Introduction
Several reconstructive methods are employed for restoration of ossicular chain continuity. These methods attempt to bridge the gap formed by erosion of the long process of the incus and/or an absent stapes, thereby rehabilitating the hearing. Some of these methods include placing a prosthesis (partial or total ossicular reconstruction prostheses), or using bone cement, tragal cartilage or sculpted incus interposition. Overall, the choice of technique and material remains a hot topic among otologists.Reference Borgstein and Achbab1–Reference Spencer7 In this study, variations of the latter technique will be described and evaluated. This is especially useful given its simplicity and cost-effectiveness.
Materials and methods
Ethical considerations
This study was approved by the Tergooi Hospital research committee.
Study design
This single-centred, retrospective study was carried out at the ENT department of the Tergooi Hospital in the Netherlands. A chart review was conducted of patients’ surgical records between June 2010 and October 2017. The study included all patients who presented with erosion of the long process of the incus with an intact stapes superstructure (Figure 1a), due to atelectasis (with or without cholesteatoma), who were treated with unsculpted incus interposition. In this patient group, solely the autologous, eroded incus was used for reconstruction. Patients who had a medical history of ossicular chain reconstruction surgery and/or radical mastoidectomy executed elsewhere were excluded.
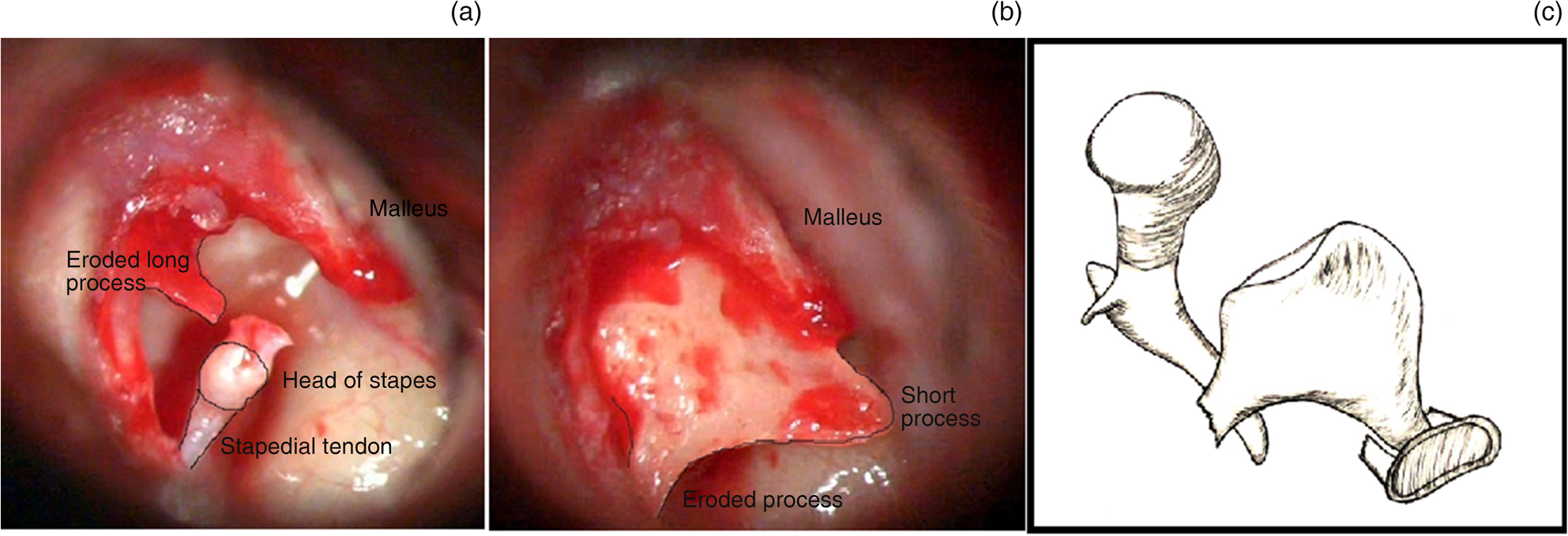
Fig. 1. Peri-operative pictures and illustration showing (a) the eroded long process of the incus with an intact stapes, and incus interposition with (b) the incus as partial and (c) as total ossicular replacement.
Techniques
All procedures were executed via a transmeatal approach. The retraction pocket, atelectasis or cholesteatoma matrix is carefully removed from the involved middle-ear structures. The mobility of the ossicular chain, the degree of erosion of the long process of the incus and the condition of the stapes superstructure are evaluated.
After disarticulation of the incudomalleolar joint, the incus remnant is carefully extracted, taking care to preserve the chorda tympani. The interposition is formed by rotating the incus on its axis and placing the corpus on the stapes, with the long process remnant just above the stapedial tendon, and the short process parallel to the malleus and against the malleus handle (Figure 1b). The incus does not need to be removed from the middle ear except for cleaning if it is involved in cholesteatoma. The incus is not modified by drilling.
In case of chain discontinuity due to erosion involving the long process of the incus and the stapes superstructure, but with a mobile footplate, the incus is similarly separated from the malleus and extracted. This is followed by gently lateralising the malleus, and placing the short process directly in the oval window and the long process remnant under the handle of the malleus (Figure 1c).
No additional material is needed for incus fixation. When the tympanomeatal flap is replaced in its original position, the tympanic membrane drapes over the most lateral part of the incus. This way, the ossicular continuity is restored.
In case of cholesteatoma, a second-look revision surgery is planned after 9–12 months. Pure tone audiograms were conducted at 1 week pre-operatively, and at 6 weeks and 6–12 months post-operatively, to evaluate the results.
Main outcome measures
The following data were collected and investigated: sex, age, operative state of the tympanic membrane, middle-ear findings, follow-up duration, revision surgical procedure details, and pre- and post-operative audiogram results. The main outcomes were: post-operative air–bone gap (across 0.5, 1, 2 and 4 kHz) and overall level of air–bone gap closure. Additionally, follow-up time and any revision surgical procedure details were examined. Data from the last available post-operative audiogram were used to calculate the hearing outcomes. A paired sample t-test was performed in SPSS Statistics version 24.0 software to compare pre- and post-operative air–bone gaps (IBM, Armonk, New York, USA).
Results
A total of 33 ears of 32 patients (18 male and 14 female) were included, 22 ears in the partial ossicular reconstruction prosthesis group and 11 ears in the total ossicular reconstruction prosthesis group. Median patient age was 39 years (range, 4–84 years). Follow-up time for the first post-operative audiogram was 6 to 8 weeks for 27 patients, 3 to 4 months for 5 patients, and 7 months for 1 patient. At the last post-operative audiogram, follow-up duration was 6–17 months for 21 patients, 3–5 years for 5 patients and 7 years for 1 patient.
In the partial ossicular reconstruction prosthesis group, the median patient age was 44 years (range, 4–84 years). The pre-operative air–bone gap ranged from 6.25 to 40 dB, with a mean of 24 dB (standard deviation (SD) = 11 dB). The last post-operative audiograms showed a mean air–bone gap of 19 dB (SD = 6.8 dB), ranging from 6.25 to 33.75 dB. The total ossicular reconstruction prosthesis group had a median age of 34 years (range, 10–45 years). The pre-operative air–bone gap ranged from 15 to 53 dB, with a mean of 34 dB (SD = 10.4 dB). The mean of the last post-operative air–bone gap was 28 dB, with a range of 6.25–51.25 dB (SD = 14.6 dB).
A mean post-operative air–bone gap under 25 dB was considered a successful result. This was achieved in 25 patients (76 per cent), 20 (91 per cent) in the partial ossicular reconstruction prosthesis group and 5 (45 per cent) in the total ossicular reconstruction prosthesis group. In 30 per cent of cases, the air–bone gap was closed to 15 dB or less, of which 70 per cent were in the partial ossicular reconstruction prosthesis group. The difference between pre- and post-operative mean air–bone gaps was statistically significant (p = 0.007). Five patients with recurrent conductive hearing loss or cholesteatoma required revision surgery where the interposition was either left untouched, remobilised or repositioned. Figures 2 and 3 show the audiogram results with corresponding revision surgical procedures, excluding planned second-look revisions in cholesteatoma cases. No sensorineural hearing loss was recorded.

Fig. 2. Partial ossicular reconstruction prosthesis group pre-operative (pre-op) and post-operative (post-op) air–bone gaps (ABGs), with long-term results as available. Patients 1, 6 and 18 underwent revision surgery. Patients 10 and 11 had otitis media with effusion at time of the last post-operative audiogram.

Fig. 3. Total ossicular reconstruction prosthesis group pre-operative (pre-op) and post-operative (post-op) air–bone gaps (ABGs), with long-term results as available. Patient 8 and 10 underwent revision surgery.
Discussion
Ossicular chain discontinuity due to erosion of the long process of the incus is a common finding secondary to cholesteatoma and atelectasis. The fibrinous middle layer of the tympanic membrane and negative pressure in the middle ear results in retraction and adhesion to the ossicles. With time, this causes erosion of the long process of the incus and stapes superstructure, and eventual conductive hearing loss.
Synopsis of key findings
This study examined a small group of patients where a functional interposition was formed from the autologous incus, without any modification. This provides cost-effective options to substitute bone allografts, synthetic partial or total ossicular reconstruction prostheses, or bone cement, using unmodified autologous material. In most patients, post-operative audiogram results showed hearing outcomes within the normal range and significant improvement of pre-operative conductive hearing loss. Moreover, no extrusion of the incus was recorded and none of the patients had post-operative sensorineural hearing loss. Where the hearing was adequate, it generally remained stable. Diffusion-weighted magnetic resonance imaging was used to determine the need for re-operation.
Clinical applicability of study
The study results are similar to those of previously published papers describing air–bone gap closure with several methods of ossicular chain reconstruction, including sculpted incus interposition. Multiple studies attained success rates of 66–74 per cent for autograft, 54–86 per cent for partial ossicular reconstruction prosthesis and 51–55 per cent for total ossicular reconstruction prosthesis ossiculoplasty.Reference Celenk, Baglam, Baysal, Durucu, Karatas and Mumbuc2,Reference Bauer8–Reference Sterrer and Loader14
• Ossicular chain reconstruction is commonly conducted during tympanoplasty for atelectasis and cholesteatoma
• Traditionally, total or partial ossicular reconstruction prostheses are used, or the incus is removed, sculpted and re-inserted
• This study shows that an unsculpted incus gives comparable results to prostheses or sculpted incus
• It is an especially useful technique in hospitals without access to prostheses or a drill for incus sculpting
• Given that the incus is unmodified, this procedure is easier to perform
Previous incus interposition series have described the use of a sculpted incus, whereas in this study the eroded incus is placed without any modification, saving time and effort. This makes the technique feasible for the less experienced otologist and in resource-poor hospitals. It is important for otologists to be aware of the possibilities and results that may be obtained, in settings where these techniques may be the only available option. With the cost of a synthetic prosthesis being approximately 150–300 Euros, in addition to the cost of the surgical sets required, placement of a prosthesis is often prohibitively expensive for patients and healthcare institutions in low-income countries. Furthermore, the risk of extrusion is minimised by using autologous material.
Other advantages of using the unmodified incus include the elimination of the risk of the ossicle falling out of the ear while handling and drilling to sculpt, which also results in a shorter operative time and avoids the possibility of damaging the incus to a degree that makes it unsuitable to use as a graft.
Considerations
Our data show a follow-up time ranging from six weeks to seven years, indicating that a few patients only had one post-operative audiogram. Given that the hearing can improve or deteriorate in the months following surgery, this could be a limitation. Nonetheless, no patients returned with persistent or recurring hearing loss or, to the extent of our registered data, were referred to other centres for further therapy. The relatively small study groups can be seen as a limitation, and further data are being collected.
The middle-ear mucosa and tympanic membrane are known to have an extraordinary regenerative ability.Reference Borgstein, Stoop, Halim and Feenstra15 Nevertheless, this study also shows that time and patience can be important factors in ossicular chain reconstructive techniques, as some patients did not have the expected hearing results within the first months after surgery but later showed remarkably better outcomes in terms of conductive hearing loss. We found improvements up to a year after surgery. It is therefore important to implement a ‘wait and see’ approach in these cases before considering re-operation, and to inform patients of this necessity. Conversely, once a good result was achieved, we did not see subsequent deterioration of the hearing, though a longer follow-up duration will be needed to confirm this finding.
In six of the patients, cartilage interposition placed earlier (using a previously detailed techniqueReference Borgstein and Achbab1) was no longer functioning due to incus erosion, and was replaced by non-sculpted incus interposition, resulting in successful hearing improvement in five cases. This shows that incus interposition, as described in this study, could also act as a second-stage option during reconstruction surgery. Several patients who had surgical revisions were found to have formed adhesions, possibly affecting hearing; during revision surgery, these adhesions were eliminated in order to remobilise the ossicular chain and optimise the function of the interposition. No evidence of bony fixation of the incus was found at revision surgery.
Conclusion
In this small study, successful preservation and improvement of overall hearing results was observed in most patients. The technique described provides time- and cost-saving options, and is very useful in the otologist's ‘arsenal’ as an alternative to other reconstruction techniques. It is especially suitable for use in resource-poor hospitals within low-income countries. Longer follow-up studies with larger patient numbers are needed to assess whether these reconstructions can withstand the test of time, or whether additional reconstruction techniques are necessary.
Competing interests
None declared





