farid, Ghanizadeh and Birashk32 The total number of participants in each study ranged from 26Reference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30 to 59.Reference Bordbar, Soltanifar and Talaei33 Overall follow-up time after the end of intervention ranged from 0 to 18 months (Table 1).
Intervention content and intervention provider
Providers of the intervention were specified in 15 of the 18 studies and included mental health specialists or practitioners (BSc psychiatric nurses,Reference Gumus, Buzlu and Cakir25–Reference Cuhadar and Cam27 MSc psychiatric nurses,Reference Rahmani, Ebrahimi, Ranjbar, Razavi and Asghari34 clinical psychologists,Reference Costa, Cheniaux, Range, Versiani and Nardi23, Reference Bahredar, Farid, Ghanizadeh and Birashk32, Reference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 MSc research psychology students,Reference Cardoso, Farias, Mondin, da Silva, Souza and da Silva21 undergraduate psychologistsReference Faria, de Mattos Souza, de Azevedo Cardoso, Pinheiro, Pinheiro and da Silva20 psychiatrists or psychiatric residentsReference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22, Reference Javadpour, Hedayati, Dehbozorgi and Azizi31, Reference Bordbar, Soltanifar and Talaei33) and therapists or people with some form of clinical experience.Reference Gomes, Abreu, Brietzke, Caetano, Kleinman and Nery24, Reference Eker and Harkin29, Reference George, Sharma and Nair35 Although the majority of the studies did not indicated how the interventions were developed or adapted, most of the studies described the core content of the interventions. The content in most of the interventions was educational: education about bipolar disorder, symptoms of mania, depression, mixed and hypomanic episodes, causes and prognosis of bipolar disorder, treatment adherence and side-effects of medication, early identification of symptoms of relapse, triggering factors, substance use and regular habits and management plans or prevention strategies.
Participant recruitment and outcome measures
The study participants were aged at least 18 years in all of the studies. Most of the participants were in remission during recruitment to the study and were recruited from the out-patient setting of a teaching or university hospital or from a public hospital. Most were receiving pharmacotherapy and follow-up from psychiatrists. In the majority of studies the Young Mania Rating Scale was used to measure manic symptom severity either as a categorical scale with an average cut-off of nineReference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22–Reference Gumus, Buzlu and Cakir25, Reference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30, Reference Bahredar, Farid, Ghanizadeh and Birashk32, Reference Rahmani, Ebrahimi, Ranjbar, Razavi and Asghari34–Reference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 or as a continuous scale.Reference Faria, de Mattos Souza, de Azevedo Cardoso, Pinheiro, Pinheiro and da Silva20, Reference Cardoso, Farias, Mondin, da Silva, Souza and da Silva21 Similarly, in the majority of the studies, the Hamilton Rating Scale for Depression was used to measure depressive symptom severity either as a categorical scale with an average cut-off point of eightReference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22, Reference Gomes, Abreu, Brietzke, Caetano, Kleinman and Nery24, Reference Gumus, Buzlu and Cakir25, Reference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30–Reference Bahredar, Farid, Ghanizadeh and Birashk32, Reference Rahmani, Ebrahimi, Ranjbar, Razavi and Asghari34, Reference George, Sharma and Nair35 or as a continuous measure.Reference Faria, de Mattos Souza, de Azevedo Cardoso, Pinheiro, Pinheiro and da Silva20, Reference Cardoso, Farias, Mondin, da Silva, Souza and da Silva21 Five studies included people with bipolar I or II disorder, three studies recruited only individuals with bipolar I disorder and two studies recruited only those with bipolar II disorder; the remaining eight studies did not specify the type of bipolar disorder. In 16 studies, the DSM-IV was used as the diagnostic tool, with psychiatrist-confirmed diagnoses in 11 studies. Two studies did not describe who confirmed the diagnosis.Reference Cuhadar and Cam27, Reference George, Sharma and Nair35 Details of other outcome measures are provided in supplementary file 1 available at https://doi.org/10.1192/bjo.2018.46.
Quality of included studies
The overall quality of reporting of the studies was not satisfactory as per the CONSORT checklist. Only three of the studies were registered in a registration database. Although all studies clearly reported the objective of the study. Only 55% of the studies reported how the sample size was determined. Sources of funding and the role of funders were reported in only two-thirds of the studies. The risk of bias assessed with the Cochrane assessment tool was moderately high. Although randomisation was carried out in all the studies, the method of randomisation was unclear in 40% of studies and allocation concealment was unclear in 80% of studies. Fifteen studies were rated as unclear and three studies had a high risk of detection bias. One-third of the studies were rated as having high attrition bias because of unequal numbers of people dropping out in the randomised groups or different reasons for drop-out or because of attrition greater than 10%. One-third of studies were rated as being at high risk of reporting bias because they did not report the mean and standard deviation of mood severity symptoms, between-group differences for selected outcomes, and number of participants who had a relapsed/recurrence (see supplementary files 2–4).
Efficacy of interventions
Prevention of relapse/recurrence
Six studies (four psychoeducation, one family psychoeducation and one CBT) examined the impact of the psychological intervention on prevention of relapse or recurrence (Table 2). Psychoeducation was effective in reducing the relapse rate,Reference Gumus, Buzlu and Cakir25, Reference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30, Reference Javadpour, Hedayati, Dehbozorgi and Azizi31, Reference Bordbar, Soltanifar and Talaei33 as well as increasing mean time to first relapse.Reference Bordbar, Soltanifar and Talaei33 However, one study showed that psychoeducation was not effective in people who had multiple previous relapses.Reference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22 CBT was ineffective in decreasing the number of relapses but was effective in prolonging the median time to first relapse compared with treatment as usual.Reference Gomes, Abreu, Brietzke, Caetano, Kleinman and Nery24
Table 2 Psychological interventions for prevention of relapse/recurrence
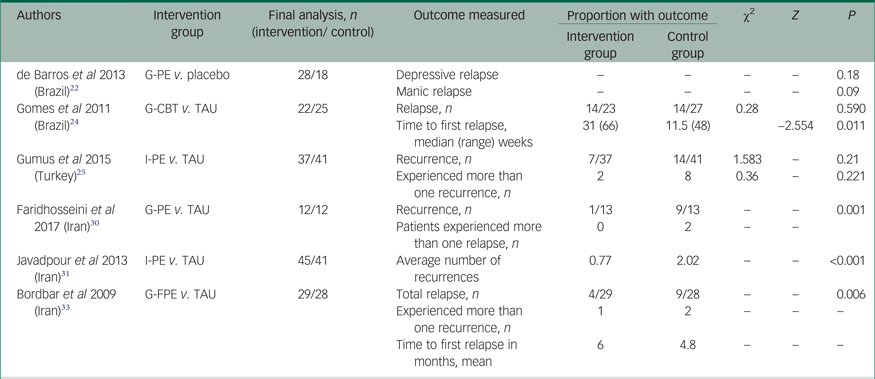
G-PE, group psychoeducation; G-CBT, group cognitive–behavioural therapy; TAU, treatment as usual; I-PE, individual psychoeducation; G-FPE, group family psychoeducation.
Reduction in symptom severity
Nine studies (seven psychoeducation, one CBT and one MBCT) assessed the efficacy of psychological intervention in reducing symptom severity. One study reported change in mood-only symptom severity within each of the randomised groupsReference Dogan and Sabanciogullari28 (Table 3).
Table 3 Psychological intervention for reducing symptom severity
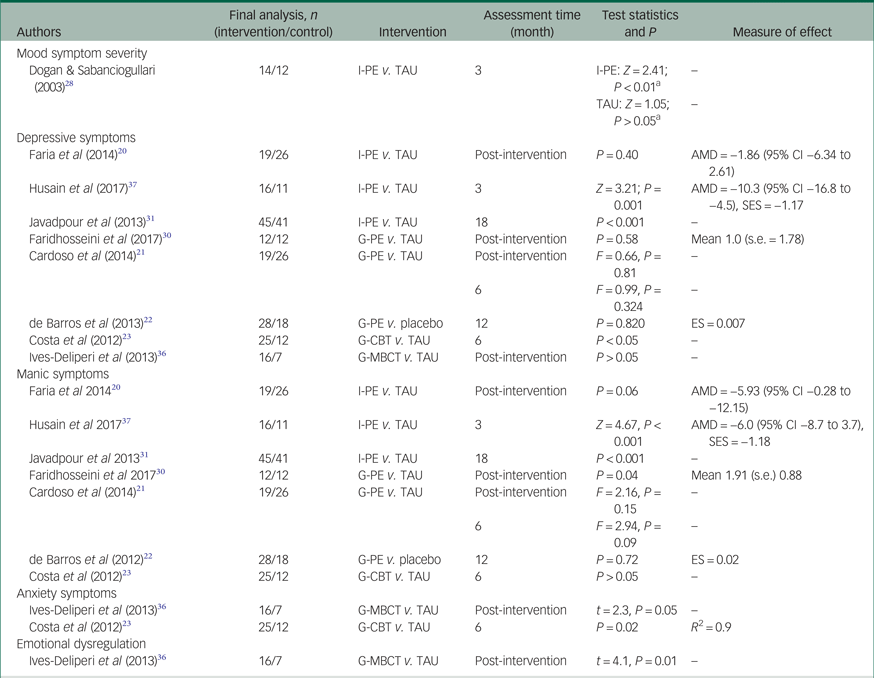
I-PE, individual psychoeducation; TAU, treatment as usual; AMD, adjusted mean difference; SES, standardised effect size; G-PE, group psychoeducation; ES, effect size; G-CBT, group cognitive–behavioural therapy; G-MBCT, group mindfulness-based cognitive therapy; R 2, squared value of correlation coefficient or the proportion of explained variation.
a. The comparison was made within arm and the reported result for the treatment group.
Studies reported significant reduction in general psychiatric symptom severity,Reference Dogan and Sabanciogullari28 depressive symptom severityReference Cardoso, Farias, Mondin, da Silva, Souza and da Silva21, Reference Javadpour, Hedayati, Dehbozorgi and Azizi31, Reference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 and manic symptom severity,Reference Faria, de Mattos Souza, de Azevedo Cardoso, Pinheiro, Pinheiro and da Silva20, Reference Cardoso, Farias, Mondin, da Silva, Souza and da Silva21, Reference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30, Reference Javadpour, Hedayati, Dehbozorgi and Azizi31, Reference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 immediately post-intervention and during follow-up. However, in one study where 60% of total participants had more than ten previous bipolar episodes, there was worsening of depressive symptoms in both groups and there was significant change and between-group difference in manic symptoms.Reference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22 CBT was effective in reducing depressive and anxiety symptoms compared with treatment as usual.Reference Costa, Cheniaux, Range, Versiani and Nardi23 MBCT was associated with significant improvement in anxiety symptoms, emotional dysregulation and mindfulness, but did not reduce depressive symptoms among intervention groups compared with the patients with bipolar disorder on the waiting list.Reference Ives-Deliperi, Howells, Stein, Meintjes and Horn36
Improvement in biological rhythms
Only one studyReference Faria, de Mattos Souza, de Azevedo Cardoso, Pinheiro, Pinheiro and da Silva20 from Brazil assessed the efficacy of six sessions of complementary psychoeducation in improving biological rhythms (sleep, activity, patterns of habitual daily behaviour (social rhythm) and eating pattern) among patients with bipolar disorder, 80% of whom had more than six previous bipolar episodes. The study reported significant improvement in the control rather than the intervention group (adjusted mean difference −10.84, 95% CI −20.6 to −1.07, P = 0.03).Reference Faria, de Mattos Souza, de Azevedo Cardoso, Pinheiro, Pinheiro and da Silva20
Improvement in knowledge, attitude and internalised stigma
Four psychoeducation studies were identified.Reference Cuhadar and Cam27, Reference Dogan and Sabanciogullari28, Reference George, Sharma and Nair35, Reference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 Three of the four studies assessed the efficacy of psychoeducation in improving knowledge and attitudes about bipolar disorder, and one trial assessed the efficacy of psychoeducation in reducing internalised stigma. Two of the four studies reported within-group difference by comparing post-intervention against baseline scores in each group.Reference Cuhadar and Cam27, Reference Dogan and Sabanciogullari28 Generally, the findings showed a positive effect of psychoeducation in improving knowledge and attitudes about bipolar disorder and internalised stigma (see supplementary file 5).
Improvement in treatment adherence
A total of nine studies, eight psychoeducation and one family-focused intervention, reported short- and long-term improvements in treatment adherence compared with treatment as usualReference Dogan and Sabanciogullari28–Reference George, Sharma and Nair35, Reference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 (Table 4).
Table 4 Psychological intervention to improve adherence
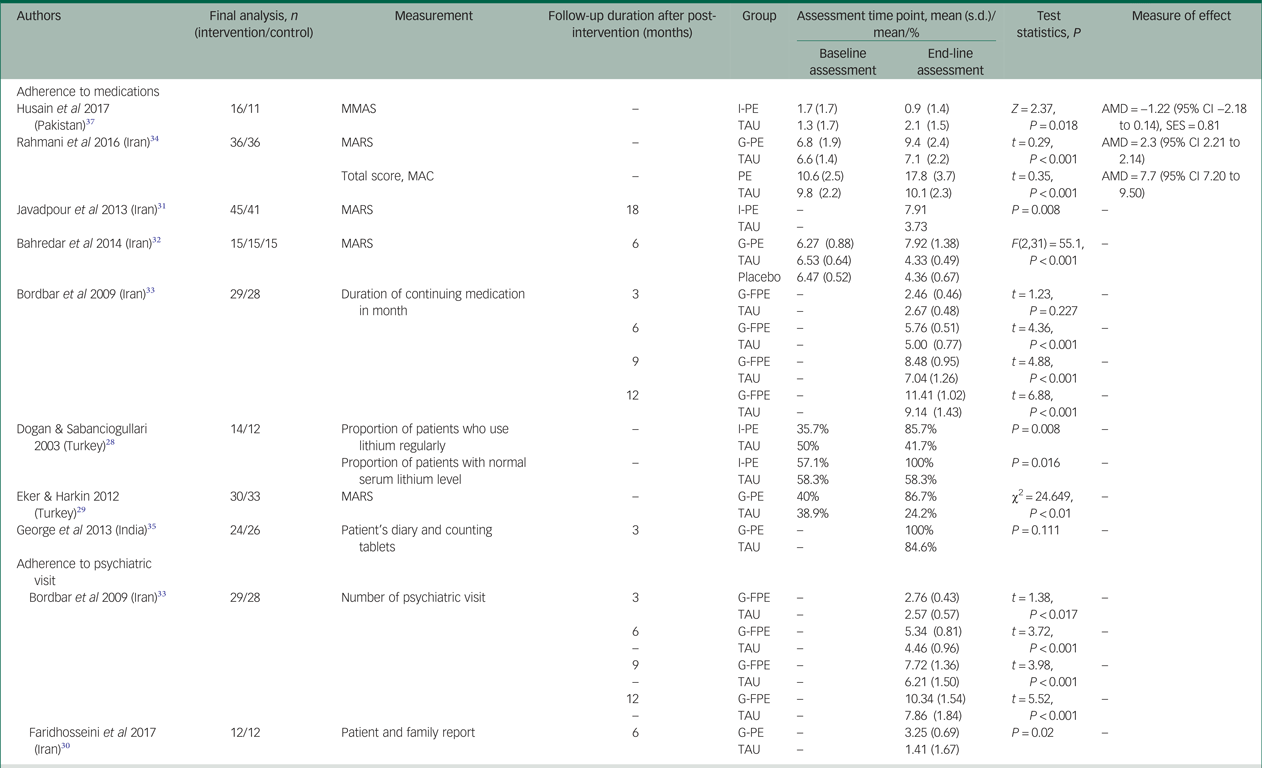
MMAS, Morisky Medication Adherence Scale; I-PE, individual psychoeducation; TAU, treatment as usual; AMD, adjusted mean difference; SES, standardised effect size; MARS, Medication Adherence Rating Scale; G-PE, group psychoeducation; MAC, Medicine Adherence Checklist; PE, psychoeducation; G-FPE, group family psychoeducation.
Reduction in hospital admissions
A total of five RCTs that assessed the efficacy of individual, group or family psychoeducation in reducing hospital admissions were identified (see supplementary file 6). Generally, the studies showed that fewer people with bipolar disorder were admitted to hospital in the intervention group compared with the control group.Reference Gumus, Buzlu and Cakir25, Reference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30, Reference Javadpour, Hedayati, Dehbozorgi and Azizi31, Reference Bordbar, Soltanifar and Talaei33
Improvement in QoL and functional status
A total of 10 of the 18 studies (9 psychoeducation and 1 CBT) assessed the efficacy of improving functional status and QoL (Table 5). The findings were mixed. Half of the studies reported, significant improvement in various domains of QoL in the intervention compared with the control groups: functioning,Reference Kurdal, Tanriverdi and Savas26, Reference Dogan and Sabanciogullari28, Reference Bahredar, Farid, Ghanizadeh and Birashk32 general health,Reference Dogan and Sabanciogullari28 physical, social,Reference Dogan and Sabanciogullari28, Reference Javadpour, Hedayati, Dehbozorgi and Azizi31 environmental and mental health domains of QoLReference Javadpour, Hedayati, Dehbozorgi and Azizi31 and in the overall QoL.Reference Husain, Chaudhry, Rahman, Hamirani, Mehmood and Haddad37 In one study, there was significant improvement in all domains of QoL except the mental health domain in those receiving CBT compared with treatment as usual.Reference Costa, Cheniaux, Range, Versiani and Nardi23 The rest of the studies did not reported significant differences between groups.Reference Cardoso, Farias, Mondin, da Silva, Souza and da Silva21, Reference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22, Reference Cuhadar and Cam27, Reference Faridhosseini, Baniasadi, Fayyazi Bordbar, Pourgholami, Ahrari and Asgharipour30
Table 5 Psychological intervention to improve quality of life and functioning
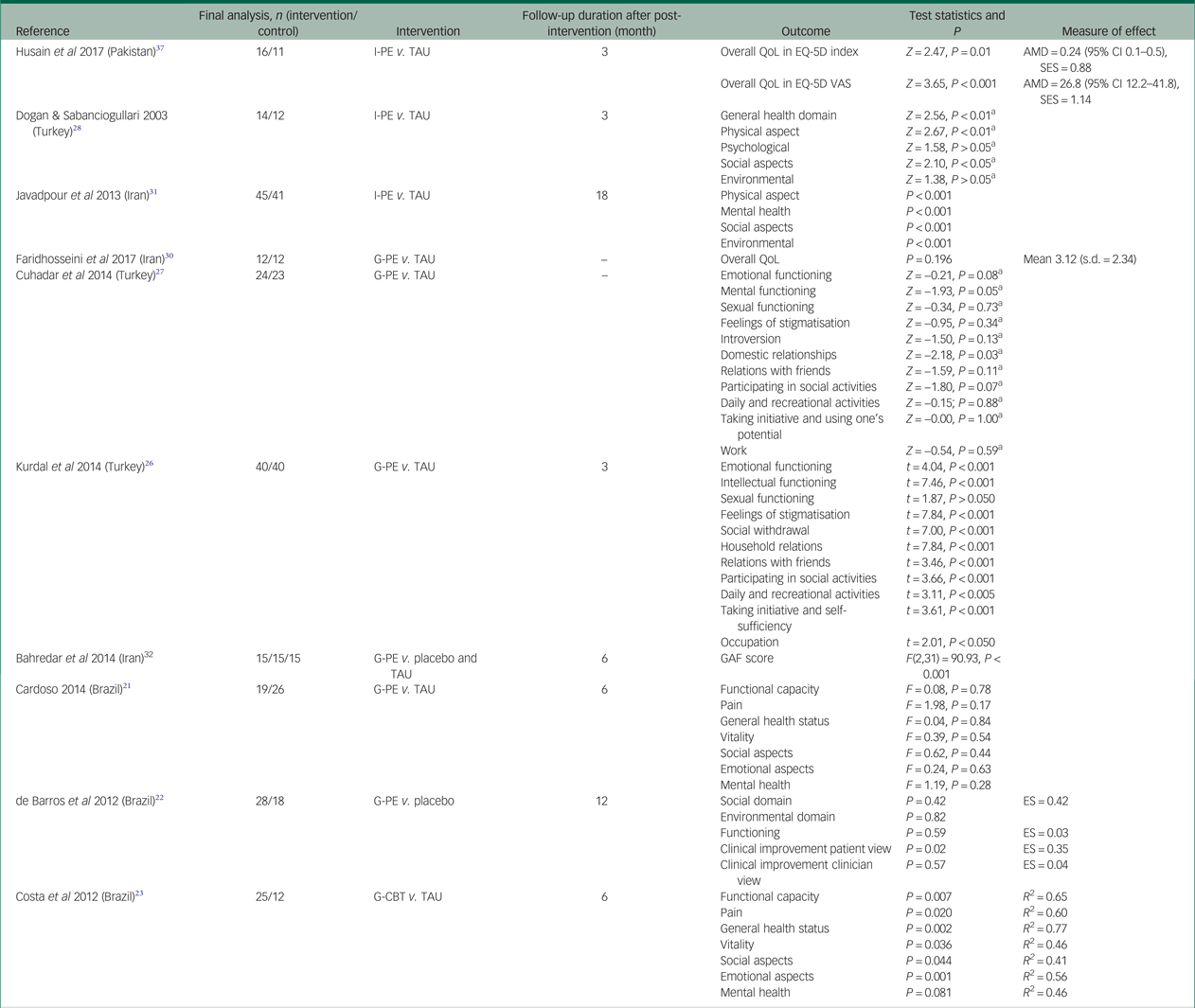
I-PE, individual psychoeducation; TAU, treatment as usual; AMD, adjusted mean difference; SES, standardised effect size; VAS, visual analogue scale; G-PE, group psychoeducation; QoL, quality of life; GAF, Global Assessment of Functioning; ES, effect size; G-CBT, group cognitive–behavioural therapy; R 2, squared value of correlation coefficient or the proportion of explained variation.
a. The comparison was made within arm and the reported result for the treatment group.
Discussion
This is the first systematic review synthesising the full range of psychological intervention studies that have been conducted among people with bipolar disorder in LMICs. In all studies reviewed, psychological interventions were given as adjuncts to treatment as usual, although the treatment as usual may have varied depending on drug licensing and treatment guidelines in each country. Nearly all of the included studies were conducted in upper-middle-income countries and none of the studies were from low-income countries compromising ability for direct generalisation of findings to low-income country settings. Absence of such studies in low-income countries may be linked to the broader lack of attention to bipolar disorder globally as well as in LMICs. The scarcity of clinician researchersReference Hanlon38 coupled with the poor funding environment may explain the scarcity of data on psychopathology, incidence, prevalence and course of bipolar disorder in LMICs.Reference Fekadu, Hanlon, Thornicroft, Lund, Kaaya and Alem39 However, even if focusing on upper-middle-income countries, these studies are important bridges to the broader LMIC setting than studies conducted in high-income countries. Additionally, the core principles of treatment were shared among the studies. For example, psychoeducation included in all the studies, is naturally consistent across settings. Most of the studies were tested in teaching or public hospitals with no intervention adaptations to the local context, which adds to the challenge of transferring these interventions. Nonetheless, identifying interventions of proven efficacy that have at least been tested outside of a high-income setting is a good starting point for adapting psychological intervention for LMICs. Therefore, they can be considered as potential candidates for further adaptation. Such an approach was taken when adapting psychological interventions for perinatal common mental disorders in LMICs with some success.Reference Clarke, King and Prost40 In general, the findings suggest the need for rigorous studies in LMICs.
Overall, the reviewed studies demonstrate the efficacy of adjunctive psychological interventions for bipolar disorder in terms of improving both depressive and manic symptoms, reducing relapse, hospital admissions and internalised stigma, improving QoL, treatment adherence and knowledge and attitudes about bipolar disorder
The majority of the studies assessed the efficacy of psychoeducation and all studies included a psychoeducation component. This is in line with the World Health Organization mhGAP intervention guideline, which endorses routine psychoeducation for people with bipolar disorders.Reference Dua, Barbui, Clark, Fleischmann, Poznyak and van Ommeren15 However, the mhGAP does not provide guidance on the number of sessions, content and delivery of the psychoeducation. In this review, 3 to 12 sessions of group, individual and family psychoeducation were effective in reducing relapse, hospital admissions and illness severity for both depression and mania. Therefore, a minimum of three sessions of psychoeducation may be required although a lower number of sessions may have to be tested. Furthermore, the mhGAP guideline is designed to be used by general health workers. However, in this review, most psychological interventions were delivered by mental health specialists and there was no evidence in relation to task-sharing with general health workers. This implies that there is no evidence to support psychoeducation provided by general health workers and calls for further evidence on this from LMICs.
It was also of interest to note that just one session of family psychoeducation improved outcomes on multiple domains: treatment adherence, relapse rates and hospital admissions.Reference Bordbar, Soltanifar and Talaei33 Given the family orientation of care in LMICs, brief family psychoeducation is a promising intervention that could be tested in the general healthcare context. Although this review confirms the benefits of psychological interventions as reported in high-income countries,Reference Miziou, Tsitsipa, Moysidou, Karavelas, Dimelis and Polyzoidou41, Reference Reinares, Sánchez-Moreno and Fountoulakis42 caution may be required in patients with a long duration of illness and multiple relapses. One of the reports where most of the participants had experienced multiple relapses and a long duration of illness (an average of 19 years), depressive symptoms worsened in both the treatment and control groups.Reference de Barros Pellegrinelli, de, Silval, Dias, Roso and Bandeira22 This may indicate that psychological interventions may be more effective for people with bipolar disorder who have experienced fewer relapses and have a short disease duration.Reference Scott, Paykel, Morriss, Bentall, Kinderman and Johnson12, Reference Reinares, Sánchez-Moreno and Fountoulakis42 Findings related to CBT were consistent with those from high-income countries.Reference Miziou, Tsitsipa, Moysidou, Karavelas, Dimelis and Polyzoidou41, Reference Reinares, Sánchez-Moreno and Fountoulakis42
Limitations
The review was comprehensive in terms of databases searched and types of psychological interventions and study designs. However, a meta-analysis was not possible because of the heterogeneity of the included studies in terms of the type of interventions, number of sessions and duration of follow-up time and format of intervention delivery. Second, studies with negative findings might not have been published. Additionally, two of the papersReference Cuhadar and Cam27, Reference Dogan and Sabanciogullari28 carried out within-group comparisons with post-assessment against baseline. Non-availability of the raw data precluded re-analysis. Third, since nearly all the studies were from upper-middle-income countries, the findings may not be directly generalisable to low-income country settings (see supplementary file 7 for a list of countries by income group).
Implications
The reviewed literature showed promising results relating to the efficacy of adjunctive psychological interventions on a broad range of clinical and QoL parameters in LMICs. However, virtually all studies identified in this comprehensive review were from upper-middle-income countries and none involved general health workers. Contextually appropriate adaptation of interventions for low-income settings and for task-shifted care as well as larger-scale studies are important next steps.
Funding
This work is supported through the DELTAS Africa Initiative (DEL-15-01) and Addis Ababa University. The DELTAS Africa Initiative is an independent funding scheme of the African Academy of Sciences (AAS)'s Alliance for Accelerating Excellence in Science in Africa (AESA) and supported by the New Partnership for Africa's Development Planning and Coordinating Agency (NEPAD Agency) with funding from the Wellcome Trust (DEL-15-01) and the UK government. The views expressed in this publication are those of the author(s) and not necessarily those of AAS, NEPAD Agency, Wellcome Trust or the UK government.
A.F. is supported by the Medical Research Council/Department for International Development through the African Research Leader scheme.
Supplementary material
Supplementary material is available online at https://doi.org/10.1192/bjo.2018.46.









eLetters
No eLetters have been published for this article.